Abstract
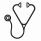
Advances in chemotherapy have improved the prognosis of patients with acute myeloid leukemia (AML), however, high-risk patients still have a poor outcome. In this category of patients, the only therapeutic strategy with curative potential remains allogeneic hematopoietic stem cell transplantation (allo-HSCT). With the aim to improve the effect of allo-HSCT by sequential use of chemotherapy followed by reduced intensity conditioning (RIC), we conducted a prospective study in high-risk AML patient. The high-risk population included intermediate II [t(9;11)(p22;q23); MLLT3-MLL, cytogenetic abnormalities not classified as favorable or adverse] and unfavourable patients [inv(3)(q21q26.2) or t(3;3)(q21;q26.2); t(6;9)(p23;q34); t(v;11)(v;q23); MLL rearranged, -5 or del(5q); -7; abnl(17p); complex karyotype] (Dohner et al. Blood 2010), secondary AML, and patients requiring 2 induction courses to obtain CR. The chemotherapy sequential regimen consisted in fludarabine 30 mg/m², high-dose cytarabine 2 g/m², and amsacrine 100 mg/m² from days -12 to -9 (FLAMSA). After 3 days of rest, RIC consisted of 4 Gy total-body irradiation (TBI) on day -5, cyclophosphamide (40 mg/kg with HLA-identical sibling, 60 mg/kg for unrelated or mismatched donors) on days -4 and -3, and rabbit antithymocyte globulin (ATG, Genzyme) (5 mg/kg total dose) from day -3 to day -1. In a group of patients, TBI was replaced by iv. busulfan (BU) (Busilvex, Pierre Fabre) 3.2 mg/kg/d during either 4 or 2 days according to patient age (>55 years) (from day -7 to -4 or from day -5 to -4). Peripheral-blood stem cells (PBSC) were preferred; bone marrow (BM) and cord blood (CB) were also accepted. Graft-versus-host disease (GvHD) prophylaxis consisted in cyclosporine from day -1, and mycophenolate mofetil (15 mg/kg bid), starting from day 0. In the absence of GvHD, MMF was discontinued by day+50 and cyclosporine was tapered from day +60 to +90. Except for CB transplantation, patients received 3 prophylactic increased doses of donor lymphocyte infusions (DLI) if they were in CR and GvHD-free at day +120 or 30 days after discontinuation of immunosuppressive agents starting at 1x106 CD3+ cells/kg. Between January 2007 and December 2013, 66 consecutive AML patients were included; 33 males and 33 females with a median age at allo-HSCT of 52 years (range: 19-66), 59 (89%) were de novo AML and 7 (11%) secondary AML. At transplantation, 22 (33%) patients were in CR (20 CR1 and 2 CR2) and 44 (67%) were in less than CR. Stem cell source was PBSC for 52 (79%) patients, CB for 6 (9%) and BM for 2 patients. Donors were 10/10 HLA matched siblings in 24 (36%) patients, 10/10 HLA matched unrelated in 18 (27%) patients and HLA mismatched for the rest of patients [unrelated 9/10 (n=18), CB 4/6 (n=6)]. For ABO compatibility, 32 (48%) were compatible, 13 (20%) had minor incompatibility and 21 (32%) had major incompatibility. For conditioning, 49 (74%) patients received TBI, 17 (26%) received BU. After transplantation, 59 (89%) patients engrafted, 7 patients did not engraft and died early (2 from relapse and 5 from infection). At day 90 post-allo-HSCT, among evaluated patients (N=52), 37 (71%) showed total donor chimerism, 15 (29%) had mixed chimerism. There were 24 patients with acute GvHD [10 gr I, 3 gr II and 7 gr III and 4 gr IV] with a cumulative incidence of 27% for grade ≥II; and 17 chronic GvHD [10 limited and 7 extensive], among them 5 after DLI, with a cumulative incidence of 48% at 2 years. After a median follow-up of 7 months (range: 0.1-76), the 2-years probability of overall survival (OS) and progression-free survival for the whole population were 30% (confidence interval: 24-36) and 40% (confidence interval: 37-52) respectively with a cumulative incidence of transplant-related mortality of 30% at 2 years. When stratifying on disease status at transplantation, patients in CR had significantly better OS and PFS at 2 years compared to patients in less than CR with 45% versus 18% (p=0.013) and 73% versus 22% (p=0.001) respectively. No statistical difference was found in outcomes of TBI compared to BU conditioning.
Patients in CR showed very promising results and could benefit the most from this strategy. A high rate of deadly infections was observed, thus an efficient prophylactic anti-infectious strategy is recommended. Patients not in CR remain having poor outcome and maybe new transplantation strategy using haploidentical donors could be interesting to evaluate in this population.
No relevant conflicts of interest to declare.
Author notes
Asterisk with author names denotes non-ASH members.
This icon denotes a clinically relevant abstract

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal