Abstract
Abstract 687
A persistently positive PET scan after just a few cycles of therapy is predictive of a poor clinical outcome in diffuse large B-cell lymphoma (DLBCL). Prior data suggested that about one third of patients remain PET positive after 2–4 cycles, with ≤ 20% 2 year progression-free survival (PFS) for such patients. A response-adapted strategy was studied in E3404 to test the hypothesis that an early treatment change to four cycles of R-ICE might reduce the treatment failure rate of patients whose PET scan remained positive after an initial 3 cycles of R-CHOP.
Previously untreated patients with DLBCL stage III, IV, or bulky II, with measurable disease, HIV negative, and with adequate organ reserve, were eligible. PET/CT scan was performed before treatment and again after 3 cycles of R-CHOP. A fourth cycle of R-CHOP was given while the scan was centrally reviewed and scored as either positive or negative for FDG-avid tumor by a single reviewer using criteria based on modifications of the Harmonization Criteria. Persistently PET-positive patients received 4 cycles of R-ICE, while PET-negative patients received 2 more cycles of R-CHOP, for a total of 6 cycles. PET/CT was performed again at the end of treatment. A ≥45% 2 year PFS for mid-treatment PET- positive patients was viewed as a promising result, with 88% power if 33 such patients were accrued. Total accrual of 99 patients was therefore planned.
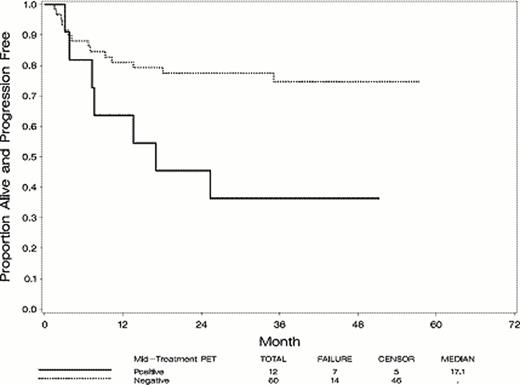
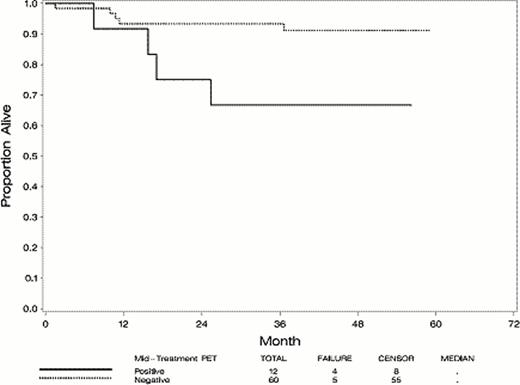
Of 100 patients accrued, 78 were eligible; all but 1 ineligibility was based on central pathology review. Fifty-eight were male; median age was 62 years (20–74); 13% IPI 0–1, 31% IPI 2, 37% IPI 3, and 19% IPI 4–5. Seventy-four of 78 (95%) patients completed the first 3 cycles of R-CHOP. Of 72 patients continuing treatment, 67 (93%) completed protocol treatment: 83% of mid-treatment PET-positive and 93% of PET-negative patients. Of 74 patients undergoing mid-treatment PET scan, 12 (16%) were scored as positive, and 62 (84%) as negative. At the end of treatment, 13% were scored as positive, and 87% as negative. Two-year PFS, from the time of study entry, was 72% among all eligible patients. Two year PFS from the time of mid-treatment PET scan was 45% (90% CI, 21–67%) for patients scored as mid-treatment PET-positive, and 77% (90% CI 67–85%) for patients scored as mid-treatment PET-negative. The 80% confidence interval (corresponding to a test with a one-sided type I error of 10%) did not include the null hypothesis of 25%, implying that the results met the pre-specified threshold. Among all 78 eligible patients, 10 have died (13%); 5-year overall survival was 87% (90% CI 78–92%) Three-year overall survival was 67% (90% CI 40–84%) for mid-treatment PET-positive patients, and 93% (90% CI 85–97%) for mid-treatment PET-negative patients.
The 2-year PFS for mid-treatment PET-positive patients met the threshold to be considered promising, but the confidence interval was wider than expected due to the small patient number. In addition, the inter-observer variability in the interpretation of mid-treatment PET scans as a binary variable in this study (studied and reported separately in Horning SJ et al. Blood 2010) implies that treatment modification based on early PET scanning should remain confined to clinical trials.
Swinnen:Celgene: Consultancy; Genentech: Research Funding. Quon:Genentech: Research Funding. Advani:Pharmacyclics: Research Funding. Kahl:Roche/Genentech: Consultancy; Celgene: Consultancy; Cell Therapeutics: Consultancy; Janssen: Consultancy; GSK: Consultancy; Gilead: Consultancy. Horning:Genentech: Employment; Roche: stock, stock Other.
Supported in part by PHS Grants CA21115, CA23318, CA66636, CA16116, CA21076, CA13650 and from NCI, NIH and DHHS.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal