In the immunosuppression accompanying the lethal systemic graft-versus-host reaction (GVHR) directed against minor histocompatibility antigens in irradiated adult mice, we previously determined that non-T, non-B, L-leucine methyl ester (LME)-sensitive cells were implicated via two different mechanisms: one, which is interferon-γ (IFN-γ)–dependent and affects both T-cell proliferative responses and thymus-independent antibody production by CD5+ B cells; and a second, which is IFN-γ–independent and affects B-cell proliferative responses. Because IFN-γ induces the production of nitric oxide (NO), a potent immunosuppressive molecule, we investigated the involvement of NO in the suppression mediated by the LME-sensitive cells. Inducible NO synthase (iNOS) mRNA, iNOS protein, and the stable end products of iNOS pathway, L-citrulline and nitrite, were detected early in GVHR in LME-sensitive spleen cells taken ex vivo and could be amplified in vitro by T and B mitogens. Inhibition of NO production with arginine analogs (aminoguanidine, NG-monomethyl-L-arginine [LMMA]), like anti–IFN-γ antibodies, reversed suppression of both T-cell responses to concanavalin A and CD5+ B-cell responses, but not of B-cell response to lipopolysaccharides (LPS). The GVHR-associated, IFN-γ–dependent immunosuppression of T-cell proliferation and of antibody synthesis by CD5+ B cells is the consequence of NO production by LME-sensitive cells. Immunohistochemical analyses indicate that these cells belong to the macrophage lineage.
THE GRAFT-VERSUS-HOST reaction (GVHR) is a major complication of bone marrow transplantation. GVHR is initiated by mature alloreactive T cells of donor origin, specific for antigenic differences that can be encoded by genes located outside the major histocompatibility complex (MHC). This may occur both in humans, when donor and recipient are HLA compatible,1,2 and in mice, when donor and recipient bear the same H-2 haplotype.3-8The development of the GVHR is associated with an active immunosuppression inducing a severe immunodeficiency syndrome responsible for much of the mortality.9 10
In a previous study,11 we analyzed GVHR immunosuppression in response to non–H-2 histocompatibility antigens in a model of murine lethal GVHR induced by injecting B10.D2 (H-2dMlsb) bone marrow and spleen cells into lethally irradiated (DBA/2 × B10.D2)F1 (H-2d/d Mlsa/b) recipients. We found that GVHR spleen cells exhibit a suppressive action that alters T- and B-cell functions such as the concanavalin A (Con A) and lipopolysaccharride (LPS) mitogenic responses of normal spleen cells, as well as the response of CD5+ B cells against a cryptic determinant on mouse erythrocytes revealed by proteolytic treatment with the enzyme bromelain (anti–Br-MRBC response). CD5+ B cells form the predominant B-cell subset (B-1) in the peritoneal and pleural cavities, and their specificity is predominantly against bacterial polysaccharides and self-antigens.12 A study of the mechanisms responsible for the GVHR suppression showed that: (1) elimination of T lymphocytes by a treatment with anti–Thy-1 monoclonal antibody (MoAb) did not modify the suppressive activity of GVHR spleen cells, indicating that T cells were not responsible for the active, nonspecific suppression; (2) an anti–interferon-γ (IFN-γ) MoAb greatly attenuates the suppression of the anti–Br-MRBC antibody response and of the mitogenic response to Con A, but not to LPS, suggesting the existence of both IFN-γ–dependent and IFN-γ–independent immunosuppression; (3) treatment of GVHR spleen cells by L-leucine methyl esther (LME), a lysosomotropic agent,13 considerably diminishes both types of suppressive activity. From these and other observations, we determined that the GVHR-associated active immunosuppression is linked to the interactions of at least two populations: (1) a T-cell population synthesizing IFN-γ, which is devoid of direct inhibitory activity; (2) an LME-sensitive, non–T-cell population, which mediates suppression of all responses studied through an effector molecule (or molecules) not identified in that study.
In the present work, we investigated whether nitric oxide (NO), whose synthesis is mainly induced by IFN-γ, is one of the effectors of the GVHR-associated immunosuppression. NO has been shown to mediate the suppressive effect of activated macrophages on lymphocyte responses to a T-cell mitogen in rats,14 and enhanced NO production has been observed in several experimental models of immunosuppression associated with GVHR.15-17 We have analyzed: inhibition of iNOS (inducible NO synthase) induction by anti–IFN-γ MoAb; inhibition of NO production by NG-monomethyl-L-arginine (LMMA) and by aminoguanidine, both competitive inhibitors of iNOS; the selective destruction of macrophages by LME treatment. The effects of these treatments on the ability of GVHR spleen cells to mediate the GVHR-associated immunosuppression were explored. We found that NO, synthesized during GVHR by an iNOS whose transcription is induced by IFN-γ, mediates the IFN-γ–dependent, but not the IFN-γ–independent immunosuppression by LME-sensitive cells. Immunohistochemical analyses using anti-iNOS and anti-CD11b/Mac-1 antibodies showed that the LME-sensitive cells synthesizing NO are macrophages.
MATERIALS AND METHODS
Animals.
DBA/2 (H-2d, Mlsa), B10.D2 (H-2d, Mlsb) and (DBA/2 × B10.D2)F1 (H-2d/d, Mlsa/b) mice were raised in our own animal facility from stock purchased from Jackson Laboratories (Bar Harbor, ME) or Harlan OLAC (Gannat, France).
Preparation of cell suspensions.
Single-cell suspensions of spleen or femoral bone-marrow cells were prepared in RPMI 1640 medium; cells from three to four donors were pooled. Viable cell numbers were determined using Trypan blue dye exclusion as criterion of viability.
Induction of GVHR.
(DBA/2 × B10.D2)F1 adult recipient mice were given a lethal dose (9 Gy) of whole-body irradiation using a 137Cs source at a dose rate of approximately 0.8 Gy/min. Twenty-four hours after irradiation, they were grafted intravenously with 107 bone marrow and 8 × 106 spleen cells from sex-matched normal B10.D2 donors; the control groups consisted of either irradiated B10.D2 recipients reconstituted with 107 bone marrow and 8 × 106 spleen cells from syngeneic donors (isografted mice), or else normal B10.D2 mice, as indicated. Grafted mice were killed at various intervals from day 5 to day 21 after transplantation for immunologic testing.
Antibodies and reagents.
Hamster antimouse IFN-γ MoAb and normal hamster IgG were purchased from Genzyme (Cambridge, MA) and Immunotech (Marseille, France) respectively. Rat anti-Thy-1 MoAb and rat antimouse CD11b/Mac-1 MoAb were obtained from PharMingen (San Diego, CA). Rabbit anti-iNOS affinity-purified polyclonal Ab were acquired from Transduction Laboratories (Lexington, KY). Rabbit anti–transforming growth factor 1 (TGF-β1) polyclonal Ab were purchased from Santa Cruz Biotechnology (Santa Cruz, CA). Biotinylated goat antirabbit immunoglobulin (Ig) was purchased from BIOSYS (Compiègne, France). Rabbit antirat Ig antibodies and rat anti-alkaline phosphatase MoAb (DAKO Rat APAAP) were obtained from DAKO (Glostrup, Denmark). Alkaline phosphatase substrate kit (Vector Blue substrate kit), Horseradish Peroxidase Streptavidin, and AEC chromogen kit were acquired from Vector Laboratories (Burlingame, CA) and Sigma (St Louis, MO), respectively. LMMA and NG-monomethyl-D-arginine (DMMA) were purchased from Calbiochem (San Diego, CA). Aminoguanidine, LME, and bromelain were obtained from Sigma. Aquatex (aqueous mounting media for microscopy) was obtained from MERCK (Darmstadt, Germany).
Cell treatments.
Where required, spleen cells were treated twice with anti–Thy-1 plus complement (C) under conditions that abrogate the response of normal spleen cells to Con A. Briefly, spleen cells (2 × 107/mL) in RPMI 1640 were first incubated at 4°C with anti–Thy-1 MoAb at 1/200 final dilution for 30 minutes. Guinea pig C was then added at a 1/10 final dilution, and the cells were incubated at 37°C for 45 minutes. At the end of this period, the cells were washed three times in cold RPMI. The entire procedure was then repeated.
Treatment of the GVHR spleen cell population with LME was performed according to the method of Thiele et al.13 Spleen cells (5 × 106/mL) were incubated for 40 minutes at room temperature in RPMI containing 5 mmol/L LME, and were then washed three times in RPMI 1640. This treatment causes lysosomal disruption and selective death of cells with a high lysosomal content, such as macrophages, natural killer (NK) cells, and precytotoxic T lymphocytes.18 Between days 5 and 21 after grafting, the proportion of LME-sensitive cells in GVHR spleen were found to range from approximately 40% to 75%; observed percentages varied from one experiment to another, but within a given experiment did not seem to be time-dependent during the period studied.
Mitogen stimulation assays.
Mitogens used were Con A (Pharmacia Fine Chemicals, Uppsala, Sweden) at a final concentration of 2.5 μg/mL and LPS (Escherichia coli055: B5; Difco, Detroit, MI) at a final concentration of 100 μg/mL. Proliferation assays were performed in RPMI 1640 medium containing 1 mmol/L L-arginine, β-mercaptoethanol (5 × 10−5 mol/L), and gentalline (Boehringer, Mannheim, Germany) and supplemented with 0.6% normal mouse serum. Experiments were performed in 96-well flat-bottomed plates (Microtest III; Falcon; Becton Dickinson, Franklin Lakes, NJ). Spleen cells taken from normal DBA/2 mice were cultured (2 × 106 cells/mL, 0.2 mL/well) either without treatment, for the response to Con A, or after treatment with anti–Thy-1 plus C, for the response to LPS. After a 48-hour period of incubation at 37°C in a 5% CO2 atmosphere, cells counts were determined and cultures were pulsed with 37 kBq of [3H]thymidine and cultured for an additional period of 18 hours. Cells were then harvested onto glass fiber filters with a Skatron unit (Skatron Instruments, Lier, Norway), and incorporated [3H]thymidine measured by liquid scintillation counting (LKB Rackbeta 1218; Wallac OY, Turku, Finland). In experiments where the suppressive activity of GVHR spleen cells was studied, normal DBA/2 cells at the same concentrations as given above were cocultured with either GVHR or B10.D2 (control) spleen cells (106 cells/mL, 0.1 mL/well). The total volume was maintained at 0.2 mL/well. Cultures were incubated and pulse-labeled as described above. In all proliferation assays, each test group was assayed in quadruplicate and, where tested, cell counts paralleled [3H]thymidine uptake.
Antibody plaque-forming cells (PFC) against bromelain-treated syngeneic erythrocytes (Br-MRBC).
One percent to 2% of B cells in normal murine spleen express the CD5 antigen and secrete, without T-cell help, antibodies against a cryptic determinant (phosphatidyl choline) on mouse erythrocytes (MRBC), which is unmasked by proteolytic treatment with the enzyme bromelain12,19; such bromelain-treated MRBC are designated herein as, Br-MRBC. LPS treatment increases the anti-Br–MRBC response of CD5+ B cells in vitro. Normal DBA/2 responding spleen cells were pretreated with anti-Thy–1 plus C, and then resuspended in RPMI 1640 medium containing β-mercaptoethanol, gentalline, and 0.6% normal mouse serum before seeding into 24-well tissue culture plates (Falcon 3008; Becton Dickinson). A total of 5 × 106 responding cells were cultured for 3 days with LPS (10 μg/mL), in the presence of either 106 GVHR or 106 control spleen cells in a total volume of 1 mL/well. Br-MRBC were prepared according to the method of Cunningham.19 The blood of B10.D2 mice was obtained by retroorbital venous puncture and was mixed with heparin. Immediately thereafter, the red blood cells were washed three times in phosphate-buffered saline (PBS), incubated for 30 minutes at 37°C as a 50% suspension with bromelain at a final concentration of 10 mg/mL in PBS, and then washed three more times. Direct PFC specific for Br-MRBC were detected by the method of Cunningham and Szenberg.20 Results are expressed as the mean number of PFC obtained with LPS minus the mean number of PFC in the absence of LPS.
Determination of NO production.
Nitrite present in cell culture supernatants was measured by a microplate assay method21: 100-μL aliquots were removed from conditioned medium and incubated with 100 μL of the Griess reagents: N(1-naphtyl) ethylene diamine dihydrochloride (0.15% in H2O), and sulfanilamide (1.5% in 1 N HCl) at room temperature for 10 minutes. Nitrites form a chromophore with the Griess reagents, absorbing at 543 nm. The absorbance was determined with a MR 700 microplate reader (Dynatech, Chantilly, VA). Nitrite concentration was calculated from an NaNO2 standard curve.
Measuring NO synthase (NOS) activity by monitoring the accumulation of nitrite, a stable oxidative end product of NO, is currently the standard assay for NOS activity. However, the NOS activity assay based on the biochemical conversion of L-arginine to L-citrulline by NOS is an incomparably specific and sensitive method compared with nitrite dosage. To analyze the whole set of radiolabeled L-arginine–derived metabolites produced by GVHR spleen cells, a fast radioactive high performance liquid chromatography (HPLC) method was used. This method, extensively described elsewhere,22 is based on the fact that L-arginine is converted either to ornithine and urea via the arginase pathway, or to L-citrulline and the toxic split product NO via the NOS pathway. In brief, GVHR spleen cells (3 × 106/mL) were incubated in RPMI 1640 medium with 37 MBq of L-[2, 3-3H]arginine (NEN, Dupont de Nemours, Le Blanc Mesnil, France) for 48 hours. The cell supernatant was then collected, and the L-[3H]arginine, L-[3H]citrulline, and [3H]ornithine it contained were measured by HPLC. Concentrations are expressed in relative terms, with (arginine) + (citrulline) + (ornithine) = 100% in each case.
iNOS mRNA analysis.
Spleen cell RNAs extracted with RNA B (Bioprobe, Montreuil, France) were fractionated by electrophoresis on 1% agarose/2.2 mol/L formaldehyde gel in MOPS running buffer (Sigma), blotted onto Hybond-N membranes (Amersham, les Ulis, France), and probed with 15 ng of random-primed32P-labeled cDNA fragments synthesized with a random priming kit as directed by the manufacturer (Appligene, Illkirch, France). Hybridizations were performed at 42°C in 50% formamide solution with the cDNA probe (950 bp 5′-end fragment) specific for murine macrophage iNOS23 and with an actin cDNA fragment.24 After two washes at 65°C in high (2X SSC [Bioprobe], 0.1% sodium dodecyl sulfate [SDS]) and low concentration (0.1X SSC, 0.1% SDS) salt solutions, the blots were exposed to x-ray films at −80°C in the presence of intensifying screens. Quantitative determination of iNOS mRNA present in each of the various samples was normalized with respect to the concentration of actin mRNA detected in the same sample.
Cell lines.
CTLL2 cells were maintained in RPMI 1640 medium supplemented with 5% heat-inactivated fetal calf serum (FCS) and recombinant interleukin-2 (IL-2). The EMT6 and RAW264.7 (American Type Culture Collection [ATCC], Rockville, MD, #TIB71) cell lines were cultured and expanded by serial transplantation in RPMI 1640 containing 5% FCS. EMT6 is a mammary adenocarcinoma from BALB/c mice, and RAW264.7 is a mouse macrophage tumor; both express iNOS activity after incubation with LPS and IFN-γ.
Dosage of IFN-γ and IL-2 in the supernatant of GVHR spleen cells.
A total of 50 μL of supernatants was tested for the presence of IFN-γ using a commercial enzyme-linked immunosorbent assay (ELISA) kit (R&D Systems, Abingdon, UK).
A total of 50 μL of supernatant was added to 5 × 103 CTLL2 (previously starved of IL-2 for 4 hours), and proliferation was measured 24 hours later by a colorimetric method.25 IL-2 concentration is given as international units per milliliter calculated from a standard curve using human recombinant IL-2, which was tested in parallel under the same conditions.
Immunohistochemistry.
GVHR or isografted control spleen cells were spotted on SuperFrost/plus slides (Menzel-Glaser, Braunschweig, Germany) after cell treatment, mitogen stimulation, and coculture with normal DBA/2 cells. Additional controls consisted of RAW264.7 cells, either uninduced (negative control) or treated (positive control) with 100 U/mL IFN-γ and 1 mg/mL LPS for 12 hours. Cytospin preparations (5 × 104 spleen cells/spot) were air dried and kept at −80°C before immunostaining. Briefly, cytospins were incubated with anti-iNOS, anti-CD11b/Mac-1, and anti–TGF-β1 primary Ab at 1/100 final dilution. iNOS is detected in the cytoplasm of NO-producing cells, CD11b/Mac-1 molecules are expressed on cell surface membranes of macrophages and granulocytes, and TGF-β1 is shown in the cytoplasm of a broad spectrum of cells. The binding of anti-iNOS and anti–TGF-β1 Ab was detected by a biotinylated goat antirabbit Ig second Ab followed by the Horseradish Peroxidase Streptavidin reagent. The binding of anti-CD11b MoAb was evidenced by a rabbit antirat Ig second Ab, which also reacts with the complex formed by a rat monoclonal anti-alkaline phosphatase antibody and alkaline phosphatase enzyme. All incubations were performed at room temperature for 1 hour with the primary antibody and 30 minutes with each of the conjugates, followed by 5-minute washes in Tris-buffered saline plus 0.3% bovine serum albumin (BSA). Endogenous alkaline phosphatase activity was blocked using Levamisole. Slides were developed at room temperature by two successive incubations in AEC chromogen (6 minutes) and in alkaline phosphatase substrate (15 minutes). Finally, slides were mounted in Aquatex.
RESULTS
Effect of arginine analogs on GVHR-associated active immunosuppression.
To determine whether NO might be responsible for the GVHR-associated immunosuppression, experiments were designed to assess the effects of GVHR spleen cells, either untreated or treated with LME or arginine analogs (LMMA, aminoguanidine), on the proliferative response of normal DBA/2 spleen cells to the mitogens Con A and LPS, as well as on the CD5+ B-cell response to Br-MRBC antigen. DBA/2 cells were chosen as responders for reasons of convenience and not because they express parent-strain antigens, which are targets of the GVHR: indeed, our previous results clearly show that the GVHR-associated immunosuppression is nonspecific and not restricted by H-2 antigens.11 Results (Table 1) show that day 7 GVHR spleen cells cocultured with normal DBA/2 spleen cells abrogate the mitogenic response of the latter to both Con A and LPS, as well as the anti–Br-MRBC antibody response. Treatment of GVHR spleen cells with LME abrogated their suppressive activity; this treatment eliminates a population of non-T, non-B cells.11
Effect of LME Treatment and LMMA on the Suppressive Activity of GVHR Spleen Cells
| Normal DBA/2 Spleen Cells Cocultured With* . | Mitogen Stimulation (cpm) . | Anti–Br-MRBC Response† (PFC/culture) . | |
|---|---|---|---|
| Con A . | LPS . | ||
| Normal B10.D2 spleen cells | 123,063 ± 10,340 | 73,521 ± 6,137 | 1,446 ± 235 |
| GVHR spleen cells | 490 ± 250 [0.4%]1-153 | 346 ± 280 [0.5%]1-153 | 80 ± 11 [5.5%]1-153 |
| GVHR spleen cells LME-treated | 90,311 ± 10,626 [73%]1-153 | 71,256 ± 4,421 [97%]1-153 | 1,070 ± 241 [74%]1-153 |
| Normal B10.D2 spleen cells + LMMA‡ | 135,563 ± 7,320 | 73,916 ± 4,290 | 1,390 ± 140 |
| GVHR spleen cells + LMMA‡ | 46,898 ± 5,733 [35%]1-155 | 0 [0%]1-155 | 450 ± 40 [32%]1-155 |
| Normal DBA/2 Spleen Cells Cocultured With* . | Mitogen Stimulation (cpm) . | Anti–Br-MRBC Response† (PFC/culture) . | |
|---|---|---|---|
| Con A . | LPS . | ||
| Normal B10.D2 spleen cells | 123,063 ± 10,340 | 73,521 ± 6,137 | 1,446 ± 235 |
| GVHR spleen cells | 490 ± 250 [0.4%]1-153 | 346 ± 280 [0.5%]1-153 | 80 ± 11 [5.5%]1-153 |
| GVHR spleen cells LME-treated | 90,311 ± 10,626 [73%]1-153 | 71,256 ± 4,421 [97%]1-153 | 1,070 ± 241 [74%]1-153 |
| Normal B10.D2 spleen cells + LMMA‡ | 135,563 ± 7,320 | 73,916 ± 4,290 | 1,390 ± 140 |
| GVHR spleen cells + LMMA‡ | 46,898 ± 5,733 [35%]1-155 | 0 [0%]1-155 | 450 ± 40 [32%]1-155 |
GVHR spleen cells at day 7 after grafting were tested for their suppressive activity on the mitogenic response of normal DBA/2 spleen cells to Con A and LPS. This experiment is representative of 8 other experiments.
Anti–Thy-1 + C-treated spleen were cultured for 3 days with LPS and then assayed for PFC.
LMMA, diluted in PBS, was added at the beginning of the culture and used at 1.5 mmol/L final concentration.
Numbers in square brackets represent the percentage of the control group (normal DBA/2 cells cocultured with normal B10.D2 cells).
Numbers in square brackets represent the percentage of the control group (normal DBA/2 cells cocultured with normal B10.D2 cells + LMMA).
LMMA, a competitive inhibitor of iNOS (the enzyme that cleaves L-arginine into L-citrulline and NO) partially reverses the inhibition by GVHR spleen cells of both the mitogenic response to Con A and the anti–Br-MRBC antibody response (35% and 32% of control, respectively). Under the same experimental conditions, LMMA fails to reverse the suppression of the mitogenic response to LPS and has no effect on the Con A and LPS responses of normal DBA/2 spleen cells cocultivated with B10.D2 control spleen cells. It should be mentioned that qualitatively similar results were obtained at time points ranging from 5 to 21 days after grafting, that GVHR spleen cells cultured alone exhibit no mitogenic responses to either Con A or LPS, and that LMMA does not modify this nonresponsiveness (not shown). Aminoguanidine, another competitive inhibitor of iNOS, was used in some experiments in parallel with LMMA. LMMA and aminoguanidine have strictly the same effect on the inhibition of mitogenic responses mediated by GVHR cells (not shown). The relatively moderate concentration of LMMA or aminoguanidine (1.5 to 2 mmol/L) used in our experiments never altered the proliferation of normal B10.D2 spleen cells stimulated by mitogens, as shown in Table 1. But, as we also observed, it was recently reported26 that arginine analogs, and in particular aminoguanidine at high concentrations (5 mmol/L), suppressed both the antigen-specific and nonspecific proliferation of T lymphocytes.
In conclusion, these results suggest that NO is implicated in the GVHR-mediated suppression of the mitogenic response of T cells to Con A and of the secretion of anti–Br-MBRC autoantibody by CD5+B-cell subset, but do not support the hypothesis that NO is involved in suppression of the mitogenic response of B cells to LPS. It should be emphasized that this pattern of activity of LMMA on GVHR-associated immunosuppression is the same as that of anti–IFN-γ MoAb, which we described previously.11
Time course of iNOS mRNA expression in GVHR spleen cells.
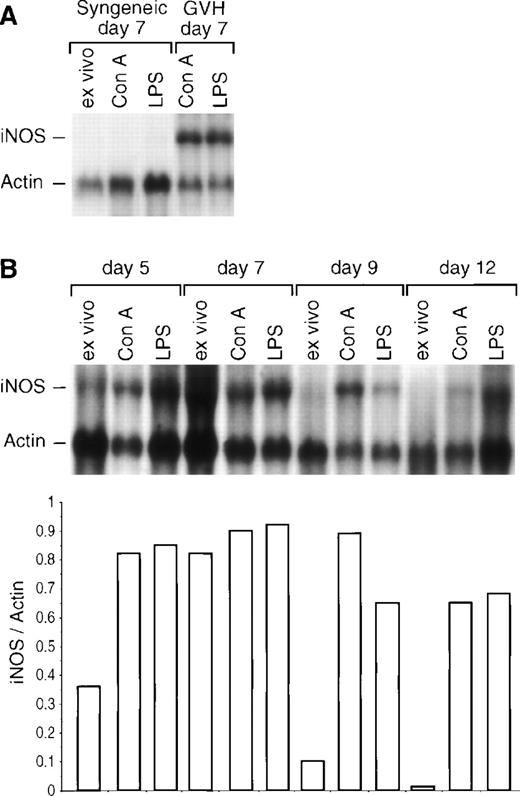
To determine the time course of iNOS transcription in GVHR spleen cells, Northern blot analyses were performed from days 5 to 14 after grafting (Fig 1). EMT6 cells stimulated with LPS and IFN-γ were included as a positive control for detection of iNOS mRNA (not shown). iNOS mRNA of 4.7-kb size became detectable in untreated GVHR spleen cells taken ex vivo in most experiments beginning on day 5 after grafting; the level of transcripts decreased on day 9 and disappeared on day 12, but was restored by in vitro stimulation with Con A or LPS (Fig 1B). Densitometric analyses of iNOS mRNA expression relative to actin are represented below the blot. Spleen cells from control mice grafted with syngeneic bone marrow (either untreated or treated by mitogens) were negative for iNOS transcription (Fig 1A).
Analysis by Northern blot of iNOS mRNA expression. Total RNA was extracted, and 10 μg of each sample was electrophoresed. The Northern blot transfer was hybridized with the specific murine macrophage iNOS cDNA probe (950 bp 5′-end fragment), and an actin probe was used as control for RNA expression. (A) iNOS RNA expression in spleen cells from control mice on day 7 after grafting with syngeneic bone marrow (either untreated or stimulated by Con A or LPS) and in mitogen-stimulated GVHR spleen cells. (B) Time course of iNOS RNA expression in GVHR spleen cells (either untreated or stimulated by Con A or LPS). Densitometric analysis of iNOS mRNA expression relative to actin is represented below the blot.
Analysis by Northern blot of iNOS mRNA expression. Total RNA was extracted, and 10 μg of each sample was electrophoresed. The Northern blot transfer was hybridized with the specific murine macrophage iNOS cDNA probe (950 bp 5′-end fragment), and an actin probe was used as control for RNA expression. (A) iNOS RNA expression in spleen cells from control mice on day 7 after grafting with syngeneic bone marrow (either untreated or stimulated by Con A or LPS) and in mitogen-stimulated GVHR spleen cells. (B) Time course of iNOS RNA expression in GVHR spleen cells (either untreated or stimulated by Con A or LPS). Densitometric analysis of iNOS mRNA expression relative to actin is represented below the blot.
When LMMA was added at the beginning of culture to day 7 GVHR spleen cells stimulated by either Con A or LPS, the 48-hour mitogen-induced iNOS mRNA levels were not decreased compared with those seen in the absence of LMMA, consistent with the role of the latter as a specific antagonist for the enzyme (not shown). A slight increase in iNOS mRNA was observed in the presence of LMMA (not shown), possibly indicative of a feedback regulatory loop influencing transcription of the iNOS gene, as suggested by others.27
Effect of LMMA and anti–IFN-γ MoAb on GVHR-mediated suppression and on nitrite and L-citrulline production.
The effects of LMMA, LME, and anti–IFN-γ MoAb on the GVHR spleen cell-mediated suppression and on the synthesis of L-citrulline and nitrite, the stable end products of the NO pathway, were studied. LMMA and anti–IFN-γ MoAb (IgG; 1.5 μg/mL), but not hamster IgG control (1.75 μg/mL), are both endowed with the ability to reverse the suppression of the mitogenic response to Con A and to reduce by 50% the level of nitrite produced by day 9 GVHR spleen cells. ELISA measurements of IFN-γ concentrations confirmed the efficacy of the anti–IFN-γ MoAb for complete inactivation of the IFN-γ present in the cultures. However, their failure to reverse the suppression of the mitogenic response to LPS contrasts with their ability to reduce by 50% the nitrite synthesis in the culture. It should be pointed out that when normal DBA/2 spleen cells are cocultured with normal B10.D2 spleen cells (controls) for 48 hours with Con A or LPS, no nitrite synthesis is observed (Table 2).
Ability of LMMA to Abrogate the Suppressive Activity of GVHR Cells and to Inhibit Nitrite Synthesis
| Normal DBA/2 Spleen Cells Cocultured With* . | Mitogen Stimulation . | |||||
|---|---|---|---|---|---|---|
| Con A . | LPS . | |||||
| [3H]Thymidine Incorporation . | Nitrite Synthesis2-155 . | IFN-γ2-154 . | [3H]Thymidine Incorporation . | Nitrite Synthesis2-155 . | IFN-γ2-154 . | |
| Normal B10.D2 spleen cells | 37,793 ± 3,605 | 0 | ND2-154 | 28,280 ± 6,000 | 0 | ND2-154 |
| GVHR spleen cells | 563 ± 176 [1.4%]2-153 | 24.3 ± 0.7 | 852 ± 462-154 | 165 ± 119 [0.5]2-153 | 25.3 ± 2.6 | 22.5 ± 52-154 |
| GVHR spleen cells + LMMA† | 16,938 ± 1,923 [45%]2-153 | 13.0 ± 0.8 | ND2-154 | 910 ± 180 [3.2]2-153 | 13.0 ± 2.3 | ND2-154 |
| GVHR spleen cells + α IFN-γ MoAb‡ | 12,538 ± 2,232 [33%]2-153 | 12.3 ± 1.6 | 2 ± 0.92-154 | 2,140 ± 480 [7.5]2-153 | 11.6 ± 2.4 | 02-154 |
| Normal DBA/2 Spleen Cells Cocultured With* . | Mitogen Stimulation . | |||||
|---|---|---|---|---|---|---|
| Con A . | LPS . | |||||
| [3H]Thymidine Incorporation . | Nitrite Synthesis2-155 . | IFN-γ2-154 . | [3H]Thymidine Incorporation . | Nitrite Synthesis2-155 . | IFN-γ2-154 . | |
| Normal B10.D2 spleen cells | 37,793 ± 3,605 | 0 | ND2-154 | 28,280 ± 6,000 | 0 | ND2-154 |
| GVHR spleen cells | 563 ± 176 [1.4%]2-153 | 24.3 ± 0.7 | 852 ± 462-154 | 165 ± 119 [0.5]2-153 | 25.3 ± 2.6 | 22.5 ± 52-154 |
| GVHR spleen cells + LMMA† | 16,938 ± 1,923 [45%]2-153 | 13.0 ± 0.8 | ND2-154 | 910 ± 180 [3.2]2-153 | 13.0 ± 2.3 | ND2-154 |
| GVHR spleen cells + α IFN-γ MoAb‡ | 12,538 ± 2,232 [33%]2-153 | 12.3 ± 1.6 | 2 ± 0.92-154 | 2,140 ± 480 [7.5]2-153 | 11.6 ± 2.4 | 02-154 |
Abbreviation: ND, not determined.
GVHR spleen cells at day 9 after grafting were tested for their suppressive activity on the mitogenic response of normal DBA/2 spleen cells to Con A and LPS and of nitrite synthesis. This experiment is representative of 4 other experiments.
The cell populations added to the culture were used at the final concentration of 106/mL. LMMA diluted in PBS was added at the beginning of the culture and used at a 1.5 mmol/L final concentration.
The concentration of anti–IFN-γ MoAb was 1.5 μg/mL. MoAb was added at the beginning of the culture. Normal hamster IgG (1.75 μg/mL) had no effect on the suppression (results not shown).
Numbers in square brackets represent the percentage of the control group (normal DBA/2 cells cocultured with normal B10.D2 cells).
Concentration (μmol/L) in the supernatant.
Concentration in pg/mL.
To unequivocally confirm that the observed nitrite production by LME-sensitive GVHR spleen cells was due to the iNOS pathway, we measured NOS activity by monitoring the conversion of L-arginine to L-citrulline. L-citrulline and NO are produced simultaneously by the action of iNOS on L-arginine, whereas accumulation of ornithine reflects the activity of arginase, the other enzyme that uses L-arginine as substrate in activated murine macrophages. IFN-γ exclusively upregulates iNOS, whereas IL-4 and IL-10 induce arginase activity.28 However, little information about possible functions of murine macrophage arginase is available. On day 7, GVHR spleen cells, either untreated or treated by mitogens, anti–IFN-γ, or LME were cultured with L-[3H]arginine in the presence or absence of LMMA. Forty-eight hours later, L-[3H]citrulline, [3H]ornithine, and L-[3H]arginine concentrations were quantified in the supernatants by HPLC. As observed in Fig 2, L-citrulline, synthesized from L-arginine (which reflects the amount of NO synthesized) is produced even by untreated GVHR spleen cells taken ex vivo, as well as after stimulation of these cells by Con A or LPS. An arginase activity is also present in GVHR spleen cells taken ex vivo and is eliminated, as expected, after LME treatment, which removes macrophages. The presence of products from both metabolic routes is indicative of the production during GVHR of Th1 and Th2 cytokines. L-citrulline production is reduced by LMMA and abrogated by anti–IFN-γ MoAb and LME treatment. As expected, the negative control, DMMA, an inactive enantiomer of LMMA, had no effect on the L-citrulline synthesis (not shown). This shows that the observed NO synthesis by GVHR spleen cells is linked to iNOS activity in LME-sensitive cells. In parallel with the HPLC analyses, GVHR immunosuppression was studied (Fig 2). As already mentioned (Tables 1and 2), the inhibition of NO production by LMMA, confirmed by the corresponding reduction of L-citrulline synthesis, abolished the suppressive effect of GVHR spleen cells on the T-cell response of normal cells to Con A. In contrast, their suppressive effect on the B-cell response of normal cells to LPS was not affected by a complete blockade of NO production, confirmed by the absence of L-citrulline in the presence of anti–IFN-γ MoAb.
Analysis by radio-HPLC of the conversion of L-[3H]arginine into L-[3H]citrulline and [3H]ornithine by GVHR spleen cells (either untreated or treated by Con A or LPS). The effects of LMMA (1.5 mmol/L), neutralizing anti–IFN-γ MoAb (1.5 μg/mL), and LME treatment on the production of L-arginine–derived metabolites is also presented (see Materials and Methods for details of experimental procedures). In parallel with HPLC analyses, the GVHR-associated immunosuppression was tested: (+) indicates that suppression was observed, (−) that it was not.
Analysis by radio-HPLC of the conversion of L-[3H]arginine into L-[3H]citrulline and [3H]ornithine by GVHR spleen cells (either untreated or treated by Con A or LPS). The effects of LMMA (1.5 mmol/L), neutralizing anti–IFN-γ MoAb (1.5 μg/mL), and LME treatment on the production of L-arginine–derived metabolites is also presented (see Materials and Methods for details of experimental procedures). In parallel with HPLC analyses, the GVHR-associated immunosuppression was tested: (+) indicates that suppression was observed, (−) that it was not.
LME-sensitive GVHR spleen cells producing NO belong to the macrophage lineage.
We next asked which GVHR spleen cell subpopulation expressed the iNOS and was responsible for nitrite synthesis. In these experiments, GVHR spleen cells were cultured either in medium alone or else in the presence of Con A or LPS. The nitrite concentrations were measured in the supernatants simultaneously with determination of the presence of iNOS protein by immunohistochemistry (see below). Results presented in Table 3 indicate that day 7 GVHR spleen cells cultured in the absence of mitogen exhibit a spontaneous nitrite synthesis (consistent with the already mentioned presence of iNOS mRNA and of L-citrulline production in GVHR spleen cells taken directly ex vivo), and that the level of this nitrite synthesis is strongly increased when GVHR cells are stimulated by Con A or LPS. Treatment of GVHR spleen cells with anti–Thy-1 + C does not modify their ability to produce nitrite after stimulation by Con A or with LPS, whereas such treatment leads to a nearly sixfold reduction of Con A–induced IL-2 synthesis. On the other hand, treatment of GVHR spleen cells with LME leads to an abrogation of nitrite synthesis after stimulation by Con A and LPS without altering the level of IL-2 synthesis. Likewise, the level of IFN-γ was not affected by LME treatment: 852 versus 827 ng/mL when stimulated by Con A and 22.5 versus 19 ng/mL when stimulated by LPS. No nitrite production could be detected in the spleens of mice grafted with syngeneic bone marrow (not shown). Taken together, these results confirm that the nitrite is synthesized in GVHR spleens by non-T, LME-sensitive cells.
Nitrite and IL-2 Production by GVHR Spleen Cells
| . | Treatment . | Mitogen Added . | ||||
|---|---|---|---|---|---|---|
| − . | Con A . | LPS . | ||||
| Nitrite3-151 . | Nitrite3-151 . | IL-23-152 . | Nitrite3-151 . | IL-23-152 . | ||
| − | 8.1 ± 0.1 | 77.0 ± 1.4 | 2.3 | 75.6 ± 2.0 | 0 | |
| GVHR spleen cells3-150 | α Thy-1 + C | 6.0 ± 0.2 | 62.6 ± 1.9 [87%]3-153 | 0.4 [17%]3-153 | 69.8 ± 0.8 [91%]3-153 | 0 |
| LME | 0 | 2 [3%]3-153 | 2 [87%]3-153 | 2 [3%]3-153 | 0 | |
| . | Treatment . | Mitogen Added . | ||||
|---|---|---|---|---|---|---|
| − . | Con A . | LPS . | ||||
| Nitrite3-151 . | Nitrite3-151 . | IL-23-152 . | Nitrite3-151 . | IL-23-152 . | ||
| − | 8.1 ± 0.1 | 77.0 ± 1.4 | 2.3 | 75.6 ± 2.0 | 0 | |
| GVHR spleen cells3-150 | α Thy-1 + C | 6.0 ± 0.2 | 62.6 ± 1.9 [87%]3-153 | 0.4 [17%]3-153 | 69.8 ± 0.8 [91%]3-153 | 0 |
| LME | 0 | 2 [3%]3-153 | 2 [87%]3-153 | 2 [3%]3-153 | 0 | |
GVHR spleen cells at day 7 after grafting were cultured for 48 hours. The cell supernatants were harvested and frozen before nitrite and IL-2 assays. This experiment is representative of 3 other experiments.
Nitrite concentration (μmol/L) in the supernatant.
IL-2 concentration is expressed in IU/mL.
Numbers in square brackets express the percentage of the result seen with untreated GVHR spleen cells.
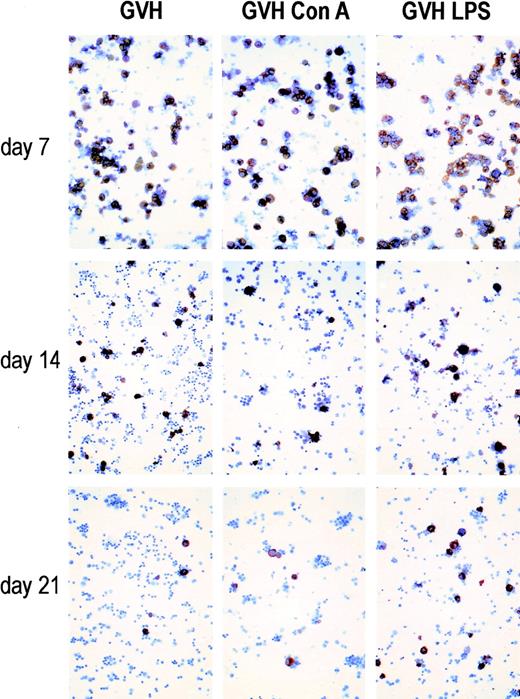
To determine the phenotype of the GVHR spleen cell subpopulation responsible for synthesizing nitrite, immunohistochemical analyses were performed at days 7, 14, and 21 after grafting, using anti-CD11b/Mac-1 antibodies, which recognize the cell surface membranes of macrophages and granulocytes, and anti-iNOS antibodies (Fig 3). As expected, RAW264.7 mouse macrophage tumor cells (positive control) stained positively with anti-CD11b/Mac-1 MoAb and with anti-iNOS Ab after stimulation with IFN-γ and LPS (not shown). Spleen cells from control mice grafted with syngeneic bone marrow were negative when stained by anti-iNOS Ab (not shown). On the other hand, in nontreated GVHR spleen cells taken ex vivo on day 7, numerous cells were intracytoplasmically stained (red) with the anti-iNOS Ab; the cell number as well as the intensity of the staining was increased when GVHR spleen cells were stimulated by Con A or LPS. In parallel, the suppressive activity of these GVHR spleen cells was tested and found to suppress at greater than 99% the mitogenic responses of normal DBA/2 cells to Con A and LPS. On day 14, immunohistochemical analyses performed on nontreated GVHR spleen cells taken ex vivo and on GVHR spleen cells stimulated by Con A or LPS showed, in both groups, a strong decrease in both the number of iNOS positive cells and the intensity of staining. Despite this pronounced reduction in staining by anti-iNOS Ab, the GVHR-associated suppression remained strong (81% and 95% for Con A and LPS, respectively). On day 21, only a few cells appeared intracytoplasmically stained; however, in this case, too, the suppression remained strong (56% and 62%). As expected, spleen cells from days 7 to 21 of the GVHR that were treated by LME lost their capacity to suppress the mitogenic responses of normal DBA/2 spleen cells to Con A and LPS; and immunostaining by anti-iNOS run in parallel on these cells was totally negative (data not shown). In addition, May-Grünwald-Giemsa staining showed that a large percentage of GVHR spleen cells, either untreated or treated by mitogens, have a monocyte/macrophage morphology (not shown). Our previous data showed that 40% to 75% of GVHR cells were LME sensitive.11 LME selectively removes macrophages, NK cells, and pre–cytotoxic T lymphocyte (CTL)13 18; and, as shown in Table 3, NO is synthesized by non-T, LME-sensitive cells. Thus, to confirm that the NO-producing cell belongs to the macrophage lineage, GVHR spleen cells were double-stained by the anti-iNOS Ab and an anti-CD11b/Mac-1 MoAb. All iNOS-positive cells were found to be stained by the CD11b/Mac-1 MoAb (data not shown). Hence, based on both immunohistochemical and cell morphological analyses, we conclude that the NO-producing cells are of the monocyte/macrophage lineage.
Immunohistochemical detection of NO-producing cells in GVHR spleen cell cytospin preparations: (GVH) untreated GVHR cells; (GVH Con A) and (GVH LPS) GVHR cells treated by Con A and LPS, respectively. Spleen cells were taken on days 7, 14, and 21 of the GVHR. Anti-iNOS antibodies stain in red the cytoplasm of NO-producing cells. Original magnification × 400.
Immunohistochemical detection of NO-producing cells in GVHR spleen cell cytospin preparations: (GVH) untreated GVHR cells; (GVH Con A) and (GVH LPS) GVHR cells treated by Con A and LPS, respectively. Spleen cells were taken on days 7, 14, and 21 of the GVHR. Anti-iNOS antibodies stain in red the cytoplasm of NO-producing cells. Original magnification × 400.
Features of TGF-β1 expression by GVHR spleen cells.
In our previous report,11 we found that TGF-β1 synthesized by T cells was one of the cytokines mediating the active immunosuppression associated with GVHR, especially the anti–Br-MRBC response and, to a lesser extent, the mitogenic response to LPS. To evaluate the part played by NO and TGF-β1 in the GVHR-associated suppression, we determined by immunohistochemistry the expression of TGF-β1, using anti–TGF-β1 Ab in parallel with that of iNOS (see above). Only a few scattered TGF-β1–positive cells were observed in both groups analyzed (untreated GVHR spleen cells taken ex vivo and GVHR spleen cells stimulated by Con A or LPS), and they were not markedly diminished by LME treatment (data not shown).
DISCUSSION
We previously showed that a nonspecific immunosuppression mediated by IFN-γ and TGF-β1 accompanies the lethal GVHR provoked by minor histocompatibility differences in irradiated adult (DBA/2 × B10.D2)F1 mice receiving bone marrow and spleen cells from semiallogeneic, H-2d identical, B10.D2 donors.11 However, IFN-γ and the latent form of TGF-β secreted by GVHR T cells have no direct suppressive effects; and only LME treatment of GVHR spleen cells, which remove macrophages, NK cells, and pre-CTL,13,18 completely abrogated their ability to suppress the responses of normal T and B cells to Con A and LPS, respectively, as well as the thymus-independent antibody response of CD5+ B cells against Br-MBRC. Antibodies produced by CD5+ B cells have a broad specificity for polysaccharides, lipids, and proteins of bacterial components. CD5+ B cells, which represent a distinct B-cell population (B-1 cells) endowed with a strong capacity for self-renewal,12,19 could therefore be important in the control of GVHR infections. Indeed, the cryptic determinant recognized on mouse erythrocytes, Br-MRBC, was identified as the phospholipid phosphatidyl choline, expressed in the outer leaflet of the plasma membrane of organisms by enzymatic cleavage of coated glycoprotein.29
The experiments reported here were designed to determine whether NO synthesized by LME-sensitive GVHR spleen cells was the effector molecule of the IFN-γ–mediated immunosuppression. NO is an important biologic mediator produced either by a constitutive enzyme in the cardiovascular and nervous system30 or by an inducible NOS in hepatocytes31 and macrophages.32 In rats, NO production by Bacillus of Calmette and Guerin (BCG)-, LPS– or IFN-γ–activated macrophages mediates their cytostatic and cytotoxic activities against microbial pathogens and tumor cells,32 as well as their inhibition of lymphocyte responses to Con A and alloantigens.14 By analogy, in our GHVR model, the involvement of IFN-γ in the nonspecific suppression of lymphocyte proliferative responses by spleen cells suggested that NO might be the effector molecule. This is in agreement with the LME-sensitivity of GVHR-associated suppressor cells, which are Thy-1 negative and μm negative, have no NK activity, and could therefore belong to the macrophage lineage. NO is endowed with multiple inhibitory activities including the ability to provoke intracellular iron loss, to inhibit the enzymes required for mitochondrial respiration, the citric aconitase enzyme,33,34 and the ribonucleotidyl transferase,35,36 and finally to inhibit protein synthesis.31 37 These activities are sufficient to account for the inhibition of the mitogenic responses and that of the anti–Br-MRBC antibody response observed with GVHR spleen cells.
The results presented here show that, in GVHR, NO synthesized by GVHR spleen cells mediates, in part, their suppressive activities. In this way LMMA or aminoguanidine, competitive inhibitors of iNOS (which cleaves L-arginine into NO and L-citrulline), partially reverse the suppression by GVHR spleen cells of both the mitogenic response to Con A and the anti–Br-MRBC antibody response by DBA/2 spleen cells. Indicators of NO release are therefore observed: GVHR spleen cells taken ex vivo exhibit a spontaneous synthesis of nitrite and L-citrulline; and the production of nitrite (which is moderate) can be amplified by triggering with Con A or LPS. These syntheses were reduced in the presence of LMMA or aminoguanidine. Both mRNA iNOS and iNOS protein were detected early in the GVHR, and their abundance was greatly increased by Con A and LPS stimulation. In contrast, L-citrulline, nitrite production, iNOS mRNA, and iNOS protein could never be detected in the spleens of mice grafted with syngeneic bone marrow. Treatment of GVHR spleen cells by LME removes the cell subpopulation involved in NO synthesis (as shown by the dosage of L-citrulline and of nitrite, and by the presence of iNOS enzyme in the cytoplasm), and abrogates their suppressive activity without altering the production of IFN-γ and the synthesis of IL-2 by T cells. NO synthesis is regulated by IFN-γ, as anti–IFN-γ MoAb, like LMMA, reduces the NO synthesis. The effector cells belong to the monocyte/macrophage lineage, as shown by immunohistochemistry using anti-iNOS and anti-CD11b/Mac-1 Ab.
It is noteworthy that LMMA, anti–IFN-γ, and LME treatment reduce NO synthesis by GVHR spleen cells and affect their capacity to suppress T-cell responses to Con A and CD5+ B-cell responses to Br-MRBC, but not their suppressive effect on B-cell responses to LPS. However, LME treatment abrogates the ability of GVHR spleen cells to inhibit the B-cell response to LPS. Taken together, these results show that IFN-γ, via NO production by an LME-sensitive population, mediates the suppressive effect of GVHR spleen cells on proliferation of normal T cells and on antibody production by normal CD5+B cells, whereas inhibition of the proliferation of normal B cells to LPS involves an LME-sensitive, IFN-γ–independent population, which does not act via the NO pathway. The implication of NO in GVHR immunosuppression has also been described by others, but mainly in experimental models involving H-2 disparities, a situation, which does not reflect that encountered in bone marrow transplantation in man. For instance, in a model of GVHR induced across an H-2 barrier (MHC class I and class II disparity) in semiallogeneic nonirradiated recipients (parent B6 → B6D2F1),15 NO production of undetermined cellular origin was reported to be responsible for a low mitogenic responsiveness of GVHR spleen cells. In that model, addition of LMMA partially restored Con A, but not LPS responsiveness; no attempt was made to measure the suppressive effect of GVHR cells on the activity of a normal responding-cell population. Consequently, the investigators postulated that a low frequency of B cells in GVHR spleens might account for the ineffectiveness of LMMA in restoring the LPS response, despite its effectiveness in decreasing nitrite levels in the same experiments. While these results are in agreement with our data, our results concerning the suppression by GVHR spleen cells of the LPS-induced proliferative response of normal spleen cells lead us to propose an alternative explanation: because LME treatment restores proliferation, but LMMA or anti–IFN-γ MoAb do not, inhibition of the LPS response during GVHR may proceed via an NO-independent mechanism. In contrast, in a fully allogeneic, but H-2 compatible model (ie, involving only minor histocompatibility differences: B10.BR → irradiated CBA/J), LMMA treatment totally restored LPS responsiveness,17 indicating that for some other minor histocompatibility differences, the NO pathway may be sufficient to account for the GVHR-induced decrease in B-cell proliferation. In a third model implicating NO in GVHR immunosuppression, GVHR was induced by donor T cells in response to an isolated MHC class II difference (bm12 → B6).16 In those studies, the investigators demonstrated the existence of a NO-dependent pathway involved in the impairment of mitogen-induced T-cell proliferation; the downregulation of IFN-γ production decreased NO production 10-fold and virtually restored splenocyte responses to Con A. We show here that the LME-sensitive cells responsible for the NO-mediated effects of IFN-γ in our model belong to the monocyte/macrophage lineage. However, whereas all NO-producing cells were found CD11b/Mac-1–positive, the converse does not hold. Thus, among the population of LME-sensitive cells, those not secreting NO might, a priori, be suspected of playing a role in suppression of the mitogenic response to LPS, a suppression that was relatively insensitive to LMMA, but completely abolished by LME treatment. In our previous report,11 we showed that TGF-β plays a role in the suppression of the mitogenic response to LPS, although synthesized in a biologically inactive (latent) form. T cells were the source of TGF-β1 in our model of GVHR-associated immunosuppression, whereas the principle source of TGF-β during inflammation is the macrophage. The present study confirmed through immunohistochemical staining that the TGF-β1–producing cells are distinct from the LME-sensitive population. Interestingly, conversion of the latent form of TGF-β to active TGF-β by macrophages has been reported.38 Hence, we hypothesized a cooperation between a T-cell population producing TGF-β1 and an LME-sensitive GVHR cell population as activator of the TGF-β latent form. However, other studies have provided evidence that IFN-γ suppresses the production of TGF-β1 by both macrophages and T lymphocytes.39 40This regulation of TGF-β by IFN-γ could explain our finding of a total absence of TGF-β protein in inflammatory macrophages during GVHR. In addition, other cytokines may intervene in GVHR-associated immunosuppression.
At present, the full range of effects of NO during GVHR is unknown. While NO production is critical for many aspects of host defense mechanisms, its production is responsible for a defective T-lymphocyte response to mitogen as well as the impairment of antibody synthesis by CD5+ B cells whose expansion and activation are induced by bacterial infections.41 NO has been shown to mediate tumoricidal activity by macrophages.32 Also, NO could be important for the graft-versus-leukemia effect associated with GVHR, although its inhibition of cytotoxic T-lymphocyte responses might be expected to counteract this potential beneficial effect. In addition to its suppressive effects on immune responses, NO has been shown to mediate the development of inflammation in the course of acute cardiac rejection in rats42 and of autoimmune MRL/lpr disease.43 It remains to be determined whether NO also plays a role in the pathogenesis of the inflammatory lesions associated with GVHR, such as the severe panniculitis observed in our experimental model.5 Despite detrimental effects on hematopoietic reconstitution44 and, possibly, on host reactivity to opportunistic infections, blockade of NO production holds some promise as a therapeutic strategy to suppress GVHR-induced immunosuppression.
ACKNOWLEDGMENT
The authors are indebted to Alexandre Yapo (CNRS, ERS 571, Université Paris-Sud, Orsay) who performed HPLC analysis and to Mohamed Oukka for the dosage of IL-2.
Deceased.
Submitted November 20, 1998; accepted April 5, 1999.
Supported by INSERM, by the Association contre le Cancer du Val de Seine, and by Association pour la Recherche contre le Cancer (Grant No. ARC 6178).
The publication costs of this article were defrayed in part by page charge payment. This article must therefore be hereby marked “advertisement” in accordance with 18 U.S.C. section 1734 solely to indicate this fact.
REFERENCES
Author notes
Address reprint requests to Pierre Bobé, INSERM Unité 267, 14, avenue Paul Vaillant-Couturier 94807 Villejuif Cedex, France; e-mail: bobe@infobiogen.fr.

![Fig. 2. Analysis by radio-HPLC of the conversion of L-[3H]arginine into L-[3H]citrulline and [3H]ornithine by GVHR spleen cells (either untreated or treated by Con A or LPS). The effects of LMMA (1.5 mmol/L), neutralizing anti–IFN-γ MoAb (1.5 μg/mL), and LME treatment on the production of L-arginine–derived metabolites is also presented (see Materials and Methods for details of experimental procedures). In parallel with HPLC analyses, the GVHR-associated immunosuppression was tested: (+) indicates that suppression was observed, (−) that it was not.](https://ash.silverchair-cdn.com/ash/content_public/journal/blood/94/3/10.1182_blood.v94.3.1028.415k24_1028_1037/5/m_blod41524002x.jpeg?Expires=1769444214&Signature=j~60bfXnZr73Zc9~A4pMxY6n7Ns6tWt19cniKEiWGmfx2kGOZ4yVBf6sAVyaoGpC-QJqJU2sSuT3JMTc2c6s4CBMExJReVn8Np83VkrqizLpY0AtoxZlLOh7Z0RN-avyMhkqyNeILCGH2KTgtolsX9CQ0of2gnoLSzPvt9bmzj2dlArKOGV9-VqywXdido8MsCg2M0nIxAVfub7BhtaYzEcGL97psWgOTzByxAZYx2TjBpNpR4VTsjMOk5Bnf4VWtcXdWRA7q89QvtxUEnS8CirLfy1Ta4fVc0uzr~XPNipuKww6yXGAvG3Wg5tOc5aiGmhyHILBMWTJ~6S0TR2UlQ__&Key-Pair-Id=APKAIE5G5CRDK6RD3PGA)
This feature is available to Subscribers Only
Sign In or Create an Account Close Modal