Abstract
Abstract 100
This trial aimed to investigate the efficacy and safety of sequential treatment with rituximab and CHOP-21 in patients with PTLD unresponsive to reduction of immunosuppression. Methods: An ongoing prospective, multicenter, international phase II trial was initiated in January 2003. Initially patients were treated with a fixed sequence of rituximab at days 1, 8, 15 and 22 (4R) followed by four cycles of CHOP-21 combined with G-CSF support starting 4 weeks after the last dose of rituximab (sequential treatment, ST). Based on the results of an earlier interim analysis showing that the response to rituximab predicts OS the trial was amended in 2007 introducing risk stratification according to the response to 4R (risk stratified sequential treatment, RSST). In RSST patients achieving a complete remission after 4R (low risk) continue with four 3-weekly courses of rituximab monotherapy while patients in PR, SD or PD (high risk) are followed by four cycles of R-CHOP-21 + G-CSF. Results: This is a scheduled interim analysis after inclusion of a total of 104 patients. The median follow up is 34.0 months for ST (64 pts.) and 9.1 months for RSST (40 pts.). 61 ST and 35 RSST patients were diagnosed with monomorphic PTLD, 3/5 with polymorphic PTLD. 27/23 patients were kidney, 3/0 kidney+pancreas, 15/8 liver, 13/6 heart, 6/3 lung or heart+lung transplant recipients. Median age at diagnosis of PTLD was 53/60 years (mean age: 48/56 years). 59%/58% of patients had an advanced stage of disease (Ann Arbor III/IV) and 49%/47% of tumors were EBV positive. 75%/75% of patients had late PTLD (i.e. later than 1 year after transplantation). LDH was elevated in 71%/64% of patients, respectively. The overall response rate (ORR) to 4 initial courses of rituximab monotherapy (4R, N=104) was 54% with a CR-rate of 32% and the subsequent completion of treatment with CHOP or R-CHOP allowed a clear increase of the response (p<0.0001, Fig. 1). With ST the final ORR was 89% (CR rate: 69%). 86%, 75% and 75% of patients were without disease progression at one, two and three years, respectively (Fig. 2a). Disease free survival was 87%, 78% and 70% at one, two and three years. There were 6 early treatment associated deaths (9%) resulting from infections (1 from CMV-colitis, 1 from PcP-pneumonia, 1 from fulminant hepatitis, 3 from sepsis) and 2/64 patients died from refractory PTLD. Two further patients died due to hemorrhage during treatment. With RSST the ORR was 90% and 73% achieved a complete remission. 90% of patients were without disease progression at one year (Fig. 2a). There was one early treatment related death due to infection (2.5%). This patient died from sepsis secondary to intestinal perforation in response to R-CHOP treatment. 2/40 patients died from refractory PTLD. With 1 event in 16 patients in both, the ST and the RSST-arms, subsequent consolidation with rituximab monotherapy (RSST) seems not to be inferior to consolidation with 4 cycles of CHOP (ST) in patients with a CR after 4R. Up to now there is no difference in toxicity between CHOP and R-CHOP in ST/RSST. Patients failing to achieve a complete remission with 4R (72 patients) seem to benefit from the subsequent escalation from CHOP to R-CHOP (Fig. 2b). Conclusions: This is the largest prospective study in PTLD. Sequential treatment with rituximab and CHOP-21 + G-CSF is well tolerated and highly effective with a treatment related mortality of less than 10% and an efficacy of up to 90%. In comparison to historic series of rituximab monotherapy, significantly more patients achieve a CR with sequential treatment and time to progression (TTP) is very much prolonged. In comparison to historic series of CHOP, sequential treatment is much better tolerated. This may result from a lower tumor burden and a better patient fitness at the time chemotherapy is applied. Introduction of risk stratification according to the response to 4 courses of rituximab monotherapy might further improve these results restricting chemotherapy related toxicity to high risk patients while these data suggest that low risk patients can effectively be treated with extended rituximab monotherapy. Thus, risk stratified sequential treatment (RSST) might further improve OS in this difficult to treat disease.
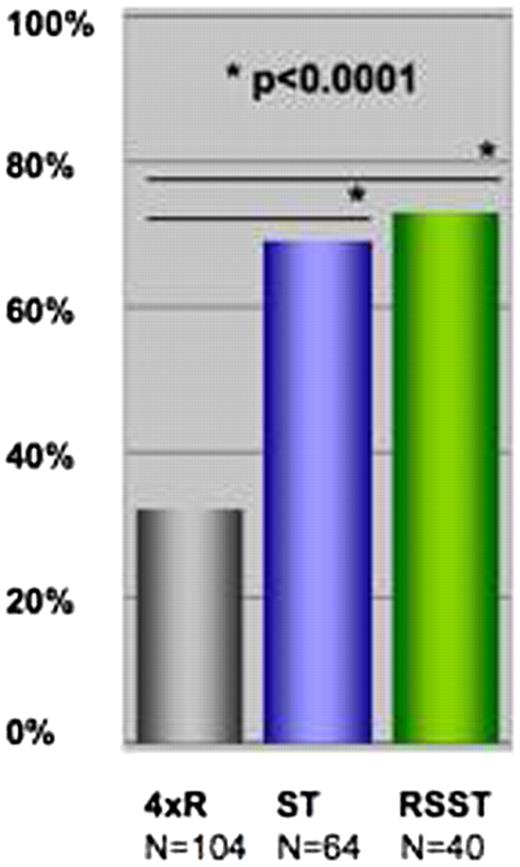
Complete remission rates after four initial courses of rituximab monotherapy (4R) and after completion of therapy in the ST and RSST treatment arms
Complete remission rates after four initial courses of rituximab monotherapy (4R) and after completion of therapy in the ST and RSST treatment arms
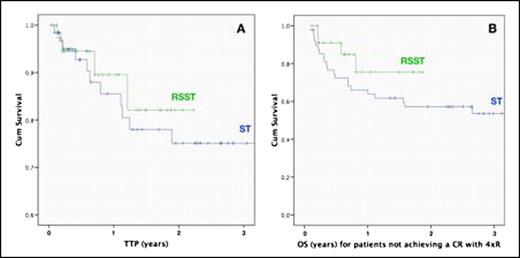
A: Time to tumor progression (TTP, N=104) and B: overall survival (OS) of patients not achieving a CR with 4 courses of rituximab (N=72) in the ST and RSST treatment approach
A: Time to tumor progression (TTP, N=104) and B: overall survival (OS) of patients not achieving a CR with 4 courses of rituximab (N=72) in the ST and RSST treatment approach
Trappe:Hoffmann La Roche Ltd.: Consultancy, Honoraria, Research Funding; AMGEN GmbH: Research Funding. Choquet:Hoffmann La Roche Ltd.: Consultancy, Honoraria. Oertel:Hoffmann La Roche Ltd.: Employment, Equity Ownership. Leblond:Hoffmann La Roche Ltd.: Consultancy, Honoraria, Research Funding. Ekman:Hoffmann La Roche Ltd.: Honoraria. Dührsen:Hoffmann La Roche Ltd.: Honoraria, Research Funding. Salles:Hoffmann La Roche Ltd.: Consultancy, Honoraria, Research Funding. Morschhauser:Hoffmann La Roche Ltd.: Honoraria. Riess:Hoffmann La Roche Ltd.: Consultancy, Honoraria, Research Funding; AMGEN GmBH: Consultancy, Honoraria, Research Funding.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal