Abstract
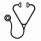
The ability to transplant across HLA disparities makes allogeneic umbilical cord blood (UCB) an attractive graft source for hematopoietic stem-cell transplantation (HSCT). Disease relapse remains a limitation, and adoptive transfer of tumor-specific T cells post UCB HSCT has not been feasible due to the functionally naïve CB T cells, and the small size as well as anonymity of the donor. We report a new approach to non-viral gene transfer using the Sleeping Beauty (SB) transposon/transposase system to stably express a 2nd generation CD19-specific chimeric antigen receptor (CAR, designated CD19RCD28) on UCB-derived T cells manufactured in compliance with current good manufacturing practice (cGMP).
After thawed UCB units are washed for clinical infusion 5% to 10% of cells are used to generate CAR+ T cells. The mononuclear cells are electroporated using a Nucleofector device to synchronously introduce two DNA plasmids coding for SB transposon (CD19RCD28) and hyperactive SB transposase (SB11). T cells stably expressing the CAR are retrieved over 28 days of co-culture by recursive additions of g-irradiated artificial antigen presenting cells (aAPC) in presence of soluble recombinant interleukin (IL)-2 and IL-21. The aAPC (designated clone #4) were derived from K562 cells and genetically modified to co-express the CD19 as well as the co-stimulatory molecules CD86, CD137L, and a membrane-bound protein of IL-15. Enrolled patients on our phase I trial receive two UCB units, thus two genetically modified T-cell products are made for each patient. We infuse thawed donor-derived CD19-specific CAR+ T cells from the dominant CB unit based on peripheral blood chimerism on days 40-100 post transplant in the adjuvant setting after double UCB HSCT
To date we have successfully manufactured 8 products for 4 patients (ALL n=3, NHL=1) enrolled on trial. The median number of T cells in the starting CB aliquot was 8.6x106 (range, 2.5x106 to 54.8x106) with final modified T cell count at median 3x109 (range,1.7x108 to 4.1x1010) at time of cryopreservation days 28-32. In the final product, the median CD19-CAR+ cell purity by flow was 88% (range, 81.9% to 95.8%). The modified T cell product consisted of median 97.3% CD3+, 2.7 CD3-/CD56+ cells. All of the products exhibited CD19-specific killing by chromium assay as illustrated (Figure ). Each clinical-grade T-cell product was subjected to a battery of in-process testing to complement release testing. One patient with ALL has been infused to date with a T cell dose of 106T cells/m2 and no toxicity has been observed. The patient remains alive and in continued molecular remission at 111 days post HSCT.
We combined the SB system and aAPC-mediated propagation of T cells to successfully manufacture disease-specific T cells from small aliquots of UCB used to restore hematopoiesis. Importantly, this approach allows us to employ adoptive therapy to enhance the graft-versus-tumor effect in UCB HSCT as an approach to improve overall survival for these recipients. Accrual to the trial continues and updated results will be presented at the meeting.
Specific lysis (Mean ± SEM, n=8) of CD19pos targets as compared to background lysis of CD19neg EL-4 (mouse T-cell line) by clinical-grade UCB-derived CD19-specific CAR+ T cells.
Specific lysis (Mean ± SEM, n=8) of CD19pos targets as compared to background lysis of CD19neg EL-4 (mouse T-cell line) by clinical-grade UCB-derived CD19-specific CAR+ T cells.
No relevant conflicts of interest to declare.
Author notes
Asterisk with author names denotes non-ASH members.
This icon denotes a clinically relevant abstract

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal