Abstract
Introduction: As clinical evidence has mounted in support of novel agents and longer treatment (Tx) durations for patients (pts) with newly diagnosed multiple myeloma (NDMM), questions have arisen regarding the economic impact of extending time to progression (TTP) in these pts, and the cost consequences once pts relapse and move to a second line of Tx. Previous analysis showed that relapsed myeloma pts incurred higher monthly costs once they advanced to later lines of Tx (Gaultney, 2013). There is limited information on the cost patterns of MM pts before and after their first relapse. A claims analysis was performed to evaluate the patterns of total direct costs of care, from Tx initiation until progression, for NDMM patients and for newly relapsed patients treated with novel agents, utilizing time to next therapy (TTNT) as a proxy measure for progression.
Methods: A retrospective study was conducted using a large US medical and pharmacy claims database, covering > 25 million lives annually. NDMM patients were identified with at least 2 outpatient claims or 1 inpatient medical claim associated with a diagnosis of MM (ICD-9-CM] code 203.0X), with the first such claim used to define the index date. Inclusion criteria required a minimum of 12 months' pre-index enrollment and 6 months' post-index continuous enrollment between 2006 and 2012. Pts with claims for stem cell transplantation (SCT) were excluded, to avoid confounding results from various factors based on timing, costs, and site of care of SCT. The analysis focused on NDMM and relapsed MM pts receiving lenalidomide (LEN)- or bortezomib (BORT)- based Tx, where complete claim history was available from Tx onset to initiation of subsequent Tx. Using methods similar to those described by Gaultney, patients' average monthly costs were determined, including medical (inpatient, ambulatory, and emergency room) and pharmacy (index and other drugs) costs, and total cost patterns over quarterly time periods were calculated. Average Charlson comorbidity scores were determined to compare baseline measures between pt groups.
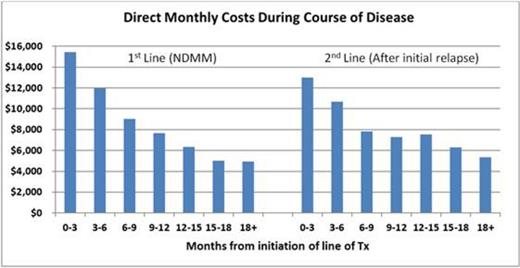
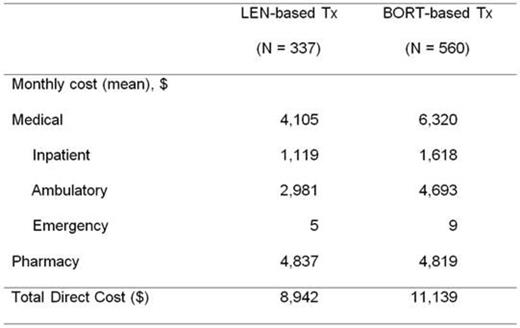
Results: 897 NDMM pts and 280 relapsed MM pts were identified with complete data through initiation of subsequent Tx. Monthly total direct costs for NDMM pts were $15,400 in the first 3 months (mos) of Tx, and declined each quarter, reaching approximately $5,000/mo at 18+ mos. At relapse, monthly costs increased to over $12,000 for the first 3 mos and followed a quarterly pattern of reduction similar to that seen for NDMM pts (Fig 1). Quarterly cost reduction patterns were consistent for patients treated with LEN or BORT for both NDMM and relapsed pts. Pts' total monthly NDMM costs over the full TTNT period averaged $8,942 with LEN vs. $11,139 for BORT (due to 54% higher monthly medical costs for BORT), while monthly drug costs were nearly identical (Table 1). The baseline Charlson comorbidity index was similar between Tx groups in both lines of Tx.
Direct monthly costs (medical and pharmacy) for LEN- and BORT-based treatments
Table 1: Direct monthly costs for NDMM pts
Conclusions: For a population of NDMM pts receiving either LEN- or BORT-based Tx without SCT, followed until TTNT, total direct monthly costs per pt declined steadily over time, decreasing by 68% from the initial quarter to the period post 18 mos. Costs spiked when pts began 2nd-line therapy, then followed a similar pattern of decline over time. This pattern may suggest that further extending the TTP for NDMM pts may also yield economic benefits for each month extended before relapse. Patterns of cost decline were similar between the LEN and BORT groups, for NDMM and for relapsed patients, although mean monthly total costs were lower for NDMM pts receiving LEN-based Tx due to lower medical costs and similar drug costs.
Arikian:Genesis Research: Consultancy. Off Label Use: Lenalidomide in newly diagnosed multiple myeloma patients . Milentijevic:Celgene Corporation: Consultancy. Binder:Celgene Corporation: Employment, Equity Ownership. Monzini:Celgene Corporation: Employment, Equity Ownership. Hu:Celgene Corporation: Employment. Nagarwala:Celgene Corporation: Employment. Hussein:Celgene Corporation: Employment. Corvino:Genesis Research LLC: Consultancy. Surinach:Genesis Research LLC: Consultancy. Usmani:Celgene Corporation: Consultancy, Honoraria, Research Funding; Millennium: Consultancy, Honoraria; Onyx: Consultancy, Honoraria, Research Funding; Sanofi: Consultancy; Array BioPharma: Research Funding; Janssen: Research Funding; Pharmacyclics: Research Funding.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal