Key Points
Small TP53 mutated subclones have the same unfavorable prognostic impact as clonal TP53 defects in chronic lymphocytic leukemia.
Abstract
TP53 mutations are strong predictors of poor survival and refractoriness in chronic lymphocytic leukemia (CLL) and have direct implications for disease management. Clinical information on TP53 mutations is limited to lesions represented in >20% leukemic cells. Here, we tested the clinical impact and prediction of chemorefractoriness of very small TP53 mutated subclones. The TP53 gene underwent ultra-deep-next generation sequencing (NGS) in 309 newly diagnosed CLL. A robust bioinformatic algorithm was established for the highly sensitive detection of few TP53 mutated cells (down to 3 out of ∼1000 wild-type cells). Minor subclones were validated by independent approaches. Ultra-deep-NGS identified small TP53 mutated subclones in 28/309 (9%) untreated CLL that, due to their very low abundance (median allele frequency: 2.1%), were missed by Sanger sequencing. Patients harboring small TP53 mutated subclones showed the same clinical phenotype and poor survival (hazard ratio = 2.01; P = .0250) as those of patients carrying clonal TP53 lesions. By longitudinal analysis, small TP53 mutated subclones identified before treatment became the predominant population at the time of CLL relapse and anticipated the development of chemorefractoriness. This study provides a proof-of-principle that very minor leukemia subclones detected at diagnosis are an important driver of the subsequent disease course.
Introduction
TP53 mutations represent strong predictors of poor survival and refractoriness in chronic lymphocytic leukemia (CLL)1-7 and, for these reasons, they have a well-established clinical relevance and direct implications for the management of this leukemia.8-11 To date, information on the clinical relevance of TP53 mutations in CLL is limited to lesions that are clonally represented in the leukemic population, as revealed by Sanger sequencing that is the most widely adopted method to assess TP53 mutation status in this leukemia.4-7,12,13
Next generation sequencing (NGS) technologies provide a novel opportunity to examine in depth the clonal heterogeneity of the CLL genome, with the potential for sensitive detection of mutations restricted to a small fraction of the total tumor cell population. Exploiting these approaches, recent genomic studies have disclosed the complexity of CLL clonal architecture and provided the proof-of-principle that genetically diverse subclones may be admixed with a dominant leukemic clone.12-15 Although genomic studies have depicted the landscape of the clonal complexity of CLL, little is known about the clinical implications and dynamics of very small subclones that may be present, but are commonly undetected, in the leukemic cell population.14-17
Understanding the significance of small CLL subclones might be particularly important if they are driven by genetic lesions associated with treatment resistance, such as TP53 mutations. In this respect, analysis of the subclonal architecture of TP53 mutations in the early disease phases may help anticipate the genetic composition of later phases of the disease, including chemorefractoriness and relapse, and may also predict the disease ultimate clinical course. In this study, by using a highly sensitive ultra-deep-NGS approach capable of detecting few mutated cells, we tested the clinical impact of small TP53 mutated subclones on CLL outcome.
Patients and methods
Patients
The study population was a consecutive series of 309 newly diagnosed CLL patients (Table 1) who were prospectively registered in the Amedeo Avogadro University CLL-database from December 1996 through October 2011. CLL diagnosis was according to International Workshop on CLL-National Cancer Institute (IWCLL-NCI) criteria.9 Fifty-three cases presented with symptomatic disease according to guidelines9 and were therefore treated at diagnosis. The study population was provided with sequential tumor samples and clinical information prospectively collected at clinically relevant time points. The database was updated in May 2013. The median follow-up of living patients was 8.1 years. No patient was lost to follow-up.
Characteristics of the whole CLL series of patients harboring solely subclonal TP53 mutations, and of patients harboring clonal TP53 mutations
| Characteristics* . | All (n = 309) . | Solely subclonal TP53 mutations (n = 18) . | Clonal TP53 mutations (n = 28) . | . | |||
|---|---|---|---|---|---|---|---|
| N . | % . | n . | % . | N . | % . | P‡ . | |
| Age >70 y | 160 | 51.8 | 11 | 61.1 | 19 | 67.9 | .6391 |
| Male | 165 | 53.4 | 10 | 55.6 | 19 | 67.9 | .3988 |
| Binet A | 245 | 79.3 | 13 | 72.2 | 16 | 57.1 | .5848 |
| Binet B | 37 | 12.0 | 2 | 11.1 | 5 | 17.9 | |
| Binet C | 27 | 8.7 | 3 | 16.7 | 7 | 25.0 | |
| IGHV identity >98%† | 108 | 35.5 | 6 | 35.3 | 13 | 46.4 | .4634 |
| Stereotyped VH CDR3† | 68 | 22.4 | 6 | 35.3 | 8 | 28.6 | .6367 |
| 13q14 deletion | 158 | 51.1 | 12 | 66.7 | 17 | 60.7 | .6831 |
| Trisomy 12 | 64 | 20.7 | 5 | 27.8 | 3 | 10.7 | .2316 |
| 11q22-q23 deletion | 24 | 7.8 | 2 | 11.1 | 2 | 7.1 | .6386 |
| 17p13 deletion | 29 | 9.4 | 3 | 16.7 | 22 | 78.6 | <.0001 |
| NOTCH1 mutations | 34 | 11.0 | 1 | 5.6 | 3 | 10.7 | 1.00 |
| SF3B1 mutations | 22 | 7.1 | 3 | 16.7 | 3 | 10.7 | .6655 |
| BIRC3 deletion | 13 | 4.2 | 1 | 5.6 | 2 | 7.1 | 1.00 |
| BIRC3 mutations | 7 | 2.3 | 0 | 0 | 0 | 0 | — |
| BIRC3 disruption | 17 | 5.5 | 1 | 5.6 | 2 | 7.1 | 1.00 |
| MYD88 mutations | 10 | 3.2 | 0 | 0 | 0 | 0 | — |
| Characteristics* . | All (n = 309) . | Solely subclonal TP53 mutations (n = 18) . | Clonal TP53 mutations (n = 28) . | . | |||
|---|---|---|---|---|---|---|---|
| N . | % . | n . | % . | N . | % . | P‡ . | |
| Age >70 y | 160 | 51.8 | 11 | 61.1 | 19 | 67.9 | .6391 |
| Male | 165 | 53.4 | 10 | 55.6 | 19 | 67.9 | .3988 |
| Binet A | 245 | 79.3 | 13 | 72.2 | 16 | 57.1 | .5848 |
| Binet B | 37 | 12.0 | 2 | 11.1 | 5 | 17.9 | |
| Binet C | 27 | 8.7 | 3 | 16.7 | 7 | 25.0 | |
| IGHV identity >98%† | 108 | 35.5 | 6 | 35.3 | 13 | 46.4 | .4634 |
| Stereotyped VH CDR3† | 68 | 22.4 | 6 | 35.3 | 8 | 28.6 | .6367 |
| 13q14 deletion | 158 | 51.1 | 12 | 66.7 | 17 | 60.7 | .6831 |
| Trisomy 12 | 64 | 20.7 | 5 | 27.8 | 3 | 10.7 | .2316 |
| 11q22-q23 deletion | 24 | 7.8 | 2 | 11.1 | 2 | 7.1 | .6386 |
| 17p13 deletion | 29 | 9.4 | 3 | 16.7 | 22 | 78.6 | <.0001 |
| NOTCH1 mutations | 34 | 11.0 | 1 | 5.6 | 3 | 10.7 | 1.00 |
| SF3B1 mutations | 22 | 7.1 | 3 | 16.7 | 3 | 10.7 | .6655 |
| BIRC3 deletion | 13 | 4.2 | 1 | 5.6 | 2 | 7.1 | 1.00 |
| BIRC3 mutations | 7 | 2.3 | 0 | 0 | 0 | 0 | — |
| BIRC3 disruption | 17 | 5.5 | 1 | 5.6 | 2 | 7.1 | 1.00 |
| MYD88 mutations | 10 | 3.2 | 0 | 0 | 0 | 0 | — |
IGHV, immunoglobulin heavy variable gene; CDR3, complementarity determining region 3.
IGHV mutation status was assessable in 304 patients; 5 patients lacked productive IGHV-IGHD-IGHJ rearrangements.
P value for the comparison between cases harboring solely subclonal TP53 mutations vs clonal TP53 mutations.
The study was designed to assess differences in overall survival (OS) between cases harboring a wild-type TP53 gene and cases harboring small TP53 mutated subclones. The exact prevalence of small TP53 mutated subclones in CLL is currently unknown. Assuming that small TP53 mutated subclones occur in at least 10% of the population, we estimated that 309 patients would allow detecting at least a 25% difference in 5-year OS between patients harboring a wild-type TP53 gene (5-year OS = 75%) and patients harboring small TP53 mutated subclones (5-year OS = 50%) (power = 81%; α = 0.01).
The REMARK criteria were followed throughout this study (supplemental Table 1, available on the Blood Web site).18 Patients provided informed consent in accordance with local institutional review board requirements and the Declaration of Helsinki. The study was approved by the Ethical Committee of the Ospedale Maggiore della Carità di Novara associated with the Amedeo Avogadro University of Eastern Piedmont (protocol code 59/CE; study number CE 8/11).
Specimen characteristics
TP53 mutation screening was performed on peripheral blood (PB) mononuclear cell samples collected at CLL diagnosis. Clonal evolution analysis was performed on PB mononuclear cell samples collected at progression requiring treatment, relapse, and last follow-up. In all cases, the fraction of tumor cells corresponded to 70% to 98% as assessed by flow cytometry. To account for tumor representation, the frequency of the mutant TP53 alleles provided by ultra-deep-NGS was corrected for the proportion of CD19+/CD5+ cells in each sample.
TP53 sequencing
Ultra-deep-NGS of the TP53 mutation hotspots (exons 4-8, including splicing sites) was performed using the 454 chemistry and was based on amplicon libraries. The TP53 region of interest was covered by 6 sequence-specific primer pairs, each flanked by tagged sequences to barcode the samples (supplemental Table 2). In each experiment, 60 amplicons, corresponding to the TP53 region of interest of 10 distinct patients, were amplified from genomic DNA by using a high-fidelity Taq polimerase (FastStart High Fidelity PCR System; Roche Diagnostics) and subjected to ultra-deep-NGS on the Genome Sequencer Junior (454 Life Sciences) to obtain a ∼2000-fold coverage per amplicon. Through this approach, the average sequencing coverage across TP53 target regions was 2660× and >87% of the sequenced amplicons had sequence coverage of >1000× TP53 mutation analysis was also performed in parallel by Sanger sequencing as previously reported.4 Further details are available in the supplemental Appendix.
Establishment of a bioinformatic approach to call subclonal TP53 mutations out of the background error noise
To establish a robust bioinformatic approach to call subclonal TP53 mutations of low abundance out of the background error noise of deep-NGS, a pivotal dilution experiment was performed. This experiment allowed us to: 1) calibrate ultra-deep-NGS for systematic biases that lead to sequencing errors; 2) derive the distribution of sequencing errors; 3) determine the sequencing depth required for a highly sensitive detection of small (<0.5% allele frequency) mutations out of the background error noise; and 4) statistically test the confidence in discovering subclonal events (supplemental Figures 1-4). The dilution experiment established the negative binomial distribution as the best fit for ultra-deep-NGS error distribution (supplemental Methods; supplemental Figure 2) that was used to estimate statistical frequency thresholds above which true subclonal mutations are distinguished from the background error noise (supplemental Figures 3 and 4).19-24 Based on these observations, a robust bioinformatic workflow was established to call subclonal TP53 variants from ultra-deep-NGS experiments in patient samples. By this approach, we were able to detect subclonal TP53 mutations represented in at least 0.3% of the alleles (3 mutated alleles out of 1000 alleles) (supplemental Figures 2 and 3). Further details of the bioinformatic algorithm are available in the supplemental Appendix.
Validation of small TP53 mutated subclones
Small TP53 mutated subclones called by the bioinformatic algorithm were validated by a double-step experimental approach. In the first step,25 subclonal variants were subjected to independent polymerase chain reaction (PCR) amplification and ultra-deep-NGS sequencing experiments using the same experimental conditions and coverage described above. In the second step, subclonal TP53 variants were further validated by allele specific PCR (AS-PCR).26 Further details are available in the supplemental Appendix.
Databases
TP53 mutations were annotated using the IARC TP53 database.27 For each TP53 missense mutation, the CDKN1A promoter-specific transcriptional activity measured in yeast functional assays was extracted and expressed as percent of wild-type activity.28 The molecular and functional profiles of clonal TP53 mutations in CLL were derived from public databases.29
Statistical analysis
OS from diagnosis was the primary end point and was measured from date of initial presentation to date of death from any cause (event) or last follow-up (censoring). Analysis of OS from first treatment was a secondary and exploratory end point, included 53 newly diagnosed patients who presented with symptomatic disease requiring treatment, and was measured from date of first treatment to date of death from any cause (event) or last follow-up (censoring). Molecular studies were blinded to the study end points. Survival analysis was performed by the Kaplan-Meier method.30 To test the independence of the prognostic value of small TP53 mutated subclones on OS, we performed a comprehensive multivariate Cox analysis with backward-stepwise elimination of nonsignificant covariates.31 None of the covariates violated the proportional hazard regression assumptions.32,33 Bias corrected c-index, calibration slope, and heuristic shrinkage estimator of the Cox model were calculated.32-37 Cox model stability was internally validated using bootstrapping procedures.32-37 These approaches provided an estimate of prediction accuracy of the Cox model to protect against overfitting. The maximally selected rank statistics was used to identify a cutoff in the size of the TP53 mutated clone to best predict OS. Categorical variables were compared by χ-square test and Fisher’s exact test. Continuous variables were compared by Mann-Whitney test. The Bonferroni test was used to correct for multiple comparisons. All statistical tests were 2-sided. Statistical significance was defined as P < .05. The analysis was performed with SPSS (version 21.0) and R statistical package 3.0.1. Further details of the statistical analysis are available in the supplemental Appendix.
Results
Small TP53 mutated subclones occur in a significant fraction of newly diagnosed CLL
We established an ultra-deep-NGS strategy coupled with a robust bioinformatic algorithm for the highly sensitive detection of small mutated subclones in CLL. The sensitivity of the ultra-deep-NGS approach allowed to detect mutant allele fractions down to 0.3% (3 mutant alleles in a background of ∼1000 wild-type alleles) with a 95% confidence interval (CI) of 0.2% to 0.5%. Highly sensitive ultra-deep-NGS was then applied to identify small TP53 mutated subclones in a consecutive series of 309 newly diagnosed CLL patients (Table 1). Ultra-deep-NGS identified 85 TP53 mutations in 14.8% (46/309) of CLL patients (Figure 1A). All mutations that had been detected by Sanger sequencing (ie, clonal TP53 mutations: 35 in 28 patients, 9.0%) were also identified by ultra-deep-NGS.
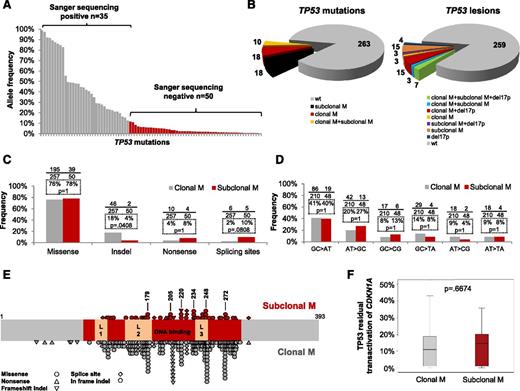
Molecular profile of subclonal TP53 mutations. (A) Allele frequency of the 85 TP53 mutations identified by ultra-deep-NGS. Mutations are ordered according to their allelic abundance. Mutations that tested positive (clonal mutations: gray bars) and negative (subclonal mutations: red bars) by Sanger sequencing are indicated. (B) Prevalence of TP53 lesions according to their clonal representation in the study cohort of 309 newly diagnosed CLL (for each category, the crude number of patients is represented). (C) Comparison of the molecular profile of subclonal mutations from the CLL study cohort (n = 50) vs clonal mutations from public CLL databases (n = 257; see Zenz et al29 ). p, P values by Fisher's exact test corrected for multiple hypothesis testing. (D) Comparison of the transition/transversion profile between subclonal TP53 substitutions from the CLL study cohort (n = 48) and clonal TP53 substitutions from public CLL databases (n = 210; see Zenz et al29 ). p, P values by Fisher's exact test corrected for multiple hypothesis testing. (E) Schematic diagram of the TP53 protein with its conserved functional domains. Color-coded shapes indicate the position of subclonal TP53 mutations from the CLL study cohort (n = 50; red shapes) and clonal TP53 mutations from public CLL databases (n = 257; gray shapes; see Zenz et al29 ). Hot spot codons recurrently affected by both subclonal and clonal TP53 mutations are highlighted. (F) Residual CDKN1A transactivation capacity of subclonal TP53 missense substitutions from the CLL study cohort (n = 39; red box) vs clonal TP53 missense substitutions from public CLL databases (n = 193; gray box; see Zenz et al29 ). The band inside the box is the median value. The bottom and top of the box are the 25th and 75th quartiles. The ends of the whiskers are the second percentile and the 98th percentile. p, P value by Mann-Whitney test.
Molecular profile of subclonal TP53 mutations. (A) Allele frequency of the 85 TP53 mutations identified by ultra-deep-NGS. Mutations are ordered according to their allelic abundance. Mutations that tested positive (clonal mutations: gray bars) and negative (subclonal mutations: red bars) by Sanger sequencing are indicated. (B) Prevalence of TP53 lesions according to their clonal representation in the study cohort of 309 newly diagnosed CLL (for each category, the crude number of patients is represented). (C) Comparison of the molecular profile of subclonal mutations from the CLL study cohort (n = 50) vs clonal mutations from public CLL databases (n = 257; see Zenz et al29 ). p, P values by Fisher's exact test corrected for multiple hypothesis testing. (D) Comparison of the transition/transversion profile between subclonal TP53 substitutions from the CLL study cohort (n = 48) and clonal TP53 substitutions from public CLL databases (n = 210; see Zenz et al29 ). p, P values by Fisher's exact test corrected for multiple hypothesis testing. (E) Schematic diagram of the TP53 protein with its conserved functional domains. Color-coded shapes indicate the position of subclonal TP53 mutations from the CLL study cohort (n = 50; red shapes) and clonal TP53 mutations from public CLL databases (n = 257; gray shapes; see Zenz et al29 ). Hot spot codons recurrently affected by both subclonal and clonal TP53 mutations are highlighted. (F) Residual CDKN1A transactivation capacity of subclonal TP53 missense substitutions from the CLL study cohort (n = 39; red box) vs clonal TP53 missense substitutions from public CLL databases (n = 193; gray box; see Zenz et al29 ). The band inside the box is the median value. The bottom and top of the box are the 25th and 75th quartiles. The ends of the whiskers are the second percentile and the 98th percentile. p, P value by Mann-Whitney test.
Ultra-deep-NGS identified 50 additional subclonal TP53 mutations that, due to their very low abundance (median allele frequency corrected for tumor representation: 2.1%; range: 0.3% to 11%) in the tumor clone, were missed by Sanger sequencing (Figure 1A; supplemental Table 3). All subclonal TP53 mutations were validated by at least 2 independent ultra-deep-NGS experiments and further confirmed on a different experimental platform by AS-PCR (Figure 2). Subclonal TP53 mutations were the sole TP53 variant in 5.8% (18/309) of CLL, while they coexisted in the same leukemic population along with a clonal TP53 mutation in 3.2% (10/309) of cases (Figure 1B). By also considering 17p13 deletion among the genetic defects targeting the TP53 gene, subclonal TP53 mutations were the sole TP53 lesion in 4.8% (15/309) of CLL (Figure 1B). Overall, patients carrying solely subclonal mutations accounted for 30% (15/50) of all cases harboring TP53 defects in this study cohort.
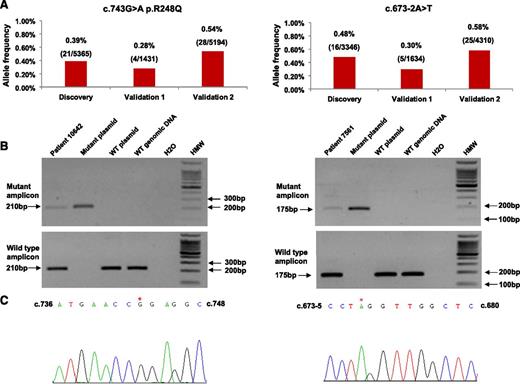
Experimental validation of subclonal TP53 mutations identified by ultra-deep-NGS. (A) Representation of the variant frequency of 2 exemplificative subclonal TP53 mutations (c.743G>A p.R248Q and c.673-2A>T) of very low allelic abundance (<0.5%). The first bar of the graphs shows the variant allele frequency in the discovery ultra-deep-NGS experiment. The second and third bars show the variant allele frequency in independent ultra-deep-NGS validation experiments. The number of mutated read outs of the total number of reads covering the variant position is reported. (B) Conventional agarose-gel electrophoresis of the AS-PCR products. Patient 10642, harboring the subclonal TP53 c.743G>A p.R248Q missense substitution (left), and patient 7561, harboring the subclonal TP53 c.673-2A>T splice site mutation (right), are represented. After AS-PCR for the mutant allele, a mutation-specific band is amplified from the patient sample and from the mutated plasmid DNA (positive control). No bands are amplified from the wild-type plasmid DNA and the wild-type genomic DNA from a healthy donor (negative controls), thus confirming the specificity of the assay. (C) Due to their low clonal abundance (<0.5%), the subclonal TP53 c.743G>A p.R248Q missense substitution (left) and the subclonal TP53 c.673-2A>T splice site mutation (right) are not detectable by conventional Sanger sequencing in patient 10 642 and patient 7561, respectively. Asterisks point to the positions of the subclonal variants.
Experimental validation of subclonal TP53 mutations identified by ultra-deep-NGS. (A) Representation of the variant frequency of 2 exemplificative subclonal TP53 mutations (c.743G>A p.R248Q and c.673-2A>T) of very low allelic abundance (<0.5%). The first bar of the graphs shows the variant allele frequency in the discovery ultra-deep-NGS experiment. The second and third bars show the variant allele frequency in independent ultra-deep-NGS validation experiments. The number of mutated read outs of the total number of reads covering the variant position is reported. (B) Conventional agarose-gel electrophoresis of the AS-PCR products. Patient 10642, harboring the subclonal TP53 c.743G>A p.R248Q missense substitution (left), and patient 7561, harboring the subclonal TP53 c.673-2A>T splice site mutation (right), are represented. After AS-PCR for the mutant allele, a mutation-specific band is amplified from the patient sample and from the mutated plasmid DNA (positive control). No bands are amplified from the wild-type plasmid DNA and the wild-type genomic DNA from a healthy donor (negative controls), thus confirming the specificity of the assay. (C) Due to their low clonal abundance (<0.5%), the subclonal TP53 c.743G>A p.R248Q missense substitution (left) and the subclonal TP53 c.673-2A>T splice site mutation (right) are not detectable by conventional Sanger sequencing in patient 10 642 and patient 7561, respectively. Asterisks point to the positions of the subclonal variants.
These data indicate that ultra-deep-NGS significantly adds to the analysis of TP53 genetic defects in CLL by allowing the identification of small TP53 mutated subclones among patients that would be otherwise considered wild type for the TP53 gene according to Sanger sequencing.
Subclonal mutations have the same detrimental impact on TP53 function as clonal defects
The molecular profile and functional impact of subclonal TP53 mutations was dissected to discriminate whether they act as pathogenic drivers or as irrelevant passengers in CLL. Subclonal TP53 mutations were mainly missense substitutions (78%, 39/50) mapping in the DNA-binding domain of the TP53 protein and recurrently affecting hotspot codons (ie, 179 and 248) that are known to be required for DNA binding (Figure 1C-E). These features predicted impairment of the transcriptional activation of TP53 response genes. Consistently, the median residual transactivational activity of subclonal TP53 mutations toward the CDKN1A (p21) promoter was only 14.5% (interquartile range: 0.9% to 20.5%) compared with wild-type TP53 (Figure 1F).28 The remaining subclonal TP53 mutations were splice site (10%, 5/50), nonsense (8%, 4/50), and indel (4%, 2/50) variants that were selected to truncate or entirely remove the DNA binding domain of TP53 (Figure 1C). Overall, the molecular and functional profiles of subclonal TP53 mutations did not significantly differ from those of TP53 variants that gained clonal representation in CLL (Figure 1).29
These data indicate that subclonal TP53 mutations do not represent random passenger events but instead negatively impact on TP53 function as clonal TP53 variants.
Small TP53 mutated subclones have the same unfavorable prognostic impact as clonal defects
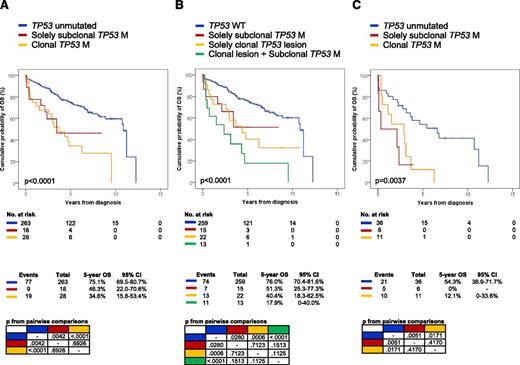
Cases harboring solely subclonal TP53 mutations and cases harboring clonal TP53 variants shared the same clinical and immunogenetic picture at presentation (Table 1; supplemental Figure 6) and showed a similarly poor clinical course. By univariate analysis, the OS of cases harboring solely subclonal TP53 mutations was significantly shorter (5-year OS: 46.3%; P = .0042) than that of cases with an unmutated TP53 gene (5-year OS: 75.1%) and was similar to that of cases harboring clonal TP53 mutations (5-year OS: 34.6%; P = .6926) (Table 2; Figure 3A).
Univariate and multivariate analysis of OS
| . | . | . | . | . | . | . | . | . | . | Multivariate analysis . | Internal bootstrapping validation . | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Univariate analysis . | Initial full model . | Final model . | Bootstrap parameters (mean) . | Bootstrap selection (%) . | |||||||||||||||||
| Events . | Total . | 5-y OS (%) . | LCI . | UCI . | HR . | LCI . | UCI . | P . | HR . | LCI . | UCI . | P . | HR . | LCI . | UCI . | P . | HR . | LCI . | UCI . | ||
| Age <70 y | 31 | 149 | 81.9 | 75.3 | 88.5 | — | — | — | <.0001 | — | — | — | <.0001 | — | — | — | <.0001 | — | — | — | 100 |
| Age >70 y | 74 | 160 | 57.7 | 49.3 | 64.1 | 3.19 | 2.06 | 4.94 | 3.42 | 2.14 | 5.46 | 3.23 | 2.05 | 5.11 | 3.40 | 2.11 | 5.48 | ||||
| Female | 47 | 144 | 70.2 | 62.0 | 78.4 | — | — | — | .3319 | — | — | — | .6376 | — | — | — | — | — | — | — | — |
| Male | 58 | 165 | 68.7 | 61.1 | 76.3 | 1.21 | 0.82 | 1.70 | 1.10 | 0.72 | 1.68 | — | — | — | — | — | — | ||||
| Binet A | 66 | 245 | 75.8 | 70.0 | 81.6 | — | — | — | <.0001* | — | — | — | .0349* | — | — | — | .0079* | — | — | — | 92 |
| Binet B | 19 | 37 | 53.1 | 34.9 | 71.3 | 1.97 | 1.18 | 3.30 | 1.46 | 0.84 | 2.53 | 1.52 | 0.89 | 2.60 | 1.36 | 0.78 | 2.17 | ||||
| Binet C | 20 | 27 | 33.9 | 15.3 | 52.5 | 3.77 | 2.24 | 6.32 | 2.28 | 1.20 | 4.33 | 2.56 | 1.39 | 4.71 | 2.24 | 1.31 | 4.13 | ||||
| IGHV homology <98% | 55 | 196 | 76.4 | 69.9 | 82.9 | — | — | — | .0039 | — | — | — | .6647 | — | — | — | — | — | — | — | — |
| IGHV homology >98% | 49 | 108 | 55.6 | 45.2 | 66.0 | 1.77 | 1.29 | 2.61 | 1.11 | 0.68 | 1.80 | — | — | — | — | — | — | ||||
| No subclonal TP53 mutations | 87 | 281 | 73.0 | 67.3 | 78.7 | — | — | — | <.0001 | — | — | — | .0252 | — | — | — | .0250 | — | — | — | 74 |
| Subclonal TP53 mutations | 18 | 28 | 34.5 | 15.5 | 53.5 | 3.22 | 1.93 | 5.38 | 2.03 | 1.09 | 3.77 | 2.01 | 1.24 | 4.38 | 2.12 | 1.13 | 3.99 | ||||
| No 11q22-q23 deletion | 91 | 285 | 71.2 | 65.5 | 76.9 | — | — | — | .0035 | — | — | — | .3087 | — | — | — | — | — | — | — | — |
| 11q22-q23 deletion | 14 | 24 | 46.4 | 22.3 | 70.5 | 2.42 | 1.33 | 4.39 | 1.55 | 0.66 | 3.64 | — | — | — | — | — | — | ||||
| No clonal TP53 lesions† | 81 | 274 | 74.6 | 68.9 | 80.3 | — | — | — | <.0001 | — | — | — | .0273 | — | — | — | .0201 | — | — | — | 79 |
| Clonal TP53 lesions† | 24 | 35 | 31.9 | 15.2 | 48.6 | 3.28 | 2.07 | 5.20 | 1.88 | 1.07 | 3.31 | 1.91 | 1.10 | 3.32 | 2.11 | 1.19 | 3.74 | ||||
| No NOTCH1 mutations | 85 | 275 | 72.5 | 66.8 | 78.2 | — | — | — | .0015 | — | — | — | .0221 | — | — | — | .0107 | — | — | — | 85 |
| NOTCH1 mutations | 20 | 34 | 36.3 | 18.3 | 54.3 | 2.20 | 1.35 | 3.59 | 1.97 | 1.10 | 3.54 | 2.00 | 1.17 | 3.42 | 2.18 | 1.25 | 3.82 | ||||
| No SF3B1 mutations | 93 | 287 | 70.8 | 65.1 | 76.5 | — | — | — | .0014 | — | — | — | .0109 | — | — | — | .0114 | — | — | — | 79 |
| SF3B1 mutations | 12 | 22 | 53.0 | 31.4 | 74.6 | 2.67 | 1.45 | 4.88 | 2.35 | 1.21 | 4.55 | 2.31 | 1.20 | 4.44 | 2.60 | 1.30 | 5.19 | ||||
| No BIRC3 disruption‡ | 94 | 292 | 71.0 | 65.3 | 76.7 | — | — | — | .0008 | — | — | — | .1319 | — | — | — | .0032 | — | — | — | 88 |
| BIRC3 disruption‡ | 11 | 17 | 41.6 | 15.9 | 67.3 | 2.92 | 1.56 | 5.48 | 1.94 | 0.82 | 4.50 | 2.62 | 1.38 | 4.99 | 2.77 | 1.41 | 5.46 | ||||
| . | . | . | . | . | . | . | . | . | . | Multivariate analysis . | Internal bootstrapping validation . | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Univariate analysis . | Initial full model . | Final model . | Bootstrap parameters (mean) . | Bootstrap selection (%) . | |||||||||||||||||
| Events . | Total . | 5-y OS (%) . | LCI . | UCI . | HR . | LCI . | UCI . | P . | HR . | LCI . | UCI . | P . | HR . | LCI . | UCI . | P . | HR . | LCI . | UCI . | ||
| Age <70 y | 31 | 149 | 81.9 | 75.3 | 88.5 | — | — | — | <.0001 | — | — | — | <.0001 | — | — | — | <.0001 | — | — | — | 100 |
| Age >70 y | 74 | 160 | 57.7 | 49.3 | 64.1 | 3.19 | 2.06 | 4.94 | 3.42 | 2.14 | 5.46 | 3.23 | 2.05 | 5.11 | 3.40 | 2.11 | 5.48 | ||||
| Female | 47 | 144 | 70.2 | 62.0 | 78.4 | — | — | — | .3319 | — | — | — | .6376 | — | — | — | — | — | — | — | — |
| Male | 58 | 165 | 68.7 | 61.1 | 76.3 | 1.21 | 0.82 | 1.70 | 1.10 | 0.72 | 1.68 | — | — | — | — | — | — | ||||
| Binet A | 66 | 245 | 75.8 | 70.0 | 81.6 | — | — | — | <.0001* | — | — | — | .0349* | — | — | — | .0079* | — | — | — | 92 |
| Binet B | 19 | 37 | 53.1 | 34.9 | 71.3 | 1.97 | 1.18 | 3.30 | 1.46 | 0.84 | 2.53 | 1.52 | 0.89 | 2.60 | 1.36 | 0.78 | 2.17 | ||||
| Binet C | 20 | 27 | 33.9 | 15.3 | 52.5 | 3.77 | 2.24 | 6.32 | 2.28 | 1.20 | 4.33 | 2.56 | 1.39 | 4.71 | 2.24 | 1.31 | 4.13 | ||||
| IGHV homology <98% | 55 | 196 | 76.4 | 69.9 | 82.9 | — | — | — | .0039 | — | — | — | .6647 | — | — | — | — | — | — | — | — |
| IGHV homology >98% | 49 | 108 | 55.6 | 45.2 | 66.0 | 1.77 | 1.29 | 2.61 | 1.11 | 0.68 | 1.80 | — | — | — | — | — | — | ||||
| No subclonal TP53 mutations | 87 | 281 | 73.0 | 67.3 | 78.7 | — | — | — | <.0001 | — | — | — | .0252 | — | — | — | .0250 | — | — | — | 74 |
| Subclonal TP53 mutations | 18 | 28 | 34.5 | 15.5 | 53.5 | 3.22 | 1.93 | 5.38 | 2.03 | 1.09 | 3.77 | 2.01 | 1.24 | 4.38 | 2.12 | 1.13 | 3.99 | ||||
| No 11q22-q23 deletion | 91 | 285 | 71.2 | 65.5 | 76.9 | — | — | — | .0035 | — | — | — | .3087 | — | — | — | — | — | — | — | — |
| 11q22-q23 deletion | 14 | 24 | 46.4 | 22.3 | 70.5 | 2.42 | 1.33 | 4.39 | 1.55 | 0.66 | 3.64 | — | — | — | — | — | — | ||||
| No clonal TP53 lesions† | 81 | 274 | 74.6 | 68.9 | 80.3 | — | — | — | <.0001 | — | — | — | .0273 | — | — | — | .0201 | — | — | — | 79 |
| Clonal TP53 lesions† | 24 | 35 | 31.9 | 15.2 | 48.6 | 3.28 | 2.07 | 5.20 | 1.88 | 1.07 | 3.31 | 1.91 | 1.10 | 3.32 | 2.11 | 1.19 | 3.74 | ||||
| No NOTCH1 mutations | 85 | 275 | 72.5 | 66.8 | 78.2 | — | — | — | .0015 | — | — | — | .0221 | — | — | — | .0107 | — | — | — | 85 |
| NOTCH1 mutations | 20 | 34 | 36.3 | 18.3 | 54.3 | 2.20 | 1.35 | 3.59 | 1.97 | 1.10 | 3.54 | 2.00 | 1.17 | 3.42 | 2.18 | 1.25 | 3.82 | ||||
| No SF3B1 mutations | 93 | 287 | 70.8 | 65.1 | 76.5 | — | — | — | .0014 | — | — | — | .0109 | — | — | — | .0114 | — | — | — | 79 |
| SF3B1 mutations | 12 | 22 | 53.0 | 31.4 | 74.6 | 2.67 | 1.45 | 4.88 | 2.35 | 1.21 | 4.55 | 2.31 | 1.20 | 4.44 | 2.60 | 1.30 | 5.19 | ||||
| No BIRC3 disruption‡ | 94 | 292 | 71.0 | 65.3 | 76.7 | — | — | — | .0008 | — | — | — | .1319 | — | — | — | .0032 | — | — | — | 88 |
| BIRC3 disruption‡ | 11 | 17 | 41.6 | 15.9 | 67.3 | 2.92 | 1.56 | 5.48 | 1.94 | 0.82 | 4.50 | 2.62 | 1.38 | 4.99 | 2.77 | 1.41 | 5.46 | ||||
Total number of patients included in the multivariate analysis: 304; Events: 104; 5 patients lacked productive IGHV-IGHD-IGHJ rearrangements. Shrinkage coefficient of the final model: 0.92.
HR, hazard ratio; IGHV, immunoglobulin heavy variable gene; LCI, 95% lower CI; UCI, 95% upper CI.
P-trend.
Clonal TP53 mutations and/or 17p13 deletion.
BIRC3 mutations and/or BIRC3 deletion.
Kaplan-Meier estimates of OS of patients harboring small TP53 mutated subclones. (A) Comparison of OS from CLL diagnosis between patients harboring solely subclonal TP53 mutations, cases harboring clonal TP53 mutations, and cases harboring an unmutated TP53 gene. (B) Comparison of OS from CLL diagnosis between patients harboring solely subclonal TP53 mutations, cases harboring solely clonal TP53 lesions (ie, mutations or deletions), cases harboring clonal TP53 lesions coexisting with subclonal TP53 mutations, and cases harboring a wild-type TP53 gene. (C) Comparison of OS from first treatment between patients harboring solely subclonal TP53 mutations, cases harboring clonal TP53 mutations, and cases harboring an unmutated TP53 gene. p, P values by log-rank test.
Kaplan-Meier estimates of OS of patients harboring small TP53 mutated subclones. (A) Comparison of OS from CLL diagnosis between patients harboring solely subclonal TP53 mutations, cases harboring clonal TP53 mutations, and cases harboring an unmutated TP53 gene. (B) Comparison of OS from CLL diagnosis between patients harboring solely subclonal TP53 mutations, cases harboring solely clonal TP53 lesions (ie, mutations or deletions), cases harboring clonal TP53 lesions coexisting with subclonal TP53 mutations, and cases harboring a wild-type TP53 gene. (C) Comparison of OS from first treatment between patients harboring solely subclonal TP53 mutations, cases harboring clonal TP53 mutations, and cases harboring an unmutated TP53 gene. p, P values by log-rank test.
To assess the impact of the TP53 mutation load on CLL survival, we divided patients into subgroups according to their TP53 mutation abundance (0.3% to 1%, 1.1% to 10%, >10% of the variant allele frequency). By this analysis, patients harboring TP53 mutations, independent of the size of the clone, were characterized by a homogeneously poor outcome and showed an OS shorter than that of patients with a wild-type TP53 gene (supplemental Figure 7). Consistently, the maximally selected rank statistics failed to identify a cutoff in the size of the TP53 mutated clone capable of best predicting CLL OS (supplemental Figure 8). This analysis is indicative of a “yes/no effect” of TP53 mutations on CLL outcome irrespective of the abundance of the mutated clone.
Given the cooccurrence of TP53 mutations with 17p13 deletion (Table 1), this lesion was incorporated in survival analysis to assess the impact of subclonal mutations as the sole TP53 defect. Also by this approach, patients harboring solely subclonal TP53 mutations showed a significantly shorter OS than cases devoid of TP53 abnormalities. Conversely, the OS of patients carrying solely subclonal TP53 mutations was similar to that of cases with clonal TP53 genetic defects (Figure 3B).
The impact of small TP53 mutated subclones on CLL survival was independent of the potential confounding effects of other variables that are clinically relevant in this leukemia.2,4 By multivariate analysis for OS, CLL patients harboring small TP53 mutated subclones had a 2.0-fold increased risk of death (hazard ratio = 2.01; 95% CI, 1.24-4.38; P = .0250) after adjusting for age, gender, disease stage, co-occurrence of clonal TP53 lesions, and other biological prognostic factors (ie, IGHV mutation status, 11q22-23 deletion, mutations of NOTCH1 and SF3B1, and BIRC3 disruption) (Table 2). Notably, the adjusted hazard of death marked by small TP53 mutated subclones was similar in magnitude to that of clonally represented TP53 lesions (Table 2).
Overall, these data document that CLL patients harboring small TP53 mutated subclones have the same clinico-biological phenotype and poor outcome as patients in whom TP53 lesions are clonally represented in the tumor.
Small TP53 mutated subclones detected at diagnosis subsequently expand under the selective pressure of treatment
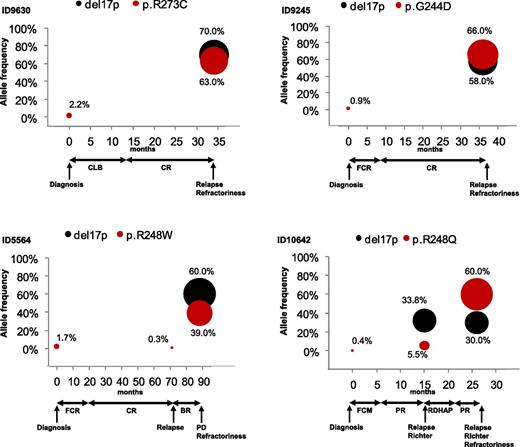
The dynamics of small TP53 mutated subclones was assessed by longitudinal ultra-deep-NGS analysis of sequential PB samples collected from patients immediately before first treatment and then at disease relapse (n = 13 patients; 61% treated with immuno-chemotherapy regimens). Among these cases, the small TP53 mutated subclones identified before treatment became the predominant tumor cell population at the time of CLL relapse (Figure 4). Selection of the small TP53 mutated subclones occurred independent of the type of treatment (ie, FCR, fludarabine-based combinations or alkylating agents). This may have resulted from the removal of the dominant TP53 wild-type clones by cytotoxic treatment, allowing the expansion of TP53 mutated subclones whose selection, because of their chemoresistance, was favored by ineffective therapies. In these patients, the expansion of small TP53 mutated subclones invariably paralleled the development of a chemorefractory phenotype.
Longitudinal analysis of clonal evolution in CLL patients harboring small TP53 mutated subclones. Graphical illustration of the kinetics of the TP53 mutated populations in 4 representative CLL patients who required treatment at diagnosis and who have been longitudinally investigated by deep-NGS. The x-axis represents time and the y-axis represents allele frequency. TP53 mutations and 17p13 deletion are represented by color-coded circles. The size of the circles is proportional to the allele frequency of the lesion. Arrows indicate the time point at which tumor samples were collected. The relationship between sample collection and treatments is also indicated. BR, bendamustine, rituximab; CLB, chlorambucil; CR, complete response according to the IWCLL-NCI criteria; FCM, fludarabine, cyclophosphamide, mitoxantrone; FCR, fludarabine, cyclophosphamide, rituximab; PD, progressive disease according to the IWCLL-NCI criteria; PR, partial response according to IWCLL-NCI criteria; RDHAP, rituximab, dexamethasone, high-dose cytarabine, cisplatin; Richter, Richter syndrome.
Longitudinal analysis of clonal evolution in CLL patients harboring small TP53 mutated subclones. Graphical illustration of the kinetics of the TP53 mutated populations in 4 representative CLL patients who required treatment at diagnosis and who have been longitudinally investigated by deep-NGS. The x-axis represents time and the y-axis represents allele frequency. TP53 mutations and 17p13 deletion are represented by color-coded circles. The size of the circles is proportional to the allele frequency of the lesion. Arrows indicate the time point at which tumor samples were collected. The relationship between sample collection and treatments is also indicated. BR, bendamustine, rituximab; CLB, chlorambucil; CR, complete response according to the IWCLL-NCI criteria; FCM, fludarabine, cyclophosphamide, mitoxantrone; FCR, fludarabine, cyclophosphamide, rituximab; PD, progressive disease according to the IWCLL-NCI criteria; PR, partial response according to IWCLL-NCI criteria; RDHAP, rituximab, dexamethasone, high-dose cytarabine, cisplatin; Richter, Richter syndrome.
We also examined sequential samples from 2 patients (interval between sampling 48 and 38 months, respectively) who harbored solely small TP53 mutated subclones at diagnosis and who did not require treatment during the clinical follow-up. In these 2 patients managed only by a watch-and-wait policy, the small TP53 mutated subclones did not increase in their size during the course of the disease (supplemental Figure 9).
Overall, these data indicate that chemotherapy is the major selective pressure favoring the expansion of TP53 mutated clones in CLL.
Small TP53 mutated subclones detected before treatment anticipate the development of a chemorefractory phenotype
Among CLL investigated at the time of treatment requirement (n = 53; 36% treated with FCR; supplemental Table 4), patients harboring small TP53 mutated subclones failed treatment and died of chemorefractoriness in a proportion similar to that of cases with clonal TP53 variants (Figure 3C). In fact, based on an exploratory analysis, the OS of cases harboring solely subclonal TP53 mutations was significantly shorter (5-year OS: 0%; P = .0171) than that of cases with an unmutated TP53 gene (5-year OS: 54.3%), and was similar to that of cases harboring clonal TP53 mutations (5-year OS: 12.1%; P = .4170) (Figure 3C).
These data indicate that, among patients requiring treatment, the detection of small TP53 mutated subclones in the early disease phases invariably anticipates the genetic composition of the disease at relapse and the development of a chemorefractory phenotype.
Discussion
This study shows that small TP53 mutated subclones detected by highly sensitive ultra-deep-NGS occur in a significant fraction of newly diagnosed CLL, have the same unfavorable prognostic impact as clonal TP53 defects, and anticipate the development of a chemorefractory phenotype among CLL patients requiring treatment.
TP53 mutation analysis is currently advised for proper management of CLL patients,8-11 and Sanger sequencing is the approach currently recommended by guidelines.11 Due to its limited sensitivity,11 conventional Sanger sequencing misclassifies as wild type ∼5% of newly diagnosed CLL otherwise harboring TP53 mutations of low clonal abundance (0.3% to 11%) and ultimately underestimates the TP53 mutation status in ∼30% of cases harboring TP53 defects. Thanks to its high sensitivity (down to 1% to 0.1%),38,39 ultra-deep-NGS is capable of detecting such minor, but clinically relevant, TP53 mutated subclones. Therefore, ultra-deep-NGS should be considered as a useful tool for a comprehensive assessment of TP53 disruption in CLL.
Though the retrospective design represents a limitation of this analysis, a strong biological rationale supports the clinical relevance of subclonal TP53 mutations in CLL and their more general application as a biomarker in this disease. Subclonal TP53 variants show molecular and functional clues that are highly consistent with those of TP53 mutations with known pathogenicity,29 thus indicating that they have been selected to damage the TP53 protein.28 The pathogenic effect of subclonal TP53 mutations is confirmed by the observation that, in patients, small TP53 mutated subclones are resistant to chemo +/− immunotherapy and are positively selected by treatments to progressively become the dominant leukemic population at the time of CLL relapse. Ultra-deep-NGS may capture newly born and highly fit TP53 mutations at the initial phases of their clonal selection. In this scenario, beside the intrinsic fitness imposed by the TP53 variant, the small TP53 mutant subclone needs further environmental pressures/constraint (ie, microenvironmental interactions, chemotherapy) to overcome and substitute the TP53 wild-type cell population.14-17
Our disease model provides a proof-of-concept that small tumor cell populations of very low clonal abundance (down to 0.3%) can drive the disease course and may represent informative and highly sensitive biomarkers of outcome prediction in cancer patients. These data suggest that limiting the knowledge of tumor genetics to the dominant clone may be uninformative for an accurate prediction of outcome and optimal therapeutic decision. Consequently, the genetic characterization of CLL, and possibly also of other tumors, should be tailored at disclosing in depth the architecture of cancer cell populations, at least for those molecular lesions that are known to harbor prognostic information or to mark chemoresistance.
These pivotal findings may have potential implications for the design of clinical trials and, possibly, for disease management. CLL patients harboring clonal TP53 defects are currently considered at high risk of failing conventional therapies and therefore represent the best candidates for new treatment strategies or stem cell transplant.2,8,10,11 Because patients harboring small TP53 mutated subclones have the same risk of failing and dying as patients harboring clonal TP53 defects, both at diagnosis and at treatment requirement, their identification is advisable in order to manage them as high-risk CLL. Treatment approaches should be selected to target both the major TP53 wild-type clone as well as small TP53 mutated subclones to avoid their subsequent selection and outgrowth that is otherwise destined to occur in all cases exposed to ineffective treatments, as documented by the current study.40 Given their promising activity against CLL cells with TP53 defects,41,42 new targeted drugs (eg, ABT-199 and ibrutinib) may represent a rational treatment to suppress or even eradicate small subclones harboring TP53 lesions.
The online version of this article contains a data supplement.
There is an Inside Blood commentary on this article in this issue.
The publication costs of this article were defrayed in part by page charge payment. Therefore, and solely to indicate this fact, this article is hereby marked “advertisement” in accordance with 18 USC section 1734.
Acknowledgments
This study was supported by Special Program Molecular Clinical Oncology 5 x 1000 no. 10007, My First AIRC grant no. 13470, and Investigator Grant IG-13227, Associazione Italiana per la Ricerca sul Cancro Foundation Milan, Italy, Progetto Giovani Ricercatori 2010, grant no. GR-2010-2317594, Ministero della Salute, Rome, Italy, Compagnia di San Paolo, grant no. PMN_call_2012_0071, Turin, Italy, Fondazione Cariplo, grant no. 2012-0689, Futuro in Ricerca 2012 grant no. RBFR12D1CB, Ministero dell'Istruzione, dell'Università e della Ricerca, Rome, Italy, U54 CA121852-05, 2012 Stewart Trust Cancer Research Fellows, Stewart Foundation. S.M. is being supported by a fellowship from Novara-AIL Onlus Foundation, Novara, Italy. C.D. is being supported by a fellowship from Comitato Gigi Ghirotti, Turin, Italy.
Authorship
Contribution: D.R., H.K., R. Foà, R.R., and G.G. designed the study, interpreted data, and wrote the manuscript; D.R. and H.K. performed statistical analysis; V.S., C.C., A.B., R. Famà, and S.R. performed and interpreted molecular studies; S.M. and C.D. performed and interpreted FISH analysis; L.D.P. collected clinical data; and J.W., V.G., and A.G. contributed to data interpretation.
Conflict-of-interest disclosure: The authors declare no competing financial interests.
Correspondence: Davide Rossi, Division of Hematology, Department of Translational Medicine, Amedeo Avogadro University of Eastern Piedmont, Via Solaroli 17, 28100 Novara, Italy; e-mail: rossidav@med.unipmn.it.
References
Author notes
D.R. and H.K. contributed equally to this study.
R.F., R.R., and G.G. contributed equally to this study.