Abstract
<Background> The prognostic impact of interim positron emission tomography scans (I-PET) for patients with diffuse large B-cell lymphoma (DLBCL) is a matter of debate because its positive predictive value (20–80%) is low. Here, we aimed to improve the prognostic impact of I-PET by combining it with interim analysis of serum soluble interleukin-2 receptor (sIL2R) levels, the levels of which at the time of diagnosis are associated with the prognosis of DLBCL.
<Patients and Methods> We retrospectively examined data from DLBCL patients diagnosed at our institution between January 2006 and October 2013. Patients were included in the analysis if they met all of the following criteria: six or more cycles of rituximab plus CHOP regimen (R-CHOP); I-PET performed after 2-4 cycles of chemotherapy; and sIL2R levels measured after each cycle. Patients with primary central nervous system lymphoma, primary mediastinal large B-cell lymphoma, or transformed DLBCL from indolent lymphoma were excluded. I-PET was assessed visually according to the International Harmonization Project criteria. The interim sIL2R (I-IL2) level was defined as the value measured just before the fourth R-CHOP cycle. I-IL2 levels > 800 U/ml, or 2000 U/ml if serum creatinine was > 2.0 mg/dl (sIL2R is influenced by renal function), were regarded as positive. The primary endpoint of the study was progression-free survival (PFS). The unadjusted probabilities of PFS were estimated using the Kaplan-Meier method. The log-lank test and multivariate Cox regression analysis were used to assess the prognostic values of each clinical variable.
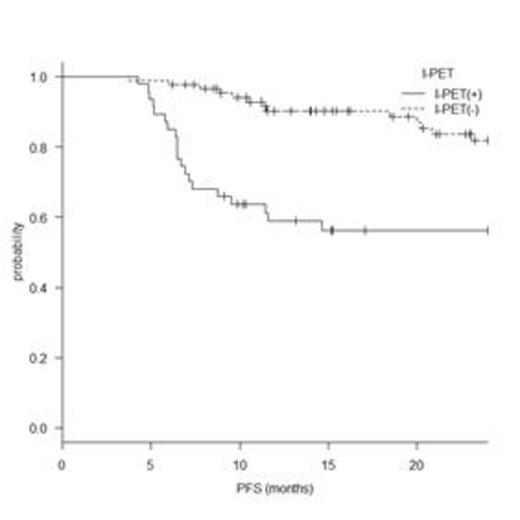
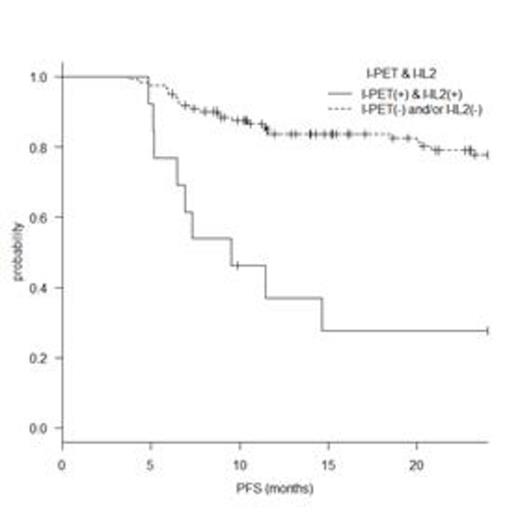
<Results> In total, 135 patients were enrolled. The median age was 66 years (range, 34–89) and 66 patients (48.9%) were male, 27 (20%) had an ECOG performance status >1, 18 (13.3%) had bulky disease, 81 (60%) had advanced disease, and 61 (45.2%) had a high or high-intermediate International Prognostic Index (IPI) score. The median follow-up time was 25.6 months (range, 6.3–88.7) and the 2 year progression-free survival rate (2-y PFS) of the entire cohort was 72.9% (95% confidence interval (CI), 63.8–80). I-PET and I-IL2 were positive in 47 (34.8%) and 15 (11.1%) patients, respectively. Univariate analysis revealed that a high IPI score, a positive I-PET, and a positive I-IL2 had statistically significant poor prognostic effects on PFS, although gender and bulky disease did not. The three significant variables were entered into multivariate analysis, which identified positive I-PET and I-IL2 values (but not IPI) as independently associated with a poor prognosis. The 2-y PFS was 81.8% (95% CI, 70.4–89.1) for I-PET-negative and 56.3% (95% CI, 40.7–69.3; p<0.001, log rank test) for I-PET positive, respectively. Although a negative I-PET was highly predictive of a favorable outcome, a positive I-PET was of limited clinical value. The 2-y PFS for the 13 patients (9.6%) that were both I-PET- and I-IL2-positive was significantly lower than that of the remaining patients (27.7% [95% CI, 7.1–53.6] and 77.7% [95% CI, 68.4–84.6], respectively; p<0.001). Patients that were positive for both I-PET and I-IL2, rather than patients that were positive for I-PET alone, had a poor outcome.
<Conclusion> DLBCL patients that were both I-PET- and I-IL2-positive suffered a high rate of progression; therefore, such patients should be targeted by novel therapeutic approaches. Because the study was based on a retrospective analysis and a limited follow-up period, further studies are needed to confirm the prognostic impact of the combined use of I-PET and I-IL2.
No relevant conflicts of interest to declare.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal