Allogeneic hematopoietic stem cell transplantation (allo-HCT) is a procedure undertaken to cure hematological malignancies, especially leukemia. Graft-Versus-Host Disease (GVHD) is a serious condition that often appears following allo-HCT. Friend Leukemia Virus Integration 1 (Fli-1) is a transcription factor highly expressed in cancers including erythroleukemia and acute myeloid leukemia while also implicated in pathogenesis of systemic lupus. We have interrogated the role of Fli-1 in T-cell responses by generating a novel T-cell specific conditional disruption of fli-1 where essential exons 3 and 4 of the gene are floxed and excised in the presence of CD4-Cre recombinase. Models of acute GVHD (aGVHD) and chronic GVHD (cGVHD) were tested utilizing hematopoietic cells from mice with a heterozygous (fli-1-/+ or Het) or homozygous (fli-1-/-or Null) disruption of the fli-1 gene, or from wild-type (fli-1+/+ or WT) littermate controls. At baseline, T cells among each of these three mouse strains showed no significant difference in CD44/CD62L expression or CD4+FoxP3+ (nTreg) frequencies.
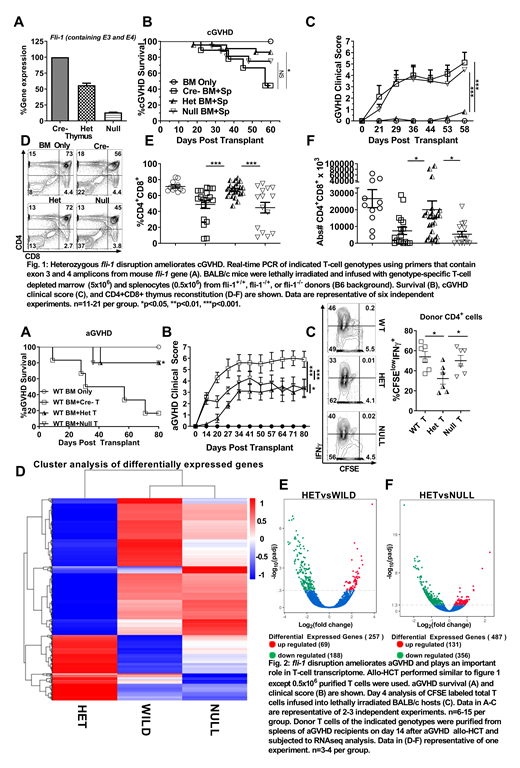
In the cGVHD model, BALB/c (H2Kd) recipients were infused with allogeneic B6 (H2Kb) genotype-respective bone marrow and splenocytes in order to induce cGVHD. Recipients that received fli-1-/+CD4Cre+ marrow and splenocytes demonstrated improved survival and mild cGVHD, whereas those that received fli-1-/-CD4Cre+ or WT donor cells developed serve cGVHD (Fig. 1 a-f). Cellular studies from lymphoid organs of cGVHD allo-HCT recipients revealed that disruption of fli-1 was associated with decreased frequencies of donor CD4+ cells expressing IL-17A, IFN-γ, T follicular-like (TFH-like) cell markers, and CD8+ cells expressing PD-1.
In aGVHD settings, donor fli-1-/+CD4Cre+ T cells had a decreased ability to induce aGVHD compared to WT donor T cells and fli-1-/- donor T cells (Fig. 2 a-b). When investigating cellular mechanisms in aGVHD settings, we found that fli-1-/+CD4Cre+ T cells produced significantly lower IFN-γ early after T-cell activation in vivo compared to WT and fli-1-/-CD4Cre+ T cells (Fig. 2 c). To then investigate the role of Fli-1 in T cells beyond GVHD, we utilized a colitis model by transferring naïve CD4+ T cells (CD44-CD25-) into Rag2-/- syngeneic recipients. While fli-1+/+ T cells induced severe colitis as expected, fli-1-/- and fli--/+ T cells caused moderate and mild colitis, respectively. These results were consistent with those observed in GVHD models.
To elucidate underlying mechanisms, we tested the effects of Fli-1 on antigen-specific T-cells using a MHC-II restricted TCR transgenic (Tg) mouse strain specific for HY-peptide. CD4+CD25- T cells from fli-1+/+, fli-1-/+, or fli-1-/- CD4Cre+ TCR-Tg mice were polarized in vitro with endogenous antigen presenting cells from spleen in presence of HY-peptide under iTreg- or Th17-polarizing conditions. Both fli-1-/+ and fli-1-/- TCR-tg T cells exhibited significant increases in iTreg (CD4+FoxP3+) frequencies and surface expression of iTreg functional markers (CD25, CD39, CD73, NRP-1), while also having significantly decreased frequencies of IL-17A producing T cells compared to WT-TCR-tg T cells.
To further explore the molecular mechanisms, we retrieved fli-1+/+, fli-1-/+, or fli-1-/- donor T cells from recipient spleens after allo-HCT and did RNAseq analysis on these cells. RNAseq data reveals significant differences in mRNA expression within acute inflammatory response and positive regulation of the immune response enrichment pathways between fli-1-/+ T cells and littermate fli-1+/+ T cells, and to a lesser extent in fli-1-/- T cells (Fig. 2 d-f). Thus, reducing Fli-1 transcriptional activity represents a potential therapeutic concept toward ameliorating GVHD after allo-HCT, while simultaneously targeting cancers such as leukemia which typically overexpress Fli-1.
No relevant conflicts of interest to declare.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal