Abstract
Abstract 3702
Romiplostim is a novel peptibody that increases platelet counts by a mechanism similar to endogenous thrombopoietin, and is approved for the treatment of chronic ITP. ITP is characterized by low platelet counts due to increased platelet destruction and suboptimal platelet production. The response rate to ITP therapies is variable and may be associated with substantial adverse effects. Splenectomy is commonly used as a treatment for ITP because it removes the major site of platelet destruction. A recent consensus report (Provan et al., 2010, 168–86) recommends delaying splenectomy for 6–12 months, in keeping with the new definition for chronic ITP (Rodeghiero et al., Blood 2009, 2386–93); therefore, we evaluated patients who had been diagnosed with ITP ≤1 year who participated in a recent study of romiplostim versus standard of care (SOC).
A randomized, open-label study was conducted in nonsplenectomized adult patients with ITP. The co-primary study endpoints were the incidence of treatment failure and the incidence of splenectomy. Treatment failure was defined as: platelet count ≤20 × 109/L for 4 consecutive weeks at the highest recommended dose and schedule of romiplostim or SOC, or major bleeding event, or change in therapy due to intolerable side-effect or bleeding symptoms. The secondary endpoints included platelet counts and safety. Patients who discontinued treatment were considered to have met both primary endpoints. To assess the impact of study discontinuation on the primary endpoints, the actual incidence of treatment failure and splenectomy were also determined (“sensitivity analysis”). An ad hoc analysis of the study endpoints was conducted in those study patients who had been diagnosed with ITP for ≤1 year.
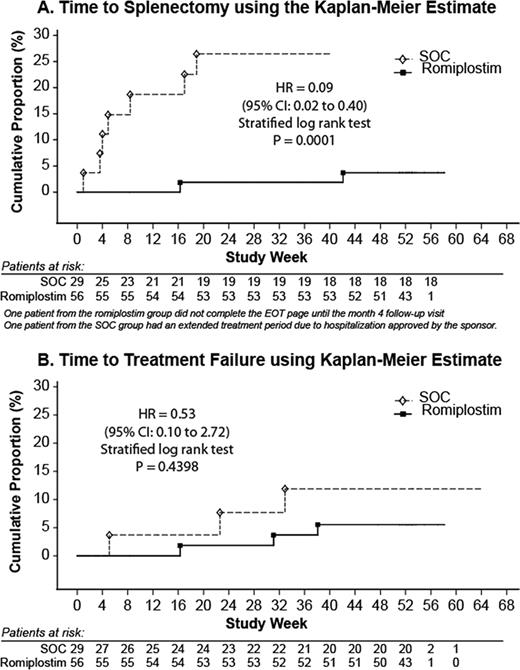
Eighty-five of 234 enrolled patients had ITP for ≤1 year; 29 received SOC and 56 received weekly subcutaneous injections of romiplostim. Patient characteristics were similar between treatment groups, as was the distribution of time since ITP diagnosis (romiplostim, 7 – 327 days; SOC 4 – 363 days). The mean (±SD) age was 53 (±20) years and 47% of the patients were male. The mean baseline platelet counts were similar in the romiplostim (26 ± 14 × 109/L) and SOC (23 ± 16 × 109/L) groups. The mean platelet count was higher in the romiplostim arm than the SOC arm at every weekly evaluation until the end of treatment (52 weeks). The incidence of treatment failure was lower in the romiplostim group (9%, 5/56) than in the SOC group (24%, 7/29) [OR, 0.34; 0.10 – 1.14; p= 0.0649]. Similarly, the incidence of splenectomy was significantly lower in the romiplostim group (7%, 4/56) than the SOC group (45%, 13/29) [OR, 0.10; 0.03 – 0.35; p<0.0001]. In addition, romiplostim-treated patients had a significantly longer time to splenectomy than SOC patients (p=0.0001) (Figure). The sensitivity analysis showed that the actual incidence of treatment failure was similar between treatment groups (romiplostim, 5%, 3/56; SOC, 10%, 3/29) [p=0.5589] and the actual incidence of splenectomy was significantly lower in romiplostim-treated patients (4%, 2/56) than in SOC-treated patients (35%, 10/29) [p=.0002]. The percentage of patients experiencing a serious bleeding event was similar (romiplostim, 6%; SOC, 4%). Serious adverse events occurred in 24% (13/55) of romiplostim patients and 46% (13/28) of SOC patients with the most common event being thrombocytopenia. No adverse events led to study withdrawal. Thromboembolic events occurred in one romiplostim-treated patient (pulmonary embolism) and one SOC patient (cerebral microangiopathy). There were no reports of increased reticulin, and no patients tested positive for neutralizing antibodies to romiplostim or TPO.
The results from this ad-hoc analysis of this subgroup indicate romiplostim may reduce the incidence of treatment failure and splenectomy in patients who have been diagnosed with ITP for 1 year or less, although the enrollment of patients with platelet counts >20 × 109/L may have contributed to reduced differences in the rates of treatment failure per the study definition. Romiplostim was well-tolerated in this patient population, and findings were similar to those previously reported for the study population overall (Kuter et al., ASH 2009, #679).
Boccia:Amgen Inc.: Consultancy, Honoraria, Research Funding, Speakers Bureau; GlaxoSmithKline: Consultancy, Honoraria, Research Funding, Speakers Bureau; Acendia: Consultancy; Celgene: Equity Ownership, Honoraria, Research Funding, Speakers Bureau; Merck: Equity Ownership; Johnson & Johnson: Equity Ownership; CTI: Research Funding; Cephalon: Research Funding; Millenium: Research Funding. Kuter:Amgen Inc.: Consultancy, Research Funding; GlaxoSmithKline: Consultancy, Research Funding; ONO: Consultancy; Pfizer: Consultancy, Research Funding; Shionogi: Consultancy, Research Funding. Macik:Amgen Inc.: Research Funding; Pfizer: Research Funding; Eisai: Research Funding; Grifols: Research Funding; FDA: Consultancy; Center for Biologics Evaluation and Research: Consultancy; Hematology Consultant: Consultancy. Pabinger:Amgen Inc.: Honoraria, Membership on an entity's Board of Directors or advisory committees; GlaxoSmithKline: Honoraria, Membership on an entity's Board of Directors or advisory committees. Selleslag:Amgen Inc.: Consultancy, Honoraria. Rodeghiero:Amgen Inc.: Consultancy, Honoraria, Speakers Bureau; GlaxoSmithKline: Consultancy, Honoraria, Speakers Bureau; Shionogi: Consultancy. Chong:CSL Australia: Consultancy, Honoraria, Membership on an entity's Board of Directors or advisory committees, Research Funding; Amgen Inc.: Honoraria, Membership on an entity's Board of Directors or advisory committees, Research Funding; GlaxoSmithKline: Honoraria, Membership on an entity's Board of Directors or advisory committees, Research Funding, Speakers Bureau. Wang:Amgen Inc.: Employment, Equity Ownership. Lizambri:Amgen Inc.: Employment, Equity Ownership.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal