Abstract
Graft-versus-host disease (GVHD) is a major cause of morbidity and mortality of allogeneic stem cell transplantation. Strategies to control GVHD while maintaining graft versus leukemia (GVL) include herpes simplex virus thymidine kinase (HSV-tk) gene transduction of donor T cells followed by treatment with ganciclovir (GCV). Alternatively, GVHD and GVL may be mediated by distinct processes. In this regard, whether cytokine polarization occurs and to what degrees various subsets of cytokine-producing T cells mediate GVHD or GVL has been an active area of research using cytokine or cytokine antibody infusion or genetically deficient mice. This study takes a different approach that allows simultaneous investigation into both the mechanisms underlying GVHD reactions and the efficacy of HSV-tk suicide gene-based T-cell deletion. A source of donor T cells, splenocytes from mice transgenic for HSV-tk controlled by elements of either the interleukin-2 (IL-2) or IL-4 promoters (IL-2-tk and IL-4-tk, respectively) was used, thus allowing investigation into the roles of T1 and T2 cells in ongoing GVHD reactions. To assess treatment rather than prevention of GVHD, GCV was started at peak disease. Remarkably, treatment at this late time point rescued mice from the clinical effects of GVHD caused by T cells expressing either transgene. Thus, both T1 and T2 cells play an important role in clinical GVHD in a minor histocompatibility antigen-mismatched setting. In addition, because clinical disease was reversible even at its maximum, these observations provide controlled evidence that this strategy of treating ongoing GVHD could be effective clinically.
Introduction
Graft-versus-host disease (GVHD) remains a major cause of morbidity and mortality from allogeneic stem cell transplantation (alloSCT). It thereby limits the application of this therapy for the cure of hematopoietic stem cell disorders. In the context of cancer therapy, GVHD is often accompanied by graft versus leukemia (GVL), which is responsible for much of the antineoplastic effect.1,2 The combination of toxic and desirable effects of donor T cells creates a therapeutic paradox. It would be ideal to devise methods of separating GVHD from GVL or to control GVHD, balancing the benefits of GVL with the toxicity of GVHD. Much effort has gone into various approaches to accomplish these goals, with partial success.3-7
Nonetheless, ultimate success will require a better understanding of the pathophysiology of GVHD and the mechanisms of GVL. An area of active GVHD research is whether cytokine polarization occurs and to what degrees various subsets of cytokine-producing T cells contribute to disease.8-16 In particular, it has been suggested that acute GVHD (aGVHD) is the result of T1 polarization, whereas chronic GVHD may be due to outgrowth of T2-polarized donor T cells.8,17-20 Indeed, there is some evidence that Th2 cells can inhibit aGVHD,11 although studies on this issue have been equivocal. Cytokine reverse transcriptase–polymerase chain reaction results from mice undergoing either aGVHD or chronic GVHD in a parent into F1 (P → F1) model have been supportive.18-21 However, in some cases infusion of Th1-promoting cytokines, such as interleukin-12 (IL-12),12,15 have augmented aGVHD, whereas in others it has protected.14 Similarly, anticytokine antibody studies have given conflicting results.12,22 GVHD has been investigated by using donor T cells from knockout (KO) mice lacking either IL-4 or interferon γ (IFN-γ).22,23 These studies have suggested a role for both T1- and T2-type cells, although the IFN-γ KO T cells were less capable of causing disease, suggesting a dominant T1 role. These studies were carried out in fully or major histocompatibility complex (MHC)–mismatched strain combinations in which the allogeneic stimulus is strong. Recently, similar results were obtained by using donor T cells from Stat4 or Stat6 KO mice, which tend to polarize to Th2- or Th1-type cells, in a fully mismatched bone marrow transplantation system.16 In view of these conflicting results, the relative roles of T1 and T2 cells in GVHD and in particular GVL remain unclear.
Other investigators have proposed strategies to gain control of GVHD or to separate GVHD from GVL,24-30 most notably suicide gene transduction.31-34 In this strategy, donor T cells express a gene, such as herpes simplex virus thymidine kinase (HSV-tk), which renders the T cell sensitive to killing by ganciclovir (GCV), provided the cell is also dividing. To apply this strategy clinically, a method of efficient gene transduction is required, along with the ability to select transduced cells. Furthermore, a number of biological issues need to be worked out, including T-cell and GCV dosing schedule, specificity/toxicity of GCV treatment, evaluation of GCV effect in various target tissues, effect on T-cell immunocompetence after treatment, and the reversibility of established GVHD lesions.35 Nonetheless, this strategy has been implemented in humans as well as in animal models. Indeed, promising although anecdotal reports have suggested efficacy in humans, arguing that further effort should be put into this approach.7,33Similarly, a few murine models using T cells from mice that are transgenic (Tg) for HSV-tk have been developed, which have largely been used to show that treatment with GCV at the time of transplantation in fully allogeneic models can prevent disease, although in one report, there was partial efficacy in a treatment model.34,36 37
We have taken a somewhat different approach that allows simultaneous investigation into both the mechanisms underlying GVHD reactions and the feasibility of HSV-tk–based T-cell deletion. Our model also takes advantage of Tg-based expression of HSV-tk, thus obviating any issues of gene transduction. We have used Tg mice in which the HSV-tk transgene is controlled by either the IL-2 or IL-4 promoters (IL-2-tk and IL-4-tk, respectively), thus allowing investigation into the roles of T1 and T2 cells in ongoing GVHD reactions.38-40 These transgenes have been well studied in vitro. Although both are expressed very early after T-cell activation, under conditions in which T cells are polarized toward Th1 cytokine expression, only the IL-2-tk transgene is expressed, whereas the opposite is true under Th2 polarization conditions.38-40 The use of conditional ablation differs from other approaches to investigating cytokine polarization in that (1) T-cell polarization is initiated normally, (2) potential developmental abnormalities associated with KO mice are avoided, and (3) deletion is more precise than cytokine infusion or inhibition via antibodies that can affect multiple tissues and does not necessarily mimic the effects of cytokine polarization. In addition, inhibition or KO of particular cytokines may not completely inhibit the biologic effect of a polarized cell (eg, IL-4 inhibition may leave the effects of IL-5 unchecked, although it may also tend to polarize cells away from the T2 type).
We have crossed these transgenes onto the B10.BR background and have used the minor histocompatibility antigen (miHA)–mismatched, MHC-matched B10.BR → AKR model of aGVHD drslt.41,42 In this model, CD4 T cells are required for full pathogenicity,42 thus making the contribution of Th1 or Th2 cells relevant. We used the spleen cells from the Tg mice as donors in GVHD experiments. To determine the contributions of T1 and/or T2 cells at the peak of GVHD, we began treating recipients at day 14 after transplantation, when weight loss is maximal and mortality begins. Remarkably, we found that treatment at this late time rescued mice from the clinical effects of GVHD, averting mortality in nearly all treated mice and allowing weight gain that typically matched that of bone marrow (BM)–only controls. This effect was seen whether the donor T cells carried the IL-2-tk or the IL-4-tk transgene, but it was not seen with Tg-negative T cells. Thus, these results indicated that both T1 and T2 cells play an important role in maximal clinical GVHD in a miHA-mismatched setting. In addition, because clinical disease was reversible even at its maximum, our observations further suggest that a strategy of controlling ongoing GVHD could be effective clinically. This system could be a good model to study the mechanism and limitations of this approach. Indeed, there may be some limitations, because histologic disease was only partly ameliorated in both types of models.
Materials and methods
Mice
Six- to 8-week-old AKR and B10.BR male mice (Jackson Laboratories, Bar Harbor, ME) were used as recipients and BM donors. For the induction of GVHD, splenocytes from male IL-2-tk or IL-4-tk Tg mice38 39 (6-9 weeks) were used as the source of alloreactive T cells. The Tg mice were crossed onto the B10.BR background; they are more than 99.9% B10.BR. All the mice were maintained under specific pathogen-free conditions at Yale University School of Medicine, New Haven, CT.
GVHD induction
Host animals received 950 cGy from a 137Cs source. Two or more hours later, T-cell–depleted allogeneic donor BM (107 cells) with splenocytes from B10.BR Tg mice (IL-2-tk, IL-4-tk) (107 cells) or from Tg-negative littermates were given via tail vein. Mice receiving only BM were included in each experiment. After 2 weeks, an osmotic pump (Alzet, Model 2004, Cupertino, CA, 0.25 μL per hour, 28 days) containing either GCV or phosphate-buffered saline (PBS) was implanted subcutaneously.
Osmotic pump implantation
Recipients were randomly divided into 2 groups at day 14 to receive pumps containing GCV (625 mg/mL; 3.75 mg/d) (Roche Laboratories, Nutley, NJ) or PBS. Animals were anesthetized by injection with a mixture of ketamine (10 mg/mL) and xylazine (2 mg/mL) at a dose of 10 μL/g intraperitoneally. The pumps were implanted on the back under sterile conditions.
Pathology techniques and staining
Tissues (skin, ear, tongue, liver, and intestine) were harvested and divided into 2 parts. For hematoxylin and eosin (H&E) staining the organs were fixed in 10% formalin and embedded in paraffin. For immunohistochemistry, tissues were fixed with diluted formalin (containing 0.7% formaldehyde) overnight at 4°C, dehydrated in 30% sucrose for 3 hours, frozen in Tissuetek (Sakura, Elkhart, IN), and stored at −80°C.
Frozen tissues were sectioned and mounted on 10% polylysine-coated slides. After blocking with 10% normal rat serum (Gemini Bioproducts, Calabasas, CA) and 3% bovine serum albumin (BSA), sections were incubated with biotinylated anti-CD8 or -CD4 monoclonal antibodies (Pharmingen, San Diego, CA) overnight at 4°C. After washing with 1% BSA in PBS, slides were stained with streptavidin-conjugated horseradish peroxidase followed by development with 3-amino-9-ethyl-carbazole (Sigma, St Louis, MO). The sections were counter stained with hematoxylin and mounted with Glycergel (Dako, Carpinteria, CA).
Sections were coded and scored without knowledge of the treatment group by pathologists (M.E.R. for gut and liver; J.M.M. for ear, skin, and tongue). Skin was scored 0 to 3 for interface/apoptosis, infiltration, fibrosis, and extent of disease and the scores were totalled. For the intestine, an integrated GVHD severity score was assigned (0 to 3) by the pathologist on the basis of the following parameters: apoptosis, reactive epithelium, and inflammation.
Flow cytometry
To determine the origin of lymphocytes in the lymphoid organs, single cell suspensions were stained with Cy5–anti-Thy1.2 (clone 30H12, purified and conjugated in our laboratory) and biotin–anti-Thy1.1 (clone 19E12, prepared in our laboratory, and is specific for the recipient) followed by streptavidin-conjugated phycoerythrin (PE). Four-color staining was performed (CD44-FITC, CD4-PE, CD8-QR, and CD62L-SA-APC) as described.43 CD44 (clone IM7) and CD62L (clone Mel-14) antibodies were prepared in our laboratory, and the others were obtained from Pharmingen. Cells were analyzed on a FACSCalibur (Becton Dickinson, Woodstock, VT). Intracellular cytokine staining was performed as described44 after culturing cells for 5 hours with phorbol myristic acid and ionomycin, including monensin during the last 2 hours of culture. Prior to permeabilization, dead cells were identified with ethidium monoazide45 and later gated out in the FL3 channel. The following antibodies (Pharmingen) were used: rat immunoglobulin (Ig)G1-PE (clone R3-34), rat IgG2b-APC (clone A95-1), anti–IFN-γ–PE (clone XMG1.2), anti–IL-4-PE (clone 11B11), anti–IL-2-APC (clone JES6-5H4).
Statistics
Differences between survival curves were assessed by Kaplan-Meier analysis. The significance of differences in weights between groups at individual time points and between percentages of cells in flow-activated cell sorter (FACS) gates was assessed by using the 2-tailed Student t test. The Mann-Whitney test was used to determine significance of histology score differences between groups.
Results
Experimental design
Our experiments had 2 goals: first, to use cell ablation to test the hypothesis that acute GVHD is a T1-polarized disease and, second, to model the treatment of aGVHD by GCV-mediated deletion of thymidine kinase–expressing T cells. To address the first aim, we used both the IL-2-tk and IL-4-tk Tg mice. Although both transgenes are expressed very early on in T-cell activation, under Th1-polarizing conditions, IFN-γ expression by IL-4-tk CD4 cells is unaffected by GCV treatment after only 2 days in culture in vitro, whereas IL-4 production from the same cells is continually sensitive to GCV. Thus, the IL-4-tk gene is a sensitive and specific tool for the ablation of Th2 cells but not Th1 cells.38-40
To address the second aim—modeling of GCV treatment, rather than prevention,34,37 46 of aGVHD—we initiated treatment at day 14 after transplantation, a time when weight loss is greatest and mice are beginning to die. This time is also a peak of histologic disease (data not shown). This design has the added benefit of allowing substantial in vivo time for any putative cytokine polarization to take place.
GCV treatment prevents death and reverses clinical GVHD as measured by weight gain
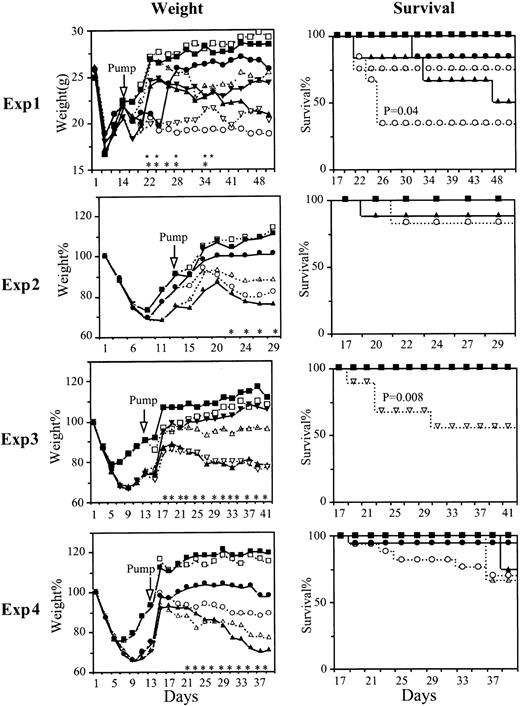
Figure 1 shows the results of 4 separate experiments in which death was the end point. IL-2-tk mice were studied in experiments 1, 2, and 4 (total of 55 treated mice) and IL-4-tk in experiments 1 and 3 (total of 28 treated mice). All experiments included BM alone and Tg-negative groups. In each case, treatment of IL-tk mice with GCV provided substantial improvement of clinical GVHD as demonstrated by weight gain (left panels). In most experiments, the treated mice eventually gained weight to match that of BM-only controls, and in every case weight equaled or exceeded pretransplantation weights. PBS-treated mice typically had weights of 80% or less of pretransplantation levels. Differences between GCV- and PBS-treated recipients of IL-tk T cells were significant on multiple days in every experiment. In contrast, GCV-treated recipients of T cells from Tg-negative mice had persistent weight loss. In fact, in all experiments except experiment 4, the recipients of Tg-negative T cells that were treated with GCV had greater weight loss than those treated with PBS, the reverse of the situation with recipients of Tg-positive T cells. This finding could reflect some degree of toxicity of GCV in these sick recipients of Tg-negative T cells that was nevertheless counterbalanced by relief of GVHD in the recipients of Tg-positive T cells.
Weight and survival curves.
Four experiments are shown. The weight curves show the average weight (Experiment 1) or the percentage of the individual weight for each group, considering the initial weight of each mouse was 100% (Experiments 2-4; squares for BM alone, triangles for Tg negative, circles for IL-2-tk, and inverted triangles for IL-4-tk splenocyte recipients). Empty symbols and dashed lines indicate control PBS, and the solid symbols and lines indicate GCV-treated groups. Asterisks or stars indicate that the difference between the GCV-treated and control groups are statistically significant (P < .05, 2-tailedt test) (in Experiment 1* for IL-2-tk, * for IL-4-tk group). The survival curves show the percentage of survival in each group. TheP values are from chi-square test, comparing the GCV-treated and control group.
Weight and survival curves.
Four experiments are shown. The weight curves show the average weight (Experiment 1) or the percentage of the individual weight for each group, considering the initial weight of each mouse was 100% (Experiments 2-4; squares for BM alone, triangles for Tg negative, circles for IL-2-tk, and inverted triangles for IL-4-tk splenocyte recipients). Empty symbols and dashed lines indicate control PBS, and the solid symbols and lines indicate GCV-treated groups. Asterisks or stars indicate that the difference between the GCV-treated and control groups are statistically significant (P < .05, 2-tailedt test) (in Experiment 1* for IL-2-tk, * for IL-4-tk group). The survival curves show the percentage of survival in each group. TheP values are from chi-square test, comparing the GCV-treated and control group.
With the use of mortality as an end point, a similar situation was seen, although only in those experiments in which GVHD was severe enough to cause substantial mortality in the PBS-treated controls (ie, experiment 1 for IL-2-tk recipients and experiment 3 for IL-4-tk recipients). Consistent with the weight gain of GCV-treated recipients of IL-tk T cells, there were very few deaths in these groups in any of the experiments.
Thus, as measured by weight loss and mortality, ablation of cells expressing IL-2 or IL-4 was sufficient to substantially ameliorate aGVHD even when it was severe at the onset of treatment (ie, when mice had already lost more than 30% of original body weight, Figure 1). The potential mechanisms for this protection will be discussed further below.
GCV treatment partially ameliorates histologic disease
To determine the effects on histologic disease, additional transplantation experiments were performed in which all surviving mice were killed at day 28. The effect of GCV on weight was similar to the prior observational experiments, thus further replicating and corroborating these experiments (data not shown). Skin, ear, tongue, small and large intestine, and liver were evaluated (Tables1 and 2 and Figure 2). Statistically significant improvements in pathology score in GCV-treated recipients of IL-tk Tg T cells were observed in some but not all organs. Disease was significantly reduced in the tongue of IL-2-tk recipients. In particular, disease was ameliorated in the large intestine in both the IL-2-tk and IL-4-tk T-cell recipients. Trends toward histologic improvement, as indicated by the median scores in Tables 1 and 2, were seen in several other organs, but they did not reach significance. Because a limited number of samples were subjected to pathologic analysis, the statistical power of the study to detect differences was somewhat limited.
Effect of GCV treatment on pathology scores in recipients of IL-2-tk spleen cells
| Organ . | Group . | |||||
|---|---|---|---|---|---|---|
| BM (PBS) (2) . | BM (GCV) (2) . | Tg− (PBS) (1) . | Tg− (GCV) (5) . | IL-2-tk (PBS) (9) . | IL-2-tk (GCV) (11) . | |
| Liver | 0.5 ± 0.7 | 0.5 ± 0.7 | 2 ± 0 | 2 ± 0.8 | 2 ± 0.4 | 1 ± 0.7 |
| Colon | 0 ± 0 | 0 ± 0 | 3 ± 0 | 3 ± 0.5 | 2 ± 0.4 | 1 ± 0.7* |
| Small intestine | 1.5 ± 0.7 | 1 ± 0 | 0 ± 0 | 2 ± 0.4 | 1 ± 0.7 | 2 ± 0.5 |
| Skin | 0 ± 0 | 0 ± 0 | 7 ± 0 | 1 ± 3.7 | 0 ± 2.2 | 0 ± 2.2 |
| Ear | 0 ± 0 | 0 ± 0 | 8 ± 0 | 6 ± 3.6 | 3 ± 2.5 | 0 ± 2 |
| Tongue | 0 ± 0 | 0 ± 0 | 2 ± 0 | 2 ± 2.2 | 2 ± 1.4 | 0 ± 0.9* |
| Organ . | Group . | |||||
|---|---|---|---|---|---|---|
| BM (PBS) (2) . | BM (GCV) (2) . | Tg− (PBS) (1) . | Tg− (GCV) (5) . | IL-2-tk (PBS) (9) . | IL-2-tk (GCV) (11) . | |
| Liver | 0.5 ± 0.7 | 0.5 ± 0.7 | 2 ± 0 | 2 ± 0.8 | 2 ± 0.4 | 1 ± 0.7 |
| Colon | 0 ± 0 | 0 ± 0 | 3 ± 0 | 3 ± 0.5 | 2 ± 0.4 | 1 ± 0.7* |
| Small intestine | 1.5 ± 0.7 | 1 ± 0 | 0 ± 0 | 2 ± 0.4 | 1 ± 0.7 | 2 ± 0.5 |
| Skin | 0 ± 0 | 0 ± 0 | 7 ± 0 | 1 ± 3.7 | 0 ± 2.2 | 0 ± 2.2 |
| Ear | 0 ± 0 | 0 ± 0 | 8 ± 0 | 6 ± 3.6 | 3 ± 2.5 | 0 ± 2 |
| Tongue | 0 ± 0 | 0 ± 0 | 2 ± 0 | 2 ± 2.2 | 2 ± 1.4 | 0 ± 0.9* |
Shown are means ± SD of scores from each indicated group. Numbers of mice in each are given in parenthesis after the group name.
P < .05.
Effect of GCV treatment on pathology scores in recipients of IL-4-tk spleen cells
| Organ . | Group . | |||||
|---|---|---|---|---|---|---|
| BM (PBS) (4) . | BM (GCV) (4) . | Tg− (PBS) (4) . | Tg− (GCV) (4) . | IL-4-tk (PBS) (7) . | IL-4-tk (GCV) (7) . | |
| Liver | 0.5 ± 0.6 | 1 ± 0.5 | 1 ± 0.5 | 1 ± 0.5 | 1 ± 0.5 | 0 ± 1.6 |
| Colon | 0 ± 1 | 0 ± 0 | 1 ± 0.5 | 1.5 ± 0.6 | 2 ± 0.8 | 0 ± 0.8* |
| Small intestine | 0.5 ± 0.6 | 0.5 ± 1 | 0 ± 1 | 1.5 ± 1 | 1 ± 0.5 | 1 ± 1 |
| Skin | 0 ± 0.5 | 0 ± 0.8 | 2.5 ± 1.7 | 3.5 ± 3.3 | 4.5 ± 2.2 | 0 ± 1.6 |
| Ear | 0.5 ± 0.96 | 1 ± 1.2 | 4.5 ± 1 | 6.5 ± 3.5 | 5 ± 2.4 | 2 ± 2.1 |
| Tongue | 0 ± 0.58 | 0 ± 1 | 3.5 ± 1.9 | 4 ± 0.6 | 0 ± 1.7 | 0 ± 1.6 |
| Organ . | Group . | |||||
|---|---|---|---|---|---|---|
| BM (PBS) (4) . | BM (GCV) (4) . | Tg− (PBS) (4) . | Tg− (GCV) (4) . | IL-4-tk (PBS) (7) . | IL-4-tk (GCV) (7) . | |
| Liver | 0.5 ± 0.6 | 1 ± 0.5 | 1 ± 0.5 | 1 ± 0.5 | 1 ± 0.5 | 0 ± 1.6 |
| Colon | 0 ± 1 | 0 ± 0 | 1 ± 0.5 | 1.5 ± 0.6 | 2 ± 0.8 | 0 ± 0.8* |
| Small intestine | 0.5 ± 0.6 | 0.5 ± 1 | 0 ± 1 | 1.5 ± 1 | 1 ± 0.5 | 1 ± 1 |
| Skin | 0 ± 0.5 | 0 ± 0.8 | 2.5 ± 1.7 | 3.5 ± 3.3 | 4.5 ± 2.2 | 0 ± 1.6 |
| Ear | 0.5 ± 0.96 | 1 ± 1.2 | 4.5 ± 1 | 6.5 ± 3.5 | 5 ± 2.4 | 2 ± 2.1 |
| Tongue | 0 ± 0.58 | 0 ± 1 | 3.5 ± 1.9 | 4 ± 0.6 | 0 ± 1.7 | 0 ± 1.6 |
Shown are means ± SD of scores from each indicated group. Numbers of mice in each are given in parenthesis after the group name.
P < .05.
Histopathology and immunohistochemistry of intestine.
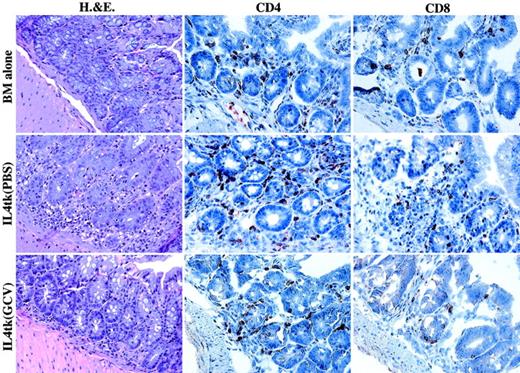
Tissue was prepared as described in “Materials and methods.” For immunohistochemistry, sections were stained with biotin-labeled rat monoclonal antibodies to either CD4 or CD8, followed by streptavidin-conjugated horseradish peroxidase and development with 3-AEC. Sections were counterstained with hematoxylin. Note on H&E-stained sections the massive inflammatory infiltration and isolated apoptotic cells in the IL-4-tk splenocyte recipient treated with PBS, which had GVHD. IL-4-tk splenocyte recipients treated with GCV and BM controls appeared normal. Immunohistochemistry revealed many more CD4+ and CD8+ cells in the IL-4-tk splenocyte recipient treated with PBS compared with a similar mouse treated with GCV or that received BM alone. Apparent magnification × 250.
Histopathology and immunohistochemistry of intestine.
Tissue was prepared as described in “Materials and methods.” For immunohistochemistry, sections were stained with biotin-labeled rat monoclonal antibodies to either CD4 or CD8, followed by streptavidin-conjugated horseradish peroxidase and development with 3-AEC. Sections were counterstained with hematoxylin. Note on H&E-stained sections the massive inflammatory infiltration and isolated apoptotic cells in the IL-4-tk splenocyte recipient treated with PBS, which had GVHD. IL-4-tk splenocyte recipients treated with GCV and BM controls appeared normal. Immunohistochemistry revealed many more CD4+ and CD8+ cells in the IL-4-tk splenocyte recipient treated with PBS compared with a similar mouse treated with GCV or that received BM alone. Apparent magnification × 250.
Figure 2 provides examples of the histology in IL-4-tk recipients. The mouse treated with PBS demonstrates multiple apoptotic cells in the epithelia as well as increased infiltrate in the lamina propria. In contrast, both BM-alone and the GCV-treated mice demonstrate relatively normal histologic pictures with few or no apoptotic cells and a sparse, normal content of lymphocytes in the lamina propria. Staining for CD4 and CD8 revealed the mixed nature of the infiltrate and increased numbers of cells in the PBS-treated mouse, consistent with the H&E staining. There are numerous intraepithelial CD4 and CD8 cells as well. In contrast, although there are CD4 and CD8 cells present in both the BM-alone and GCV-treated mice, they were fewer in number and were more rarely found in the epithelial layer, particularly for CD4 cells that are not normally detected in this location but are clearly present in the PBS-treated mouse.
Overall, we conclude that GCV treatment substantially ameliorated but did not eliminate histologic GVHD. Differences among organs were noted, but it is difficult to draw conclusions about their meaning given the relatively small numbers of mice that were evaluated. In addition, the clinical significance of these residual lesions is uncertain, as there is no way to determine whether they are active or represent residua of previously active lesions. Because GCV only kills dividing cells that express thymidine kinase, the lesions may have been visible histologically but may not have contained dividing cells. Nonetheless, this result suggests that actively dividing cells are critical to the maintenance of clinical disease.
GCV treatment restores naive, activated, and memory T-cell populations
Mice undergoing aGVHD demonstrate increases in CD44+ T cells, particularly of CD62Llo cells that include memory phenotype T cells.47 Concurrently, the fraction of naive, CD44lo/CD62Lhi cells is reduced. We therefore asked if treatment with GCV of aGVHD induced by IL-tk Tg T cells would correct these alterations in T-cell activation phenotype subsets. Indeed, GCV treatment normalized these subsets for both CD4 and CD8 T cells in both the IL-2-tk and IL-4-tk mice. The distribution of T cells in these subsets was the same in BM-alone controls as in GCV-treated mice (Table3), whereas in PBS-treated mice there was a lower frequency of naive T cells and most notably a higher proportion of memory-type CD44hi/CD62Llo cells. There was no effect of GCV on these subsets in Tg-negative mice (not shown). These data provide further objective evidence of the effect of GCV in reversing ongoing GVHD and are consistent with the effect occurring directly on T cells.
Effect of GCV treatment on T-cell subsets in spleen
| Cell population . | Experiment A . | Experiment B . | ||||||
|---|---|---|---|---|---|---|---|---|
| BM . | IL-2-tk . | BM . | IL-4-tk . | |||||
| PBS . | GCV . | PBS . | GCV . | PBS . | GCV . | PBS . | GCV . | |
| CD4 | ||||||||
| Naive | 29 ± 5.2 | 28 ± 3.3 | 19 ± 8.1 | 33 ± 6.73-150 | 32 ± 0.1 | 23 ± 3.5 | 10 ± 5.8 | 17 ± 9.3 |
| Activated | 19 ± 1.1 | 24 ± 2.2 | 9 ± 1.6 | 13 ± 2.23-150 | 26 ± 11 | 30 ± 7.4 | 27 ± 9.9 | 34 ± 6.7 |
| Memory | 40 ± 0.8 | 41 ± 2.5 | 63 ± 10.1 | 46 ± 6.63-150 | 34 ± 5.4 | 41 ± 0.2 | 59 ± 9.2 | 44 ± 7.83-151 |
| CD8 | ||||||||
| Naive | 8 ± 3.5 | 9 ± 4.5 | 8 ± 4.1 | 13 ± 4.13-152 | 20 ± 1.0 | 19 ± 3.4 | 4 ± 2.4 | 12 ± 5.83-152 |
| Activated | 28 ± 13 | 32 ± 10 | 21 ± 4.6 | 28 ± 6.83-152 | 37 ± 10 | 37 ± 8 | 22 ± 11.8 | 34 ± 8.03-152 |
| Memory | 50 ± 9.5 | 49 ± 12 | 60 ± 7.3 | 46 ± 7.63-150 | 27 ± 8.4 | 33 ± 1.8 | 61 ± 6.2 | 45 ± 8.03-151 |
| Cell population . | Experiment A . | Experiment B . | ||||||
|---|---|---|---|---|---|---|---|---|
| BM . | IL-2-tk . | BM . | IL-4-tk . | |||||
| PBS . | GCV . | PBS . | GCV . | PBS . | GCV . | PBS . | GCV . | |
| CD4 | ||||||||
| Naive | 29 ± 5.2 | 28 ± 3.3 | 19 ± 8.1 | 33 ± 6.73-150 | 32 ± 0.1 | 23 ± 3.5 | 10 ± 5.8 | 17 ± 9.3 |
| Activated | 19 ± 1.1 | 24 ± 2.2 | 9 ± 1.6 | 13 ± 2.23-150 | 26 ± 11 | 30 ± 7.4 | 27 ± 9.9 | 34 ± 6.7 |
| Memory | 40 ± 0.8 | 41 ± 2.5 | 63 ± 10.1 | 46 ± 6.63-150 | 34 ± 5.4 | 41 ± 0.2 | 59 ± 9.2 | 44 ± 7.83-151 |
| CD8 | ||||||||
| Naive | 8 ± 3.5 | 9 ± 4.5 | 8 ± 4.1 | 13 ± 4.13-152 | 20 ± 1.0 | 19 ± 3.4 | 4 ± 2.4 | 12 ± 5.83-152 |
| Activated | 28 ± 13 | 32 ± 10 | 21 ± 4.6 | 28 ± 6.83-152 | 37 ± 10 | 37 ± 8 | 22 ± 11.8 | 34 ± 8.03-152 |
| Memory | 50 ± 9.5 | 49 ± 12 | 60 ± 7.3 | 46 ± 7.63-150 | 27 ± 8.4 | 33 ± 1.8 | 61 ± 6.2 | 45 ± 8.03-151 |
Spleen cells from the indicated groups of mice (either BM alone or IL-tk transgenic T-cell recipients) treated with either PBS or GCV were recovered 4 weeks after treatment (6 weeks after transplantation) and analyzed by 4-color flow-activated cell sorter as described in “Materials and methods.” Cells were gated to analyze either CD4- (first 3 lines) or CD8- (last 3 lines) positive cells and then considered as naive (CD44lo/CD62hi), activated (CD44hi/CD62Lhi), or memory (CD44hi/CD62Llo) as described.44Shown are percentages ± SD. Experiment A used IL-2-tk donor T cells, and experiment B used IL-4-tk donor T cells. There was no difference among Tg− recipients treated with PBS or GCV, which were included in both experiments (not shown). Pvalues refer to comparisons between PBS- and GCV-treated groups receiving the same types of cells.
P < .001.
P < .01.
P < .05.
GCV treatment results in selective depletion of cytokine-secreting cells
Because treatment of mice that received IL-tk Tg T cells led to amelioration of disease, one might expect that, at least in some organs, there would be a discernible effect of GCV treatment on the frequency of cytokine-secreting cells. To search for this effect, we killed mice 1 week after pump implantation (day 21 after transplantation), a time when the effect of GCV on weight is noticeable (Figure 1 and data not shown) and also when there are substantial cytokine-secreting cells (J.L. and M.J.S., unpublished observations and Figure 3, 2001) in untreated mice. Indeed, in recipients of IL-2-tk T cells, treatment for 1 week with GCV led to a significant decrease in IL-2–secreting cells in both spleen (P = .03) and liver (P = .008), as detected by FACS. The frequencies of IFN-γ were also reduced in spleen (P = .019), but the frequency of IL-4–secreting cells was not significantly altered. Interestingly, in IL-4-tk T-cell recipients, the frequency of IL-4–secreting cells was significantly reduced by GCV treatment, but only in liver (P= .03) and not in spleen (P = .13, Figure 3). Treatment of IL-4-tk recipients with GCV did not affect IL-2– or IFN-γ–secreting cell frequencies in either organ. These data provide evidence that GCV does have a specific effect on the intended target cells and indicate that the independent effects of IL-4-tk and IL-2-tk inhibition do not work by cross-inhibition of the opposite cytokine. Because a proportion of IL-2–secreting cells also express IFN-γ, it is not unexpected that GCV treatment had a minor but significant effect on these cells in spleen. The frequencies of donor T cells and of cytokine-secreting donor T cells in mice receiving BM alone were substantially lower than in T-cell recipients for all cytokines in all tissues; their frequency was also unaffected by GCV treatment (data not shown).
Flow cytometric analysis of cytokine production by donor T cells in spleen and liver.
(A) Dot plots of intracellular cytokine staining from aGVHD mouse spleen and livers. Samples are gated on Thy1.2+ and EMA-negative (ie, live) cells. The percentage of positive cells is given in each quadrant. (B,C) Graphs show the means and SDs of the percentages of cytokine-positive cells as determined in A. (B) IL-2-tk spleen cell recipients treated with PBS (n = 10, solid bars) or GCV (n = 10, hatched bars) are compared. Notice that GCV treatment significantly decreased the percentage of IFN-γ–positive cells in the spleen and the percentage of IL-2–positive cells in both organs (P < .05, indicated by asterisk). However, no significant effect on IL-4–positive cells was observed. (C) Graphs show the significant decrease of IL-4–positive cells in the liver of IL-4-tk spleen cell recipients treated with GCV (n = 10) in comparison with the PBS group (n = 9). No other cytokine-positive population was affected in either organ.
Flow cytometric analysis of cytokine production by donor T cells in spleen and liver.
(A) Dot plots of intracellular cytokine staining from aGVHD mouse spleen and livers. Samples are gated on Thy1.2+ and EMA-negative (ie, live) cells. The percentage of positive cells is given in each quadrant. (B,C) Graphs show the means and SDs of the percentages of cytokine-positive cells as determined in A. (B) IL-2-tk spleen cell recipients treated with PBS (n = 10, solid bars) or GCV (n = 10, hatched bars) are compared. Notice that GCV treatment significantly decreased the percentage of IFN-γ–positive cells in the spleen and the percentage of IL-2–positive cells in both organs (P < .05, indicated by asterisk). However, no significant effect on IL-4–positive cells was observed. (C) Graphs show the significant decrease of IL-4–positive cells in the liver of IL-4-tk spleen cell recipients treated with GCV (n = 10) in comparison with the PBS group (n = 9). No other cytokine-positive population was affected in either organ.
GCV treatment does not impair donor engraftment of T cells
One potential drawback of GCV treatment in this setting is that it might lead to nonselective depletion of donor T cells. Unfortunately, congenic mice that would allow us to easily distinguish donor from recipient hematopoiesis are unavailable on these strains.48 Furthermore, in this model, engraftment of even T-cell–depleted BM is complete. Nevertheless, as B10.BR and AKR mice differ at the Thy1 allele, we were able to assess the development of donor-derived T cells via analysis of thymi and spleens (Table4) of GCV-treated GVHD mice. Thymi of GCV-treated spleen cell recipients were much more cellular than PBS-treated mice at day 42 (data not shown), consistent with the clinical amelioration of GVHD in GCV-treated animals. The majority of thymocytes in GCV-treated GVHD mice was donor derived and had the typical thymic distribution of CD4 and CD8 staining (data not shown), suggesting that T-cell progenitor and likely pluripotent hematopoietic stem cell engraftment occurred in GCV-treated mice, as also found by others.49 The hypocellular thymi of PBS-treated mice precluded meaningful comparison with GCV-treated mice, but GCV if anything facilitated engraftment rather than hindered it in the thymus. Spleens at this point were predominantly populated with donor-derived T cells as well in all groups of mice (Table 4). When animals were killed at day 21, after 1 week of GCV and at a time when thymi were hypocellular in all mice, the majority of splenic T cells was Thy1.2+ and therefore donor in origin as well (data not shown). In these groups, there were substantially higher frequencies of donor-derived T cells in mice receiving BM plus T cells than BM alone, again indicating that mature T cells also engraft quantitatively in the presence or absence of GCV treatment. Thus, GCV treatment did not lead to the elimination of all mature donor T cells, again in accord with the idea that we selectively ablated cytokine-producing cells (Figure 3).
Engraftment of donor T cells is not inhibited by GCV treatment
| Group . | n . | Thy1.1 (mean ± SD) . | Thy1.2 (mean ± SD) . |
|---|---|---|---|
| BM (GCV−) | 3 | 2.4 ± 1.2 | 23.4 ± 7 |
| BM (GCV+) | 2 | 4.5 ± 3.7 | 14.4 ± 5.0 |
| Tg−(GCV−) | 7 | 1.4 ± 1.3 | 10.4 ± 7.3 |
| Tg−(GCV+) | 2 | 0.7 ± 0.5 | 10.3 ± 10.8 |
| IL-2-tk (GCV−) | 2 | 0.7 ± 0.4 | 7.4 ± 5.8 |
| IL-2-tk (GCV+) | 4 | 2.1 ± 1.9 | 12.5 ± 6.5 |
| IL-4-tk (GCV−) | 2 | 3.4 ± 1.6 | 15.0 ± 0.23 |
| IL-4-tk (GCV+) | 4 | 2.4 ± 2.2 | 18.1 ± 5.1 |
| Group . | n . | Thy1.1 (mean ± SD) . | Thy1.2 (mean ± SD) . |
|---|---|---|---|
| BM (GCV−) | 3 | 2.4 ± 1.2 | 23.4 ± 7 |
| BM (GCV+) | 2 | 4.5 ± 3.7 | 14.4 ± 5.0 |
| Tg−(GCV−) | 7 | 1.4 ± 1.3 | 10.4 ± 7.3 |
| Tg−(GCV+) | 2 | 0.7 ± 0.5 | 10.3 ± 10.8 |
| IL-2-tk (GCV−) | 2 | 0.7 ± 0.4 | 7.4 ± 5.8 |
| IL-2-tk (GCV+) | 4 | 2.1 ± 1.9 | 12.5 ± 6.5 |
| IL-4-tk (GCV−) | 2 | 3.4 ± 1.6 | 15.0 ± 0.23 |
| IL-4-tk (GCV+) | 4 | 2.4 ± 2.2 | 18.1 ± 5.1 |
Spleen cells were stained with antibodies to recipient (Thy1.1) and donor (Thy1.2) Thy1 alleles and then analyzed by FACS. The percentage of donor and recipient cells among the total cell population is indicated, along with the number of mice analyzed. It is evident that GCV treatment did not adversely affect donor T-cell engraftment.
Discussion
These studies had 2 main goals: to test the hypothesis that aGVHD is a T1-mediated disease and to determine the feasibility of GCV treatment of established severe aGVHD in a murine miHA-matched model.
We addressed the first issue because cytokine polarization, which is known to control the phenotype of several autoimmune syndromes,50 could have important implications for the mechanism of GVH/L and its therapeutic manipulation. For example, polarization could explain the nature of lesions in various tissues and the differences between aGVHD and chronic GVHD.51 In addition, it has been proposed that control of polarization or selective inhibition of one T-cell cytokine subset may be a way to separate GVHD from GVL.3 51-54
We addressed the second goal, a model of suicide gene–based control of GVHD, in part because of its promising clinical utility.33 35 So far this has been demonstrated in only a limited way, and it is clear to us that animal models will be useful if not indispensable in truly understanding the mechanism of HSV-tk–based T-cell deletion and how it controls ongoing GVHD. To most closely mimic the clinical situation, we have used an MHC-matched, miHA-mismatched system and have administered GCV only after GVHD was well established.
Clinical disease as measured by weight gain and survival regressed in GCV-treated IL-2-tk and IL-4-tk recipients. This clinical improvement correlated with partial amelioration of histologic disease, reduction in the frequency of the specifically targeted cytokine-secreting cells, and a decrease in memory T-cell accumulation, consistent with GCV-induced death of activated, dividing, alloreactive donor T cells.
The significance of residual lesions and some residual cells expressing the “target” cytokine is difficult to assess. They could represent healing or inactive lesions. Alternatively, they could be the result of ongoing inflammation induced by (1) nondividing terminally differentiated T cells, (2) T cells no longer producing IL-4 or IL-2, or (3) processes that have become independent of the previously infused T cells. Finally, the lesions could be due to inefficiency in the GCV-mediated deletion of IL-tk T cells.
Regarding the second goal, our data demonstrate that in a MHC-matched model, established GVHD can be reversed by using GCV ablation of tk-expressing T cells. It is important to emphasize that the evidence for this in humans thus far is anecdotal, limited to a few patients in an uncontrolled trial.7,33 Although these human trials are promising and in fact a rationale for our work, the extensive experiments shown here establish the efficacy of the strategy in a controlled way and, perhaps more importantly, provide a model for further investigation. There have been a few other reports on the use of tk-Tg mice and GCV for GVHD inhibition. In all but one report, GCV was given at the time of transplantation or shortly thereafter, thus providing a prevention and not a treatment model.34,37,46In one case, GCV treatment was delayed.36 In that study, there was full MHC and miHA mismatch, a situation in which a very high frequency of both CD4 and CD8 cells is expected to be activated, unlike most human transplantations. It may be difficult to extrapolate this to the human miHA-mismatched or haplomismatched situation. Indeed, although some efficacy was shown in this full-mismatch model, mice remained symptomatic if GCV was delayed even until day 5 after transplantation, and, if delayed until 2 weeks, only partial protection was seen.
Our studies are also informative on the roles of T1 and T2 cells in aGVHD. This is a complex issue. It is well established that once a T-cell clone is polarized, progeny of that clone maintain the T1 or T2 phenotype of the parent slt.39,40,55,56 For this reason, we chose to treat our mice at day 14 when one would reasonably expect that most mature donor T cells that were going to both survive 14 days and see a recipient antigen strongly enough to contribute to GVHD would have been activated. Indeed, infiltrating T cells—which must include some effector cells—are present in GVHD lesions at day 1457 (J.L. and M.J.S., unpublished observations, 2001). Further, we see strong T-cell activation and few naive T cells in spleens from mice killed well before day 14 (not shown). Most importantly, we see strong T-cell polarization in both spleen and liver at day 21 (Figure 3). Although both Th1- and Th2-type T cells are present, Th2 cells are a minor population. Although GCV treatment did not completely ablate the target populations of T cells, it did have a significant effect without affecting the nontargeted population. It is not surprising that GCV did not have a complete ablative effect, as this effect may depend on whether the cells are cycling and how much of the cytokine is being expressed, among other factors. Taking these considerations together, we favor the interpretation that GCV-mediated ablation of IL-tk T cells in our GVHD model represents at least in part specific ablation of T1- and T2-type T cells, supporting roles for both in aGVHD. This is also in agreement with prior in vitro data using these Tg mice.38-40
In particular, the lack of effect of GCV treatment on IL-4–secreting cells in the IL-2-tk recipients argues against the possibility that manipulations designed to block either T1 or T2 cells are instead acting on T0 cells. Starting GCV treatment at day 14, when polarization has had enough time to occur, probably explains the specific effect. However, the issue of inhibiting T0 cells likely does apply in those strategies in which inhibition is constant from the beginning of allogeneic T-cell transfer, when a T0 phenotype would be expected among newly activated T cells.39,58 59
It is important to put our data in the context of other work on the role of cytokine subsets in GVHD.38-40 The concept that aGVHD is a T1-mediated syndrome (and chronic GVHD a T2-mediated syndrome) was initially proposed by Ferrara.9 They found that Th2-polarized cells do not cause GVHD and, in fact, inhibit it when cotransferred with Th1 T cells10,11 and that IL-11 was found to promote T2 polarization and to reduce GVHD.53,60 However, administration of IL-10, a cytokine that is sometimes associated with T2 responses, either did not prevent61 or else exacerbated62 aGVHD. IL-12, a cytokine associated with T1 polarization, has had variable effects on GVHD. During induction, neutralization of IL-12–inhibited GVHD in a P→F1 model,63 whereas administration of exogenous IL-12 also inhibited GVHD in a fully mismatched model.14 In this same system, IL-12 if given later can enhance GVHD by inducing host-derived IFN-γ.64 These results alone illustrate the complexity of the situation and how difficult it is to probe the system by cytokine administration or neutralization, which can have effects on multiple donor and host cell types and activate several downstream pathways.
More recently, using KO strategies, both Murphy et al22 and Nikolic et al16 provided evidence that Th2 cells could be important. T cells from IFN-γ KO mice, surprisingly, caused a more virulent aGVHD in a fully MHC-mismatched model, suggesting a protective effect of IFN-γ, a T1 cytokine. This finding had been demonstrated before by infusion, although again this must occur early because late infusion had the opposite effect.65 However, in a P→F1 model, the lack of donor T-cell IFN-γ modified disease and delayed mortality, demonstrating the dependence of the results on the particular model used.23 However, if donor T cells lack IL-4 in a fully mismatched or MHC-mismatched model, disease was moderately but significantly mitigated. However, these workers did not find that anti–IL-4 antibodies had the same effect.22Stat4 or Stat6 KO mice, which have defects in CD4 T-cell polarization toward Th1 or Th2 phenotypes, respectively, have also recently been used as T-cell donors, again in an MHC-mismatched system.16 Here, donor T cells from either KO had reduced capacity to cause disease, although those which could not evolve into T1 cells were much more impaired, suggesting a dominant role for T1 cells. Nevertheless, those that differentiated more toward T2 did produce disease that preferentially targeted skin and liver but not gut. Thus, this result demonstrated that either type of T cell could cause GVHD, albeit of somewhat different character.
GCV/HSV-tk ablation differs from other strategies of cytokine inhibition. In selective ablation, the T cells develop normally in the donor, whereas this may not be the case in KO mice. In the IL-tk system, after donor T-cell transfer to the recipient, disease evolves normally, including initial T-cell polarization, until the point at which GCV is given. This again might differ from the situation using KO T cells. Ideally, the ablative approach deletes cytokine-producing T cells and thus negates the effects of secreted cytokines as well as other cytotoxic mechanisms such as FasL, granzyme, and tumor necrosing factor α (TNF-α), all known to be important in GVHD.5,66 67 The latter effect might not be the case for both KO and anticytokine antibody approaches. Therefore, the interleukin-tk system adds a different dimension to the body of work that has addressed the issue of cytokine polarization in GVHD.
One curious aspect of our results is that both types of T cells seem obligatory for clinical disease. In other GVHD models, either T1 or both subsets were shown to contribute, but there was still residual disease when one or the other was inhibited.16,22,23 This finding could reflect a difference in models. We use MHC-matched strains, in which donor T-cell activation is not likely as widespread as the MHC-mismatched models. Thus, the contribution from each T-cell cytokine subset may be relatively more important. The relatively complete inhibition of clinical disease with ablation of either IL-2– or IL-4–producing T cells could also reflect a difference in the mechanism of inhibition, with T-cell deletion perhaps being more efficient and thus showing a stronger phenotype. It is also possible that the 2 cell types are synergistic. There is precedent for this, including asthma,68-70 autoimmune gastritis,71 immune responses,72 tumor models,73 and in vitro.74,75 Clinical GVHD may be a threshold phenomenon, as is likely the case with frank clinical autoimmunity.76 This would be consistent with residual histopathology we observed in clinically well-appearing animals.
That selective ablation of either T1 or T2 cells was enough to reverse clinical GVHD in this system, raises the possibility that GVHD could be treated while preserving some GVL. This is particularly tantalizing as the cytokine secretion data suggest that ablation in the 2 different settings are working at least in part via different mechanisms. Polarization as an approach to maintain GVL while treating GVHD has also been suggested by others.16,53,77 GVHD proceeds via multiple mechanisms, at least involving FasL, perforin/granzyme, TNF-α, macrophage activation by CD4 cells, and other systemic cytokine effects (eg, IL-1). At present we do not know the mechanisms for GVL, which could even vary by tumor, but which may be a subset of the above. For example, FasL could be an important mechanism and its expression is largely limited to Th1 cells.78 If this were the case, then Th2 inhibition might treat GVHD without hindering GVL. We plan to test this hypothesis by using a novel primary chronic myeloid leukemia model based on retroviral transformation of BM.79
We thank Ann Haberman for critical reading of the manuscript and Richard Flavell for donating the tk transgenic mice.
Supported by grant P50HL54516 from the National Institutes of Health. J.L. is a Leukemia and Lymphoma Society Postdoctoral Fellow. W.D.S. is supported by NIH grant K08-HL03979.
W.D.S. and M.J.S. are cosenior authors.
The publication costs of this article were defrayed in part by page charge payment. Therefore, and solely to indicate this fact, this article is hereby marked “advertisement” in accordance with 18 U.S.C. section 1734.
References
Author notes
Mark J. Shlomchik, Department of Laboratory Medicine, Rm CB465, Yale University School of Medicine, 333 Cedar St, Box 208035, New Haven, CT 06520-8035; e-mail: mark.shlomchik@yale.edu.


This feature is available to Subscribers Only
Sign In or Create an Account Close Modal