Abstract
Introduction
Atrial fibrillation (AF) occurs in 5-9% of patients treated with ibrutinib for CLL. We previously reported on the clinical characteristics and management outcomes of 56 patients with ibrutinib-associated AF (n=52) or atrial flutter (n=4) retrospectively identified from centers of the FILO group (French Innovative Leukemia Organization, France/Belgium, n=29), MD Anderson Cancer Center (USA, n=21), and Peter MacCallum Cancer Centre (Australia, n=6) (Thompson et al BJH 2016). We found that (1) the median time from the initiation of ibrutinib to AF was 3.8 months (range: 6 - 1410 days); (2) AF recurred or became persistent in 63% despite medical management; (3) AF and its management was associated with serious sequelae including severe cardiac failure (n=3, 1 fatal), ischemic stroke (n=3) and severe bleeding events (n=8); (4) immediate cessation of ibrutinib therapy was required in 22/56 (39%). Given the reported poor outcomes for patients who discontinue ibrutinib for toxicity, we update the results of this cohort with respect to CLL outcomes and survival.
Aim
To describe long term overall and disease-specific outcomes in patients who develop ibrutinib-associated AF.
Methods
This is an update of an international, retrospective cohort of patients who developed ibrutinib-associated AF. Patients are managed according to local best standard practice. The median follow-up from onset of AF is 21 months.
Results
The median overall survival after development of AF is 43 months. Twenty-two (39%) patients stopped ibrutinib at the time of AF. Among these patients, 7 (32%) eventually died from CLL progression (n=3), infection (1), cardiac failure (1), pulmonary hemorrhage (1) and colon cancer (1). Of the 34 patients who initially continued ibrutinib, 5 (15%) died; causes of death were: Richter transformation (RT) (n=2), septic shock (1), CLL progression (1), and stroke in the context of AF (1).
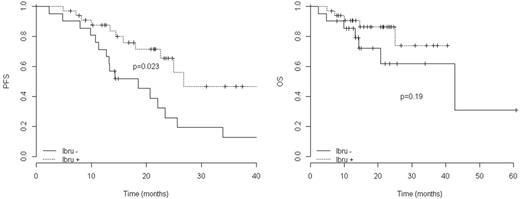
In order to gain insight into disease control in relationship to AF and its management, we examined PFS from the time of AF onset. The following features had no impact on PFS: single AF episode vs paroxysmal/permanent AF or time from ibrutinib initiation to onset of AF. However, patients who had ibrutinib interrupted at the time of AF onset (n=22) had a significantly inferior PFS (median 19 months) compared with those who had dose reduction without interruption (n=13) or those who continued full dose ibrutinib (n=21, median 27 months, p=0.023, Figure 1). There was a trend toward inferior overall survival in those who interrupted ibrutinib (62% at 3 years) compared with those who continued without interruption (74% at 3 years, p=0.10), but this did not reach statistical significance at the time of analysis.
Only 3 of 22 (14%) patients who had initial interruption of ibrutinib successfully restarted ibrutinib following control of AF; all 3 remain in continuous partial remission. Four other patients restarted ibrutinib, but subsequently discontinued due to pulmonary hemorrhage (n=1), stroke (1), CLL progression (1) and RT (1).
Among patients who discontinued Ibrutinib permanently, only 9 did so solely because of uncomplicated AF. The others discontinued because of: (a) complications of AF or its management such as cardiac failure (n=1), recurrent AF (n=5) and bleeding events (n=4; one each of hemopericardium, pulmonary hemorrhage, subdural hematoma and gastrointestinal hemorrhage); (b) complications related to CLL such as CLL progression (n=1) and RT (n=2); or (c) other causes such as lung cancer (n=1) or unknown reasons (n=2). Altogether, 21 patients were still on Ibrutinib among 44 patients alive at last follow-up.
Conclusion
Occurrence of AF at any time during ibrutinib treatment was associated with an initial discontinuation rate of 39%, and only 37.5% of patients remain alive and on drug after a median of 21 months follow-up. Patients who interrupted ibrutinib at the time of AF onset have an inferior PFS compared to those who continued ibrutinib or were managed with dose reductions. This inferior outcome in CLL control is likely related to the low rate of patients (14%) who subsequently successfully restarted ibrutinib. Development of AF was associated with serious complications, including hemorrhage, ischemic stroke and cardiac failure. Management of ibrutinib-associated AF is complex and requires international consensus guidelines and a multidisciplinary approach.
Thompson:Pharmacyclics: Consultancy, Honoraria. Levy:Abbive: Honoraria; Roche: Honoraria; Janssen: Honoraria; Gilead: Honoraria. Tam:janssen: Honoraria, Research Funding; AbbVie: Honoraria, Membership on an entity's Board of Directors or advisory committees; Roche: Honoraria, Membership on an entity's Board of Directors or advisory committees. Quinquenel:janssen: Honoraria, Research Funding. Dupuis:ABBVIE: Membership on an entity's Board of Directors or advisory committees; janssen: Honoraria. Cymbalista:Roche: Honoraria; Abbvie: Honoraria; Gilead: Consultancy, Honoraria; Janssen: Consultancy, Research Funding.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal