Abstract
INTRODUCTION: Relapse after allogeneic hematopoietic stem cell transplantation (alloHSCT) remains a major therapeutic challenge: outcome is very poor, without curative option in most cases. Second alloHSCT may be considered in few selected patients because of anticipated limitations: 1) donor availability; 2) high toxicity due to previous treatments; 3) low efficacy considering the very advanced disease situation. We hypothesized that the use of post transplantation Cyclophosphamide (pCY) haplo-SCT may be an interesting alternative to overcome these limitations. In particular, the presence of full haplotype HLA mismatch could provide a decisive antileukemic effect relative to alloreactivity. In absence of large series in this setting, we report here the outcome after HaploSCT for patients who relapse after a first alloHSCT.
METHODS: We retrospectively studied adult patients, who received a second pCy Haplo-SCT for hematological malignancies. Patients were treated between 2009 and 2016. The objective was to assess both the feasibility and the efficacy of HaploSCT in this setting.
RESULTS: Twenty seven patients were included: median time between first alloHSCT and relapse was 11 months (range: 1-82). Median age at second transplantation was 49 years old (range: 21-61).
Most of patients had acute myeloid leukemia (n=12, 44%) or Hodgkin lymphoma (n=6 patients, 22%). Fifteen patients (55%) were in complete remission at the time of pCY Haplo-SCT.
Hematopoietic cell transplantation-comorbidity index was ≥ 3 in 20 patients (74%). Thirteen patients (48 %) received non-myeloablative conditioning regimen (as Baltimore schema, Luznik et al. BBMT 2008) prior to HaploSCT while remaining patients received busulfan-based regimen.
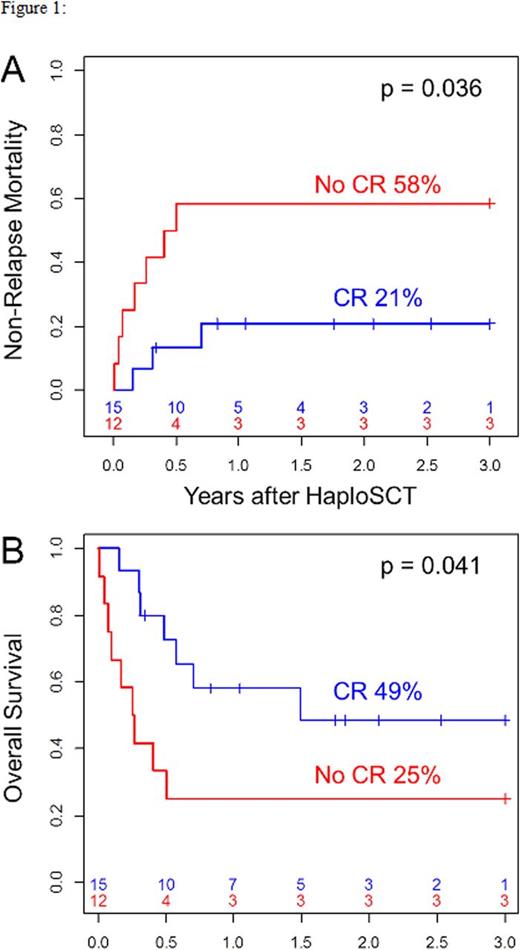
Day+100 cumulative incidence of grade 2 to 4 and 3 to 4 acute GVHD was 15% and 7%. 2-year cumulative incidence of chronic GVHD was 12%. The cumulative incidence of non-relapse mortality and relapse at 2 years were 38% and 27%, respectively. With a median follow up of 25 months (range: 4-63), 2-year progression-free and overall survivals were 36% and 39%, respectively. Disease status at the time of HaploSCT was a major determinant for outcome. Indeed, 2-year NRM and OS were 58% and 25% in patients transplanted with active disease, respectively, while corresponding values in patients transplanted in CR were 21% (p=0.036) and 49% (p=0.041), respectively (Figure 1A and 1B).
CONCLUSION: We can conclude that in selected patients who could be candidate for second transplantation, HaploSCT is feasible and may represent a curative option.
The overall incidence of relapse of 27% is promising in this situation for which no alternative for cure is available, with relatively good survival in patients transplanted in CR. However, the very high NRM (58%) in refractory patients should make us consider second transplant with caution in this setting. For these patients, specific developments are needed to avoid procedure-related toxicity.
No relevant conflicts of interest to declare.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal