Abstract
Introduction: Insulin-like growth factor binding proteins (IGFBP) are carriers of insulin-like growth factors (IGFs). They prolong their half-life and modulate their availability and activity. The IGF-signaling system has been shown to have an important role in various solid cancers and hematologic malignancies. High levels of IGFBP2 and IGFBP7 have been associated with chemoresistance, relapse and inferior survival in different leukemias. Acute promyelocytic leukemia (APL) is a distinct subtype of acute myeloid leukemia (AML), which has been reported to have increased expression of IGFBP2. However, there is no data on its impact on prognosis. In addition, no data exist on IGFBP7 in APL. The aim of this study was to elucidate the influence on prognosis of both candidate genes in APL patients.
Methods: Expression levels of IGFBP2 und IGFBP7 were retrospectively analysed in bone marrow (BM) samples at the time of initial diagnosis from 69 APL patients (42 female, 27 male) after informed consent. Median age of patients was 46 years (range 19 to 82 years). All patients were diagnosed and treated in the German AML Cooperative Group (AMLCG) studies. Treatment consisted of simultaneous ATRA and double induction chemotherapy including high dose ara-C, one cycle of consolidation chemotherapy and 3 years monthly maintenance chemotherapy. In patients older than 60 years, the second induction cycle was at the discretion of the treating physician. Three patients (4%) received an induction of ATRA and an anthracycline without ara-C. BM samples of 22 healthy volunteers served as a control group. Multiplex reverse transcriptase quantitative real-time PCR (qRT-PCR) was performed on a LightCycler® 480 (Roche, Mannheim, Germany) PCR system. Glucose-6-phosphat isomerase was used as a housekeeping gene. For quantification of relative expression values a modified delta-delta CT calculation model according to Pfaffl was used after determination of PCR efficiencies. cDNA from the cell line K562 served as a calibrator in each run. All reactions were performed in triplicates. IGFBP2 expression groups were defined as follows: Patients with IGFBP2 expression below or equal the 25th percentile (IGFBP2low) were compared to patients with higher IGFBP2 expression (IGFBP2high). Overall survival (OS), relapse free survival (RFS) and the cumulative incidence of relapse (CIR) were calculated using the Kaplan-Meier method and a log-rank test was used to compare differences between the groups (p < 0.05).
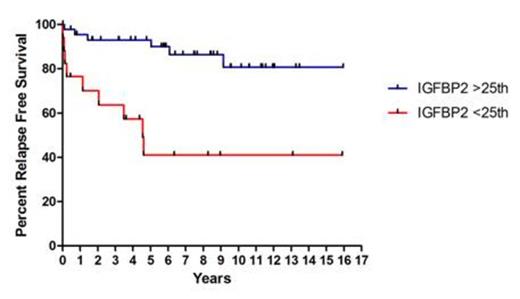
Results: Expression levels of IGFBP2 did not differ between APL patients and healthy controls. However, there was a significantly higher relapse rate in APL patients with low IGFBP2 expression (CIR: 25% in the IGFBP2low group vs. 5% in the IGFBP2high group; p=0.04). Accordingly, RFS of patients in the IGFBP2low group was also inferior (41% vs. 81% in the IGFBP2high group; p=0.0002; Fig. 1). The OS of patients who had responded to induction therapy was also influenced by IGFBP2 expression (OS of responders: 61% for IGFBP2low vs. 83% for IGFBP2high; p=0.02). However, there was no significant difference in the analysis of OS of all patients including patients who suffered early death.
In contrast to these findings, IGFBP7 was expressed significantly lower in APL patients compared to healthy controls (p<0.0001) but there was no association with outcome of APL patients.
Conclusion: Of the two analysed IGFBP family members only IGFBP2 showed impact on the prognosis of APL patients. Remarkably, IGFBP2 was not overexpressed compared to healthy controls in our patient cohort. The reason might be that whole BM samples of healthy controls were used instead of subpopulations. Still, among the APL patients cohort its expression showed a strong influence on prognosis especially on relapse rate and RFS. To find low expression as a negative prognostic marker is surprising as for leukemias only high expression has been reported as a negative factor. However, IGFBP2 has been proposed to suppress tumor development through binding IGFs and preventing IGF-receptor driven tumorigenesis. This is supported by the fact that the IGFBP2 promotor is hypermethylated in various types of cancer. In summary, we identified low IGFBP2 expression as a novel prognostic marker for APL. Further investigations are warranted to clarify its possible role in leukemia.
No relevant conflicts of interest to declare.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal