Abstract
Introduction
Venous thromboembolism (VTE) is a common complication of both solid and hematologic malignancies. Risk factors for VTE and standard recommendations for prevention and treatment primarily pertain to solid tumor patients. There are fewer data in patients who have undergone allogeneic hematopoietic cell transplant (HCT). Therefore, we studied the incidence, risk factors, and impact of VTE on post-HCT outcomes.
Methods
We retrospectively reviewed 431 patients who underwent allogeneic HCT between 1/2014 and 8/2019 to identify patients with VTE. VTE was estimated with cumulative incidence methods. Risk factors for VTE were identified with Fine and Gray regression and results are reported as hazard ratio (HR) with a 95% confidence interval (CI). An apriori list of potential risk factors for VTE included age, gender, race, performance status, co-morbidity index, number of prior chemotherapy regimens, history of VTE, disease risk, donor/graft source, transplant conditioning regimen, and acute or chronic graft vs. host disease (GVHD). VTE was analyzed as a time-dependent covariate relative to other post-HCT outcomes.
Results
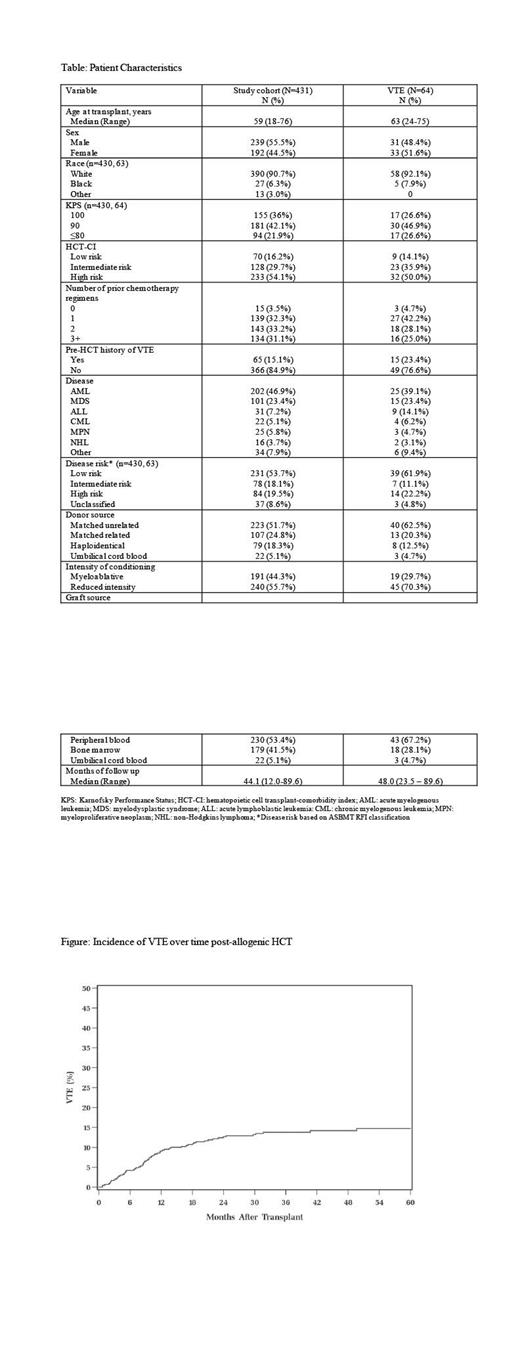
Patient characteristics are shown in the Table. The median age at time of transplant was 59 years, (range 18-76); 55.5% were male, the majority (90.7%) were White. The most common indication for transplant was acute myelogenous leukemia and myelodysplastic syndrome (70.3%). Within our cohort, 64 patients (14.8%) developed VTE after allogeneic HCT. The cumulative incidence of VTE at 1 year was 9% (CI 7-12%). Median time to VTE was 9.8 months (range 0.7-74.0) (Figure). Thrombosis site breakdown included the following: lower deep vein thrombosis (DVT) n=47 (74%), catheter related DVT n=12 (19%), DVT and pulmonary embolism (PE) n=12 (19%), PE alone n=4 (6%). Patients were most commonly treated with a direct oral anticoagulant (n=27, 42%), followed by enoxaparin (n=15, 23.4%). The majority of patients (n=38, 58%) were treated with anticoagulation for more than 6 months. Six (9.4%) patients had recurrent thrombosis after completion of anticoagulation therapy from the time of transplant until last known follow-up. Only 9 (14%) had an inferior vena cava filter placed due to contraindications for anticoagulation. In patients treated with anticoagulation, there was a low overall incidence of clinically significant bleeding (n=3, 5%). In multivariable analysis, age (HR 1.36 per 10-year increase, CI 1.09-1.70, P=0.006), history of VTE (HR 1.95, CI 1.09-3.48, P=0.024), and grade 2-4 acute GVHD (HR 1.75, CI 1.05-2.94, P=0.033) were significantly associated with VTE. VTE was not associated with relapse mortality (HR 0.95, CI 0.44-2.04, P=0.89), however VTE was significantly associated with an increased risk of non VTE-associated non-relapse mortality (NRM) (HR 4.09, CI 2.47-6.74, P<0.001) and decreased overall survival (OS) (HR 2.19, CI 1.48-3.24, P<0.001).
Discussion
VTE is an important complication after allogeneic HCT and is associated with significantly increased NRM and inferior OS. Older patients, those with a prior history of VTE, and patients with acute GVHD are at increased risk for development of VTE after HCT. We found an overall low risk of bleeding with anticoagulation and further study to investigate the role of prophylaxis in this high-risk cohort is needed.
Sobecks: CareDX: Membership on an entity's Board of Directors or advisory committees. Majhail: Incyte Corporation: Consultancy; Anthem, Inc: Consultancy. Angelini: Sanofi: Membership on an entity's Board of Directors or advisory committees. Hamilton: Syndax: Membership on an entity's Board of Directors or advisory committees; Equilium: Membership on an entity's Board of Directors or advisory committees.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal