Abstract
Objective: Neuroblastoma (NB) is the most common extra cranial solid tumor in childhood. It accounts for approximately 7% of pediatric cancer diagnoses each year in the United States yet is responsible for 15% of pediatric cancer deaths annually. Occurring overwhelmingly in patients with high-risk (HR) disease.
Measurable immune surveillance correlates with improved overall disease-free survival in patients with a myriad of cancer subtypes, including NB. Current therapeutic strategies in HR-NB incorporate manipulation of the host immune response, including autologous stem cell transplantation (autoSCT), cis-retinoic acid, and chimeric antibody targeting the tumor-associated antigen disialoganglioside (GD2). Understanding how such therapies affect the immune system and its relation to clinical response is of critical importance. We speculate that patients with higher proportions of regulatory T cells (Tregs) and slower recovery of other lymphocyte subsets will have higher rates of progressive disease and/or relapse.
Methods: We reviewed the records of all University of Chicago patients between 2009 and 2015 who received autoSCT as part of upfront therapy for HR neuroblastoma. Data included complete blood count and peripheral blood lymphocyte flow cytometric (FACS) subset monitoring. Our analysis aimed to determine the association between lymphocyte subset kinetics following autoSCT with pre-transplant treatment, transplant conditioning, and disease-free/overall survival. Patients who had a follow-up of greater than one-year post-transplantation were included in the analysis.
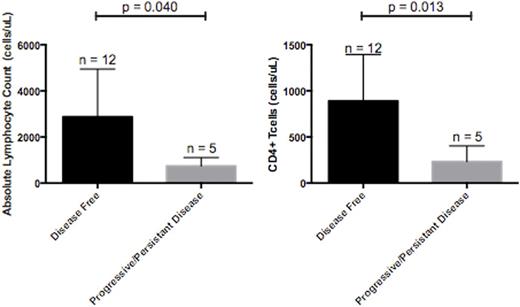
Results: Thirty-four patients (59% male, median age 5.6 years) received autoSCT between 2009 and 2015 for HR neuroblastoma. Seventy-six percent (n = 26) received either carboplatin, etoposide, melphalan (CEM) or busulfan/melphalan (BuMel) for conditioning. Among those patients, twenty-seven percent received MIBG prior to their autoSCT. The other patients received BSO/melphalan or tandem transplantations. Sixty-eight percent of these patients went on to receive chimeric antibody after their autoSCT irrespective of their conditioning regimen. Antibody therapy with IL-2 or GM-CSF was initiated at a median of 101 days (mean 98.9) post-autoSCT. All patients had normal neutrophil counts at 100 days post transplant, while the total absolute lymphocyte count (ALC), CD8+ T cells, NK cells and CD19+ B cells, were below normal levels in the majority of patients, (100%, 89%, 79% and 94% of patients respectively). Patients who received MIBG prior to autoSCT had a higher proportion of CD3+CD4+CD25+ T cells, the subset containing Tregs, among their total CD3+ population at 100 days post-transplant, (79.8% versus 32.8% p-value = 0.02). Following single autoSCT, patients with higher ALC and CD4+ cells had increased disease free survival in evaluations after six months post transplant. (Figure 1) CD8+ cells, NK cells and CD19+ cell counts were not significant in this analysis.
Conclusions: Patients with HR NB have differential immune cell recovery following autoSCT that is dependent on the type of therapy received prior to autoSCT. Specifically, patients who received MIBG had markedly higher proportion of CD3+CD4+CD25+ T cell recovery compared to patients not receiving pre-autoSCT MIBG. This is the subset containing Tregs, which may indicate suppression of an anti-NB immune response long-term. Immune reconstitution is globally poor in all patients at the time of chimeric antibody immunotherapy that is initiated around day 100-post autoSCT. There are features of immune reconstitution that appear to correlate with improved outcomes, including elevated ALC, CD8+ and CD4+ cell counts when evaluated at least six months post transplantation. Additional characterization of T cell subsets is currently being performed to quantify the number of Treg cells in the CD3+CD4+CD25+ T cell subset population. Prospective evaluation of both immune cell recovery and functional evaluation of cells is required to confirm these findings, which may have a profound impact on how immune modulatory therapy is scheduled for those patients with high-risk neuroblastoma.
(Panel A) Patients with higher ALC (panel A) and CD4+ cells (panel B) checked at least 6 months after stem cell transplantation had increased disease-free survival (DFS) compared to those patients with diminished ALC and CD4+ cells recovery.
(Panel A) Patients with higher ALC (panel A) and CD4+ cells (panel B) checked at least 6 months after stem cell transplantation had increased disease-free survival (DFS) compared to those patients with diminished ALC and CD4+ cells recovery.
No relevant conflicts of interest to declare.
Author notes
Asterisk with author names denotes non-ASH members.