Abstract
Background: AML remains highly fatal, therefore understanding the mechanisms that cause chemoresistance is critical for developing more effective therapies. The leukemia bone marrow microenvironment (BME) and component MSC supports leukemia development and cell survival, implying a key role for MSC in resistance. We hypothesize that differences in the physiology of MSC in the leukemia BME (AML-MSC), relative to normal MSC (NL-MSC), exist and could be therapeutic targets.
Methods: To compare the function of AML-MSC from NL-MSC a custom reverse phase protein array (RPPA) was made using cultured MSC from AML (N = 106) and healthy donor MSC (NL; N = 71) and probed with 151 antibodies against 114 total, 36 phospho sites (on 29 proteins) and 1 cleavage site. Both biased clustering and unbiased hierarchical clustering along with principal component analysis were used to analyze data. To examine the influence of age on protein expression, age matched AML and NL MSC were compared.
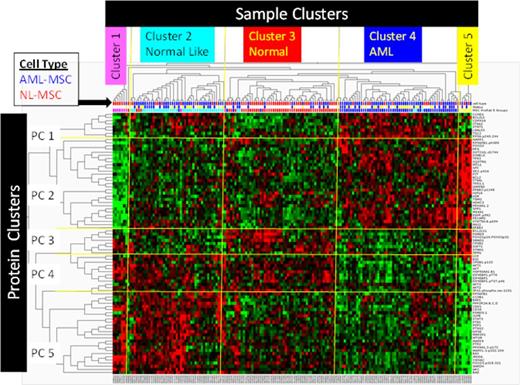
Results: Comparison of protein expression in NL-MSC and AML-MSC identified 5 Sample Clusters (SC1..SC5) based on the differential expression of 83 of 151 proteins, which formed 5 Protein Clusters (PC1..PC5) (P < 0.000001, FDR = 0.0000017)(FIG 1). Distribution of NL-MSC was significantly skewed to SC1 (7 of 8) and SC3 (38 of 52) while AML-MSC dominated SC2 (37 of 45) and SC4 (45 of 59), (Χ2 = 45.3, df=4, P <0.0001). NL-MSC were characterized by low expression of proteins in PC1 and 2 and higher expression within PC 3,4 & 5 with SC1 having more extreme levels than SC3. Protein levels in AML dominant SC4 was opposite of SC1 and SC3 for all 5 PC and was designated as "AML". SC5 was a more extreme version of SC4, for PC2, 4 and 5 but resembled SC3 for PC1 and 3. In contrast, the AML dominant SC2 resembled NL-MSC dominant SC1 and SC3 for PC2, 4 and 5, resembling SC4 only in PC1 and 3. This cluster was designated as "NL-like AML". Proteins with universally higher expression in NL-MSC included: SMADs 1 and 4, STMN1, SIRT1, p-Foxo1/3 (S32), HSP90 and EIF2S1. AML MSC had higher levels of 18 proteins across all groups including CCND1, BCL-XL, STAT5, and PPP2R2A. Salvage cases were more often in SC2 (17 of 36) and SC4 (26 of 45) than in SC3 (3 of 15) (Χ2 = 6.44, df=2, P <0.04). The observed changes were similar within three age groups (<30, 30-49, 50-59) in 22 of 25 universally differentially expressed proteins, demonstrating age independence. MSC cluster membership correlated with cytogenetics: Unfavorable cytogenetics (41 % overall) comprised 30% of NL-Like SC2, 42% of "Normal" SC3 but 52% of "AML" SC4 cases (p= 0.04), and both favorable cytogenetics cases were in SC3. MSC subpopulation type was not associated with overall survival, remission duration, or AML mutation status (FLT3, NPM1, RAS). We confirmed higher differential expression of mRNA (by qRT-PCR) for some (BCL2L1, CCND1) but not all (p21) in 10 AML-MSC and 10 NL-MSC, suggesting that both transcriptional and translational mechanisms are involved. In a separate ASH submission Battula shows that AML-MSC cannot differentiate into adipocytes like NL-MSC. Ingenuity pathway analysis (IPA) of this dataset finds that PC3 members, which are highly expressed in NL-MSC SC1, 3 & 5, but low in AML SC2 & 4, are associated with adipogenesis. Notably PI3K/AKT and JAK/STAT signaling is higher in AML dominant SC4. Hierarchical clustering revealed that 9 proteins showed differential expression between diagnosis and salvage status ( P=0.05) with p-β catenin, p-RPS6, and Galectin 3 higher in salvage samples, while SMAD6, TCF4, LYN, integrin β3, p-EIF4BP1, and p-ELK1 were higher at diagnosis. IPA reveals these proteins are highly associated with osteoblast differentiation, molecular mechanism of cancer and stem cell pluripotency, suggesting potential mechanisms for how alterations in MSC protein expression could affect chemosensitivity.
Summary: This study demonstrates that AML-MSC have two dominant protein expression signatures that are distinct from those of NL-MSC, with SC4 being associated with unfavorable cytogenetics and the salvage setting. Up-regulated pathways in AML-MSC are known to impact MSC cell survival and differentiation. Down regulated pathways may explain skewing towards osteogenic and away from adipogenic differentiation by AML-MSC. Experiments targeting MSC and assessing effects on AML blast survival are underway to determine if targeting MSC can reverse chemoresistance.
Konopleva:Novartis: Research Funding; AbbVie: Research Funding; Stemline: Research Funding; Calithera: Research Funding; Threshold: Research Funding. Andreeff:Oncoceutics, Inc.: Membership on an entity's Board of Directors or advisory committees.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal