Abstract
Background: Donor selection is one of key factors for better outcomes after hematopoietic stem cell transplantation (HSCT). It is shown that increased donor age is associated with high mortality. In the era of high-resolution typing of HLA and various methodological options in HSCT (e.g. conditioning regimens or cell source), however, the significance of donor age in the selection of donor or cell source is unclear. Here we examined the impact of donor age on clinical outcome after unrelated bone marrow transplantation (UBMT) and compared to the outcome after unrelated cord blood transplantation (UCBT).
Patients and methods: For this retrospective cohort study, clinical data of donors and recipients were obtained from the registry data of the Japan Society of Hematopoietic Cell Transplantation (JSHCT). This study included 6035 adult patients 16 years of age or older with AML, MDS, ALL, or CML who received the first HSCT between 2000 and 2010. Among them, 3304 recipients received UBMT from 8/8 HLA-matched or 7/8 HLA-matched for HLA-A, -B, -C, and -DRB1 allele-level donor and 2731 recipients received single-unit UCBT from maximum 2-antigen (HLA-A, -B, -DR antigen-level) mismatched donor. Risk factors for overall mortality and other endpoints were analyzed using Cox proportional hazards models and Fine and Gray's proportional hazards models, respectively.
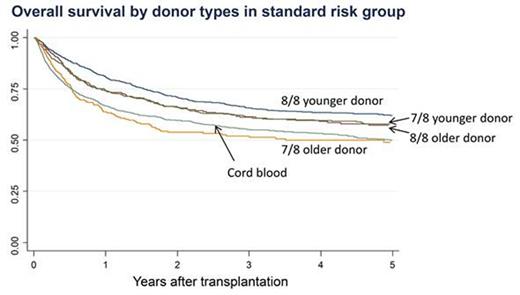
Results: The median ages of UBMT and UCBT recipients were 42 years (range, 16-77) and 50 years (range, 16-82), respectively. The median age of UBMT donor was 34 years (range, 20-55). Among 3304 UBMT recipients, older donor age (≥40 years) was a significant risk factor for overall mortality (adjusted HR, 1.14; 95% CI, 1.03-1.27, p=0.015) and grades II-IV acute graft-versus-host disease (aGVHD) (adjusted HR, 1.27; 95% CI, 1.13-1.43, p<0.001) after adjusting for other significant factors in the multivariable model. Similar results were obtained using donor age as a continuous variable (overall mortality: adjusted HR, 1.01; 95% CI, 1.00-1.02, p=0.007, aGVHD: adjusted HR, 1.02; 95% CI, 1.01-1.03, p<0.001). The effect of donor age on overall mortality was strongly detected in patients with the standard risk disease (interaction p=0.058) or recipients from 7/8 HLA-matched donor (interaction p=0.078). Therefore, we compared outcomes of the five groups including UCBT by donor types (8/8 matched younger donor, 8/8 matched older donor, 7/8 matched younger donor, 7/8 matched older donor and cord blood) only among the standard risk group (Figure). Survival in recipients from 8/8 matched older donor was similar to that in recipients from 7/8 matched younger donor (adjusted HR, 1.03; 95% CI, 0.83-1.28, p=0.790). In recipients from 7/8 matched older donor, the survival was comparable to that in recipients of cord blood (adjusted HR, 0.91; 95% CI, 0.73-1.13, p=0.398).
Conclusions: The outcome of HSCT recipients with older donor (≥40 years) was worse compared with that of recipients with younger donor, especially in the standard risk group or HLA-mismatched donors. A 7/8 matched younger donor is a viable option as well as an 8/8 matched older donor in the absence of an 8/8 matched younger donor. In addition, UCBT is a reasonable option in the absence of these donors. Intensive GVHD prophylaxis in recipients with older donor might improve outcome, but further studies are needed to test this hypothesis.
Probability of overall survival by donor types among HCT recipients with standard risk.
Probability of overall survival by donor types among HCT recipients with standard risk.
No relevant conflicts of interest to declare.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal