Abstract
Introduction
Population level data about the survival outcomes of patients with hematologic malignancies occurring as second cancers is limited. We undertook one of the largest analyses of second hematologic malignancies (SHM) using the Surveillance, Epidemiology & End Results (SEER) registry to identify factors associated with survival.
Methods
SEER 9 &13 registries were queried to identify adult patients (pts>18 years) diagnosed with SHM that comprised of Acute Myeloid Leukemia (AML), Acute Lymphoid Leukemia (ALL), Myelodysplastic Syndromes (MDS), Chronic Myeloid Leukemia (CML) & Other Acute Leukemias (OAL, biphenotypic leukemias, myeloid sarcomas & leukemias NOS) > 1 year (yr) after diagnosis of a primary unrelated cancer, using ICD-O-3 codes over a 40 yr period (1973-2012). Data on demographics, follow up, primary tumor & survival were abstracted. Univariate & multivariate analyses were performed to identify factors influencing survival of SHM & compared with hematologic malignancies occurring as first cancers. Hazard ratios (HR) with 95% confidence intervals (CIs) are reported & significance was set at p< 0.01.
Results
SHM cases included 4665 AML, 3569 MDS, 1140 OAL, 1076 CML & 536 ALL pts. Median age at diagnosis of SHM was 73 yrs (range, 18-100) for AML, 79 yrs (18-100) for MDS, 74 yrs(20-99) for OAL, 74 yrs(18-98) for CML & 70 yrs(19-97) for ALL. Pts>60 yrs comprised 79.2% of AML, 92% of MDS, 88.7% of OAL, 82.9% of CML & 75.2% of ALL cases. Gender distribution was similar across all categories, with females comprising 48.5% of AML, 42.2% of MDS, 45.3% of OAL, 42.8% of CML & 50.2% of ALL cases. More than 85% of pts in each group were Caucasians. While the majority of pts had one primary unrelated cancer (82-89%), 14% of AML pts, 17.8% of MDS pts, 13.8% of OAL, 15.3% of CML pts& 10.6% of ALL pts had >1 primary unrelated cancer. Most common primary sites were prostate (19.1-29.6%), breast (16.1-21.9%) & colorectal (9.3-14.5%). Median survival (range) was as follows: AML 0.2 yrs (0-28.2); MDS 1.5 yrs (0-14); OAL 0.2 yrs (0-29.1); CML 2.5 yrs (0-27.1); & ALL 0.7 yrs (0-28.8). Median latency periods (range) for secondary cancers were as follows: AML 5.2 yrs (1.0-24.2); MDS 7.6 yrs (1.0-35.5); OAL 5.7 yrs (1.0-=34.3); CML 5.2 yrs (1.0-31.6); & ALL 6.2 yrs (1.0-35.5).
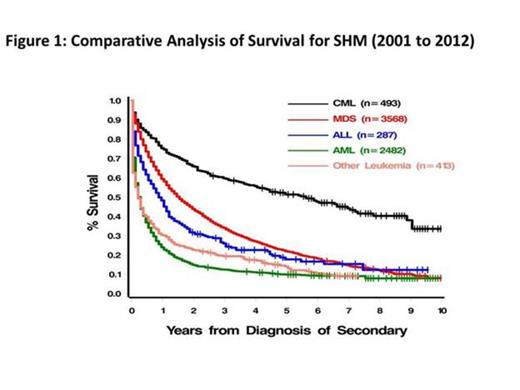
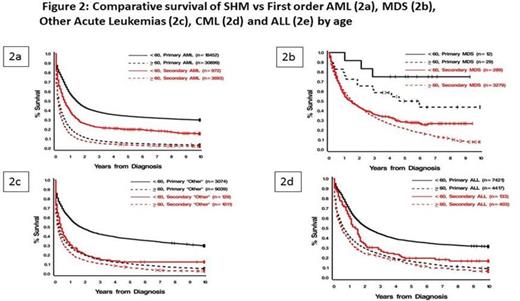
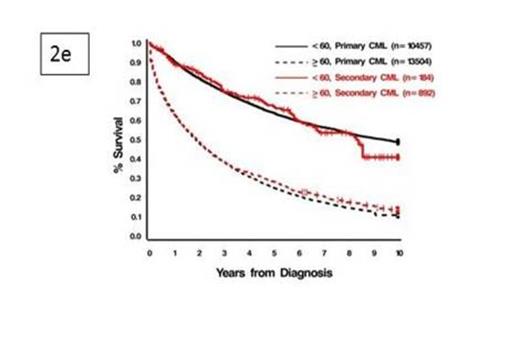
In univariable analyses, age <60 yrs predicted for better survival (p<0.0001) for all SHM, as did diagnosis in recent yrs (2001-2012) (p< 0.0001 for AML, OAL, CML & ALL). Effect of time period on survival for MDS was not done, as it became formally reportable in 2001. Having >2 primaries was associated with an unfavorable outcome for subsequent AML (HR=1.15; 1.08-1.23; p < 0.0001), MDS (HR=1.13; 1.05-1.22: p=0.001) & CML (HR=1.30; 1.13-1.48: p=0.0002). In multivariable analyses, advancing age was an independent adverse prognostic factor for all secondary leukemias & MDS, both as a continuous variable & when categorized as <60 yrs vs. >60 yrs (p<0.001). Race & gender did not impact survival. Using breast cancer as a referent primary, AML pts had worse outcomes following colorectal (HR=1.31; 1.14-1.5; p=0.0002) or lung (HR=1.46; 1.22-1.74; p< 0.0001) primaries, while MDS pts fared worse with prior lung (HR=1.61; 1.22-2.12; p=0.0007) or Non-Hodgkin lymphoma (HR=1.58; 1.3-1.92: p< 0.0001). Of all 2ndCML cases, those after colorectal cancer had worst survival (HR=1.54; 1.12-2.13; p=0.008). Among SHM pts, MDS pts had better survival than those with AML (HR=0.42; 0.4-0.44: p< 0.0001), as did pts with CML (HR=0.37; 0.35-0.41: p< 0.0001) & ALL (HR=0.64; 0.58-0.70; p< 0.0001). Out OAL had similar outcomes compared to AML (HR=0.99; 0.92-1.05; p=0.66). Pts with CML fared better than MDS (HR=0.47; 0.41-0.54; p< 0.0001) & OAL (HR=0.37; 0.34-0.41: p< 0.0001). Pts with ALL had worse survival than CML (HR=1.8; 1.6-2.03: p< 0.0001) & MDS (HR=1.28; 1.11-1.48: p=0.0005), but better than OAL (HR=0.65; 0.58-0.73: p< 0.0001). (Figure 1) Patients with all SHM, except CML, had worse outcomes compared to those with primary hematologic cancers (Figure 2).
Conclusion
The prolonged latencies for SHM in this study suggest that they are likely therapy-related. Our findings show that type & number of primary cancers influence survival of subsequent leukemias & MDS. SHM have worse survival compared to those with primary hematologic malignancies except CML where non-separation of survival curves suggest that CML as SHM does not behave like a therapy-related neoplasm.
Sekeres:TetraLogic: Membership on an entity's Board of Directors or advisory committees; Amgen: Membership on an entity's Board of Directors or advisory committees; Celgene Corporation: Membership on an entity's Board of Directors or advisory committees.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal