Abstract
Background:
Thrombotic and hemorrhagic complications are commonly encountered in uncontrolled essential thrombocythemia (ET). Both anagrelide and hydroxyurea (HU) have proven efficacious in cytoreduction as well as reducing these events and remain first line therapy for most high-risk ET patients. Independent of their role in risk-reduction, little is known about how these therapies impact patient symptomatology or quality of life. In this study, we compared the clinical and symptomatic profiles of ET patients receiving HU or anagrelide against patients with no previous experience with these agents.
Methods:
Data was assessed from a prospectively collected international database of ET patients in which demographics, disease features, and ET symptoms utilizing the myeloproliferative neoplasm symptom assessment form (MPN-SAF; Scherber et al, 2011). The MPN-SAF includes the patient's perceptions of common MPN-related symptoms and overall quality of life (QOL) on a 0 (absent) to 10 (worst imaginable) scale. Total symptom score (TSS) was computed based on symptom items using the published scoring algorithm on a 0 (all reported symptoms absent) to 100 (all reported symptoms worst imaginable) scale. ET risk scores were calculated using the IPSET scoring algorithm (Passamonti 2012). Thrombocytopenia was defined as a platelet count <100 x 10(9)/L, anemia was defined as hemoglobin<10 g/dL and leukopenia was defined as a white blood cell count <4.0 x 10(9)/L. Associations between the MPN-SAF individual symptoms were investigated using chi-square test for categorical data and ANOVA F-test for continuous variables.
Results
Hydroxyurea vs. HU Naive
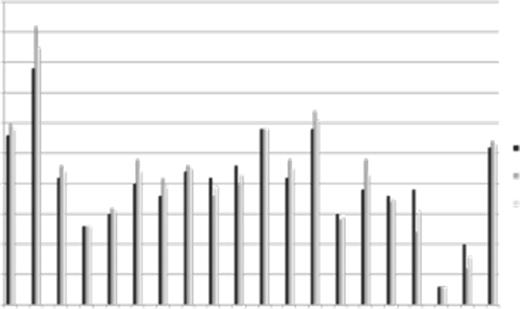
A total of 402 ET patients with active HU use were compared to 392 ET patients with no history of HU use. Patients using HU were older (63.5 years vs. 52.3 years, p<0.001) and had a greater concentration of both high risk (24.9% vs. 11.4%, p=0.001) and intermediate risk (53.9% vs 38.4%, p<0.001) patients. They also had a higher rate of prior thrombosis (29.8% vs 11.3%, p<0.001) and leukopenia (10.1% vs. 3.0%, p<0.001). No differences were noted between gender, a history of prior hemorrhage, red blood cell transfusion requirements, or the presence of anemia/thrombocytopenia. In comparing symptom profiles, no significant differences were noted between TSS or individual symptoms with the exception of slightly more severe cough in HU patients (1.5 vs. 1.1, p=0.02, Figure 1).
Anagrelide vs. Anagrelide Naive
A total of 49 ET patients with active anagrelide use were compared to 794 ET patients with no history of anagrelide use. Patients using anagrelide had a longer mean disease duration (8.1 years vs. 5.8 years) and were more anemic (9.1% vs. 1.2%, p<0.001). No differences were noted between age, gender, risk scores, the presence of leukopenia/thrombocytopenia, a history of prior thrombosis or hemorrhage complications or red blood cell transfusion requirements. Additionally, there were no significant differences between TSS or individual symptom items (Figure 1).
HU vs. Anagrelide
A total of 402 patients currently using HU were compared to 39 patients currently using anagrelide. Overall, HU users were slightly older (63.5 years vs. 55.1 years, p<0.001) with a greater population of patients meeting high risk criteria (24.9% vs. 2.8%, p=0.002) and having a history of prior thrombosis (29.8% vs. 12.8%, p=0.02). Patients receiving anagrelide had a slightly longer disease duration (8.2 years vs. 6.0 years, p=0.0446). In comparing symptom profiles, no differences were noted in TSS or individual symptom items between cohorts.
Discussion
In this retrospective analysis, it does not appear cytoreduction with either HU and/or anagrelide has a significant impact on ET symptom burden despite reducing vascular events. Importantly, the higher risk scores in HU patients did not translate directly into greater patient symptomatology supporting previous studies demonstrating a poor association between these two items. Prospective trials measuring ET symptom change, in the setting of randomized trials will better quantify impact of cytoreduction on symptom burden as well as quantify impact of newer agents such as interferon or jak inhibition.
Symptom Comparisons Between HU, Anagrelide and Other Therapy
Symptom Comparisons Between HU, Anagrelide and Other Therapy
Kiladjian:Incyte Corporation: Consultancy; Novartis: Other: Travel grant; Research Funding paid to institution (Hôpital Saint-Louis et Université Paris Diderot); Novartis: Consultancy. Zweegman:Takeda: Membership on an entity's Board of Directors or advisory committees, Research Funding; Celgene: Membership on an entity's Board of Directors or advisory committees, Research Funding; Janssen: Membership on an entity's Board of Directors or advisory committees, Research Funding. Harrison:Sanofi: Honoraria, Speakers Bureau; Shire: Speakers Bureau; Gilead: Honoraria; CTI Biopharma: Consultancy, Honoraria, Speakers Bureau; Novartis: Honoraria, Research Funding, Speakers Bureau. Cervantes:Sanofi-Aventis: Consultancy; Novartis: Consultancy, Speakers Bureau; CTI-Baxter: Consultancy, Speakers Bureau. Barbui:Novartis: Speakers Bureau. Etienne:ARIAD: Consultancy, Honoraria, Speakers Bureau; Novartis: Consultancy, Honoraria, Other: Congress Travel/Accomodations, Research Funding, Speakers Bureau; BMS: Consultancy, Honoraria, Speakers Bureau. Roy:Novartis: Consultancy, Research Funding; BMS: Consultancy, Research Funding. te Boekhorst:Novartis: Consultancy; CTI Biopharma: Consultancy. Vannucchi:Novartis: Membership on an entity's Board of Directors or advisory committees, Speakers Bureau; Shire: Speakers Bureau; Novartis: Other: Research Funding paid to institution (University of Florence), Research Funding; Baxalta: Membership on an entity's Board of Directors or advisory committees. Mesa:Novartis. Research- incyte, Gilead, cti, Genentech, promedior, NS Pharma: Consultancy.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal