Key Points
Compared with TBI, IV-BU resulted in superior survival with no increased risk for relapse or TRM.
The results support the use of myeloablative IV-BU vs TBI-based conditioning regimens for treatment of myeloid malignancies.
Abstract
We conducted a prospective cohort study testing the noninferiority of survival of ablative intravenous busulfan (IV-BU) vs ablative total body irradiation (TBI)-based regimens in myeloid malignancies. A total of 1483 patients undergoing transplantation for myeloid malignancies (IV-BU, N = 1025; TBI, N = 458) were enrolled. Cohorts were similar with respect to age, gender, race, performance score, disease, and disease stage at transplantation. Most patients had acute myeloid leukemia (68% IV-BU, 78% TBI). Grafts were primarily peripheral blood (77%) from HLA-matched siblings (40%) or well-matched unrelated donors (48%). Two-year probabilities of survival (95% confidence interval [CI]), were 56% (95% CI, 53%-60%) and 48% (95% CI, 43%-54%, P = .019) for IV-BU (relative risk, 0.82; 95% CI, 0.68-0.98, P = .03) and TBI, respectively. Corresponding incidences of transplant-related mortality (TRM) were 18% (95% CI, 16%-21%) and 19% (95% CI, 15%-23%, P = .75) and disease progression were 34% (95% CI, 31%-37%) and 39% (95% CI, 34%-44%, P = .08). The incidence of hepatic veno-occlusive disease (VOD) was 5% for IV-BU and 1% with TBI (P < .001). There were no differences in progression-free survival and graft-versus-host disease. Compared with TBI, IV-BU resulted in superior survival with no increased risk for relapse or TRM. These results support the use of myeloablative IV-BU vs TBI-based conditioning regimens for treatment of myeloid malignancies.
Introduction
Cyclophosphamide (CY) combined with ablative doses of total body irradiation (TBI) or the oral alkylating agent busulfan (BU), have been the main conditioning regimens for allogeneic hematopoietic cell transplantation (HCT) for patients with myeloid malignancies.1,2 Limited randomized trials in the 1990s suggested that in some settings such as sibling donor transplants for acute myeloid leukemia (AML) in adults, TBI was superior with lower relapse rates and less nonrelapse mortality risks.3,4 For chronic myelogenous leukemia (CML) in the chronic phase, though, the 2 regimens provided similar outcomes.5
In the last decade, intravenous busulfan (IV-BU) has increasingly replaced oral BU in conditioning regimens for allogeneic HCT. IV-BU is associated with more predictable pharmacokinetics (PK) and, in some studies, has improved the tolerability of myeloablative BU/CY.6-8 The substitution of fludarabine (FLU) for CY has led to the development of the “reduced-toxicity” myeloablative FLU/BU-conditioning regimen. Other advances during the last several decades have also contributed to generally superior outcomes after allogeneic transplants.9 Despite its increasing use, no prospective studies have been performed comparing IV-BU vs TBI-based myeloablative HCT. We performed a large prospective cohort study to test the hypothesis that survival of patients receiving myeloablative IV-BU–based conditioning regimens before a related or volunteer unrelated donor allogeneic HCT for AML, myelodysplastic syndrome (MDS), or CML is not inferior to the recipients of ablative TBI-based regimens.
Methods
Study design
This study was a prospective multicenter cohort study comparing myeloablative IV-BU with TBI-based regimens in patients with myeloid malignancies undergoing matched related or unrelated donor blood or bone marrow transplants. Patients were prospectively enrolled through the Center for International Blood and Marrow Transplant Research (CIBMTR) data collection mechanism. The CIBMTR is a collaborative working group of more than 450 transplantation centers worldwide that contribute detailed data on consecutive HCT to a statistical center at the Medical College of Wisconsin in Milwaukee and the National Donor Program Coordinating Centers in Minneapolis, Minnesota.10 Observational studies conducted by the CIBMTR are performed in compliance with the Privacy Rule (HIPAA) as a Public Health Authority, and in compliance with all applicable federal regulations pertaining to the protection of human research participants as determined by continuous review of the Institutional Review Boards of the National Marrow Donor Program and the Medical College of Wisconsin since 1985.
CIBMTR transplantation centers from North and South America were invited to participate. Enrollment started March 2009, and data reporting from participating centers were screened for eligibility to enter the study cohort. Eligible patients were selected for comprehensive CIBMTR data reporting track plus additional study-specific data collection of practices related to IV-BU administration. Data reporting and enrollment were monitored monthly during the study period, and compliance with forms reported was greater than 95%.
Eligibility
Patients eligible for enrollment met the following criteria: i) age ≤60 years; ii) undergoing first allogeneic blood or bone marrow HCT; iii) HLA-matched related or volunteer unrelated donor; iv) diagnosis of AML, MDS, CML; v) graft-versus-host disease (GVHD) prophylaxis that included a calcineurin inhibitor (CNI); vi) consensus criteria ablative pretransplant conditioning regimen that was based either on IV-BU (>9 mg/kg) plus CY (≥60mg/kg) or FLU (≥80 mg/m2) or was based on TBI (≥500 cGY single fraction or ≥800 cGY fractionated) plus CY (≥60 mg/kg) or etoposide (≥30 mg/kg).11 Informed consent was obtained in accordance with the Declaration of Helsinki.
Study end points and definitions
The primary outcome was survival duration. Other outcomes included neutrophil and platelet recovery, progression-free survival (PFS), treatment-related mortality (TRM), relapse or progression, incidence of veno-occlusive disease/sinusoidal obstruction syndrome (VOD/SOS), incidence and severity of acute GVHD (aGVHD), incidence of chronic GVHD (cGVHD), incidence of interstitial pneumonitis (IPN), and incidence of severe renal toxicity requiring dialysis and cause of death.
Neutrophil recovery was defined as the first of 3 consecutive laboratory values obtained on different days with an absolute neutrophil count ≥0.5 × 109/L without growth factor support. Platelet recovery was defined as the first of 3 consecutive laboratory values obtained on different days with platelets ≥ 20 × 109/L without platelet transfusions for 7 days immediately preceding this date. TRM was defined as death from any cause without evidence of relapsed disease. Relapse was defined as reoccurrence of disease after a complete response. Among patients who presented with active disease at the time of transplant (advanced disease) if no complete remission was documented after HCT, the date of disease progression was input as day +1 posttransplant. For patients with leukemia in remission at the time of transplant, relapse was determined whether the disease was morphologically evident or if the treating physician elected to initiate treatment in the setting of cytogenetic or molecular relapse. For the purposes of the analysis, disease progression and relapse were considered as the same event. For PFS, patients were considered to experience failures at the time of relapse, progression, or death from any cause. For survival, the event was death from any cause. For unrelated donors, “well-matched” was defined as no known disparity between donor and recipient at HLA-A, B, C, and DRB1 (8/8), partially matched as 1 known or 1 likely disparity and mismatched as ≥2 disparities.12 Disease status was classified as early (patients in first complete remission or first chronic-phase CML, refractory anemia with or without ringed sideroblasts); intermediate (patients in second complete remission or higher, second chronic phase); and advanced (patients with active leukemia [relapse or primary induction failure], accelerated-phase or blast-crisis CML, or refractory anemia with excess blasts).
Statistical analysis
The primary objective of this cohort study was to test the noninferiority of survival between IV-BU and TBI-based myeloablative regimens. The targeted accrual was 1460 patients at an accrual rate of 730 patients per year. This sample size provided 80% power to detect a noninferiority threshold comparing overall mortality after IV-BU with TBI-based regimens on a hazard ratio (HR) scale of 1.26.
Patient, disease, and treatment characteristics were summarized by a conditioning regimen with continuous variables described by median and range and categorical variables described by frequency and percentage. Probabilities of survival and PFS were calculated using the Kaplan-Meier estimator.13 Probabilities of neutrophil and platelet recovery, aGVHD, cGVHD, TRM, and relapse were calculated using the cumulative incidence function to accommodate competing risks.13 For neutrophil and platelet recovery, aGVHD, and cGVHD, death without the event was considered the competing risk. For TRM, relapse was the competing event, and for relapse, TRM was the competing event. In all analyses, patients without an event were censored at last follow-up.
In multivariate analysis, the risk for overall morality (inverse of survival), treatment failure (inverse of relapse-free survival [RFS]), TRM, relapse, grade 3 to 4 acute GVHD, and cGVHD were compared between conditioning regimens using the Cox models.13 The proportional-hazard assumption was evaluated for all variables. The final models were stratified on disease type, donor type, and performance score that did not meet the proportionality assumption. Adjusted survival and RFS curves were generated based on the final Cox model using the method of Zhang et al.14 Multivariate Cox models were built using stepwise selection procedures with the conditioning regimen included in all steps of model building. All variables with a P value ≤.05 were included in the final models. Variables considered in the analysis include age (≤19 vs 20 – 49 vs ≥50), gender, race (Caucasian vs not Caucasian), performance score (<90 vs 90-100), comorbidity index (≤3 vs >3), disease status (AML early vs AML intermediate vs AML advanced vs CML early vs CML intermediate vs CML advanced vs MDS early vs MDS advanced), graft type (bone marrow vs peripheral blood), donor type (HLA-id sib vs matched unrelated vs partially matched unrelated), donor-recipient gender match (F-M vs M-F vs M-M vs F-F), donor-recipient cytomegalovirus (CMV) status (+/+, +/−, −/+, −/−), (GVHD prophylaxis (CNI + methotrexate [MTX] vs CNI + MTX + other vs CNI + mycophenolate mofetil (MMF) ± other vs CNI ± other (no MTX, MMF)), and antithymocyte globulin (ATG)/Campath (yes vs no). Interactions between the conditioning regimen and other covariates were tested for in all models. None was found to be statistically significant. All treatment effects were stated as HR with a 95% confidence interval (CI).
Post hoc comparison of 2-year survival probabilities between IV-BU and TBI-based regimens by disease and disease status was performed. An additional subset analysis within the IV-BU cohort comparing survival, RFS, TRM, and relapse between BU/CY vs FLU/BU was conducted using the Cox models. Patient, disease, and transplant characteristics were also compared across these 2 IV-BU–containing regimens. Analyses were done using SAS software version 9.1 (SAS, Cary, NC).
Results
Accrual
From March 2009 to February 2011, a total of 1483 eligible patients were enrolled from 120 transplantation centers (IV-BU, N = 1025 and TBI, N = 458).
Patient characteristics
Patient, donor, disease, and treatment characteristics are shown in Table1. The IV-BU and TBI groups were well balanced with respect to age (median age, 45 years), gender (50% women), race (88% Caucasian), performance status (68% in more than 90 patients), and comorbidities. Most patients had AML (68% BU and 78% TBI). The disease status was early (51%), intermediate (18%), and advanced (31%) and was similar in the cohorts. Transplants were performed primarily with peripheral blood grafts (77%) from either related (40%) or well-matched unrelated (48%) donors. Donor age, gender-matching, and donor-recipient CMV status were similar between the cohorts. For GVHD prophylaxis, the CNI was most commonly combined with short-course MTX (79%).
Demographic characteristics by conditioning regimen among patients with myeloid malignancies who received HCT with myeloablative conditioning from 2009 to 2011
| Characteristics of patients . | IV-BU . | TBI . |
|---|---|---|
| N = 1025 (%) . | N = 458 (%) . | |
| Number of centers | 104 | 79 |
| Geographic region | ||
| North America | 1020 (99) | 444 (97) |
| South America | 5 (<1) | 14 (3) |
| Age, median (range), years | 46 (<1-60) | 43 (1-60) |
| Gender | ||
| Male | 510 (50) | 238 (52) |
| Patient ethnicity | ||
| White | 906 (88) | 404 (88) |
| African American | 54 (5) | 19 (4) |
| Asian | 29 (3) | 12 (3) |
| Other | 36 (4) | 23 (5) |
| Performance score | ||
| Karnofsky: 90%-100% | 598 (66) | 277 (65) |
| Lansky: 90%-100% | 106 (91) | 29 (88) |
| HCI-CI | ||
| 0 | 400 (39) | 209 (46) |
| 1-2 | 302 (29) | 112 (24) |
| ≥3 | 323 (32) | 137 (30) |
| Disease and disease status | ||
| AML early | 415 (40) | 182 (40) |
| AML intermediate | 143 (14) | 82 (18) |
| AML advanced | 143 (14) | 95 (21) |
| CML early | 59 (6) | 24 (5) |
| CML intermediate | 21 (2) | 24 (5) |
| CML advanced | 28 (3) | 6 (1) |
| MDS early | 62 (6) | 11 (2) |
| MDS advanced | 151 (15) | 33 (7) |
| MDS NOS | 3 (<1) | 1 (<1) |
| Prior autologous transplant | 21 (2) | 11 (2) |
| Graft type | ||
| Bone marrow | 238 (23) | 110 (24) |
| Peripheral blood | 787 (77) | 348 (76) |
| Donor type | ||
| HLA-identical sibling | 417 (41) | 180 (39) |
| Well-matched unrelated | 479 (47) | 231 (50) |
| Partially matched unrelated | 115 (11) | 43 (9) |
| Mismatched | 2 (<1) | 2 (<1) |
| HLA match information missing unrelated | 12 (1) | 2 (<1) |
| D-R sex match | ||
| F-M | 194 (19) | 91 (20) |
| F-F | 204 (20) | 88 (19) |
| M-M | 316 (31) | 147 (32) |
| M-F | 311 (30) | 132 (29) |
| D-R CMV status | ||
| −/− | 301 (29) | 136 (30) |
| +/+ | 267 (26) | 117 (26) |
| +/− | 135 (13) | 58 (13) |
| −/+ | 321 (31) | 146 (32) |
| Missing | 1 (<1) | 1 (<1) |
| Conditioning regimen | ||
| FLU + BU | 289 (28) | 0 |
| FLU + BU + ATG/Campath | 135 (13) | 0 |
| BU + CY +/− others | 500 (49) | 0 |
| BU + CY +/− OTHERS + ATG/Campath | 101 (10) | 0 |
| CY + TBI +/− others | 0 | 396 (86) |
| CY + TBI +/− others + ATG/Campath | 0 | 47 (10) |
| Etoposide + TBI (No Cy) | 0 | 15 (3) |
| Total BU dose for patients who received IV BU, median (range), mg/kg | 13 (10-28) | — |
| BU schedule | — | |
| Every 6 h | 586 (57) | — |
| Daily | 427 (42) | — |
| Twice daily | 7 (<1) | — |
| Other schedule | 5 (<1) | — |
| PKs vs non-PKs | — | |
| No | 447 (44) | — |
| Yes | 578 (56) | — |
| BU dose-adjusted based on PK with a plan | — | |
| No | 122 (22) | — |
| Yes | 443 (78) | — |
| Fractionated TBI | ||
| No | — | 21 (5) |
| Yes | — | 437 (95) |
| TBI dose median (range) cGy | ||
| Unfractionated | — | 550 (550-900) |
| Fractionated | — | 1200 (990-1440) |
| BU dose if no PK, median (range), mg/kg* | 13 (10-17) | — |
| BU dose if PK, median (range), mg/kg† | 14 (10-27) | |
| GVHD prophylaxis | ||
| Tacro+MTX+/− other | 645 (63) | 322 (70) |
| Tacro+MMF+/− other | 133 (13) | 20 (4) |
| CSA+MTX+/− other | 146 (14) | 74 (16) |
| CSA+MMF+/− other | 30 (3) | 9 (2) |
| CSA or Tacro +/− other | 71 (7) | 33 (7) |
| ATG/Campath | ||
| CNI-based +ATG/Campath | 297 (29) | 65 (14) |
| Median follow-up of survivors, range, months | 22 (3-36) | 23 (8-37) |
| Characteristics of patients . | IV-BU . | TBI . |
|---|---|---|
| N = 1025 (%) . | N = 458 (%) . | |
| Number of centers | 104 | 79 |
| Geographic region | ||
| North America | 1020 (99) | 444 (97) |
| South America | 5 (<1) | 14 (3) |
| Age, median (range), years | 46 (<1-60) | 43 (1-60) |
| Gender | ||
| Male | 510 (50) | 238 (52) |
| Patient ethnicity | ||
| White | 906 (88) | 404 (88) |
| African American | 54 (5) | 19 (4) |
| Asian | 29 (3) | 12 (3) |
| Other | 36 (4) | 23 (5) |
| Performance score | ||
| Karnofsky: 90%-100% | 598 (66) | 277 (65) |
| Lansky: 90%-100% | 106 (91) | 29 (88) |
| HCI-CI | ||
| 0 | 400 (39) | 209 (46) |
| 1-2 | 302 (29) | 112 (24) |
| ≥3 | 323 (32) | 137 (30) |
| Disease and disease status | ||
| AML early | 415 (40) | 182 (40) |
| AML intermediate | 143 (14) | 82 (18) |
| AML advanced | 143 (14) | 95 (21) |
| CML early | 59 (6) | 24 (5) |
| CML intermediate | 21 (2) | 24 (5) |
| CML advanced | 28 (3) | 6 (1) |
| MDS early | 62 (6) | 11 (2) |
| MDS advanced | 151 (15) | 33 (7) |
| MDS NOS | 3 (<1) | 1 (<1) |
| Prior autologous transplant | 21 (2) | 11 (2) |
| Graft type | ||
| Bone marrow | 238 (23) | 110 (24) |
| Peripheral blood | 787 (77) | 348 (76) |
| Donor type | ||
| HLA-identical sibling | 417 (41) | 180 (39) |
| Well-matched unrelated | 479 (47) | 231 (50) |
| Partially matched unrelated | 115 (11) | 43 (9) |
| Mismatched | 2 (<1) | 2 (<1) |
| HLA match information missing unrelated | 12 (1) | 2 (<1) |
| D-R sex match | ||
| F-M | 194 (19) | 91 (20) |
| F-F | 204 (20) | 88 (19) |
| M-M | 316 (31) | 147 (32) |
| M-F | 311 (30) | 132 (29) |
| D-R CMV status | ||
| −/− | 301 (29) | 136 (30) |
| +/+ | 267 (26) | 117 (26) |
| +/− | 135 (13) | 58 (13) |
| −/+ | 321 (31) | 146 (32) |
| Missing | 1 (<1) | 1 (<1) |
| Conditioning regimen | ||
| FLU + BU | 289 (28) | 0 |
| FLU + BU + ATG/Campath | 135 (13) | 0 |
| BU + CY +/− others | 500 (49) | 0 |
| BU + CY +/− OTHERS + ATG/Campath | 101 (10) | 0 |
| CY + TBI +/− others | 0 | 396 (86) |
| CY + TBI +/− others + ATG/Campath | 0 | 47 (10) |
| Etoposide + TBI (No Cy) | 0 | 15 (3) |
| Total BU dose for patients who received IV BU, median (range), mg/kg | 13 (10-28) | — |
| BU schedule | — | |
| Every 6 h | 586 (57) | — |
| Daily | 427 (42) | — |
| Twice daily | 7 (<1) | — |
| Other schedule | 5 (<1) | — |
| PKs vs non-PKs | — | |
| No | 447 (44) | — |
| Yes | 578 (56) | — |
| BU dose-adjusted based on PK with a plan | — | |
| No | 122 (22) | — |
| Yes | 443 (78) | — |
| Fractionated TBI | ||
| No | — | 21 (5) |
| Yes | — | 437 (95) |
| TBI dose median (range) cGy | ||
| Unfractionated | — | 550 (550-900) |
| Fractionated | — | 1200 (990-1440) |
| BU dose if no PK, median (range), mg/kg* | 13 (10-17) | — |
| BU dose if PK, median (range), mg/kg† | 14 (10-27) | |
| GVHD prophylaxis | ||
| Tacro+MTX+/− other | 645 (63) | 322 (70) |
| Tacro+MMF+/− other | 133 (13) | 20 (4) |
| CSA+MTX+/− other | 146 (14) | 74 (16) |
| CSA+MMF+/− other | 30 (3) | 9 (2) |
| CSA or Tacro +/− other | 71 (7) | 33 (7) |
| ATG/Campath | ||
| CNI-based +ATG/Campath | 297 (29) | 65 (14) |
| Median follow-up of survivors, range, months | 22 (3-36) | 23 (8-37) |
ALL, acute lymphoblastic leukemia; CSA, cyclosporine A; Tacro, tacrolimus.
Higher doses were in pediatric patients.
Higher doses were in a dose-escalated trial at a single center.
IV-BU was most commonly given in combination with CY (59%). Dosing of BU was more often 4 times a day with CY (82%) and more commonly once a day with FLU (78%). ATG or Campath was used as part of the conditioning regimen or GVHD prophylaxis in 33% of patients in the IV-BU group and in 17% of patients in the TBI group. BU PK was performed in 56% of patients; in 78%, PK resulted in dose adjustment. PK testing was most commonly performed with a BU dosing of 4 times per day (63%). Of 103 centers that used IV-BU regimens, 54 centers performed PK in all patients, 26 centers performed PK in selected patients, and 23 centers never performed PK.
Survival duration
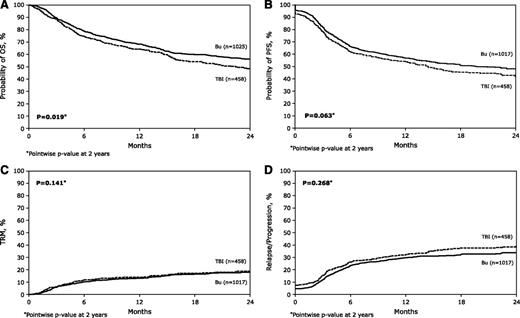
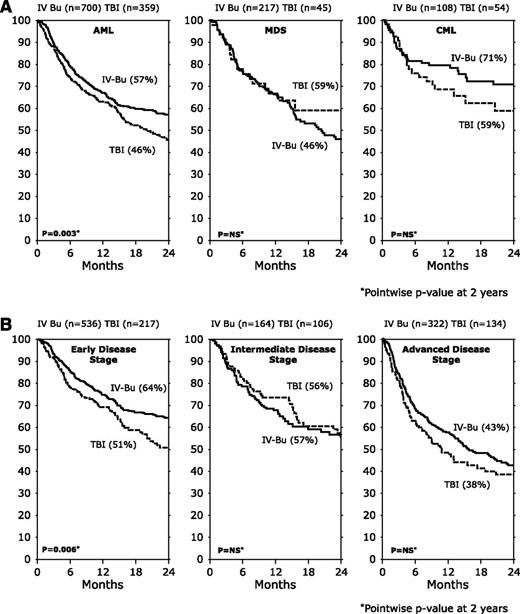
The 2-year probabilities of survival were 56% (95% CI, 53%-60%) and 48% (95% CI, 43%-54%) for IV-BU and TBI-based regimens, respectively (P = .019) (Figure 1A). Survival curves according to diagnosis and disease status are shown in Figure 2A-B, respectively. For patients with AML patients, the 2-year survival rate was 57% (95% CI, 53%-61%) and 46% (95% CI, 40%-52%) in the IV-BU and TBI-based regimens, respectively (P = .003). Two-year survival duration was not different for patients with MDS or CML based on conditioning. For patients with early disease, the 2-year survival rate was 64% (95% CI, 59%-69%) and 51% (95% CI, 42%-59%) for IV-BU and TBI-based regimens, respectively (P = .006). Survival duration was not different for patients with intermediate or advanced disease based on conditioning regimen. In multivariate analysis, IV-BU–based conditioning was associated with a decreased risk for death (HR, 0.82; 95% CI, 0.68-0.98; P = .03) compared with TBI-based conditioning. In addition to conditioning, other factors associated with an increased risk for death included older age, race other than Caucasian, and a HCT comorbidity index score >3 (Table 2).
Outcomes of allogeneic HCT with IV-BU or TBI conditioning regimens. (A) Survival by conditioning regimens. (B) Progression free survival by conditioning regimens. (C) Cumulative incidence of TRM by conditioning regimens. (D) Cumulative incidence of disease relapse by conditioning regimens.
Outcomes of allogeneic HCT with IV-BU or TBI conditioning regimens. (A) Survival by conditioning regimens. (B) Progression free survival by conditioning regimens. (C) Cumulative incidence of TRM by conditioning regimens. (D) Cumulative incidence of disease relapse by conditioning regimens.
Survival after allogeneic HCT with IV-BU or TBI conditioning stratified on diagnosis and disease status. (A) Survival by diagnosis and conditioning regimens. (B) Survival by disease status and conditioning regimens
Survival after allogeneic HCT with IV-BU or TBI conditioning stratified on diagnosis and disease status. (A) Survival by diagnosis and conditioning regimens. (B) Survival by disease status and conditioning regimens
Multivariate analysis comparing intravenous formulation busulfan to TBI-based myeloablative conditioning regimens before HCT for myeloid malignancies
| Overall mortality* . | Level . | N . | HR (95% CI) . | P value . |
|---|---|---|---|---|
| Conditioning regimen | TBI | 446 | 1 | |
| IV-BU | 993 | 0.819 (0.683-0.981) | .0302 | |
| Patient age (y) | ≤19 | 199 | 1 | .0008† |
| 20-49 | 704 | 1.347 (0.989-1.836) | .0592 | |
| ≥50 | 536 | 1.727 (1.258-2.371) | .0007 | |
| Race | White | 1278 | 1 | |
| Other | 161 | 1.409 (1.084-1.831) | .0104 | |
| HCT CI | ≤3 | 1186 | 1 | |
| >3 | 253 | 1.417 (1.153-1.743) | .0009 | |
| TRM* | ||||
| Conditioning regimen | TBI | 446 | 1 | |
| IV-BU | 988 | 0.800 (0.596-1.075) | .1395 | |
| Patient age, years | ≤19 | 198 | 1 | .0167† |
| 20-49 | 701 | 1.309 (0.810-2.114) | .2710 | |
| ≥50 | 532 | 1.829 (1.123-2.979) | .0153 | |
| Race | White | 1271 | 1 | |
| Other | 160 | 1.719 (1.158-2.551) | .0072 | |
| Disease relapse* | ||||
| Conditioning regimen | TBI | 446 | 1 | |
| IV-BU | 988 | 0.933 (0.766-1.137) | .4940 | |
| HCT CI | ≤3 | 1179 | 1 | |
| >3 | 252 | 1.329 (1.050-1.683) | .0180 | |
| Treatment failure*‡ | ||||
| Conditioning regimen | TBI | 446 | 1 | |
| IV-BU | 985 | 0.894 (0.759-1.053) | .1795 | |
| HCT CI | ≤3 | 1179 | 1 | |
| >3 | 252 | 1.354 (1.119-1.638) | .0018 |
| Overall mortality* . | Level . | N . | HR (95% CI) . | P value . |
|---|---|---|---|---|
| Conditioning regimen | TBI | 446 | 1 | |
| IV-BU | 993 | 0.819 (0.683-0.981) | .0302 | |
| Patient age (y) | ≤19 | 199 | 1 | .0008† |
| 20-49 | 704 | 1.347 (0.989-1.836) | .0592 | |
| ≥50 | 536 | 1.727 (1.258-2.371) | .0007 | |
| Race | White | 1278 | 1 | |
| Other | 161 | 1.409 (1.084-1.831) | .0104 | |
| HCT CI | ≤3 | 1186 | 1 | |
| >3 | 253 | 1.417 (1.153-1.743) | .0009 | |
| TRM* | ||||
| Conditioning regimen | TBI | 446 | 1 | |
| IV-BU | 988 | 0.800 (0.596-1.075) | .1395 | |
| Patient age, years | ≤19 | 198 | 1 | .0167† |
| 20-49 | 701 | 1.309 (0.810-2.114) | .2710 | |
| ≥50 | 532 | 1.829 (1.123-2.979) | .0153 | |
| Race | White | 1271 | 1 | |
| Other | 160 | 1.719 (1.158-2.551) | .0072 | |
| Disease relapse* | ||||
| Conditioning regimen | TBI | 446 | 1 | |
| IV-BU | 988 | 0.933 (0.766-1.137) | .4940 | |
| HCT CI | ≤3 | 1179 | 1 | |
| >3 | 252 | 1.329 (1.050-1.683) | .0180 | |
| Treatment failure*‡ | ||||
| Conditioning regimen | TBI | 446 | 1 | |
| IV-BU | 985 | 0.894 (0.759-1.053) | .1795 | |
| HCT CI | ≤3 | 1179 | 1 | |
| >3 | 252 | 1.354 (1.119-1.638) | .0018 |
Model stratified by disease status (AML early vs AML intermediate vs AML advanced vs CML early vs CML intermediate vs CML advanced vs MDS early vs MDS advanced), donor type (HLA-id sib vs well-matched unrelated vs partially matched unrelated), and performance score (<90% vs ≥90%).
Overall P value.
Treatment failure is 1/relapse-free survival; events are death or disease relapse.
PFS
Two-year probabilities of PFS were 48% (95% CI, 45%-51%) and 42% (95% CI, 37-47) for IV-BU and TBI-based regimens, respectively (P = .063) (Figure 1B).
In multivariate analysis of treatment failure, IV-BU was equivalent to the TBI-based regimen (Table 2).
Engraftment
The cumulative incidence of neutrophil recovery at day 28 were 96% (95% CI, 95%-97%) and 93% (95% CI, 90%-95%) for IV-BU and TBI-based regimens, respectively (P = .01). Corresponding cumulative incidences for platelet recovery at day 28 were 76% (95% CI, 74%-79%) and 73% (95% CI, 69%-77%), respectively (P = .147).
Toxicities and TRM
The 100-day cumulative incidences for VOD/SOS were 5% (95% CI, 4%-6%) and 1% (95% CI, 0%-3%; P < .001); for IPN, 4% (95% CI, 2%-5%) and 6% (95% CI, 4%-8%; P = .055); and for renal failure requiring dialysis, 6% (95% CI, 4%-7%) and 7% (95% CI, 5%-10%; P = .243) for IV-BU and TBI-based regimens, respectively.
Corresponding 2-year cumulative incidences of TRM were 18% (95% CI, 16%-21%) and 19% (95% CI, 15%-23%; P = .75), respectively (Figure 1C).
In multivariate analysis for TRM, IV-BU was similar to TBI-based regimens (Table 2).
GVHD
The 100-day cumulative incidences of grades 2 to 4 acute GVHD were 46% (95% CI, 43%-49%) and 51% (95% CI, 46%-55%; P = .128), and grades 3 to 4 acute GVHD were 18% (95% CI, 16%-21%) and 23% (95% CI, 19%-27%; P = .052) for IV-BU and TBI-based regimens, respectively. Corresponding 1-year cumulative incidences of cGVHD were 44% (95% CI, 41%-47%) and 42% (95% CI, 37%-46%; P = .397), respectively. Multivariate analysis shows no treatment effect on grade 3 to 4 acute GVHD (0.81; 95% CI, 0.63-1.05; P = .11) and no treatment effect on cGVHD (HR, 1.07; 95% CI, 0.90-1.29; P = .44). Additional variables associated with GVHD outcomes are shown in supplemental Tables 1 and 2.
Disease relapse/progression
The 2-year cumulative incidences of disease relapse/progression were 34% (95% CI, 31%-37%) and 39% (95% CI, 34%-44%; P = .084) for IV-BU and TBI-based regimens, respectively (Figure 1D).
In multivariate analysis for disease relapse, IV-BU was equivalent to the TBI-based regimen (Table 2).
Causes of death
Causes of death as reported by the transplant center were similar in the 2 cohorts and are outlined in Table 3.
Causes of death by conditioning regimens
| Description . | IV-BU . | TBI . |
|---|---|---|
| N = 400 (%) . | N = 207 (%) . | |
| Primary disease | 197 (49) | 107 (52) |
| GVHD | 56 (14) | 22 (11) |
| Infection | 62 (16) | 27 (13) |
| Organ failure | ||
| Lung (IPS/ARDS) | 23 (6) | 18 (9) |
| Liver | 4 (1) | 0 |
| Renal | 4 (1) | 2 (<1) |
| Other/multiple | 18 (5) | 11 (5) |
| Thromboembolic/hemorrhage | 2 (<1) | 2 (<1) |
| Graft failure | 5 (1) | 3 (1) |
| Second primary malignancy | 1 (<1) | 1 (<1) |
| Other causes | 28 (8) | 14 (6) |
| Description . | IV-BU . | TBI . |
|---|---|---|
| N = 400 (%) . | N = 207 (%) . | |
| Primary disease | 197 (49) | 107 (52) |
| GVHD | 56 (14) | 22 (11) |
| Infection | 62 (16) | 27 (13) |
| Organ failure | ||
| Lung (IPS/ARDS) | 23 (6) | 18 (9) |
| Liver | 4 (1) | 0 |
| Renal | 4 (1) | 2 (<1) |
| Other/multiple | 18 (5) | 11 (5) |
| Thromboembolic/hemorrhage | 2 (<1) | 2 (<1) |
| Graft failure | 5 (1) | 3 (1) |
| Second primary malignancy | 1 (<1) | 1 (<1) |
| Other causes | 28 (8) | 14 (6) |
ARDS, adult respiratory distress syndrome; IPS, idiopathic pneumonia syndrome.
BU/CY vs FLU/BU
There were some differences between the patients conditioned with BU/CY and FLU/BU. Patients receiving BU/CY were younger, with 22% of these patients being younger than 20 years vs 6% for patients receiving FLU/BU. Patients undergoing BU/CY also had a greater proportion with a performance score of 90 to 100 and an HCT comorbidity index score of 0 to 3. Patients receiving BU/CY more commonly received a bone marrow graft. IV-BU was administered every 6 hours in 82% of recipients of BU/CY vs daily in 78% of recipients of FLU/BU (supplemental Table 3). Despite these differences, in multivariate analysis, study outcomes did not differ between patients receiving BU/CY-based vs FLU/BU-based conditioning, including overall mortality (HR, 0.95; P = .63), treatment failure (HR, 1.02; P = .81), relapse (HR, 0.96; P = .75), and TRM (HR, 1.14; P = .44). In addition, the incidence of VOD was not different between the BU/CY and FLU/BU cohorts (5% vs 4%; P = .53)
Discussion
The practice of HCT is in continual evolution as new therapies are developed, evaluated, and reported in the literature. Although it is not feasible to test every development in prospective trials, it is problematic to apply results of outdated studies to current practice. The last randomized trial comparing CYTBI with BU/CY was reported more than 15 years ago. Since then, numerous changes have been introduced and general transplant results have improved for almost all patient groups.9,10,15 More has also been learned regarding the late effects of transplant conditioning.16-18 A gradual decrease in ablative TBI-based transplants and an increase in IV-BU–based transplants have occurred without supportive prospective data comparing the approaches.
Although a randomized controlled trial is the reference standard for comparing treatments, such a trial was considered unlikely to accrue based on physician bias and competition for limited resources. Instead, using the data collection capabilities of the CIBMTR, we conducted a large prospective cohort study with strict eligibility and reporting requirements and adjusted for differences between the groups using standard multivariable statistical methods.
Our study was designed to test, in the modern era, the noninferiority of IV-BU–based vs TBI-based myeloablative conditioning for allogeneic transplantation. We included several common BU-based and TBI-based regimens in the 2 cohorts; of note, there were not significant outcome differences between the regimens in each group. Specifically, our hypothesis was that IV-BU–based conditioning does not lead to inferior survival compared with TBI-based conditioning for patients with AML, MDS, and CML receiving related or volunteer unrelated donor grafts. The results strongly support this hypothesis. The data actually suggest a possible advantage to using IV-BU in this patient population. This advantage was most evident in patients with early-stage disease and AML.
Among IV-BU–containing regimens, some studies suggest that FLU/BU results in lower regimen-related toxicity compared with BU/CY.19-22 Results from a recently reported prospective randomized trial found similar nonrelapse mortality rates but improved survival outcomes with BU/CY compared with FLU/BU.23 The current study demonstrated that FLU/BU most commonly used IV-BU once daily, and it was administered to older patients and a higher proportion of patients with a lower performance score or a higher HCT comorbidity index. Despite these differences in the populations, the outcomes between FLU/BU and BU/CY were similar. Thus, this subset analysis supports that the 2 most commonly used non-TBI regimens are equivalent, despite differences in practices on when they are generally selected.
Adverse outcomes were similar with IV-BU–based and TBI-based approaches with slightly lower rates of TRM and relapse with IV-BU, although they did not reach statistical significance. There was a higher incidence of VOD/SOS with IV-BU. Other toxicities including IPN, the need for dialysis by 1 year posttransplant, cGVHD, and causes of death were remarkably similar in the 2 cohorts. The multivariate analyses on severe acute GVHD (grades 3-4) and cGVHD showed no benefit for IV-BU.
ATG/Campath was more commonly included with the FLU/BU regimens as developed by Russell et al.20 The use of ATG/Campath did not significantly affect survival or relapse outcomes. However, in the GVHD multivariate models, the use of ATG/Campath was associated with lower rates of acute and cGVHD (supplemental Tables 1 and 2). Unfortunately, we do not have the details of IV-BU dose adjustments for patients undergoing PK testing. Toxicity and TRM are known to be increased in patients with high levels of BU, whereas relapse and graft rejection increase with low levels.24-26
Prospective cohort studies are capable of accruing large number of patients and of measuring outcomes of contemporary transplant practices. Approximately 80% of patients undergoing transplantation in the United States who met eligibility criteria for the study during the accrual period were enrolled on this trial, providing an evaluation of these treatment approaches in the real world. In addition, data completeness approaching 100% through active monitoring outlines a novel and robust application of the CIBMTR infrastructure and outcomes database to address transplantation questions. These feature of a prospective cohort study address some of the pitfalls often assailed against retrospective cohort studies, particularly retrospective eligibility determination, data accuracy, and completeness. Although the issue of treatment assignment vs random selection will always remain for cohort studies, in this study, the similarities between the treatment groups and the ability to perform a robust statistical analysis because of the large sample size mitigate these concerns. Furthermore, it is unlikely that a randomized controlled trial of TBI-based vs IV-BU–based conditioning will ever be performed; we must work with the tools at hand.
For patients meeting the eligibility and practice approach of this study, IV-BU–based conditioning was not inferior to TBI-based conditioning. This information is helpful to clinicians for choosing conditioning regimens and counseling patients. The results went further to suggest that IV-BU resulted in a small but significant improvement in survival duration. The role of BU PK as part of such an approach requires further study. Future studies are required to understand the mechanism by which IV-BU–based regimens resulted in superior survival outcomes for patients with early-stage disease and AML in our study.
The online version of this article contains a data supplement.
There is an Inside Blood commentary on this article in this issue.
The publication costs of this article were defrayed in part by page charge payment. Therefore, and solely to indicate this fact, this article is hereby marked “advertisement” in accordance with 18 USC section 1734.
Acknowledgments
The authors are thankful for the support by Otsuka Pharmaceutical Development and Commercialization, Inc, and for the participation of 120 centers in North and South America.
The CIBMTR is supported by Public Health Service Grant/Cooperative Agreement U24 CA076518 from the National Institutes of Health National Cancer Institute (NCI); the National Heart, Lung, and Blood Institute (NHLBI); and the National Institute of Allergy and Infectious Diseases; Grant/Cooperative Agreement U10 HL069294 from NHLBI and NCI; contract HHSH250201200016C with the Health Resources and Services Administration/US Department of Health and Human Services; grants N00014-12-1-0142 and N00014-13-1-0039 from the Office of Naval Research; and grants from Allos Therapeutics, Inc; Amgen, Inc; Anonymous donation to the Medical College of Wisconsin; Ariad; Be the Match Foundation; Blue Cross and Blue Shield Association; Celgene Corporation; Fresenius-Biotech North America, Inc; Gamida Cell Teva Joint Venture Ltd; Genentech, Inc; Gentium SpA; Genzyme Corporation; GlaxoSmithKline; HistoGenetics, Inc; Kiadis Pharma; The Leukemia & Lymphoma Society; The Medical College of Wisconsin; Merck & Co, Inc; Millennium: The Takeda Oncology Co; Milliman USA, Inc; Miltenyi Biotec, Inc; National Marrow Donor Program; Onyx Pharmaceuticals; Optum Healthcare Solutions, Inc; Osiris Therapeutics, Inc; Otsuka America Pharmaceutical, Inc; Remedy Informatics; Sanofi US; Seattle Genetics; Sigma-τ Pharmaceuticals; Soligenix, Inc; StemCyte, A Global Cord Blood Therapeutics Co; Stemsoft Software, Inc; Swedish Orphan Biovitrum; Tarix Pharmaceuticals; TerumoBCT; Teva Neuroscience, Inc; THERAKOS, Inc; and Wellpoint, Inc. The views expressed in this article do not reflect the official policy or position of the National Institutes of Health, the Department of the Navy, the Department of Defense, or any other agency of the US Government.
Authorship
Contribution: C.B., K.K, and M.C.P. designed the study, analyzed results, and wrote the manuscript; J.L. and X.Z. provided the statistical support; and J.F.D., E.A., S.M.D., F.R.A., M.R.T., G.G.L., P.L.M., V.T.H., K.R.C., E.A., A.S., J.D.R., and J.M.B. interpreted data and critically reviewed the manuscript. All authors approved the final manuscript.
Conflict-of-interest disclosure: Independent research funding was provided to the CIBMTR from study sponsor (Otsuka Pharmaceutical Development and Commercialization, Inc) to conduct study. All data collection analyses and interpretation are independent of sponsor influence.
Correspondence: Christopher Bredeson, Blood Disease Centre, L2265b, 501 Smyth Road, Ottawa, ON, Canada, K1H 8L6; e-mail: cbredeson@ohri.ca.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal