Abstract

Introduction: Therapeutic options for the management of venous thromboembolism (VTE) in patients with cancer remain limited. Guidelines recommend anticoagulation with low molecular weight heparin (LMWH) monotherapy for ≥3-6 months, and possibly indefinitely, for patients with active cancer. However, drug cost and patient preference issues may lead to non-compliance with these recommendations. The objective of this study is to describe current treatment patterns and to evaluate patient persistence on various anticoagulants.
Methods: Medical and pharmacy claims from the Humana Database were analyzed. To reflect recent treatment patterns, the study population was restricted to patients who had their first VTE between 1/1/2013 and 12/31/2014. Newly diagnosed cancer patients with a first VTE diagnosis (deep vein thrombosis [DVT] or pulmonary embolism [PE]) occurring after their first cancer diagnosis (a 30-day window before the cancer diagnosis was allowed), and with ≥1 dispensing of an anticoagulant agent within 30 days after their VTE diagnosis, were selected. Based on the first anticoagulant agent received, patients were classified into one of the following cohorts: LMWH, LMWH/warfarin, warfarin and rivaroxaban. Use of other anticoagulants including fondaparinux, heparin, apixaban, or dabigatran was low and could not be analyzed due to small sample size. The observation period spanned from the date of the first anticoagulant dispensing to the end of insurance eligibility or the end of data availability, whichever occurred earlier. Discontinuation of the index therapy was defined by a time gap without refill of the index anticoagulant for more than 60 days after the presumed exhaustion of the last known dispensing. For patients in the LMWH/warfarin group, the 2 medications were filled simultaneously as an index therapy, with the expectation that the patients were bridged to warfarin; therefore, their persistence was evaluated based on warfarin therapy. Persistence on therapy was assessed for 12 months using Kaplan-Meier rates, and unadjusted Cox proportional hazards models were used to compare the time to discontinuation between cohorts.
Results: A total of 2,941 newly diagnosed patients with cancer who developed VTE and received anticoagulation in outpatient settings were identified. Of these, 97% received anticoagulation with either LMWH (n=735; 25%), LMWH/warfarin (n=550; 18.7%), warfarin (n=853; 29%), rivaroxaban (n=709; 24.1%). Mean age and gender were similar across treatment cohorts. Approximately 90% of the patients had diagnoses of solid tumors. Diagnoses for DVT, PE, and DVT/PE were 55%, 27%, and 18%, respectively, and were similar across cohorts. Treatments for cancers associated with very high VTE risk (stomach, pancreas, and brain) ranged from 15% in LMWH to 6% in rivaroxaban cohorts, while high VTE risk (lung, lymphoma, gynecologic, bladder, testicular, and renal) ranged from 39% in LMWH to 30% in warfarin and LMWH/warfarin cohorts. Around 75% (warfarin) to 58% (rivaroxaban) of the VTE cases were diagnosed in inpatient settings.
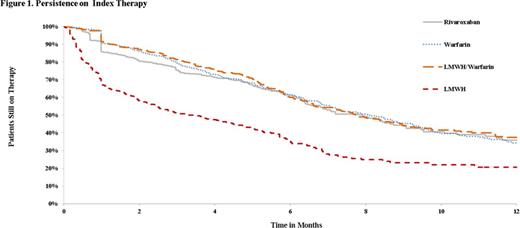
The median treatment durations for LMWH, LMWH/warfarin, warfarin, and rivaroxaban users were 3.29, 7.76, 8.12, and 7.92 months, respectively. Kaplan-Meier rates of persistence to the initial therapy were 37%, 60%, 62%, and 61% at 6 months, and 21%, 37%, 34%, and 36% and at 12 months for the LMWH, LMWH/warfarin, warfarin and rivaroxaban cohorts, respectively (Figure 1). LMWH/warfarin, warfarin, and rivaroxaban users were significantly more likely to remain on their initial therapy compared to LMWH, with hazard ratios (HRs; 95% CI) of 0.38 (0.32-0.45), 0.40 (0.34-0.46), and 0.42 (0.36-0.50), respectively (all p-values <0.0001). The proportion of patients that switched from their initial treatment to another anticoagulation treatment was 22.9%, 8.9%, 7.3% and 4.7% in the LMWH, LMWH/warfarin, warfarin, and rivaroxaban cohorts, respectively.
Conclusion: This real-world analysis showed that despite guidelines recommendations, warfarin and rivaroxaban are nearly equally utilized as LMWH for the treatment of cancer-associated thrombosis. LMWH was associated with significantly lower persistence and shorter duration of treatment than warfarin and rivaroxaban. More patients switched from LMWH to other anticoagulants compared to patients starting on warfarin or rivaroxaban treatments.
Khorana:sanofi: Consultancy, Honoraria; Leo Pharma: Consultancy, Honoraria, Membership on an entity's Board of Directors or advisory committees; Pfizer: Consultancy, Honoraria; Boehringer-Ingelheim: Consultancy, Honoraria; Janssen: Consultancy, Honoraria, Membership on an entity's Board of Directors or advisory committees; Daiichi Sankyo: Consultancy, Honoraria. McCrae:Janssen Scientific Affairs: Membership on an entity's Board of Directors or advisory committees. Milentijevic:Janssen Scientific Affairs: Employment, Equity Ownership. Fortier:Janssen Scientific Affairs: Research Funding. Nelson:Johnson & Johnson: Equity Ownership; Janssen Scientific Affairs: Employment. Laliberté:Janssen Scientific Affairs: Research Funding. Crivera:Janssen Scientific Affairs, LLC: Employment, Equity Ownership. Lefebvre:Janssen Scientific Affairs: Research Funding. Yannicelli:Janssen Scientific Affairs: Employment, Equity Ownership. Schein:Janssen Scientific Affairs, LLC: Employment.
Author notes
Asterisk with author names denotes non-ASH members.

This icon denotes a clinically relevant abstract

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal