Abstract
Background: Gilteritinib (ASP2215) is a novel, highly selective, potent oral FLT3/AXL inhibitor with preclinical activity against FLT3-ITD activating and FLT3-D835 resistance mutations. The objectives of this phase 1/2 study were to assess gilteritinib safety/tolerability, pharmacokinetic (PK) and pharmacodynamic (PD) profiles after single- and multiple-day dosing, and antileukemic effects in patients with R/R AML.
Methods: This open-label study (NCT02014558) enrolled patients (≥18 yr) into 1 of 7 dose-escalation cohorts (20-450 mg once daily [QD]) or concomitant dose-expansion cohorts. While confirmed FLT3 mutation was not an inclusion criterion, each expanded dose level enrolled ≥10 patients with FLT3 mutations (FLT3mut+); 120 and 200 mg dose levels were further expanded with ≥40 FLT3mut+ patients. The choice to expand these dose cohorts was based upon FLT3 inhibition in correlative assays and clinical activity seen during dose escalation. Safety and tolerability were primary endpoints; blood samples were drawn from patients in the dose-escalation cohorts to evaluate gilteritinib PK parameters and PD effects. Antileukemic response rates (eg, complete remission [CR], CR with incomplete platelet recovery [CRp], CR with incomplete hematological recovery [CRi], overall response rate [ORR]) were secondary endpoints.
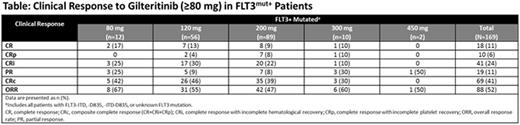
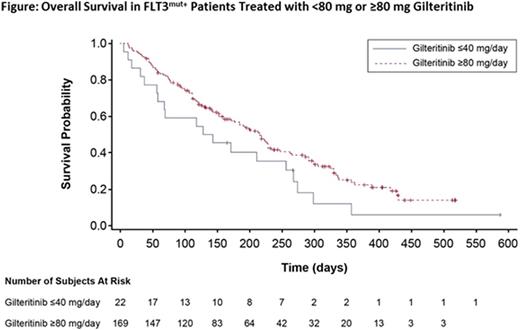
Results: Patients (N=252; 129M:123F, median age 62 yr [range: 21-90]) enrolled between October 2013 and August 2015 received ≥1 dose of gilteritinib. The study population was heavily pretreated: 70% (n=177) had ≥2 prior AML therapies, 29% (n=73) had a prior stem cell transplant, and 25% (n=63) had prior TKI treatment with sorafenib most commonly used. Across the study, 194 patients had a locally confirmed FLT3 mutation (ITD, n=159; D835, n=13; ITD-D835, n=16; other, n=6). For all enrolled patients, progressive disease (n=75), lack of efficacy (n=44), adverse events (n=34), and death (n=29) were the most common reasons for treatment discontinuation. Seven deaths were considered possibly/probably related to treatment: pulmonary embolism, respiratory failure, hemoptysis, intracranial bleed, ventricular fibrillation, septic shock, and neutropenia (all n=1). Maximum tolerated dose was determined to be 300 mg when 2 of 3 patients in the 450 mg cohort experienced diarrhea and/or hepatic transaminase elevation as dose-limiting toxicities. Diarrhea (16%) and fatigue (15%) were the most commonly reported treatment-related adverse events of any grade. Less than 5% of patients (11/252) had a maximum post-baseline QTcF interval >500 msec. Gilteritinib concentrations were generally dose proportional and showed both a long-elimination half-life (45-159 h) and substantial accumulation (3.2-10 fold) by day 15. An exposure-related increase in the inhibition of FLT3 phosphorylation with increasing doses of gilteritinib was also observed. Gilteritinib showed strong antileukemic activity in FLT3mut+ patients (ORR=49%); response was observed less frequently in patients with wild-type FLT3 (ORR=12%). While CR, CRi, and CRp occurred at all doses, responses were enriched among FLT3mut+ patients with gilteritinib steady-state trough concentrations ≥100 ng/mL, which correlated with potent FLT3 inhibition in PD assays and corresponded to doses ≥80 mg. The ORR in 169 FLT3mut+ patients receiving ≥80 mg was 52% (Table); median overall survival in this patient population was ~31 wk (range: 1.7-61; Figure) and median duration of response was 20 wk (range: 1.1-55). Clinical responses occurred in FLT3mut+ patients with -ITD, -D835, and both mutations (ORR: 55%, 17%, and 62%, respectively) as well as in FLT3mut+ patients with or without prior TKI treatment (ORR: 42% vs 56%, respectively).
Conclusions: This PD-driven, first-in-human study shows that gilteritinib was well tolerated and generated frequent, prolonged, clinically important responses in FLT3mut+ patients with R/R AML. Antileukemic responses were enriched in FLT3mut+ patients treated at doses that consistently and potently inhibited FLT3 phosphorylation. The survival of these patients appears better than expected for this patient population when treated with standard therapy. Our data suggest that FLT3 inhibition may improve survival in patients with FLT3mut+R/R AML; as such, phase 3 testing of oral gilteritinib 120 mg QD in patients with FLT3mut+R/R AML after first-line therapy is underway (NCT02421939).
Perl:Astellas US Pharma Inc.: Consultancy, Membership on an entity's Board of Directors or advisory committees; Daichi Sankyo: Consultancy, Membership on an entity's Board of Directors or advisory committees; Asana Biosciences: Consultancy, Membership on an entity's Board of Directors or advisory committees; Arog Pharmaceuticals: Consultancy, Membership on an entity's Board of Directors or advisory committees; Actinium Pharmaceuticals: Consultancy, Membership on an entity's Board of Directors or advisory committees. Altman:Janssen: Other: advisory board; BMS: Membership on an entity's Board of Directors or advisory committees; Spectrum: Other: advisory board; Ariad: Other: advisory board; Seattle Genetics: Other: advisory board; Syros: Other: advisory board. Cortes:ARIAD: Consultancy, Research Funding; BMS: Consultancy, Research Funding; Novartis: Consultancy, Research Funding; Pfizer: Consultancy, Research Funding; Teva: Research Funding. Smith:Astellas: Research Funding. Erba:Jannsen: Consultancy, Research Funding; Millennium Pharmaceuticals, Inc.: Research Funding; Agios: Research Funding; Juno: Research Funding; Incyte: Consultancy, DSMB, Speakers Bureau; Daiichi Sankyo: Consultancy; Ariad: Consultancy; Amgen: Consultancy, Research Funding; Astellas: Research Funding; Gylcomimetics: Other: DSMB; Seattle Genetics: Consultancy, Research Funding; Sunesis: Consultancy; Novartis: Consultancy, Speakers Bureau; Celator: Research Funding; Celgene: Consultancy, Speakers Bureau; Pfizer: Consultancy. Gill:Astellas: Employment. Goldberg:Bristol Myers Squibb, Novartis: Speakers Bureau; Novartis: Consultancy; COTA Inc: Employment; Pfizer: Honoraria; Neostem: Equity Ownership. Jurcic:Astellas: Research Funding. Larson:Astellas: Consultancy, Research Funding; Bristol-Myers Squibb: Consultancy. Liu:Astellas: Employment. Ritchie:Celgene: Consultancy, Other: Travel, Accomodations, Expenses, Speakers Bureau; Incyte: Consultancy, Speakers Bureau; Novartis: Consultancy, Other: Travel, Accommodations, Expenses, Research Funding, Speakers Bureau; Ariad: Speakers Bureau; Pfizer: Consultancy, Research Funding; Astellas Pharma: Research Funding; Bristol-Meyers Squibb: Research Funding; NS Pharma: Research Funding. Schiller:Incyte Corporation: Research Funding. Strickland:Celator: Research Funding; Cyclacel: Research Funding; Karyopharm Therapeutica: Research Funding; GlaxoSmithKline: Research Funding; Baxalta: Consultancy; Boehringer Ingelheim: Consultancy, Research Funding; Ambit: Consultancy; Alexion Pharmaceuticals: Consultancy; Astellas Pharma: Research Funding; CTI Biopharma: Consultancy; Daiichi Sankyo: Consultancy; Sunesis Pharmaceuticals: Consultancy, Research Funding; Abbvie: Research Funding; Sanofi: Research Funding. Wang:Incyte: Speakers Bureau; Immunogen: Research Funding. Stuart:Sunesis: Consultancy, Honoraria, Other: Travel, Accomodations, Expenses, Research Funding; Agios: Research Funding; Incyte: Research Funding; Bayer: Research Funding; Celator: Research Funding; Astellas: Research Funding. Martinelli:Ariad: Consultancy, Speakers Bureau; Pfizer: Consultancy, Speakers Bureau; BMS: Speakers Bureau; Roche: Consultancy, Speakers Bureau; MSD: Consultancy; Genentech: Consultancy; Novartis: Speakers Bureau; Celgene: Consultancy, Speakers Bureau; Amgen: Consultancy, Speakers Bureau. Bahceci:Astellas: Employment. Levis:Millennium: Consultancy, Research Funding; Astellas: Consultancy, Honoraria, Research Funding; Daiichi-Sankyo: Consultancy, Honoraria; Novartis: Consultancy, Honoraria, Research Funding.
Author notes
Asterisk with author names denotes non-ASH members.
This icon denotes a clinically relevant abstract

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal