Background:
Sickle Cell Disease (SCD) predominantly affects people of African ancestry, causing significant morbidity and mortality. In high-income countries children, who are more likely to receive comprehensive care than adults, have better health care outcomes. Young adults (YA) are in a period of transition from pediatric to adult models of care and the effect of receiving care at multiple medical facilities (fragmentation) during this time on outcomes has not been well-described. In this study we sought to examine fragmentation of care for YA SCD patients and the association of fragmentation on mortality.
Methods:
Using a previously published definition, longitudinal records from the California Patient Discharge, Emergency Department, and Ambulatory Surgery datasets were used to identify SCD patients from 1991-2016.
SCD patients were placed into three different age cohorts: children (10-17), YA (18-25) and adults (26-33). Each patient required the full 7 year follow up time in each age category; patients could be in multiple age cohorts. Patients with no inpatient admissions were excluded. The number of inpatient admissions during each age group period was used as a measure of disease severity (<10, 10-19, 20-29, ≥30). SCD specialty care centers (SCD SC) were determined using all SCD inpatient admissions; facilities in the top 5% based on number of unique SCD patients seen were considered SCD SC. Patients were classified as always, sometimes and never seen at SCD SC facilities in each age group.
We classified care fragmentation by the number of facilities an individual received inpatient care (1, 2, 3-4 or ≥5 unique facilities) during their time in each age group. Descriptive statistics were used to describe patients' characteristics by age group. Multivariable Poisson regression was used to identify risk factors associated with fragmented care. Multivariable Cox regression was used to determine the impact of fragmented care, disease severity and care at SCD SC on all-cause mortality, conditional on surviving to 26 years of age for the YA group.
Results
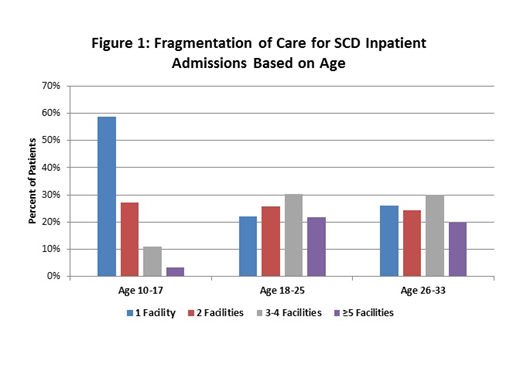
We identified a cohort of 6,977 unique SCD patients: 1,019 children, 1,122 YAs and 1,015 adults. The YA cohort consisted of predominately African Americans (91.3%) with 43.9% male and 56.1% female. Forty-two % YAs had Medi-Cal followed by 26.7% with private insurance as first reported health insurance. Forty-four % (494) had <10, 20.1% (226) had 10-19, 11.1% (125) had 20-29 and 24.7% (277) had ≥30 inpatient admissions while in the YA age period. Twenty-two % (248) YAs were seen at 1, 25.8% (290) were seen at 2, 30.2% (339) were seen at 3-4, and 21.8% (245) were seen at > 5 inpatient facilities. YAs and older adults were seen at a similar number of facilities while children were seen at less (Figure 1).
In multivariable regression models among YAs, those with private insurance (vs. Medi-Cal) were at lower risk of fragmentation (Incident Rate Ratio (IRR)=0.85, CI 0.78-0.93, p=0.0002), while those without insurance were at a higher risk (IRR 1.45, CI 1.22-1.72, p<0.0001). Patients with more admissions (vs. <10) were at higher risk of fragmentation (IRR for 10-19 =1.42, CI 1.29-1.57; IRR for 20-29 1.49, CI 1.33-1.67, IRR for >30 admissions 2.13, CI 1.98-2.43 p<0.0001). Patients who were sometimes admitted to an SCD SC (IRR=2.19, CI 1.98-2.43, p<0.0001) or never (IRR=1.15, CI 1.15-1.46, p<0.0001) were at increased risk of fragmented care compared to those who were always admitted to an SCD SC.
In the multivariable mortality model, YAs with increasing number of admissions, regardless of location, were at increased risk of death (10-19 HR 2.36, CI 1.13-4.91 p=0.022; 20-29 HR 4.25, CI 2.03-8.92, p=0.0001; > 30 admissions HR 7.79, CI 4.09-14.83, p<0.0001). Fragmentation of care and always or sometimes being admitted to an SCD SC were not associated with mortality.
Conclusion
Most young adult SCD patients (78%) received inpatient care at >1 facility. Of all age groups, children were most likely to be seen at only 1 facility, suggesting that fragmentation of care begins in early adulthood. Young adults without insurance, patients with more frequent admissions and those who did not always receive care at an SCD SC were at higher risk for fragmented care. Young adults with more frequent admissions were also at an increased risk of mortality. The effect of specialty centers and more consistent location of care on health-related outcomes for patients with SCD requires further study.
Wun:Janssen: Other: Steering committee; Pfizer: Other: Steering committee.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal