Abstract
The atypical form of the kidney disease hemolytic uremic syndrome (aHUS) is associated with defective complement regulation. In addition to mutations in complement regulators, factor H (FH)–specific autoantibodies have been reported for aHUS patients. The aim of the present study was to understand the role of these autoantibodies in aHUS. First, the binding sites of FH autoantibodies from 5 unrelated aHUS patients were mapped using recombinant FH fragments and competitor antibodies. For all 5 autoantibodies, the binding site was localized to the FH C-terminus. In a functional assay, isolated patient IgG inhibited FH binding to C3b. In addition, autoantibody-positive patients' plasma caused enhanced hemolysis of sheep erythrocytes, which was reversed by adding FH in excess. These results suggest that aHUS-associated FH autoantibodies mimic the effect of C-terminal FH mutations, as they inhibit the regulatory function of FH at cell surfaces by blocking its C-terminal recognition region.
Introduction
Hemolytic uremic syndrome (HUS) is characterized by hemolytic anemia, thrombocytopenia, and acute renal failure. HUS is most often caused by bacterial infection and is associated with diarrhea (D+ HUS), or arises rarely as atypical HUS (aHUS).1 Mutations identified in complement genes in aHUS patients indicate that complement dysregulation is involved in disease development.2 In addition, factor H (FH) autoantibodies have been reported for 3 aHUS patients.3
FH is a major regulator of the alternative complement pathway. FH is composed of 20 short consensus repeats (SCRs). The 4 N-terminal domains (SCR1-4) mediate cofactor and decay accelerating activity, and the C-terminal domains (SCR19-20) form a recognition region, which contains binding sites for C3b, glycosaminoglycans, and endothelial cells.4-6 SCR19-20 represent a hot spot for aHUS-associated FH mutations,2 several of which have been shown to impair FH binding to C3b and to cellular surfaces.7-9 Thus suggesting that by affecting the C-terminal domains, aHUS-associated mutations reduce FH regulatory activity on cells. Indeed, reduced FH binding leads to enhanced complement activation on host cells and results in cell lysis as shown by analysis of a mutant FH protein lacking most of SCR20,10 by using blocking monoclonal antibodies (mAbs),11 or recombinant SCR19-20 fragment.12
In contrast to the FH mutations, aHUS-associated FH autoantibodies have not yet been analyzed in detail. In the present report, we describe how 5 FH autoantibodies affect FH function.
Patients, materials, and methods
Approval was obtained from the Ethics Committee of the Medical Faculty of Friedrich Schiller University for these studies. Informed consent was obtained in accordance with the Declaration of Helsinki.
Identification and domain mapping of FH autoantibodies
C3b binding assay
IgG was isolated from plasma according to standard protocols. Microtiter plate wells were coated with 5 μg/mL FH (Merck Biosciences, Schwalbach, Germany). After blocking, the wells were preincubated with purified IgG, and then C3b (2 μg/mL) was added and binding was measured using C3-specific antiserum (Merck Biosciences).
Hemolysis assay
Hemolysis assays were performed in 100 μL buffer (20 mM HEPES, 7 mM MgCl2, 10 mM EGTA, 144 mM NaCl, 1% BSA, pH 7.4) containing 5 × 106 sheep erythrocytes (SRBCs; BioTrend Chemikalien, Cologne, Germany) and 10% to 40% plasma. After incubation at 37°C for 30 minutes, optical density of the supernatants was measured at 414 nm.
Results and discussion
FH autoantibodies of aHUS patients bind to the C-terminus of FH
Plasma samples from 60 patients with hemolytic uremic syndrome (51 with aHUS and 9 with D+ HUS) were screened for the presence of FH autoantibodies. Five positive cases, children diagnosed with aHUS at 4 to 12 years of age, were identified using an ELISA assay. This corresponds to approximately 10% of the patients, which is similar to the approximately 6% reported recently.3 FH specificity of the autoantibodies was verified by demonstrating dose-dependent binding to FH and reduced binding after IgG depletion, and by analyzing FH-specific IgG isotypes (Figure S1, available on the Blood website; see the Supplemental Materials link at the top of the online article).
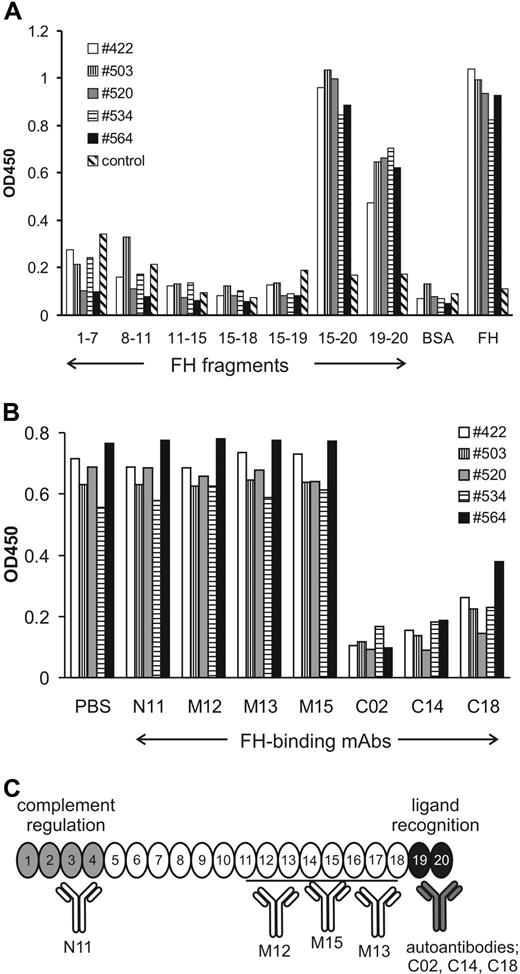
In order to localize the binding domain of the FH autoantibodies, their reactivity with recombinant FH fragments was measured. All 5 autoantibodies bound to FH fragments that include SCR20 (ie, SCR15-20 and SCR19-20; Figure 1A). No specific binding of the autoantibodies to the N-terminal or middle region of FH was observed. A weak binding of plasma no. 503 to SCR8-11 was also detected, which was not further analyzed. To confirm the autoantibody binding site, a competition assay using domain mapped mAbs was performed.6,11 In all 5 cases, binding of the autoantibody to FH was reduced by mAbs that bind to the FH C-terminus, namely mAbs C02 (binding in SCR19), C14, and C18 (both binding within SCR20). By contrast, mAbs that recognize the N-terminus (mAb N11) or the middle region (mAbs M12, M13, M15) of FH did not affect autoantibody binding (Figure 1B). Moreover, binding was competed with FH SCR15-20 fragment (Figure S2).
Autoantibodies bind to the C-terminus of FH. (A) Reactivity of autoantibodies of 5 aHUS patients was tested with recombinant FH fragments, covering all domains of FH. BSA was used as negative control and FH as positive control. Normal human serum was included as additional control. Data are representative of 3 experiments with similar results. (B) Autoantibody binding to FH was blocked with mAbs (25 μg/mL) specific to the C-terminal domains SCR19-20 of FH (ie, C02, C14, and C18), whereas mAbs N11, M12, M13, and M15, which bind in the N-terminal and middle regions of FH, did not inhibit autoantibody binding. Representative data of 3 experiments are shown. (C) Binding domains of the identified FH autoantibodies and the mAbs used in this study. Important functional domains of FH are highlighted.
Autoantibodies bind to the C-terminus of FH. (A) Reactivity of autoantibodies of 5 aHUS patients was tested with recombinant FH fragments, covering all domains of FH. BSA was used as negative control and FH as positive control. Normal human serum was included as additional control. Data are representative of 3 experiments with similar results. (B) Autoantibody binding to FH was blocked with mAbs (25 μg/mL) specific to the C-terminal domains SCR19-20 of FH (ie, C02, C14, and C18), whereas mAbs N11, M12, M13, and M15, which bind in the N-terminal and middle regions of FH, did not inhibit autoantibody binding. Representative data of 3 experiments are shown. (C) Binding domains of the identified FH autoantibodies and the mAbs used in this study. Important functional domains of FH are highlighted.
FH autoantibody inhibits C-terminus–mediated function of FH
Reduced C3b binding of FH and impaired C3b processing on the cell surface, which results in enhanced complement activation and cell damage, are caused by the mAbs C18 and C14,11 which share binding epitopes with the autoantibodies of all 5 analyzed aHUS patients (Figure 1C). Therefore, we measured whether FH autoantibody has the same effect as mAbs C18 and C14.
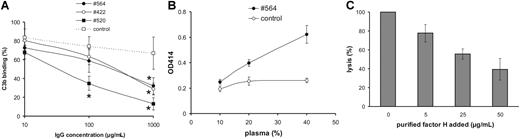
To this end, the IgG fraction was isolated from plasma of 3 patients. Purified patient-derived IgG showed the same reactivity with FH as the whole plasma (Figure S3). C3b binding was strongly reduced when FH was preincubated with patient-derived IgG, which contained FH autoantibodies, whereas control IgG had no effect (Figure 2A). A previous report found no effect of the autoantibody on FH binding to C3b, which is likely due to the different experimental conditions.3
FH autoantibody blocks C-terminal recognition function of FH. (A) Patient-derived IgG, added in the indicated concentrations, reduced binding of human C3b to immobilized FH in an ELISA assay, when compared with control IgG. Data represent mean plus or minus SD from 3 experiments. Difference between samples was analyzed by Student t test. *P < .05. (B) Plasma of patient no. 564 (●) caused dose-dependent lysis of sheep erythrocytes, whereas normal human plasma (○) showed no effect. Hemoglobin release was measured as described in “Patients, materials, and methods.” Mean plus or minus SD of data from 5 measurements is shown. (C) Addition of excess FH rescued sheep erythrocytes from complement-mediated lysis. Cells were incubated in 40% no. 564 plasma without FH added and in the presence of the indicated amounts of purified FH, and hemoglobin release was measured. Erythrocyte lysis in the absence of FH was set to 100%. Mean plus or minus SD of data from 4 independent experiments is shown.
FH autoantibody blocks C-terminal recognition function of FH. (A) Patient-derived IgG, added in the indicated concentrations, reduced binding of human C3b to immobilized FH in an ELISA assay, when compared with control IgG. Data represent mean plus or minus SD from 3 experiments. Difference between samples was analyzed by Student t test. *P < .05. (B) Plasma of patient no. 564 (●) caused dose-dependent lysis of sheep erythrocytes, whereas normal human plasma (○) showed no effect. Hemoglobin release was measured as described in “Patients, materials, and methods.” Mean plus or minus SD of data from 5 measurements is shown. (C) Addition of excess FH rescued sheep erythrocytes from complement-mediated lysis. Cells were incubated in 40% no. 564 plasma without FH added and in the presence of the indicated amounts of purified FH, and hemoglobin release was measured. Erythrocyte lysis in the absence of FH was set to 100%. Mean plus or minus SD of data from 4 independent experiments is shown.
Sera derived from aHUS patients with heterozygous C-terminal FH mutations cause SRBC lysis.13 When performing a similar assay, incubation with the autoantibody-positive plasma of patient no. 564 resulted in enhanced hemolysis of SRBCs (Figure 2B). Furthermore, the hemolytic activity was reversed in a dose-dependent manner by addition of excess FH to the patient's plasma, and thus increasing the concentration of autoantibody-free FH (Figure 2C). This effect of the autoantibody is in line with the observation that the C-terminally binding mAbs C18 and C14 cause enhanced SRBC lysis when added to normal human plasma (data not shown).
That the autoantibodies of all 5 patients do not bind to the N-terminus of FH, where the complement regulatory domains are localized, is in agreement with a previous report, and explains the normal FH activity in fluid phase in the presence of autoantibody (data not shown).3
The presence of C-terminally binding FH autoantibodies, which influence FH activity, has relevance for diagnosis and treatment of aHUS patients. FH autoantibody titer can be decreased by plasma exchanges,3 which in the case of patient no. 564 were accompanied with improvement of clinical parameters (data not shown). However, for the autoantibody-positive patients, kidney transplantation is likely at high risk, as the autoreactive antibodies will remain in plasma.
Domain mapping and functional analysis of additional aHUS-associated FH autoantibodies are required to assess whether the mechanism suggested here applies in general. Other autoantibodies may have a different binding site and affect, for example, FH stability or conformation. However, it is striking that all 5 FH autoantibodies identified in the present study bind predominantly to the FH C-terminus. Thus, in aHUS, FH dysfunction of autoimmune origin (ie, caused by autoantibodies) seems analogous to the C-terminal mutations, and both scenarios result in an impaired recognition of host cells by FH during complement attack.
The online version of this article contains a data supplement.
The publication costs of this article were defrayed in part by page charge payment. Therefore, and solely to indicate this fact, this article is hereby marked “advertisement” in accordance with 18 USC section 1734.
Acknowledgments
This work was supported by grants from the Deutsche Forschungsgemeinschaft and the Kidneeds Foundation (Cedar Rapids, IA).
We thank Gerlinde Heckrodt, Ina Löschmann, and Eva-Maria Neumann for technical assistance.
Authorship
Contribution: M.J. designed and performed research, interpreted data, and wrote the paper; S.S. and H.-M.D. performed research; P.F.H. and W.L. collected biologic samples and developed the clinical concept; M.O. contributed vital reagents; C.S. interpreted data; and P.F.Z. designed research and wrote the paper.
Conflict-of-interest disclosure: The authors declare no competing financial interests.
Correspondence: Mihály Józsi, Junior Research Group Cellular Immunobiology, Leibniz Institute for Natural Product Research and Infection Biology-Hans Knöll Institute, Beutenbergstr 11a, D-07745 Jena, Germany; e-mail: mihaly.jozsi@hki-jena.de.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal