Abstract
Abstract 4476
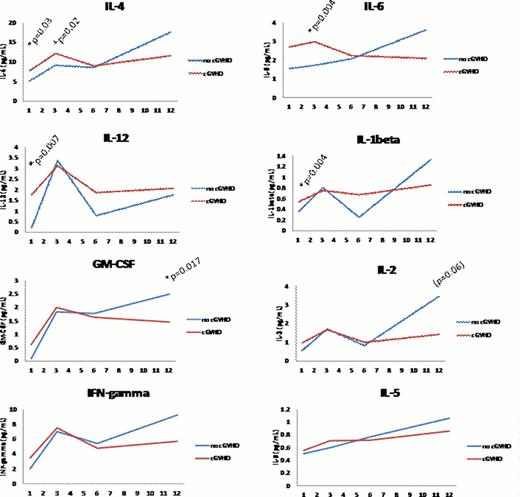
Chronic graft-versus-host disease (cGVHD) is a serious and frequent complication of allogeneic hematopoietic stem cell transplantation (HSCT). It is not known why some patients develop cGVHD and others do not, but identifying predictive biomarkers would facilitate the development of pre-emptive therapeutic strategies. Investigation into the pathophysiology of cGVHD has revealed different patterns of immune reconstitution in patients who develop cGVHD following HSCT. This suggests that the development of cGVHD occurs as a result of altered immune homeostasis and the inability to establish B and T cell tolerance. We prospectively examined 88 patients with hematologic malignancies following allogeneic HSCT at the Brigham and Woman's Hospital/Dana-Farber Cancer Institute between the years 2004 and 2008 and measured plasma cytokines known to modulate effector T cell, regulatory T cell, and B cell homeostasis and function. Seventy-six patients (86%) received reduced intensity conditioning; 84 (95%) received filgrastim-mobilized peripheral blood stem cells. Median follow-up for all patients was 5 years (range 2.9 to 7.3 years). Fifty-nine percent developed cGVHD. Plasma samples were collected at 1, 3, 6, and 12 months after HSCT and multiplex Luminex bead assays were used to measure levels of the following cytokines: Interferon-γ, IL-2, IL-7, IL-1β, IL-12, TNFα, IL-4, IL-5, IL-6, IL-10, and GM-CSF. Cytokine levels in patients who developed cGVHD were compared to patients who did not develop cGVHD. Results are shown in figure 1. Significantly higher levels of IL-4, IL-6, IL-12, and IL-1β were observed at 1 and/or 3 months after transplantation in patients who subsequently developed cGVHD. IL-4 and IL-6 are characteristic of T-helper-2 (TH2) cellular and humoral immune responses previously associated with cGVHD and fibrogenesis. IL-12 and IL-1β have heterogeneous functions including stimulating interferon-γ and TNFα production, enhancing cytotoxic and helper T cells, and promotion of autoimmunity. IL-1α also stimulates IL-6 production and activates fibroblasts. Finally, GM-CSF was significantly elevated in patients who do not develop cGVHD at 1 year following HSCT (2.5 v 1.46 pg/mL, p=0.017). As shown in figure 1, we observed a general pattern for many cytokines, including IFNγ, IL-2, IL-4, IL-5, IL-6, and IL-1β, in which these cytokines are initially similar in both groups, or lower in patients without cGVHD, but gradually increase over time in patients who do not develop cGVHD. In contrast, cytokine levels remain stable in patients with cGVHD and are generally lower 1 year after transplantation in these patients. These late differences may reflect immune suppressive therapies as well as persistent abnormalities of immune homeostasis. Taken together, these results support the hypothesis that alterations in immune homeostasis early after allogeneic HSCT are significantly associated with the subsequent development of cGVHD. Manipulation of the cytokine environment early after HSCT can modulate immune homeostasis and may be of potential prophylactic value. Administration of homeostatic cytokines late after HSCT may also have therapeutic benefit.
No relevant conflicts of interest to declare.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal