Introduction: Hemophagocytic lymphohistiocytosis (HLH) is a life-threatening hyper-inflammatory syndrome which may occur in adults with hematologic malignancies (HM). The diagnosis of HLH in this context (HM-HLH) is hindered by a number of factors. First, the currently used HLH 2004 diagnostic criteria are derived from pediatric patients commonly with HLH-associated genetic lesions, a very different population than adults with cancer. Second, most parameters used for diagnosis of HLH are directly impacted by the underlying HM and may reflect the presence of the malignant clone itself rather than an inflammatory process. Finally, appropriate diagnostic cutoff values for laboratory abnormalities in HM-HLH have not been defined. In this study we determine the diagnostic value of the laboratory components of the HLH 2004 diagnostic criteria and establish optimal cutoffs for the diagnosis of HM-HLH in HM patients.
Methods: This is a multicenter, retrospective study of adult patients with a hematologic malignancy in whom sCD25 was measured because of clinically suspected HM-HLH or as part of routine screening of patients with a newly diagnosed hematologic malignancy, between January 2012 and March 2020. We considered patients fulfilling the five of eight of the HLH 2004 diagnostic criteria to have HM-HLH. Patients fulfilling fewer than five criteria were assigned to the HM group. These cohorts were well balanced in terms of disease distribution. We established the optimal cutoffs for laboratory parameters used for the diagnosis of HM-HLH using receiver operating curves (ROC) in a discovery cohort and tested their performance in a validation cohort. In order to improve the results obtained using the individual ROC, we then created a combined ROC using parameters demonstrating the highest individual performance (highest area under the curve (AUC)), in order to develop a diagnostic index. Finally, we examined the performance of each parameter in each cohort by using a contingency table and Chi-square and Fisher's exact test to determine the positive predictive value (PPV), negative predictive value (NPV), sensitivity, specificity and likelihood ratio (LR) of disease for each parameter.
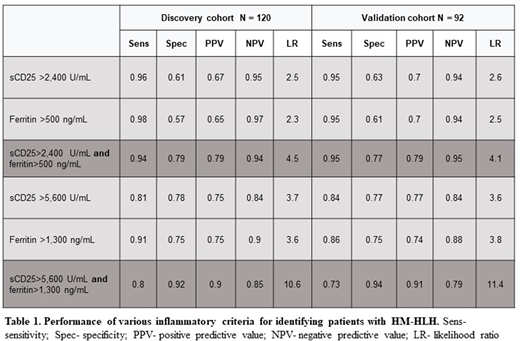
Results: 212 adults with HM with or without HLH in whom testing for HLH was performed were included in the study. HMs were: B cell lymphoma (41%), T cell lymphoma (26%), Hodgkin lymphoma (9%), acute myeloid leukemia (8%), myelodysplastic syndrome (8%), myeloproliferative neoplasms (5%) and chronic lymphocytic leukemia (4%). 99 (47%) patients had HM-HLH. Despite considerable overlap in laboratory values between the patient groups, all parameters apart from fibrinogen were able to distinguish HM-HLH from HM alone, with ferritin and sCD25 having the greatest discriminatory power. ROC analysis revealed an optimal cutoff value of >5,600 U/mL for sCD25 (sensitivity/specificity 76%/78%, AUC=0.83) and >1,300 ng/ml for ferritin (sensitivity/specificity 76%/76%, AUC=0.83). Combining the two markers to create a novel inflammatory index (HM-INFL) yielded superior diagnostic ability (AUC =0.86). Using HLH 2004 cutoff levels the HM-INFL index had a sensitivity of 94% and NPV of 94% and when using the optimal cutoff levels, it had a specificity of 92% and PPV of 90% (Table 1).
Conclusions: HM-INFL is an index comprising only ferritin and sCD25. Using the original HLH 2004 cutoffs the index is an effective screening tool. Using our newly defined cutoff levels obtained by ROC analysis it is highly specific and can be used as a confirmatory test for the diagnosis of HLH in HM patients. These findings also support the hypothesis that HLH in the context of HM is an inflammatory condition associated with immune dysregulation.
Miller:Foundation Medicines, Inc.: Consultancy. Daver:Daiichi Sankyo: Consultancy, Membership on an entity's Board of Directors or advisory committees, Research Funding; Bristol-Myers Squibb: Consultancy, Membership on an entity's Board of Directors or advisory committees, Research Funding; Pfizer: Consultancy, Membership on an entity's Board of Directors or advisory committees, Research Funding; Karyopharm: Research Funding; Servier: Research Funding; Genentech: Research Funding; AbbVie: Consultancy, Membership on an entity's Board of Directors or advisory committees, Research Funding; Astellas: Consultancy, Membership on an entity's Board of Directors or advisory committees, Research Funding; Novimmune: Research Funding; Gilead: Consultancy, Membership on an entity's Board of Directors or advisory committees, Research Funding; Amgen: Consultancy, Membership on an entity's Board of Directors or advisory committees, Research Funding; Trovagene: Research Funding; Fate Therapeutics: Research Funding; ImmunoGen: Research Funding; Novartis: Consultancy, Membership on an entity's Board of Directors or advisory committees; Celgene: Consultancy, Membership on an entity's Board of Directors or advisory committees; Jazz: Consultancy, Membership on an entity's Board of Directors or advisory committees; Trillium: Consultancy, Membership on an entity's Board of Directors or advisory committees; Syndax: Consultancy, Membership on an entity's Board of Directors or advisory committees; Amgen: Consultancy, Membership on an entity's Board of Directors or advisory committees; KITE: Consultancy, Membership on an entity's Board of Directors or advisory committees; Agios: Consultancy, Membership on an entity's Board of Directors or advisory committees. Jordan:Sobi: Consultancy.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal