Abstract

Introduction: Diffuse large B-cell lymphoma (DLBCL) is the largest subgroup of malignant lymphoma. Today more than 80% of the patients will achieve partial or complete remission. However more than 20 % will either relapse or present with refractory disease. The standard approach for patients without major comorbidity is salvage treatment followed by high dose therapy with autologous stem cell transplant (HDT). This potentially curative treatment is toxic with many side effects and procedure related mortality, and therefore identification of patients eligible for HDT is a difficult challenge.
Objectives: Patients with relapse of de novo DLBCL and transformed indolent lymphoma (TIL) were included. The aim was to identify clinical prognostic markers that can identify patients who will not benefit from HDT.
Methods: From the national lymphoma registry patients with relapse of B-cell lymphoma in Denmark in the period 2000-2012, who underwent HDT, were extracted. Medical records were reviewed for clinical, pathological, and treatment information, and outcome. Patients were followed until death or emigration or until February 1, 2015. The Kaplan-Meier method was used to estimate overall survival (OS) and progression free survival (PFS). Cox regression models were used to assess prognostic factors.
Results: A total of 370 patients were included, 174 with de novo DLBCL, and 196 with TIL, 143 of the 196 had histologically confirmed transformation. Median age was 58 (22-73), and 59% of the patients were male.
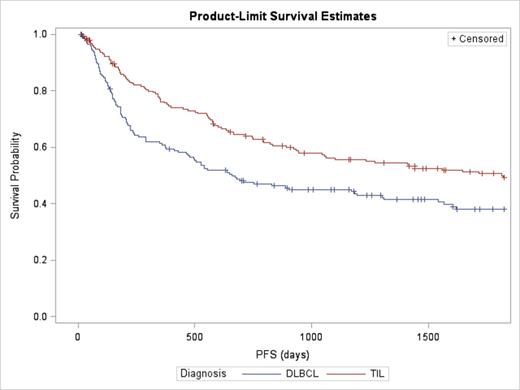
With a median follow-up of 82 months from HDT, the 5-year OS was 52% and the 5-year PFS was 44% (median PFS 3.2 years). For the DLBCL patients the 5-year OS was 43% and the 5-year PFS was 38%. For TIL patients the OS was 62% and the PFS 49% (figure 1).
During the first 100 days, 29 patients (8%) were admitted to the intensive care unit (14 DLBCL), and only four of these patients were alive at six months. The non-relapse mortality (NRM) at day 100 was 6 % for both groups, after five years 25% for DLBCL and 15% for TIL.
No significant difference in 5-year PFS was seen between sexes or age, but patients younger than 58 had better 5-year OS compared to patients aged 58 or above (p=0.047).
There was no difference in relapse treatment (DHAP vs ICE). Smoking (ever vs. never) caused a significantly worse OS (p=0.034). All IPI-factors, except Ann Arbor stage, was of prognostic importance (PFS). Primary refractory disease was of poor prognostic importance (p=0.001), and in patients, for whom the time from last salvage treatment to reinfusion of stem cells was more than 2 months, had a worse outcome (p=0.006). Patients, with less than 20 days of hospital admission in the period from the date of relapse to start of HDT, had a significantly higher survival (OS and PFS) (p>0.001).
In a multivariate analysis (PFS), LDH above upper normal reference, HR 1.4 (95% CI: 1.0;2.1), involvement of more than one extranodal site, HR 1.6 (1.1;2.3) primary refractory disease, HR 1.6 (1.1;2.3) and more than two earlier relapses, HR 1.9 (1.1;3.5) were all factors associated with adverse outcome.
For OS, the multivariate analysis showed, that patients with TIL had a better outcome, HR 0.7 (0.5;0.9), compared to DLBCL. Age above 58, HR 1.5 (1.1;2.1), involvement of more than one extranodal site, HR 1.9 (1.4;2.8), and primary refractory disease, HR 1.6 (1.1;2.3) were factors associated with adverse outcome.
Discussion:
In this population based study we find a 5-year OS of 52% after HDT and a 5-year PFS of 44%. Patients with TIL have a significantly higher 5-year PS (49%) than patients with de novo DLBCL (38%) whereas NRM is identical for the two groups at day 100 (6%). However, NRM increases subsequently more for DLBCL than for TIL over time to 25% and 15 % respectively after five years. Furthermore we show that hospitalization days less than 20 and postponement of stem cell infusion beyond 2 month after harvest may be useful parameters that can identify patients that have better or worse outcome after HDT.
This nationwide study cohort with the long follow-up period is applicable to a general population of patients, and this may explain the somewhat lower outcome compared to other published HDT cohorts.
Progression Free Survival (PFS) curves for Diffuse Large B-Cell Lymphomas (DLBCL) and Transformed Indolent Lymphomas (TIL) after high dose therapy with autologous stem cell transplant
Progression Free Survival (PFS) curves for Diffuse Large B-Cell Lymphomas (DLBCL) and Transformed Indolent Lymphomas (TIL) after high dose therapy with autologous stem cell transplant
Brown:Bayer: Consultancy; Roche: Consultancy, Speakers Bureau.
Author notes
Asterisk with author names denotes non-ASH members.

This icon denotes a clinically relevant abstract

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal