Abstract
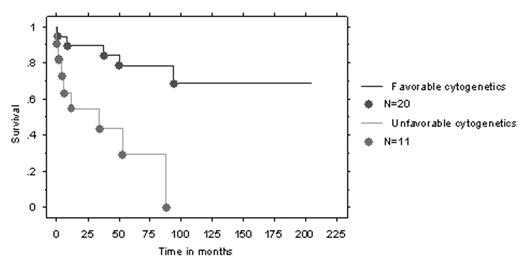
Post-polycythemic (PPMM) and post-thrombocythemic (PTMM) myeloid metaplasia are consensually referred to as secondary myelofibrosis (sMF). Prognostic variables in sMF are not as well defined as they are for agnogenic myeloid metaplasia (AMM). Such information is particularly crucial for management decisions in transplant-eligible patients. Accordingly, we examined the prognostic impact of several clinical and laboratory variables in 66 young patients (age < 60 years) with sMF including 37 with PPMM and 29 with PTMM. Multivariate analysis of parameters other than cytogenetics identified older age (p=0.02), anemia (hemoglobin level < 10 g/dL; p=0.007), and PPMM (p=0.009) as independent risk factors for shortened survival. However, when such analysis was restricted to patients in whom cytogenetic studies were performed (n=31), the presence of unfavorable cytogenetic abnormalities (i.e. clones other than 20q- and 13q-) became the one and only adverse prognostic factor for survival (p=0.001).
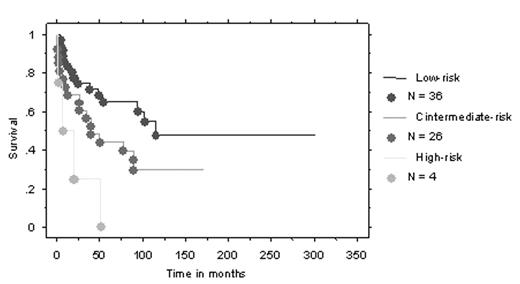
The prognostic value of cytogenetics was independent of the Dupriez prognostic score (p=0.003).
A similar analysis in a temporal cohort of 50 age-matched patients with AMM also identified unfavorable cytogenetics as an independent predictor of poor survival along with thrombocytopenia and anemia. The current study suggests an important prognostic role for cytogenetics in both de novo and secondary myelofibrosis.
Author notes
Corresponding author

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal