Abstract
The application of antibodies is a promising option in the treatment of B-cell malignancies, including acute lymphoblastic leukemia (ALL) and B-cell Non-Hodgkin lymphoma (B-NHL). Although patient outcomes have improved by applying combinations of chemotherapy and antibodies, certain patients characterized by a high expression of anti-apoptotic Bcl-2 have a poor prognosis. These include adult B-NHL patients with "double-hit lymphomas" (DHLs) and pediatric ALL patients harboring a t(17;19) translocation. Furthermore, a substantial number of Burkitt´s lymphoma (BL) patients also express Bcl-2 even though the impact of this finding on prognosis is yet unclear.
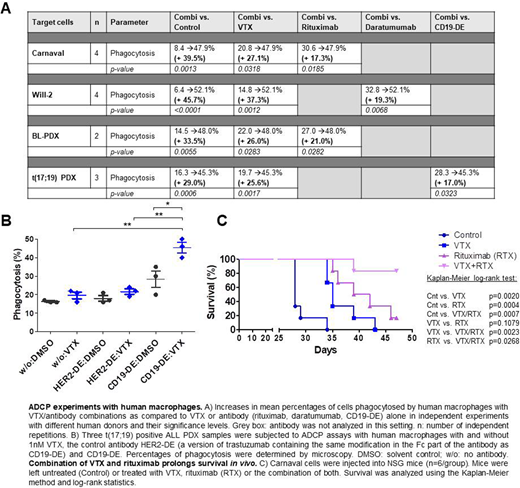
Here, we examine the role of low doses of the Bcl-2 inhibitor venetoclax (VTX, 1nM) on the efficacy of the therapeutic antibodies rituximab (CD20), daratumumab (CD38) and CD19-DE (a variant of the CD19 antibody MOR208 engineered for improved effector cell binding). Natural killer (NK)-cell mediated antibody-dependent cell-mediated cytotoxicity (ADCC) and antibody-dependent cell-mediated phagocytosis (ADCP) were evaluated. The CD20-expressing DHL cell line Carnaval and patient-derived xenograft (PDX) cells from two BL patients were used as target cells for rituximab, the CD20-negative/CD38-positive DHL cell line Will-2 was used with daratumumab and three PDX samples from t(17;19) positive ALL patients were used with CD19-DE. For the assessment of ADCP, human monocyte-derived macrophages were incubated with labelled target cells and microscopy assays were performed.
NK-cell mediated ADCC was not enhanced by VTX in any of our models. However, 17-37% increases in ADCP by macrophages were detected when Carnaval cells were subjected to combinations of VTX/rituximab and when Will-2 cells were treated with VTX/daratumumab as compared to VTX or antibody alone (p=0.0318/p=0.0185 and p=0.0012/p=0.0068, respectively, Figure A). When BL PDX cells were subjected to ADCP assays with VTX/rituximab, mean phagocytosis levels were also enhanced by 26.0% and 21.0% in the combination treatment group as compared to VTX (p=0.0283) and rituximab alone (p=0.0282; Figure A). ADCP assays with t(17;19) positive ALL-PDX cells and CD19-DE confirmed these results as phagocytosis was increased to similar extents in the combination group as compared to VTX (p=0.0017) or CD19-DE alone (p=0.0323) (Figure A/B). In order to exclude that our observations were due to an enhancement of apoptosis in target cells only, we measured cleaved caspase-3 with VTX, antibodies alone or the combination of both. Cleaved caspase-3 levels were equal in all groups suggesting that the addition of VTX resulted in an apoptosis-independent activation of macrophages. In order to minimize heterogeneity in ADCP assays, phagocytosis was next examined using expanded macrophages from NOD.Cg-Prkdcscid Il2rgtm1Wjl/SzJ (NSG) mice for our assays. Regardless of target cells and antibody, the combination of antibody treatment with VTX resulted in enhanced phagocytosis by murine macrophages, confirming our results.
The effects of VTX on the efficacy of rituximab were finally examined in vivo. Carnaval cells were injected intravenously into NSG mice and animals treated with VTX (100 mg/kg 5 days/week by oral gavage), rituximab alone (1 mg/kg once weekly intraperitoneally) or the combination of both (n=6/group). Mice were sacrificed when mice showed clinical lymphoma or leukemia engraftment and survival differences were assessed using Kaplan-Meier log-rank statistics. Compared to control, mice treated with VTX displayed a slight survival advantage, which was more marked in mice treated with rituximab (p=0.0020/p=0.0004, respectively, Figure C), suggesting a better efficacy of rituximab than VTX as monotherapy. Most importantly, mice treated with the combination VTX/rituximab showed significantly superior survival as compared to either VTX or rituximab alone (p=0.0023/p=0.0268, respectively, Figure C), suggesting additive effects in vivo.
Altogether, we show that VTX enhances the efficacy of therapeutic antibodies in models of B-cell malignancies including PDX samples. The mechanism is most likely dependent on distinct influences of VTX on macrophage activation, e. g. by myeloid immune checkpoints. Our in vivo data suggest that this combination strategy may become a promising therapeutic option for the treatment of Bcl-2 expressing B-cell malignancies in the future.
Bourquin:Amgen: Other: Travel Support. Valerius:Affimed: Research Funding. Peipp:Affimed: Research Funding.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal