Background: RBC-transfusion dependency (RBC-TD) is associated with a decreased probability of overall survival (OS) and progression free survival (PFS) in patients with myelodysplastic syndromes (MDS) (Malcovati L et al. J Clin Oncol 2007 25:3505) but it is unclear if transfusion dose burden is an independent prognostic factor. The purpose of this study was to assess the impact on lower-risk MDS patients, of RBC-transfusion (RBCT) burden status defined according to revised 2018 IWG criteria (Platzbecker et al; Blood 2018).
Material and Methods: According to the R-IPSS selection criteria, we identified in our database 474 lower-risk (R-IPSS risk very low, low and intermediate) MDS patients diagnosed at the Catalan Institute of Oncology of Barcelona (01/1992-07/2018). Transfusion burden history was prospectively registered in our database. Data on the transfusion burden was calculated dividing the cumulative total of units of blood received at the end by the time since the beginning of the interval in which the first transfusion was received. RBCT burden, defined according to 2018 IWG criteria, divided patients into 3 categories (non-transfused [NTD], low transfusion burden [LTB] (3 to 7 units in 16 weeks) and high transfusion burden [HTB] patients (³ 8 units in 16 weeks). In this analysis, patients who had received 1 or 2 RBC units in 16 weeks, where included in the NTD category. Overall survival (OS) and progression free survival (PFS) were measured in years since diagnosis.
Results: Median age at diagnosis was 72 years (range 32-101). 332 (70%) patients were male. WHO diagnosis was: 3% CRDU, 7% RA, 42% RCMD, 14% RAEB-1, 4% RAEB-2, 26% CMML, the remaining 4% were MDS-U and isolated 5q deletion. R-IPSS categories were: 178 (38%) very low risk, 219 (46.2%) low risk and 77 (16%) intermediate risk. Median follow up time for survivors was 5.4 years (range 0.25-23.8). 132 (28%) of patients were transfusion dependents (LTB and HTB patients). Mean dose density of packed red blood cells amongst those who were transfusion dependents was 3.2 units per month, with a median of 2.9 units per month (IQR 1.9-4.3). At the time of last follow up, 274 (58%) patients had died and 72 (15%) had progressed to AML.
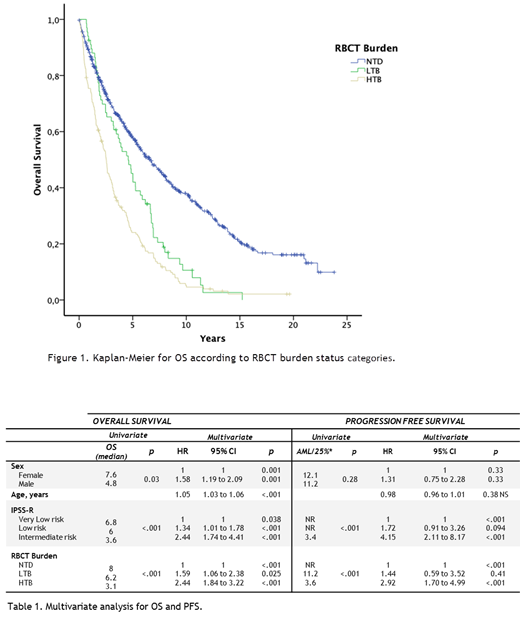
According to 2018 IWG criteria, RBCT burden categories were 342 (72%) NTD, 35 (7%) LTB and 97 (21%) HTB patients. Median OS for RBCT burden categories: NTD (8 years; 95% CI 6.6-9.5), LTB (6.2 years; 95% CI 4.2-8.1) and HTB (3.1 years; 95% CI 2.4-3.8) were significantly different (p<0.001; Figure 1). Moreover, the rate of progression to acute myeloid leukemia was 39 (11%), 7 (20%) and 26 (27%) for categories NTD, LTB and HTB respectively (p<0.001). Multivariate analysis performed included gender, age at diagnosis, IPSS-R and RBCT burden status and showed that RBCT burden status was associated with poor OS and PFS, independent of R-IPSS category, age and gender (Table 1). Transfusion burden was inversely associated with OS and PFS with an increasing effect on hazard ratio.
Conclusions: Our results confirm in our single-centre experience the negative impact on survival and progression-free survival of RBCT treatment, even at relatively low dose burden. As therapeutical decisions are based on the initial prognostic risk assessment, the inclusion of RBCT burden categories may provide more precise prognostic information with impact on the therapeutic approach.
Sureda:Novartis: Consultancy, Honoraria; Takeda: Consultancy, Honoraria, Speakers Bureau; Sanofi: Consultancy, Honoraria; Roche: Honoraria; BMS: Consultancy, Honoraria; Gilead: Consultancy; Janssen: Consultancy, Honoraria.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal