Abstract
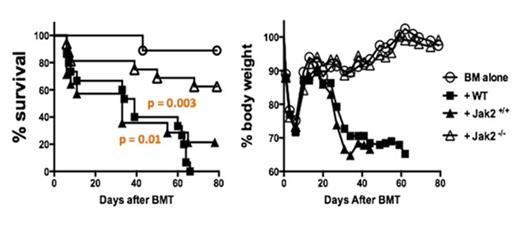
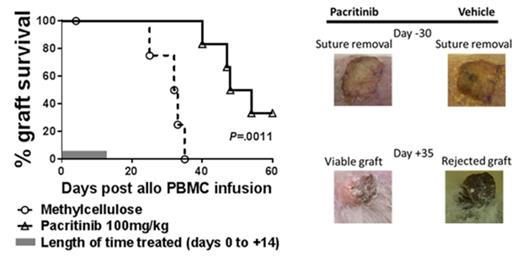
Janus kinase 2 (JAK2) signal transduction is a critical mediator of immune response. JAK2 activation promotes T-cell allosensitization, as well as Th1 and Th17 differentiation. JAK2-mediated STAT3 phosphorylation limits the generation of induced regulatory T cells (iTregs) by disrupting interactions between STAT5 and Foxp3. JAK2 is implicated in the onset of graft-versus-host disease (GVHD), which is a significant cause of transplant-related mortality after allogeneic hematopoietic cell transplantation (allo-HCT). Using murine models of allo-HCT we show here that transfer of donor JAK2-/- T cells is associated with significantly less GVHD, compared with wild-type or JAK2 replete donors (Figure 1, P =.003 and 0.01, respectively). Th1 differentiation among JAK2-/- T-cells is dramatically decreased, compared with controls. Conversely, iTreg polarization and stability are significantly increased among the JAK2 deficient T cells. To investigate the effect of pharmacologic JAK2 inhibition on T-cell alloresponses, pacritinib (supplied by CTI BioPharma), was chosen as it does not induce myelosuppression or increase risk for opportunistic infections in myelofibrosis patients - unlike JAK1/JAK2 inhibitors. Pacritinib potently inhibits JAK2, but also has suppressive activity toward JAK3, CSF1R, and IRAK1. Pacritinib was administered at 100mg/kg twice a day by oral gavage for 4 weeks beginning on the day of MHC-disparate allo-HCT, significantly reducing GVHD in recipient mice compared with methylcellulose vehicle control. In allogeneic mixed leukocyte reactions using human cells, pacritinib (2.5μM) significantly reduces T-cell proliferation after 5 days of culture (P <.0001). In vitro studies verified pacritinib eliminates STAT3 activity by IL-6 in human CD4+ T-cells, while permitting IL-2 induced STAT5 phosphorylation despite its effects on JAK3. This offers a platform to reduce Th17 development, while promoting iTreg populations. As such, pacritinib dramatically suppresses Th17 differentiation reflected by RORgammaT expression among naïve CD4+ T cells stimulated by allogeneic dendritic cells (DC), compared with DMSO (P <.0001). iTregs were generated with allogeneic DCs in the presence of pacritinib or DMSO for 5 days, and then cultured with self T-cell responders and fresh DCs without additional drug exposure. The suppressive potency of either pacritinib- or DMSO-treated iTregs was similar, suggesting JAK2 is not required for iTreg function. We then evaluated whether JAK2 inhibition could prevent human skin graft rejection in an NSG mouse xenograft model. A 1x1 cm split-thickness human skin graft was transplanted onto the animal dorsally. The mice rested for 30 days after surgery to permit engraftment, then received 5x106 allogeneic peripheral blood mononuclear cells (PBMC) by intraperitoneal injection. Pacritinib was administered at the same dose and schedule for 2 weeks beginning at time of PBMC injection as tolerated by the NSG mice. The treatment significantly delayed allograft rejection by the human donor PBMCs, compared with vehicle control (Figure 2: Median graft survival 32.5 v 51 days, Day +60 survival 0% v 33.3%, pooled data from 2 experiments, n=5-6 mice per arm, P =.0011). Collectively, these data clearly identify JAK2 as a therapeutic target to control donor alloreactivity and promote iTreg responses after HCT or solid organ transplantation.
*BCB and DB contributed equally to this work.
Decreased human skin graft rejection with JAK2 inhibitor, pacritinib
Singer:CTI BioPharma, Corp: Employment, Equity Ownership.
Author notes
Asterisk with author names denotes non-ASH members.