Introduction
Oh what a difference a decade makes! In a landmark paper published in 1996, Feder and colleagues identified the long-sought gene mutated in patients with classical hereditary hemochromatosis. In many ways, this seemed to ignite an explosion in iron biology which, over the next 10 years, led to a remarkably detailed (though still incomplete) understanding of the pathophysiology of hemochromatosis. Many discoveries critical for understanding iron homeostasis, however, were kindled by earlier work dating back half a century and more. This review will emphasize advances made between the birth of the American Society of Hematology (ASH) in 1958 and the present. In the early part of that period, ferrokinetic studies provided important insights into human iron homeostasis in vivo (reviewed in Finch et al1 ). More recently, modern molecular biology and genetic studies of model organisms have extended our knowledge of normal iron biology and led to detailed understanding of human iron disorders. Ironically, a comprehensive review on iron metabolism appeared in Blood exactly 50 years ago, describing a current state of knowledge that was viewed as quite complete at the time.2 Adding to the irony, that author, Hugh Josephs (another pediatric hematologist), had 54 journal pages and I only have 12!
Cellular regulation of iron homeostasis
The earliest molecular studies of iron metabolism focused on 2 molecules that are both abundant and easy to isolate. In 1937, horse spleen ferritin was the second of all proteins to be crystallized.3 Transferrin was identified as an abundant plasma iron transport protein a decade later.4 Both of these molecules are now used clinically in assays of iron status. Both ferritin and transferrin sequester iron to keep it nonreactive, thus precluding the Fenton chemistry that promotes formation of oxygen radicals. But they do so in very different ways. Ferritin, which has homologs in all organisms except yeast, is a cagelike heteropolymer of 24 subunits of H- (heavy or heart) and L- (light or liver) types, which can hold up to 4500 iron atoms.5 As pointed out by Munro, it is unique among enzymes in that it stores its substrate after acting upon it.6 H-ferritin is slightly larger than L-ferritin, and has ferroxidase activity important for movement of iron into the solid-state core of the protein. Most ferritin is used to store within cells, but a very small amount enters a distinct secretory pathway, destined for glycosylation and release into the serum. Aside from its useful role as a semiquantitative indicator of iron stores, the biologic purpose of serum ferritin remains unknown. Ferritin receptors are present on lymphocytes and some other cell types, but their physiologic function has not been fully defined.7 Ferritin is also the precursor to hemosiderin, a heterogeneous aggregate of iron, lysosomal components, and other products of intracellular digestion.8
In contrast, transferrin is actively secreted by hepatocytes, the cells that express it most vigorously. Transferrin is also produced on the sanctuary sides of the blood/testes barrier, by Sertoli cells, and the blood/brain barrier, by several distinct cell types. It serves the general purpose of binding iron, keeping it soluble in an aqueous environment and delivering it to tissues. The mammalian transferrin molecule has 2 similar iron-binding lobes, each capable of holding one atom. Lower eukaryotes have transferrins analogous to 1 of the 2 mammalian lobes. It has been proposed that the double site transferrin molecule evolved at the same time that functional kidneys appeared, increasing the size of the protein to prevent loss by filtration.9
Transferrin keeps iron nonreactive in the circulation and in extravascular fluid, delivering it to cells bearing specific transferrin receptors. The classical transferrin receptor, TFR1, is found in largest amounts on rapidly dividing cells, on activated lymphocytes, and on erythroid precursors. It selectively binds diferric transferrin to internalize it through a constitutive pathway of receptor-mediated endocytosis (the transferrin cycle), which has become a paradigm in cell biology (Figure 1).
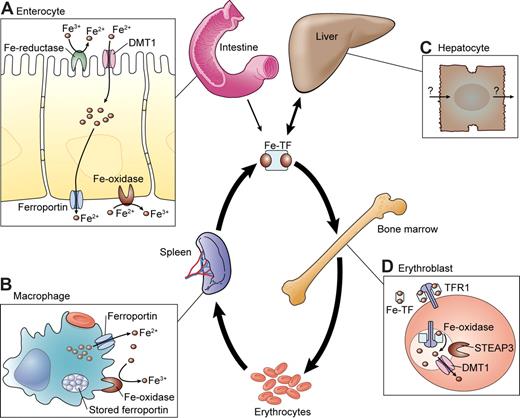
Overview of iron homeostasis. The central portion of the figure depicts the flow of iron into the body (through the small intestine), to transferrin (Tf), to the major site of utilization (the erythroid bone marrow), to circulating erythrocytes, to tissue macrophages that phagocytose senescent erythrocytes and recycle iron (spleen), to storage in hepatocytes, and back to TF through mobilization of iron stores. Cellular iron transport is described in detail in the text and shown in schematic form on the outside edges of this figure. (A) Nonheme iron transport across an intestinal enterocyte. (B) Erythrophagocytosis and iron recycling in a tissue macrophage. The aqua oval in the cytoplasm represents a storage depot for ferroportin protein within the cell. (C) Hepatocyte iron transport, with arrows indicating that neither import nor export is well understood. (D) Iron uptake through the transferrin cycle in the erythoblast. Illustration by Kenneth Probst.
Overview of iron homeostasis. The central portion of the figure depicts the flow of iron into the body (through the small intestine), to transferrin (Tf), to the major site of utilization (the erythroid bone marrow), to circulating erythrocytes, to tissue macrophages that phagocytose senescent erythrocytes and recycle iron (spleen), to storage in hepatocytes, and back to TF through mobilization of iron stores. Cellular iron transport is described in detail in the text and shown in schematic form on the outside edges of this figure. (A) Nonheme iron transport across an intestinal enterocyte. (B) Erythrophagocytosis and iron recycling in a tissue macrophage. The aqua oval in the cytoplasm represents a storage depot for ferroportin protein within the cell. (C) Hepatocyte iron transport, with arrows indicating that neither import nor export is well understood. (D) Iron uptake through the transferrin cycle in the erythoblast. Illustration by Kenneth Probst.
To initiate the transferrin cycle, patches of cell-surface membrane carrying receptor-ligand complexes invaginate to form clathrin-coated endosomes. After clathrin is removed the endosomes become acidified through proton influx, leading to conformational changes in both transferrin and TFR1, and promoting iron release. Liberated inorganic iron is then reduced by the ferrireductase STEAP3 to Fe2+,10 which is the substrate for transmembrane transport by divalent metal transporter 1 (DMT1 or SLC11A2, formerly called NRAMP2, DCT1).11-13 Both STEAP3 and DMT1 were discovered through positional cloning of genes altered in rodents carrying spontaneous mutations impairing iron transport.10,11 The use of mutant animal models to identify key iron transport molecules has been remarkably productive, and a hallmark of work of the past decade (reviewed in Andrews14 ). This powerful strategy takes advantage of mutants discovered and maintained over the last century, analyzed using modern genetic techniques.
Gunshin13 and Hediger15 showed that DMT1 is electrogenic, requiring proton cotransport to move Fe2+ across the membrane. This need is met by the low pH milieu of the transferrin cycle endosome (internal pH approximately 5.5). The subsequent fate of iron that exits the transferrin cycle endosome is not well understood, but in erythroid cells most is needed for heme biosynthesis. To make heme, iron must again cross an ion-impermeable membrane to enter the mitochondrion. The mitochondrial iron importer was recently identified as mitoferrin (also known as SLC25A37), a transmembrane protein that plays a critical role in supplying iron to ferrochelatase for insertion into protoporphyrin IX. Mitoferrin was originally discovered in yeast (called MRS3/MRS416 ) and in a mutant zebrafish.17 Interestingly, mutations in mitoferrin result in a clinical disorder that is very similar to erythropoietic protoporphyria caused by ferrochelatase mutations.17
Although many tissues express TFR1 at low levels, relatively few cell types are strictly dependent on the transferrin cycle for iron uptake. Targeted disruption of the Tfr1 gene in mice demonstrated that most tissues develop normally without Tfr1, but erythroid precursors, early lymphoid cells, and neuroepithelial cells require Tfr1 for differentiation.18,19 The likely role of TFR1 in erythropoiesis is obvious—the transferrin cycle serves to concentrate iron in the vicinity of DMT1 to maximize iron assimilation for hemoglobin production. However, it is less clear why lymphopoiesis and neurodevelopment should require TFR1.
In the past it was assumed that iron assimilated by erythroid precursors was incorporated into hemoglobin, remaining within the cells until erythrocyte senescence. Recently, however, Quigley and colleagues20 have described a heme exporter, FLVCR, which appears to be necessary for normal erythroid development. They hypothesize that erythroblasts need to have a pop-off valve for extra heme to avoid its toxicity. Targeted disruption of the mouse gene encoding FLVCR demonstrated the importance of this protein in vivo.21 FLVCR-null mice had a failure of definitive erythropoiesis, resulting in fetal demise. Interestingly, the fetuses had craniofacial and limb deformities suggestive of Diamond-Blackfan anemia. When the FLVCR gene was inactivated after birth the animals developed severe, macrocytic anemia, implying that heme export is important for normal erythropoiesis.
Regulation of intracellular iron homeostasis
Intracellular iron homeostasis is maintained, at least in part, through a very elegant posttranscriptional regulatory mechanism. In 1987, investigators observed that conserved sequences in the 5′ untranslated regions (UTRs) of both H- and L-ferritin mRNAs were needed to control a ready but quiescent pool of ferritin mRNA in the cell, which could quickly be mobilized to produce ferritin protein when iron was abundant.22,23 Thermodynamic predictions indicated that the UTR sequences could form stable RNA hairpins with a characteristic secondary structure, termed iron responsive (or regulatory) elements (IREs).24 Soon afterward it was shown that cytoplasmic proteins, now known as iron regulatory proteins (IRPs, formerly IREBPs), recognize and bind to the IREs.25-28
The 2 known IRPs share sequence homology but have distinctive properties. At the time of its discovery, IRP1 was recognized to bear strong similarity to aconitase, a mitochondrial enzyme of the tricarboxylic acid cycle. Remarkably, IRP1 also has aconitase activity, making it a prime candidate for a previously described cytoplasmic aconitase.29,30 But the aconitase and IRE-binding activities are mutually exclusive, providing a clue to a clever regulatory switch. Similar to a number of other iron-containing proteins, IRP1 incorporates an iron-sulfur cluster (4Fe•4S). The iron-sulfur cluster forms when iron is abundant, but disassembles when iron is scarce. Haile and Rouault showed that the aconitase activity of IRP1 is present only when the iron-sulfur cluster is complete; when it is not, IRP1 acts as an RNA binding protein, recognizing IREs.31 IRP2, on the other hand, does not incorporate an iron-sulfur cluster. Rather, its activity is regulated at the level of protein stability. Under low iron conditions IRP2 accumulates, but when iron is abundant it triggers IRP2 degradation.32-36 It is still not entirely clear why it is necessary to have 2 IRPs, but recent observations suggest that the 2 may respond differently over the physiologically relevant range of oxygen tensions.37 They may also have somewhat different target selectivity among IRE-containing mRNAs.
The ferritin IRE is located just upstream of the start codon for protein translation. Muckenthaler and colleagues showed that IRP binding sterically blocks recruitment of the small ribosomal subunit to the initiation complex, thus preventing translation.38 As a result, ferritin protein production is abrogated under low iron circumstances when the small amount of intracellular iron is needed for cellular functions. On the other hand, when iron is abundant, translational repression is relieved and newly made ferritin subunits assemble to provide iron storage capacity.
The IRE/IRP regulatory system is also used to control expression of other proteins. The best studied is TFR1, which has multiple IREs in the 3′ UTR of its mRNA.39 In this case, IRP regulation operates in a very different fashion. Under low iron conditions, IRP binding has no direct effect on translation, but rather it protects the TFR1 mRNA from endonucleolytic cleavage and consequent degradation. When iron is abundant, nucleases attack A-U rich mRNA sequences adjacent to the IREs and destabilize TFR1 mRNA. Thus, more TFR1 can be produced when cells are in need of iron, but TFR1 expression is interrupted when cells are iron replete.
Other mRNAs encoding important proteins of iron metabolism have been shown to have 5′ IREs (eg, ferroportin, aminolevulinic acid synthase) or 3′ IREs (eg, DMT1), though their regulation by the IRE/IRP system has not been thoroughly studied.40
Perhaps surprisingly, targeted disruption of the IRP1 gene in mice produces no apparent phenotypic abnormalities.41 In contrast, targeted disruption of IRP2 leads to a disorder of iron homeostasis characterized by microcytic, hypochromic anemia,42,43 and, at least in one laboratory, a late onset neurodegenerative disorder.42,44,45 When genes encoding both proteins are inactivated, the compound mutant mice die early in embryonic development, establishing the overall importance of these proteins in vivo.
Spontaneous IRE mutations have been described in human patients and in mice.46-48 Beaumont and colleagues48 showed that disruption of the L-ferritin IRE results in hyperferritinemia-cataract disease, with prominent ocular findings and elevated serum ferritin but no evidence of disturbed iron homeostasis. Disruption of the H-ferritin IRE in one Japanese family was associated with a familial iron overload disorder.49 Interestingly, a mutation that prevents formation of the mouse ferroportin IRE causes an unusual and complex disorder of iron homeostasis, underscoring the significance of this IRE in vivo.50
Intestinal iron absorption
In nontransfused individuals, iron enters the body exclusively through the diet. Because there is no regulated excretion of iron through the liver or kidneys, iron balance is primarily controlled at the level of intestinal absorption. Elegant ferrokinetic studies carried out in the middle of the last century gave important physiologic insights into human iron absorption and distribution51 but a molecular understanding of iron absorption came decades later (and is still not complete). When we and others began efforts to find intestinal iron transporters in the mid-1990s the available clues were not particularly helpful: (1) the transferrin cycle was known to have no direct role in intestinal iron absorption, (2) mammalian iron transport appeared to be mechanistically distinct from that of bacteria and single-celled eukaryotes, and (3) ATPase copper transporters, discovered several years earlier, showed no affinity for iron. Protein purification had been attempted for decades without success. In spite of these obstacles and entirely by chance, the first mammalian transmembrane iron transporter was discovered simultaneously in 2 laboratories, located within a city block of each other in Boston, using singularly modern techniques.12,13 Ours was one of those labs, and this marked our entrée into the field of iron biology. Our approach was to take advantage of well-characterized mouse strains that carried spontaneous mutations perturbing iron homeostasis. At the time, 6 strains had been identified; all are now understood in molecular detail.14 One in particular, microcytic anemia (mk), had been carefully studied and shown to have a defect in intestinal iron absorption.52
Iron absorption takes place in the proximal portion of the duodenum (Figure 1), where polarized cells are arranged in fingerlike villi that protrude into the intestinal lumen to maximize absorptive surface area. Each individual absorptive cell, or enterocyte, has a microvillous brush border at the apical (luminal) surface. Most dietary nonheme iron is in the ferric (Fe3+) form. It must be reduced to ferrous (Fe2+) iron, either chemically or through the action of a brush border ferrireductase such as duodenal cytochrome B (CYBRD1, also known as DCYTB), a cytochrome B561 homolog that may use ascorbic acid as a cofactor.53 CYBRD1 was one of 2 iron transport–related molecules discovered by McKie through a very productive RNA subtraction approach.53,54 Surprisingly, although Cybrd1 expression is markedly induced in iron-deficient animals, targeted disruption of the murine Cybrd1 gene was not associated with any apparent phenotype in mice fed standard chow.55 Members of the STEAP ferrireductase family are also expressed in the intestine.56 While they are good candidates for enzymatic ferrireductases at the brush border, the roles of CYBRD1 and STEAPs in intestinal iron absorption remain uncertain.
Fe2+ iron enters absorptive enterocytes through DMT1, the same iron transporter used for endosomal transfer in the transferrin cycle. The intestinal form of DMT1 is produced from a different mRNA splice isoform, resulting in an alternate C-terminus of the protein.57,58 Intestinal DMT1 is primarily localized to the apical membrane and to subapical endosomes.59 Protons necessary for metal cotransport are provided by gastric acid flowing into the proximal portion of the duodenum where DMT1 is most highly expressed and likely most active. The requirement for proton cotransport explains why treatment with antacids or H2 histamine blockers interferes with iron absorption. DMT1 expression is dramatically induced in iron deficiency,13 and possibly regulated at a posttranscriptional level by a 3′ IRE present in the splice isoform expressed in intestine.57 DMT1 may also serve as a physiologically significant portal of entry for other divalent metal cations including Mn2+, Co2+, Zn2+, Cu2+, and Pb2+, though its importance has only been definitively established for Fe2+ in vivo.13
The sole mammalian homolog of DMT1, designated NRAMP1 for natural resistance associated macrophage protein 1, was identified by Vidal et al through positional cloning of a mouse locus involved in host defense against intracellular pathogens in mouse macrophages.60 NRAMP1 is expressed in phagosomes of professional phagocytes.61 After DMT1 was shown to serve as a transmembrane metal transporter, functional studies indicated that NRAMP1 had similar activity.62 It has bacteriostatic but not bacteriocidal activity, presumably because it acts to deplete metals from the phagosomes in which microorganisms replicate, thus depriving them of iron and/or manganese. Homologous proteins in yeast,63 flies,64 and zebrafish65 also transport iron and similar divalent cations.
Targeted disruption of the murine gene encoding DMT1 confirmed that DMT1 is the primary transmembrane iron transporter bringing dietary nonheme iron into intestinal epithelial cells and mediating iron uptake through the transferrin cycle in erythroid precursors.66 Surprisingly, however, most other cell types do not appear to require DMT1 for iron uptake. This suggests that other transmembrane iron importers exist. Studies of non–transferrin bound iron uptake by cultured cells support this conclusion.67-72 However, aside from L-type calcium channels, which have some iron carrying capability,73 no compelling candidates have been identified that transport iron atoms directly into cells. There is a siderophore-like iron uptake pathway mediated by lipocalin-2 (also called NGAL, 24p3) but its physiologic role is not fully worked out.74-76
Once inside the intestinal epithelial cell, iron has at least 2 possible fates. A portion remains in the cell for use or storage. This iron is never absorbed into the body; rather, it is lost when enterocytes senesce and are sloughed into the gut lumen. Only iron exported across the basolateral membrane of the enterocyte is absorbed. The basolateral iron transporter, discovered simultaneously by 3 labs, is ferroportin (also called IREG1, MTP1, SLC39A1, and now SLC40A1).54,77,78 Ferroportin is resident on the basolateral membrane, and also found in macrophages involved in recycling iron from the hemoglobin of effete erythrocytes (Figure 1). Targeted disruption of the murine ferroportin gene demonstrated its importance in both sites.79
Although functional studies are incomplete, ferroportin likely transports ferrous ion. Transport is facilitated by multicopper ferroxidases including the abundant serum protein ceruloplasmin and its membrane-bound intestinal homolog hephaestin.80-83 Until recently, the ferroxidases were thought to be important simply for oxidizing Fe2+ to load it onto transferrin. However, De Domenico and colleagues have recently shown that ceruloplasmin is required to maintain cell-surface localization of ferroportin.84 This situation is somewhat analogous to iron transport in yeast, where the ferrous iron permease FTR1 (functionally analogous but structurally unrelated to DMT1) requires the multicopper ferroxidase FET3 for correct localization on the cell surface.85,86
Intestinal absorption of nonheme iron is now understood in some detail, but the absorption of heme iron, primarily derived from meats, remains poorly understood. A description of a putative heme importer in 200587 later proved to be incorrect.88 While heme exporter proteins have been described,20,89 it seems likely that most iron dietary heme iron is liberated from protoporphyrin by heme oxygenase to enter a common pathway with dietary nonheme iron before it leaves the absorptive epithelium.
Regulation of iron homeostasis by hepcidin
Although its handling is frequently termed iron “metabolism,” iron itself is not metabolized in a classical sense. Accordingly, human iron disorders are invariably disorders of iron balance or iron distribution. Iron deficiency anemia, hemochromatosis, and the anemia of chronic disease (also known as the anemia of inflammation) are all common examples of this principle, as will be discussed later. Hence, understanding iron homeostasis is critical for understanding these disorders. Conversely, understanding genetic iron disorders (Table 1) has provided important insights into iron homeostasis.
Genes involved in inherited human iron disorders
| Protein (gene symbol) [aliases] . | Human chromosome (map position) . | Protein function . | Disease (caused by loss-of-function mutations unless otherwise noted) . |
|---|---|---|---|
| Ceruloplasmin (CP) | 3 (150 Mb) | Plasma ferroxidase | Aceruloplasminemia184 |
| DMT1 (SLC11A2) [NRAMP2, DCT1] | 12 (50 Mb) | Transmembrane iron transporter (importer) | Anemia with hepatic iron overload172 |
| Ferritin H chain (FTH1) | 11 (61 Mb) | Subunit of iron storage protein; has ferroxidase activity | Iron overload (mutation disrupting iron regulatory element)49 |
| Ferritin L chain (FTL) | 19 (54 Mb) | Subunit of iron storage protein | Hyperferritinemia-cataract syndrome (mutation disrupting iron regulatory element)48 |
| Ferroportin (SLC40A1) [IREG1, MTP1] | 2 (190 Mb) | Transmembrane iron transporter (exporter) | Macrophage-predominant iron overload (loss-of-function mutations that cause protein mis-localization)156 |
| Hemochromatosis (gain-of-function mutations that cause insensitivity to hepcidin)158,159 | |||
| Frataxin (FXN) | 9 (71 Mb) | Mitochondrial iron chaperone | Friedreich ataxia212 |
| Glutaredoxin 5 (GLRX5) [GRX5] | 14 (95 Mb) | Participates in Fe-S cluster biogenesis | Anemia with iron overload and sideroblasts171 |
| Hemojuvelin (HFE2) [RGMC] | 1 (144 Mb) | Bone morphogenetic protein coreceptor | Juvenile hemochromatosis138 |
| Hepcidin (HAMP) [LEAP1] | 19 (40 Mb) | Iron regulatory hormone, binds ferroportin to cause its inactivation and degradation | Juvenile hemochromatosis161 |
| HFE (HFE) [HLA-H] | 6 (26 Mb) | Regulates hepcidin expression, mechanism uncertain; interacts with TFR1 and TFR2; may participate in a signaling complex with TFR2 | Classic HLA-linked hemochromatosis121 |
| Mitoferrin (SLC25A37) | 8 (23 Mb) | Mitochondrial iron import | Erythropoietic protoporphyria17 |
| Transferrin (TF) | 3 (135 Mb) | Plasma iron binding protein, ligand for TFR1 and TFR2 | Atransferrinemia (hypotransferrinemia)178 |
| Transferrin receptor-2 (TFR2) | 7 (100 Mb) | Sensor for diferric transferrin; regulates hepcidin expression; may participate in a signaling complex with HFE | Hemochromatosis213 |
| Protein (gene symbol) [aliases] . | Human chromosome (map position) . | Protein function . | Disease (caused by loss-of-function mutations unless otherwise noted) . |
|---|---|---|---|
| Ceruloplasmin (CP) | 3 (150 Mb) | Plasma ferroxidase | Aceruloplasminemia184 |
| DMT1 (SLC11A2) [NRAMP2, DCT1] | 12 (50 Mb) | Transmembrane iron transporter (importer) | Anemia with hepatic iron overload172 |
| Ferritin H chain (FTH1) | 11 (61 Mb) | Subunit of iron storage protein; has ferroxidase activity | Iron overload (mutation disrupting iron regulatory element)49 |
| Ferritin L chain (FTL) | 19 (54 Mb) | Subunit of iron storage protein | Hyperferritinemia-cataract syndrome (mutation disrupting iron regulatory element)48 |
| Ferroportin (SLC40A1) [IREG1, MTP1] | 2 (190 Mb) | Transmembrane iron transporter (exporter) | Macrophage-predominant iron overload (loss-of-function mutations that cause protein mis-localization)156 |
| Hemochromatosis (gain-of-function mutations that cause insensitivity to hepcidin)158,159 | |||
| Frataxin (FXN) | 9 (71 Mb) | Mitochondrial iron chaperone | Friedreich ataxia212 |
| Glutaredoxin 5 (GLRX5) [GRX5] | 14 (95 Mb) | Participates in Fe-S cluster biogenesis | Anemia with iron overload and sideroblasts171 |
| Hemojuvelin (HFE2) [RGMC] | 1 (144 Mb) | Bone morphogenetic protein coreceptor | Juvenile hemochromatosis138 |
| Hepcidin (HAMP) [LEAP1] | 19 (40 Mb) | Iron regulatory hormone, binds ferroportin to cause its inactivation and degradation | Juvenile hemochromatosis161 |
| HFE (HFE) [HLA-H] | 6 (26 Mb) | Regulates hepcidin expression, mechanism uncertain; interacts with TFR1 and TFR2; may participate in a signaling complex with TFR2 | Classic HLA-linked hemochromatosis121 |
| Mitoferrin (SLC25A37) | 8 (23 Mb) | Mitochondrial iron import | Erythropoietic protoporphyria17 |
| Transferrin (TF) | 3 (135 Mb) | Plasma iron binding protein, ligand for TFR1 and TFR2 | Atransferrinemia (hypotransferrinemia)178 |
| Transferrin receptor-2 (TFR2) | 7 (100 Mb) | Sensor for diferric transferrin; regulates hepcidin expression; may participate in a signaling complex with HFE | Hemochromatosis213 |
Systemic iron homeostasis involves meticulous control of intestinal iron absorption, effective utilization of iron for erythropoiesis, efficient recycling of iron from effete erythrocytes, and controlled storage of iron by hepatocytes and macrophages (Figure 1). Erythroid iron utilization is primarily determined by the efficiency of transferrin cycle assimilation of serum iron. In contrast, intestinal absorption, iron recycling, and iron storage are controlled systemically and coordinately. In this context, we now know that hepcidin, a peptide hormone produced in the liver, has primary responsibility for modulating iron availability to meet iron needs.
Discovered independently by 3 laboratories and first reported in 2000 and 2001, hepcidin is a 25-amino-acid protein produced by processing of a larger precursor.90-92 Although it bears resemblance to defensin peptides involved in innate immunity, its primary function appears to be regulation of iron homeostasis through a mechanism that was elegantly elucidated by Kaplan, Nemeth, Ganz, De Domenico, and their coworkers. Hepcidin binds to cell-surface ferroportin, triggering its tyrosine phosphorylation, internalization, and ubiquitin-mediated degradation in lysosomes.93,94 By removing ferroportin from the plasma membrane, hepcidin shuts off cellular iron export. This is particularly important in the intestine, where inactivation of basolateral ferroportin leads to retention of iron in the intestinal epithelium, and in iron-recycling macrophages of the reticuloendothelial system, where inactivation of ferroportin interrupts release of iron recovered from senescent red cells (Figure 2A). Both events have the same consequence—decreased serum iron. Interestingly, the importance of controlling basolateral transfer to effect regulation of intestinal iron absorption was initially postulated by Crosby and Conrad more than 40 years before the mechanism was elucidated.95
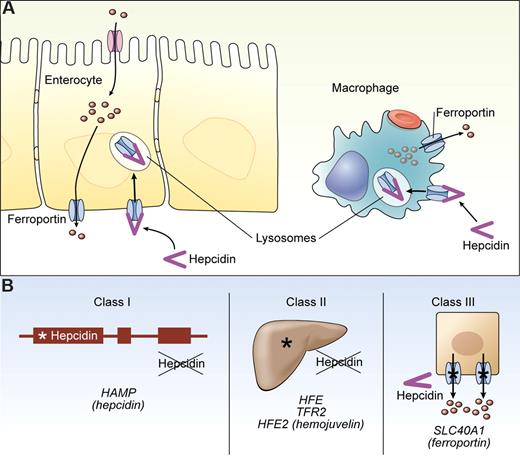
Hepcidin and hemochromatosis. (A) The activity of hepcidin is depicted, showing ferroportin as a target both on enterocytes and macrophages. Hepcidin binds to ferroportin triggering its internalization and lysosomal degradation. (B) Three classes of hemochromatosis disorders all affect the hepcidin/ferroportin regulatory axis: Class I, defects in the hepcidin gene (HAMP) preventing production of functional hepcidin; Class II, defects in HFE, TFR2, or HFE2 genes preventing normal hepatic regulation of hepcidin expression; Class III, defects in ferroportin preventing normal regulation by hepcidin. Illustration by Kenneth Probst.
Hepcidin and hemochromatosis. (A) The activity of hepcidin is depicted, showing ferroportin as a target both on enterocytes and macrophages. Hepcidin binds to ferroportin triggering its internalization and lysosomal degradation. (B) Three classes of hemochromatosis disorders all affect the hepcidin/ferroportin regulatory axis: Class I, defects in the hepcidin gene (HAMP) preventing production of functional hepcidin; Class II, defects in HFE, TFR2, or HFE2 genes preventing normal hepatic regulation of hepcidin expression; Class III, defects in ferroportin preventing normal regulation by hepcidin. Illustration by Kenneth Probst.
Hepcidin is primarily made in hepatocytes, and secreted into the circulation. The liver acts as a clearinghouse for a variety of signals affecting iron homeostasis. Because of its small size, hepcidin is probably filtered by the kidneys on the first pass. It has been detected and quantitated in urine samples,91,96 and, with more difficulty, in serum.97 Its rapid excretion implies that most regulation of serum hepcidin levels occurs at the level of production. Proteolytic processing of the prohormone is carried out by furin in a relatively unregulated manner.98 In contrast, hepcidin transcription is tightly regulated over a very wide dynamic range.
Initially, murine hepcidin mRNA was shown to be elevated in response to iron overload92 and decreased in response to iron deficiency.99,100 The functional effects of altered hepcidin expression in vivo were apparent when Nicolas, Lesbordes-Brion, and colleagues showed that inactivation of the hepcidin gene in mice was associated with severe iron overload.101,102 Conversely, transgenic overexpression of hepcidin resulted in iron deficiency.103,104 In addition, the amount of hepcidin mRNA in liver cells is decreased in response to hypoxia and ineffective erythropoiesis (overlapping with the response to iron deficiency)99,105 and induced in response to treatment with lipopolysaccharide or by inflammation of other etiologies.92,99 These responses all make sense: when erythropoiesis needs to accelerate, interruption of hepcidin expression results in increased iron availability. In contrast, induction of hepcidin in inflammation and consequent iron sequestration augments innate immune defenses against invading pathogens.106
Current information about the hepcidin promoter indicates that it is relatively compact, as it must be to avoid encroaching on a closely neighboring gene encoding USF2. The most proximal region is highly conserved across mammalian species.107 A consensus STAT3 binding site has been shown to mediate the induction of hepcidin in inflammation, through a signaling pathway triggered by interleukin-6.107,108 The von Hippel-Lindau/hypoxia-inducible transcription factor (HIF) system also appears to control hepcidin expression, with HIF1α acting as a repressor when it binds to the hepcidin promoter.109 Potential binding sites for C/EBPα, USF2, HNF4α, p53 and other widely expressed transcription factors have also been identified in the hepcidin promoter, but it is not yet clear what roles, if any, they have in regulation of hepcidin expression in vivo.110-112
Signaling through the bone morphogenetic protein (BMP)/SMAD pathway is the most powerful mechanism known to activate hepcidin transcription. This surprising connection between BMPs and hepcidin was initially discovered through 2 independent avenues of research. In the course of their general studies of cellular signaling, Wang and colleagues inactivated the gene encoding an essential SMAD protein, SMAD4, exclusively in hepatocytes.113 To their surprise, the dominant phenotype that resulted was severe hemochromatosis, similar to that seen in mice lacking hepcidin. In parallel, Babitt and colleagues studied hemojuvelin, a protein mutated in patients with severe, early onset “juvenile hemochromatosis.”114 They showed that hemojuvelin acts as a BMP coreceptor to stimulate hepcidin transcription. Both groups demonstrated that treatment of hepatic cells with BMPs stimulated hepcidin expression, in a manner dependent on the presence of SMAD4,113 BMPs, and hemojuvelin.114
It seems likely that activated SMADs bind directly to the hepcidin promoter in response to BMP signaling. However, in contrast to some other transcription factors, consensus sites for SMAD binding are highly variable and difficult to predict by sequence analysis alone. Truksa et al have localized putative BMP-responsive elements in the hepcidin promoter,115 but it is still uncertain exactly how BMP transcriptional regulation occurs. Nonetheless, BMP treatment is a potent stimulus for hepcidin expression both in cultured cells113,114,116,117 and in animals.117
Hemochromatosis
Our understanding of hepcidin regulation has been greatly enhanced through efforts to understand hemochromatosis, a genetic iron overload disorder. Described as “bronze diabetes” by Trousseau in 1865,118 hemochromatosis was not known to be an iron disorder until well into the 20th century.119 It was one of the first genetic diseases to be linked to a discrete chromosomal position, through the groundbreaking work of Simon, an astute French physician-scientist who found that hemochromatosis patients were disproportionately likely to have particular HLA haplotypes.120 Two decades later that insight led to the identification of HFE (originally called HLA-H), the gene mutated in the large majority of patients with hemochromatosis.121 The positional cloning of HFE by a now-defunct biotechnology company was a tour de force, and one of the landmark accomplishments of the middle years of the human genome project.
As is often the case, however, the situation is more complex than originally appreciated. We now know that HFE is one of several genes that can be mutated in hemochromatosis. Furthermore, penetrance of HFE hemochromatosis is incomplete, and only a fraction of affected patients have clinical disease, presumably due to both genetic and environmental modifiers.122 Several modifier gene candidates have been explored and, in some cases, verified.123-135 Not surprisingly, heterozygous mutations in other hemochromatosis-associated genes can exacerbate the clinical course for patients who are also homozygous for HFE mutations.
Like hemojuvelin, both HFE and transferrin receptor-2 (TFR2, another hemochromatosis-associated protein) are inferred to be involved in regulation of hepcidin expression. Human patients with mutations in the genes encoding hemojuvelin, HFE, or TFR2 have inappropriately low urinary hepcidin levels for their overall body iron status.136-139 As a consequence, intestinal iron absorption and macrophage iron release are not properly controlled, leading to iron overload, increased serum iron, and iron deposition in the liver, heart, and endocrine tissues. Similarly, mouse models of hemochromatosis developed through targeted disruption of any of these 3 genes have diminished hepcidin mRNA in their livers.140-144 While this is strong evidence that all 3 proteins are involved in hepcidin regulation, the roles of HFE and TFR2 are not as well understood as that of hemojuvelin.
HFE is an atypical major histocompatibility class I–like molecule that forms a heterodimer with β2-microglobulin but is incapable of binding a small peptide.145 Soon after its discovery, HFE was shown to interact with TFR1 to form a protein-protein complex.145-147 Initially, its role in iron homeostasis was thought to involve perturbation of the transferrin cycle, either in hepatocytes or in intestinal epithelial cells (reviewed in Roy and Enns148 ). However, more recent results suggest a different scenario: that TFR1 regulates HFE activity and inhibits HFE by sequestering it.149 Because TF and HFE compete for binding to TFR1, displacement of HFE from TFR1 by TF may be a means to activate HFE to signal through an as-yet-unknown mechanism to increase hepcidin transcription.
TFR2 probably fits into this scenario in some intimate way. Mutations in TFR2 are much less common than mutations in HFE, but the clinical disease can be indistinguishable.133 Like TFR1, TFR2 interacts with HFE to form a stable protein complex.150 However, as shown by Chen and Enns, HFE does not bind to homologous portions of TFR1 and TFR2.151 Although TFR2 is 43% homologous to TFR1 in its extracellular domain, it does not take up diferric-TF efficiently.152 Rather, its primary function seems to be to interpret body iron status. Amounts of TFR2 protein increase in response to iron-saturated transferrin.151,153-155 Taking this into account, we have proposed a model in which TFR2 escorts HFE away from TFR1 when the serum iron level (reflected in the transferrin saturation) is elevated.149,150 The implication of this model is that HFE and TFR2 collaborate in a signaling complex that acts to augment hepcidin expression. These proteins may be part of a larger BMP signaling complex along with hemojuvelin (P.J. Schmidt, F.W. Huang, and N.C.A., unpublished results).
Hemochromatosis can also result from mutations in the gene encoding ferroportin, the target of hepcidin activity. The first mutations in ferroportin were discovered simultaneously by Montosi et al156 and Njajou et al157 in families with iron overload segregating in an autosomal dominant pattern. Many other mutations have been reported subsequently. Initially there was disagreement about the clinical presentation: some patients seemed to have macrophage-predominant iron loading and occasional anemia, while others had clinical features indistinguishable from HFE hemochromatosis. Strikingly, all ferroportin mutations caused missense changes, rather than truncations or frameshifts. Furthermore, knockout mice heterozygous for a null ferroportin allele had no significant iron phenotype, and did not seem to model the human disease.79
These issues were resolved by the discovery that there are 2 broad categories of ferroportin mutations.158,159 Missense mutations that affected the subcellular localization or transporter function of ferroportin (“loss-of-function”) were associated with macrophage iron loading but few, if any, sequelae resembling classical hemochromatosis. In contrast, missense mutations that rendered ferroportin insensitive to regulation by hepcidin (“gain-of-function”) caused hemochromatosis. The fact that both types of mutations have autosomal dominant patterns of clinical expression can be reconciled by the conclusion that ferroportin polypeptides assemble into homo-multimers.158 Recently, a mouse model of the disease associated with loss-of-function ferroportin mutations, flatiron, was identified through a positional cloning effort.160
There are not many precedents for inactivating and activating mutations in one gene causing 2 different diseases. Accordingly, there is no consensus yet on nomenclature for these disorders. It has been suggested that the condition associated with loss-of-function mutations should be called “ferroportin disease” and the condition associated with gain-of-function mutations should be called type IV hemochromatosis. The classification scheme is blurred, however, by the fact that some mutations appear to have features of both types.
Thus, based on our current understanding, the molecular pathogenesis of hemochromatosis can be divided into 3 classes (Figure 2B). First, mutations in the hepcidin gene itself (called HAMP) cause hemochromatosis by preventing the production of functional hepcidin protein.161 Second, mutations in the genes encoding HFE (HFE), TFR2 (TFR2), and hemojuvelin (HFE2) inactivate signaling pathways that normally up-regulate hepcidin expression. Finally, mutations in the gene encoding ferroportin (SLC40A1) can cause hemochromatosis by rendering the transporter insensitive to hepcidin regulation.158,162
Iron deficiency anemia
Iron deficiency anemia continues to be a major public health problem worldwide, with an estimated 3 billion people affected. Arguably, the first thorough descriptions of iron deficiency and its treatment involved chlorosis, a perplexing condition due at least in large part to iron deficiency anemia that was diagnosed between the Middle Ages and the end of the Victorian era in the 1920s. It is remarkable to think that some of the founders of ASH may have seen patients with this disorder. Sydenham, in 1681, recognized that chlorosis could be cured by “the effects of steel.”163 Ferrous sulfate pills, still a mainstay for treatment of iron deficiency, have been in use for nearly 2 centuries.164 The efficacy of iron treatment was formally established in a classic experiment carried out by Castle. He proved that the active substance was iron when he administered parenteral iron and showed a proportionate rise in hemoglobin in patients with hypochromic anemia.165
The vast majority of cases of iron deficiency are acquired, resulting from blood loss (eg, from intestinal parasitosis), from insufficient dietary iron intake, or both. Young children and menstruating women are disproportionately affected because their iron status is marginal to begin with. Recently it was rediscovered that infection with H pylori, even in the absence of significant bleeding, can lead to profound iron deficiency anemia that is poorly responsive to oral iron therapy. This disorder is typically seen in young women, is associated with gastric atrophy, and can be associated with other autoimmune phenomena.166,167 As pointed out by Hershko and colleagues,168 this constellation of findings was reported a century ago by Faber169 and further described by Wintrobe and Beebe.170 Eradication of H pylori infection can lead to correction of the anemia.167
It is now recognized that rare genetic defects can also cause iron deficiency anemia. Mutations in the genes encoding DMT1 (SLC11A2) and glutaredoxin 5 (GLRX5) are associated with autosomal recessive hypochromic, microcytic anemia.171,172 Interestingly, the clinical phenotype of patients with DMT1 mutations differs slightly from the corresponding mouse model, mk.12 The human patients have similar blood films and erythrocyte abnormalities, but also have hepatic iron overload that is not fully explained by their transfusion histories.172-176 Perhaps less surprising, the clinical phenotype of a unique patient carrying a GLRX5 mutation also differs somewhat from an earlier animal model with a deletion of that gene, the shiraz zebrafish.177
Two forms of genetic iron deficiency anemia are associated with iron overload outside of the erythron. Deficiency of serum transferrin, due to mutations in the TF gene itself,178,179 interrupts iron delivery to erythroid precursors, triggering a massive but futile increase in intestinal iron absorption and consequent tissue iron deposition. This disorder, hypotransferrinemia (also called atransferrinemia), has been observed in both human patients and in mice.180-183 Through a different mechanism, deficiency of another major plasma protein, cerulopasmin, also causes mild iron deficiency anemia associated with iron accumulation in the liver and brain.184 As reported by Harris and colleagues,184 iron deficiency results from lack of ferroxidase activity needed to mobilize iron from storage. Although both of these disorders are rare, each can be confused with hemochromatosis if the entire clinical picture is not taken into account.
We and others have observed that some patients have congenital, iron-refractory, iron-deficiency anemia (IRIDA) that cannot be explained by mutations in the genes encoding DMT1, GLRX5, TF, or ceruloplasmin.185-190 These individuals appear to have a defect in cellular iron export,191 but the disorder has an autosomal recessive pattern of inheritance and no mutations have been detected in ferroportin or in the regulatory regions of the hepcidin gene.190 An important clue to the etiology of IRIDA came recently when Ernest Beutler and his son Bruce identified Tmprss6, encoding matriptase-2, as the gene mutated in a novel mouse mutant, Mask.192
In addition to a bizarre hair pattern that led to the strain name, Mask mice have severe iron deficiency anemia attributable to elevated hepcidin expression. Matriptase-2 is a type II transmembrane serine protease of unknown function, which is expressed at high levels in the liver. The mechanism through which matriptase-2 regulates hepcidin expression has not yet been determined. We asked whether mutations in the human ortholog, TMPRSS6, might cause IRIDA. We had been collecting DNA samples from IRIDA patients since I first saw a young boy with this disorder in 1996. Every patient who fit our strict criteria for IRIDA carried inactivating mutations in TMPRSS6 that could explain the disease.190,192 Further studies will be needed to determine the prevalence of this rare disorder, and to evaluate the possibility that less severe mutations increase susceptibility to common, acquired iron deficiency anemia.
Anemia of chronic disease
The anemia of chronic disease (also called anemia of inflammation) is an acquired disorder of iron homeostasis (reviewed in Roy and Andrews193 ). A common explanation for anemia in chronically ill patients, anemia of chronic disease was largely a diagnosis of exclusion in the past. Elegantly described by Cartwright in a classic review,194 this condition may be associated with infection, malignancy, organ failure, trauma, or other causes of inflammation. The anemia is typically mild to moderate, and erythrocytes may not show any stigmata of iron deficiency. But the underlying iron etiology is evident: macrophages that normally recycle iron are found to sequester it, intestinal iron absorption is interrupted, and erythroid precursors respond very rapidly when iron-transferrin is made available. An association with proinflammatory cytokines has been suspected for some time,195 but was not well understood until recently.
Studying an unusual group of patients, we developed an hypothesis to explain the anemia of chronic disease, which has subsequently been validated by others.196 Treated survivors of glycogen storage disease type 1a frequently develop benign hepatic adenomas in early adulthood. With Weinstein, Roy, and colleagues, we observed that these patients also develop anemia resembling the anemia of chronic disease, the severity of which correlates directly with the extent of tumor burden.100 We found that the hepatocyte-like cells of the adenomas expressed very high levels of hepcidin100 and speculated that our results could be generalized—that induction of hepcidin expression in response to inflammation might explain the anemia of chronic disease. Subsequent studies by Nemeth and colleagues96,197 strongly supported our hypothesis, and it is now widely accepted.
In a sense, anemia of chronic disease is the phenotypic opposite of hemochromatosis. Expression of hepcidin that is inappropriately high for body iron status results in interruption of intestinal iron absorption and iron recycling. Consequently, decreased serum iron is available for erythropoiesis. Accordingly, Roy and colleagues have developed a transgenic mouse model expressing hepcidin, which shows that most consistent features of the anemia of chronic disease can be attributed to increased hepcidin expression.104 Our recent discovery that IRIDA is also caused by inappropriately high hepcidin expression suggests that IRIDA and the anemia of chronic disease should have common clinical features. While this is true in some regards, one striking difference is that IRIDA is associated with severe microcytosis, whereas the anemia of chronic disease is typically normocytic. Mice expressing a hepcidin transgene are microcytic, similar to IRIDA.104 I speculate that the normocytic erythrocytes in the anemia of chronic disease result from the combination of iron insufficiency and an as-yet-unexplained tendency to macrocytosis. For example, it is plausible that folate homeostasis is also perturbed in response to inflammation.
Conclusions and future directions
Iron biology is a vast field and, necessarily, there are important areas that I have neglected in this review. These include mitochondrial iron metabolism, heme metabolism, brain iron accumulation in neurodegenerative disorders, Fe•S cluster formation, therapeutic chelation, classical ferrokinetics, microbial iron metabolism, and others. Focusing on physiology more than biochemistry, I have not given due attention to recent structural characterizations of TFR1, HFE, or IRP1 alone and in interactions with the molecules they bind to.145,198-200 My choice of topics should not be viewed as a judgment of what is most important; rather, it simply reflects my areas of expertise and a focus on diseases that have only recently become understood. Looking ahead, it is fun to speculate on what we will learn in the next round of discoveries in iron biology. In my opinion, any wish list has to focus on the iron disorders that affect our patients—in the final analysis, they are why most of us have chosen to work in this area.
First, I think there will be a new surge of interest in iron deficiency. We are in an unprecedented position to understand the genome/environment interactions that make some people particularly susceptible to iron deficiency. Among these interactions, we should soon understand why infection with H pylori causes profound iron deficiency that cannot be explained by blood loss or failed iron absorption. We will understand the “erythroid regulator” that communicates body iron needs to liver hepatocytes producing hepcidin, allowing for mobilization of all available iron when erythropoiesis accelerates. New understanding of iron biology may have therapeutic benefits as well. Perhaps it will lead to novel methods for oral iron repletion, allowing it to be accomplished in days, rather than months. If this becomes possible, it will have enormous implications around the globe. Finally, pica, an enigmatic but almost pathognomonic symptom of severe iron deficiency, may provide clues to help us understand the intricate links between nutrition and behavior.
Second, we still have more to learn about primary iron overload disorders. Mutations in the 5 genes currently associated with hemochromatosis probably do not account for all patients with the disease. There is likely to be at least one additional gene yet to be identified. Even when the list is complete, we will need a better understanding of genetic modifiers to fully understand why clinical presentations vary dramatically. Knowledge of the full genetic landscape of hemochromatosis may lead to new approaches to replace blood-letting (phlebotomy), a treatment that was introduced almost a decade before ASH was founded. Because phlebotomy is cheap, easy, safe, and effective, it will be difficult to supplant. But considering how responsive hepcidin expression is to a variety of stimuli, it is quite possible that a safe and effective drug currently used for a different purpose might turn out to have unexpected hepcidin-inducing activity, solving the problem. Finally, although we have made great strides in understanding hemochromatosis in individuals of European descent, we remain largely ignorant of the causes and manifestations of iron overload in individuals of African descent, in spite of the apparent prevalence of the condition in that population.201-210
Transfusional iron overload is relatively well understood. In my opinion, the goal in coming years should be to use biology, rather than chemistry, to treat it. By that I mean that detailed knowledge of iron homeostasis will suggest new therapeutic opportunities to deliberately remove iron from the body, even though there is no natural excretion pathway through the liver or kidneys. Deliberate manipulation of iron loss through the gut epithelium or through the kidneys are 2 possible approaches.
Our understanding of the anemia of chronic disease has progressed enormously over the past few years. As we refine our understanding of hepcidin-related manifestations and other manifestations, it should become possible to stratify this disorder according to causes and effects. Undoubtedly there will be new treatment strategies based on our understanding of the biology of the anemia of chronic disease. It is quite likely that this understanding will also lead to a better appreciation of the molecular pathology of the anemia of aging.
A better understanding of iron homeostasis may also enhance treatments for other disorders. We still have much to learn about iron homeostasis in solid tumors, and about possible roles for lipocalin-2 and its receptor76 in malignant transformation. Iron deposition is a hallmark of many neurodegenerative disorders,211 and manipulating iron distribution in the central nervous system may become an important therapeutic approach. Similarly, iron-depleting strategies may someday be used to alter innate immunity and to enhance host defense against invading pathogens. I would venture that a better understanding of iron biology will reap benefits for virtually every field of medicine, keeping our students and fellows busy for decades to come.
Acknowledgments
I would like to thank colleagues in the field of iron biology who generously welcomed me into their world 12 years ago, and in particular Mark Fleming, a long-term collaborator who gave me a strong push to get into it. I feel quite privileged to work in a field that has benefited so much from the diversity of its investigators: iron biology is a truly international pursuit that has developed from the efforts of scientists in Europe, Australia, Asia, Africa, and the Americas; fruitful approaches have ranged from traditional biochemistry to modern mouse genetics to clinical measurements and everything in between. Like me, many others have stumbled into iron biology, often proclaiming that they will just do a bit of work and then return to their home field, but almost always deciding to stay. Their fresh perspectives have made the field even more exciting, and more welcoming to young scientists. Finally, I have had far more than my share of luck in working with outstanding students, postdoctoral fellows, and technicians in my own laboratory. I owe them a great deal for having made this journey so rewarding and so much fun.
The work in my laboratory is currently supported by National Institutes of Health R01 grants HL051057, DK066373, and DK053813, as well as a grant from the Roche Foundation for Anemia Research.
National Institutes of Health
Authorship
Contribution: N.C.A. wrote the paper.
Conflict-of-interest disclosure: The author declares no competing financial interests.
Correspondence: Nancy C. Andrews, Duke University School of Medicine, DUMC 2927, Durham, NC 27710; e-mail: nancy.andrews@duke.edu.