Abstract
Inhibition of Ca2+ mobilization by cyclic nucleotides is central to the mechanism whereby endothelial-derived prostacyclin and nitric oxide limit platelet activation in the intact circulation. However, we show that ∼ 50% of the Ca2+ response after stimulation of glycoprotein VI (GPVI) by collagen, or of Toll-like 2/1 receptors by Pam3Cys-Ser-(Lys)4 (Pam3CSK4), is resistant to prostacyclin. At low agonist concentrations, the prostacyclin-resistant Ca2+ response was predominantly because of P2X1 receptors activated by ATP release via a phospholipase-C–coupled secretory pathway requiring both protein kinase C and cytosolic Ca2+ elevation. At higher agonist concentrations, an additional pathway was observed because of intracellular Ca2+ release that also depended on activation of phospholipase C and, for TLR 2/1, PI3-kinase. Secondary activation of P2X1-dependent Ca2+ influx also persisted in the presence of nitric oxide, delivered from spermine NONOate, or increased ectonucleotidase levels (apyrase). Surprisingly, apyrase was more effective than prostacyclin and NO at limiting secondary P2X1 activation. Dilution of platelets reduced the average extracellular ATP level without affecting the percentage contribution of P2X1 receptors to collagen-evoked Ca2+ responses, indicating a highly efficient activation mechanism by local ATP. In conclusion, platelets possess inhibitor-resistant Ca2+ mobilization pathways, including P2X1 receptors, that may be particularly important during early thrombotic or immune-dependent platelet activation.
Introduction
Platelet activation is the initial required event during the physiologic process of hemostasis. With increasing age, the onset of atherosclerosis lowers the threshold for platelet reactivity and consequently the risk of thrombosis. In the intact circulation, there are inhibitors of platelet reactivity that serve to maintain blood fluidity. These inhibitors include endothelial-derived prostacyclin (PGI2) and nitric oxide (NO) that elevate intraplatelet cyclic AMP (cAMP) and cyclic GMP (cGMP), respectively.1 cAMP- and cGMP-dependent kinases target several platelet signaling pathways, particularly mobilization of the key second messenger Ca2+.1,2 Degradation of nucleotides by enzymes in the plasma and on the surface of endothelium and leukocytes represents a further important inhibitory influence. The dominant ectonucleotidase CD39 converts the platelet agonists ATP and ADP to inert AMP, and AMP is subsequently degraded by CD73 to adenosine and therefore further inhibits platelets through stimulation of Gs-coupled A2a and A2b receptors.3–5 After breach of vascular integrity, disruption of the endothelial layer leads to local loss of these inhibitory pathways that will facilitate platelet activation by adhesive macromolecules such as collagen and diffusible agonists such as ADP, thromboxane A2 (TxA2), and thrombin.6 In identifying potential strategies to manage thrombosis, it is therefore important to consider the relative effectiveness of natural platelet inhibitory influences on various platelet activation pathways.
Platelets possess multiple mechanisms whereby agonists can generate an increase in cytosolic Ca2+ concentration ([Ca2+]i).2 For agonists coupled to phospholipase C, a central pathway is inositol trisphosphate (IP3)–dependent Ca2+ release from the dense tubular system. This is followed by Ca2+ entry through Orai1 store-operated Ca2+ entry channels,2,7,8 and possibly also TRPC6 (transient receptor potential, canonical, type 6) channels activated by diacylglycerol, phosphatidylinositol bisphosphate depletion, or both.9–11 Cyclic nucleotides are highly effective inhibitors of platelet IP3-dependent Ca2+ release12–14 and thus also will indirectly prevent store-operated Ca2+ entry. Phospholipase C is reported to be another target of cyclic nucleotide-dependent kinases;15 therefore, PGI2 and NO will also reduce TRPC6 activation and secretion of secondary mediators. A further pathway for Ca2+ entry across the platelet plasma membrane is the P2X1 receptor, an ATP-gated nonselective cation channel.16 Under conditions designed to limit the desensitization of P2X1 receptors that readily occurs in vitro, secondary activation of this pathway is responsible for a large proportion of the Ca2+ responses to a range of agonists.17 However, such studies of P2X1 receptors have been conducted in the absence of endothelial-derived inhibitors encountered by platelets within the intact circulation. The aim of the present work was therefore to investigate how endogenous platelet inhibitors regulate Ca2+ responses to a range of stimuli under conditions where P2X1 receptors are protected from desensitization. In addition to collagen, thrombin, and TxA2, we assessed responses to stimulation of Toll-like receptors (TLRs) that play important roles in innate immune responses to invading pathogens.18 Platelets express multiple TLR receptors,19,20 with the TLR 2/1 complex representing the major functional subtype.21–24 These receptors may therefore contribute to the emerging roles of platelets in immune responses and thus also the development of atherosclerosis.25,26
Methods
Preparation of washed platelet suspensions
Blood was obtained by standard phlebotomy from informed, consenting donors in accordance with the Declaration of Helsinki into acid citrate dextrose anticoagulant (85mM trisodium citrate, 78mM citric acid, and 111mM glucose). The study was approved by the University of Cambridge Human Biology Research Ethics Committee and the University of Leicester Committee for Research Ethics concerning human subjects (non-NHS). The blood and acid citrate dextrose mixture (6:1 by volume) was centrifuged at 700g for 5 minutes. Platelet-rich plasma was removed and treated with aspirin (100μM, a concentration that maximally inhibits TxA2 production under the conditions of these experiments27 ) and apyrase type VII (0.32 U mL−1). Platelets were loaded with the Ca2+ indicator fura-2 by incubation of platelet-rich plasma with 2μM fura-2AM for 45 minutes at 37°C. Washed platelet suspensions were then prepared by centrifugation for 20 minutes at 350g and resuspension of the pellet in nominally Ca2+-free saline (145mM NaCl, 5mM KCl, 1mM MgCl2, 10mM HEPES, and 10mM glucose, titrated to pH 7.35 with NaOH) with type VII apyrase (0.32 U mL−1). Most experiments were conducted in a volume of saline equal to twice the original volume of plasma obtained from the donor, referred to in the dilution experiments as a relative platelet density of 50%. The typical platelet count in the 50% samples was in the range 1.4 to 1.9 × 109 mL−1 as assessed with a Z2 particle counter (Beckman Coulter).
Intracellular Ca2+ measurements
Ratiometric fluorescence measurements were conducted at 37°C in a spectrofluorometer system (Cairn Research) as described in detail previously.28 Fura-2 fluorescence signals at 340 and 380 nm excitation (> 490 nm emission) were calibrated using a dissociation constant of 224nM. Extracellularly derived calibration constants were obtained after permeabilization with digitonin (50nM) and after correction for background levels obtained with 10mM Mn2+. CaCl2 (2mM) or an additional 2mM MgCl2 was added to the cuvette 30 seconds before the agonist for studies in the presence and absence of external Ca2+, respectively. To buffer intracellular Ca2+ responses with cytosolic BAPTA, 15μM BAPTA-AM was included for the last 30 minutes of the fura-2 loading procedure. This BAPTA loading procedure abrogated even the most rapid Ca2+ responses in this preparation, namely, maximal P2X1-dependent Ca2+ increases stimulated by 10μM α,βmeATP (C.Y.E.F., unpublished observations, 2006).
Reagents
Collagen type I, as a suspension of native fibers from bovine tendon, was the gift of Ethicon. BAPTA-AM, α,βmeATP, PGI2, and type VII apyrase were from Sigma-Aldrich. Spermine NONOate was from Alexis Biochemicals. 2-[1-(3-Dimethylaminopropyl)indol-3-yl]-3-(indol-3-yl) maleimide (GF109203X), N6-(2-methyl-thioethyl)-2-(3,3,3-trifluoropropylthio)-β,γ-dichloromethylene-ATP (U73122), and 1-(6-{[17β-3-methoxyestra-1,3,5(10)-trien-17-yl]-amino}hexyl-2,5-pyrrolidine-dione (U73343) were from Tocris Bioscience. The triacetylated lipopeptide Pam3CSK4 that activates platelets via the TLR 2/1 complex,21–24 was from Source Bioscience.
Luminescence measurement of ATP secretion
ATP secretion was measured with a Model 400 lumi-aggregometer (Chronolog), using the CHRONO-LUME luciferin:luciferase assay kit from Labmedics according to the manufacturer's guidelines.
Analysis
Sample records of [Ca2+]i and ATP release are representative of experiments from at least 4 separate donors. Because of variability in responses between donors, average results (± SEM) are expressed as a percentage of control runs. Statistical analysis was assessed using the Student paired t test (significance is indicated at levels of *.05, **.01, and ***.001).
Results
Marked heterogeneity in the ability of PGI2 to inhibit Ca2+ responses downstream of different platelet receptors
To assess the effect of PGI2 on platelet Ca2+ responses stimulated by a range of agonists, we initially identified a supramaximal concentration of this potent endothelial-derived inhibitor (60μM) from preliminary experiments using the strong agonist thrombin (C.Y.E.F., unpublished observations, 2006). PGI2 abolished robust [Ca2+]i responses evoked by near-EC50 concentrations of the G protein-coupled receptor agonists U46619 (TxA2 analog, 0.5μM; 0.0% ± 0.2% of control, P < .001; Figure 1A,F) and thrombin (0.03 U mL−1; 2.1% ± 0.5% of control, P < .001; Figure 1B,F) under conditions where a substantial component of the response is because of secondary activation of P2X1 receptors.17 In contrast, a large component of the Ca2+ response stimulated by low or intermediate concentrations of collagen that we have shown previously to depend entirely on GPVI,17 remained in the presence of PGI2 (48.2% ± 4.3% and 56.2% ± 6.2% of control at 0.5 and 2.0 μg mL−1, respectively, P < .001; Figure 1C,F). Interestingly, a similar proportion of the Ca2+ increase stimulated by 1 and 10 μg mL−1 Pam3CSK4 (46.2% ± 2.4% and 52.3% ± 1.9%), which activates platelets via TLR2/1,21–24 was also resistant to 60μM PGI2 (Figure 1D,F). Finally, P2X1 receptor-evoked Ca2+ responses stimulated by the selective agonist α,βmeATP (10μM) were completely insensitive to this supramaximal concentration of PGI2 (Figure 1E-F), as shown for lower concentrations of PGE1 in a previous study.29 Thus, it is clear that the Ca2+ responses downstream of different platelet receptors vary markedly in their sensitivity to inhibition by PGI2.
The potent endogenous inhibitor PGI2 abolishes platelet Ca2+ responses to G protein-coupled receptors but not those after activation of GPVI, Toll-like receptors, or P2X1 cation channels. Effect of a supramaximal concentration of PGI2 (60μM; 90 seconds) on [Ca2+]i increases mediated via a range of receptors. Representative responses from more than 4 donors are shown in panels A through E, and the average as a percentage of a paired control is shown in panel F. The G protein–coupled receptor agonists U46619 (A,F; U4) and thrombin (B,F; Thr) were used at near-EC50 concentrations (0.5μM U46619 and 0.03 U mL−1 thrombin). GPVI and TLR2/1 receptor Ca2+ responses were stimulated with a low or intermediate concentration of collagen (0.5 and 2 μg mL−1; C,F; Coll) or Pam3CSK4 (1 and 10 μg mL−1, D,F; Pam), respectively. P2X1 receptors were maximally activated with 10μM α,βmeATP (E-F). The asterisks indicate significance levels compared with samples in the absence of PGI2; the hash symbols indicate significance level compared with thrombin in the presence of PGI2. U4 indicates U46619; Pam, Pam3CSK4; Thr, thrombin; and Coll, collagen.
The potent endogenous inhibitor PGI2 abolishes platelet Ca2+ responses to G protein-coupled receptors but not those after activation of GPVI, Toll-like receptors, or P2X1 cation channels. Effect of a supramaximal concentration of PGI2 (60μM; 90 seconds) on [Ca2+]i increases mediated via a range of receptors. Representative responses from more than 4 donors are shown in panels A through E, and the average as a percentage of a paired control is shown in panel F. The G protein–coupled receptor agonists U46619 (A,F; U4) and thrombin (B,F; Thr) were used at near-EC50 concentrations (0.5μM U46619 and 0.03 U mL−1 thrombin). GPVI and TLR2/1 receptor Ca2+ responses were stimulated with a low or intermediate concentration of collagen (0.5 and 2 μg mL−1; C,F; Coll) or Pam3CSK4 (1 and 10 μg mL−1, D,F; Pam), respectively. P2X1 receptors were maximally activated with 10μM α,βmeATP (E-F). The asterisks indicate significance levels compared with samples in the absence of PGI2; the hash symbols indicate significance level compared with thrombin in the presence of PGI2. U4 indicates U46619; Pam, Pam3CSK4; Thr, thrombin; and Coll, collagen.
PGI2-insensitive Ca2+ responses downstream of GPVI and TLRs are because of both P2X1 activation and release of intracellularly stored Ca2+
Selective deletion of P2X1 receptor responses, by desensitization with 0.6μM α,βmeATP before addition of extracellular Ca2+,17 inhibited most of the PGI2-insensitive Ca2+ response at the lower concentration of either collagen (0.5 μg mL−1) or Pam3CSK4 (1 μg mL−1), with a reduction to 10.9% ± 1.4% and 11.4% ± 2.7% of control, respectively (Figure 2A-B). At the higher concentration of both collagen (2 μg mL−1) and Pam3CSK4 (10 μg mL−1), the initial peak was also lost after P2X1 desensitization; however, a slowly developing Ca2+ response was still observed (19.3% ± 4.2 and 29.2% ± 8.0% control, respectively; Figure 2C-F). This remaining Ca2+ response was still present in the absence of external Ca2+ (1mM EGTA saline; Figure 2E-F) or after inhibition of fibrinogen binding to the αIIbβ3 integrin using Reopro (data not shown), but it was reduced to very low levels by the phospholipase C inhibitor U73122 (10μM; Figure 2E-F). Interestingly, a concentration of wortmannin that blocks PI3-kinase (100nM)30 had no effect on this Ca2+ response when collagen was the agonist (Figure 2E), but it blocked the response to Pam3CSK4 (Figure 2F). P2Y12 receptors are known to stimulate PI3-kinase and have been reported to enhance Ca2+ release in the platelet.31 However, secondary stimulation of P2Y receptors does not contribute to the PGI2-resistant Ca2+ release downstream of TLR2/1 or GPVI because the Ca2+ release evoked by 10μM ADP was completely blocked by PGI2 (reduction to 0.6% ± 0.6% of control, P < .001; data not shown). Together, these data clearly demonstrate a major role for P2X1 receptors in the PGI2-resistant Ca2+ responses through GPVI and the TLR2/1 complex. In addition, 1 or more PGI2-insensitive Ca2+ release mechanism(s) are activated via a PLC-dependent pathway downstream of GPVI and TLRs 2/1, which for the latter requires PI3-kinase activation.
PGI2-resistant Ca2+ responses to GPVI and Toll-like receptors are mediated through both P2X1 receptor-dependent entry and release of intracellular stores. (A-D) Sample [Ca2+]i responses to collagen and Pam3CSK4 in the presence of 60μM PGI2 with and without functional P2X1 receptors. P2X1 receptors were desensitized by addition of 0.6μM α,βmeATP 60 seconds before addition of external Ca2+ and 90 seconds before agonist addition. PGI2-resistant Ca2+ responses at a low concentration of agonist (A, 0.5 μg mL−1 collagen and B, 1 μg mL−1 Pam3CSK4), were mainly because of P2X1 receptors. At a higher agonist concentration (C, 2 μg mL−1 collagen and D, 10 μg mL−1 Pam3CSK4), a slower, P2X1-independent component was revealed. (E-F) Average peak [Ca2+]i responses to 2 μg mL−1 collagen (coll; E) and 10 μg mL−1 Pam3CSK4 (Pam; F) under various conditions (60μM PGI2, desensitization of P2X1 receptors with 0.6μM α,βmeATP, 1mM EGTA (0 Ca2+) medium, 10μM U73122, and 100nM wortmannin. Asterisks indicate the significance level compared with control samples in the absence of PGI2, and hash symbols indicate the significance level compared with samples in the presence of PGI2 after desensitization of P2X1.
PGI2-resistant Ca2+ responses to GPVI and Toll-like receptors are mediated through both P2X1 receptor-dependent entry and release of intracellular stores. (A-D) Sample [Ca2+]i responses to collagen and Pam3CSK4 in the presence of 60μM PGI2 with and without functional P2X1 receptors. P2X1 receptors were desensitized by addition of 0.6μM α,βmeATP 60 seconds before addition of external Ca2+ and 90 seconds before agonist addition. PGI2-resistant Ca2+ responses at a low concentration of agonist (A, 0.5 μg mL−1 collagen and B, 1 μg mL−1 Pam3CSK4), were mainly because of P2X1 receptors. At a higher agonist concentration (C, 2 μg mL−1 collagen and D, 10 μg mL−1 Pam3CSK4), a slower, P2X1-independent component was revealed. (E-F) Average peak [Ca2+]i responses to 2 μg mL−1 collagen (coll; E) and 10 μg mL−1 Pam3CSK4 (Pam; F) under various conditions (60μM PGI2, desensitization of P2X1 receptors with 0.6μM α,βmeATP, 1mM EGTA (0 Ca2+) medium, 10μM U73122, and 100nM wortmannin. Asterisks indicate the significance level compared with control samples in the absence of PGI2, and hash symbols indicate the significance level compared with samples in the presence of PGI2 after desensitization of P2X1.
PGI2-sensitive and -insensitive ATP release
Consistent with a role for secondary activation of P2X1 receptors in the PGI2-resistant Ca2+ responses, we found that 60μM PGI2 completely blocked the ATP release evoked by U46619 and thrombin (0.9% ± 0.2% and 1.2% ± 0.4% at 0.5μM U46619 and 0.03 U mL−1 thrombin, respectively; Figure 3A,B,E) but that it only partially reduced the secretion response to collagen (35% ± 12.0% and 60% ± 5.4% of control for 0.5 and 2 μg mL−1 collagen, respectively; Figure 3C,E). At 1 μg mL−1 Pam3CSK4, we failed to detect any ATP secretion; however, at 10 μg mL−1 of the TLR2/1 agonist, a proportion (13.9% ± 2.9%) of the ATP secretion was still observed in the presence of 60μM PGI2 (Figure 3D-E). Among the 4 agonists tested, the variable sensitivity to PGI2 was not dependent on the absolute size of the secretory response, as can be clearly seen by comparing the sample recordings in Figure 3A through D.
Dense granule secretion stimulated by collagen and Pam3CSK4 is partially resistant to PGI2. Representative (A-D) and average peak (E) extracellular ATP levels monitored by luciferin:luciferase showing the effect of a supramaximal concentration of PGI2 (60μM; 90 seconds) on dense granule secretion evoked by U46619, thrombin, collagen, and Pam3CSK4. Agonist concentrations match those used in Ca2+ responses (Figures 1–2), with the exception that no detectable ATP release was observed with the lower concentration of Pam3CSK4 (1 μg mL−1). Asterisks indicate the significance level compared with control samples in the absence of PGI2, and hash symbols indicate the significance level compared with thrombin in the presence of PGI2.
Dense granule secretion stimulated by collagen and Pam3CSK4 is partially resistant to PGI2. Representative (A-D) and average peak (E) extracellular ATP levels monitored by luciferin:luciferase showing the effect of a supramaximal concentration of PGI2 (60μM; 90 seconds) on dense granule secretion evoked by U46619, thrombin, collagen, and Pam3CSK4. Agonist concentrations match those used in Ca2+ responses (Figures 1–2), with the exception that no detectable ATP release was observed with the lower concentration of Pam3CSK4 (1 μg mL−1). Asterisks indicate the significance level compared with control samples in the absence of PGI2, and hash symbols indicate the significance level compared with thrombin in the presence of PGI2.
ATP secretion stimulated by collagen and Pam3CSK4 depends on coactivation of PKC and Ca2+ mobilization but is not amplified by P2X1 receptors
Desensitization of P2X1 receptors had no effect on the collagen-evoked release of ATP from dense granules (100.7% ± 17.0% and 98.3% ± 7.8% of control at 0.5 μg mL−1 and 2.0 μg mL−1 collagen, respectively, P > .05; Figure 4A-B). Thus, although previous studies have shown that Ca2+ influx through this ionotropic receptor causes granule centralization,32 this does not potentiate the initial dense granule secretion after collagen stimulation. Instead, collagen-evoked secretion was dependent on activation of phospholipase C because it was virtually abolished by the PLC inhibitor U7312233 (reduction to 7.0% ± 2.6% of control after 10 minutes incubation with 10μM, P < .001; Figure 4C,E). Although U73122 is a recognized and widely used PLC inhibitor, off-target effects have been reported previously34 ; however, the same concentration (10μM) of the inactive analog U73343 had no significant effect on secretion evoked by 0.5 μg mL−1 collagen (89% ± 13%, P > .05; n = 3). The downstream signaling leading to secretion involved a combination of protein kinase C (PKC) and Ca2+ mobilization as both the pan-PKC inhibitor GF109203X (20μM; 10 minutes)35 and loading with the Ca2+ chelator BAPTA (15μM; 30 minutes) partially blocked ATP secretion (reduction to 26.5% ± 5.7% [P < .05] and 41.2% ± 5.6% [P < .001] of control, respectively; Figure 4E). When combined, GF109203X and BAPTA (5.7% ± 1.5% of control, P < .001) were as effective as PLC inhibition with 10μM U73122 (Figure 4D). Evidence for a similar secretory pathway also was obtained for TLR2/1 receptors, because ATP release stimulated by 10μM Pam3CSK4 was sensitive to U73122, cytosolic BAPTA, and GF109203X, although Ca2+ chelation and PKC inhibition were as effective as PLC blockade (Figure 5).
Collagen-evoked ATP release requires PLC activation but not P2X1 receptors and involves costimulation of Ca2+ mobilization and PKC. Sample (A,C,D) and average (B,E) ATP secretion responses to collagen (0.5 μg mL−1), monitored by luciferin:luciferase. (A-B) Effect of desensitization of P2X1 receptors using 0.6μM α,βmeATP before addition of external Ca2+. (C-E) Effect of the PLC inhibitor U73122 (10μM; 10 minutes), cytosolic loading of the Ca2+ chelator BAPTA (15μM BAPTA-AM), the PKC inhibitor GF109203X (20μM; 10 minutes; GF), or combined BAPTA loading and GF109203X.
Collagen-evoked ATP release requires PLC activation but not P2X1 receptors and involves costimulation of Ca2+ mobilization and PKC. Sample (A,C,D) and average (B,E) ATP secretion responses to collagen (0.5 μg mL−1), monitored by luciferin:luciferase. (A-B) Effect of desensitization of P2X1 receptors using 0.6μM α,βmeATP before addition of external Ca2+. (C-E) Effect of the PLC inhibitor U73122 (10μM; 10 minutes), cytosolic loading of the Ca2+ chelator BAPTA (15μM BAPTA-AM), the PKC inhibitor GF109203X (20μM; 10 minutes; GF), or combined BAPTA loading and GF109203X.
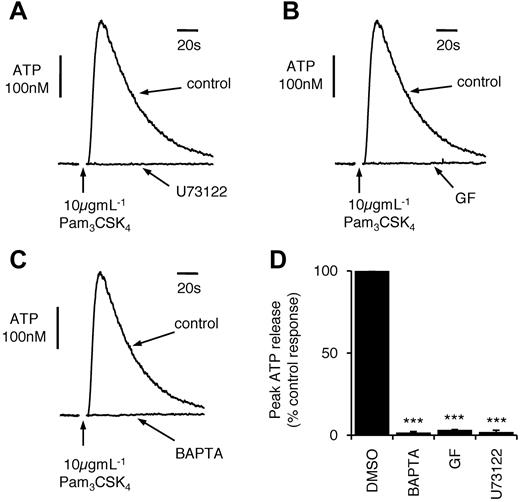
Toll-like receptor–evoked ATP release requires activation of PLC, PKC, and an increase in intracellular Ca2+. Sample (A-C) and average (D) ATP release stimulated by 10 μg mL−1 Pam3CSK4, showing the effect of the PLC inhibitor U73122 (10μM; 10 minutes), intracellular loading with the Ca2+ chelator BAPTA (15μM BAPTA-AM) or the PKC inhibitor GF109203X (20μM; 10 minutes; GF).
Toll-like receptor–evoked ATP release requires activation of PLC, PKC, and an increase in intracellular Ca2+. Sample (A-C) and average (D) ATP release stimulated by 10 μg mL−1 Pam3CSK4, showing the effect of the PLC inhibitor U73122 (10μM; 10 minutes), intracellular loading with the Ca2+ chelator BAPTA (15μM BAPTA-AM) or the PKC inhibitor GF109203X (20μM; 10 minutes; GF).
Secondary P2X1 activation also displays resistance to nitric oxide but is substantially reduced by soluble ectonucleotidase activity.
Endothelial-derived NO is a further important endogenous regulator of platelet activation, acting predominantly by elevating platelet cyclic GMP concentrations.1 As observed for PGI2, a large component of the peak Ca2+ increase stimulated by a low concentration of collagen or Pam3CSK4 (71.8% ± 5.9%, P < .01 and 55.3% ± 5.5%, P < .001, respectively) was resistant to a maximal concentration (K.M.N., unpublished observations, 2006) of the NO donor spermine NONOate (100μM for 10 minutes; Figure 6A-B,E). The NO-resistant component was mainly attributable to secondary activation of P2X1 receptors because Ca2+ increases were reduced to 11.2% ± 1.2 and 12.5 ± 1.7% of control for collagen and Pam3CSK4 after desensitization with α,βmeATP (Figure 6A-B,E).17 Consistent with this effect, secretion stimulated by collagen and Pam3CSK4 was far less sensitive to elevation of NO compared with ATP release after G protein-coupled receptor stimulation (Figure 6F).36,37 In addition, 100μM spermine NONOate had no effect (99.4% ± 8.4% of control, P > .05) on P2X1-evoked Ca2+ increases stimulated with α,βmeATP (10μM; Figure 6C,E). Therefore, collagen- and TLR2/1-evoked Ca2+ signals are also able to continue in the presence of NO and elevated cGMP mainly because of secondary activation of ionotropic P2X1 receptors.
Secondary P2X1 receptor activation is resistant to nitric oxide but is substantially attenuated by increased ectonucleotidase activity. [Ca2+]i responses (A-E) and ATP secretion (F) induced by a range of agonists (U46619 [U4], thrombin [Thr], collagen [Coll], Pam3CSK4 [Pam], and α,βmeATP) were studied under control conditions and after exposure to either spermine NONOate (sNO; 100μM) or increased apyrase (3.2 U mL−1). In addition, the contribution of P2X1 receptors was assessed by desensitization before addition of external Ca2+ using 0.6μM α,βmeATP. Asterisks indicate the significance level compared with control samples in the absence of sNO, and hash symbols indicate the significance level compared with samples in the presence of sNO (E) or compared with thrombin in the presence of sNO (F).
Secondary P2X1 receptor activation is resistant to nitric oxide but is substantially attenuated by increased ectonucleotidase activity. [Ca2+]i responses (A-E) and ATP secretion (F) induced by a range of agonists (U46619 [U4], thrombin [Thr], collagen [Coll], Pam3CSK4 [Pam], and α,βmeATP) were studied under control conditions and after exposure to either spermine NONOate (sNO; 100μM) or increased apyrase (3.2 U mL−1). In addition, the contribution of P2X1 receptors was assessed by desensitization before addition of external Ca2+ using 0.6μM α,βmeATP. Asterisks indicate the significance level compared with control samples in the absence of sNO, and hash symbols indicate the significance level compared with samples in the presence of sNO (E) or compared with thrombin in the presence of sNO (F).
A low concentration of apyrase, a form of NTPDase from potato that displays similar properties to human CD39,38 was present at 0.32 U mL−1 in all experiments to limit spontaneous platelet activation and reduce desensitization of P2 receptors.28 Interestingly, elevation of apyrase to 3.2 U mL−1 in the experimental saline reduced the Ca2+ response stimulated by 0.5 μg mL−1 collagen to 31.3% ± 2.3% of control (P < .001; Figure 6D-E). We have found previously that combined inhibition of platelet P2Y1 and P2Y12 receptors in the presence of 0.32 U mL−1 apyrase reduces the peak collagen-evoked Ca2+ increase to 80% ± 4% of control,17 and it is well established that increasing apyrase levels to less than 3.2 U mL−1 eliminates secondary platelet P2Y receptor responses after release of ADP.39 Thus, we estimate that the 10-fold increase in apyrase in our experiments reduces P2X1-evoked Ca2+ signals by at least 49% (80%-31%) of control. A small P2X1-dependent signal remained in 3.2 U mL−1 apyrase, because the peak was further reduced to 12.1% ± 1.3% of the response (P < .05) by pre-addition of α,βmeATP (Figure 6D-E).
Collagen-evoked P2X1 receptor activation is efficiently maintained at reduced platelet densities, indicating a local mechanism of activation
The above-mentioned data demonstrate that P2X1 cation channels can be activated downstream of GPVI and TLR2/1 receptors even when ATP secretion is greatly reduced by PGI2, NO, or apyrase (Figures 3 and 6), or when it is undetectable, as in the case of 1 μg mL−1 Pam3CSK4 (see “PGI2-sensitive and -insensitive ATP release”). This can be explained by a predominantly autocrine compared with paracrine mechanism of P2X1 activation. To further explore this hypothesis, we measured the contribution of P2X1 receptors to collagen-evoked Ca2+ increases as the platelet density was varied 10-fold (Figure 7). We reasoned that a paracrine response would be reduced, whereas a purely autocrine response would be unaffected by platelet density. The peak ATP increase after stimulation with 0.5 μg mL−1 collagen varied with platelet density as expected for an assay that detects the average extracellular ATP concentration (Figure 7A-B). The peak collagen-evoked Ca2+ response, with and without the P2X1 component, also decreased as the number of platelets in the cuvette was reduced and displayed a slower time course in the most dilute samples (Figure 7C-D). This effect on GPVI activation probably results from use of macroscopic collagen fibers where the ligand distribution within the medium is not homogeneous, and thus the probability of interacting with a surface receptor falls with platelet density. Importantly, the percentage contribution of P2X1 receptors to the collagen-evoked Ca2+ increase was not affected by platelet density (P > .05; Figure 7E). The peak ATP level measured in the bulk phase was in the order of 150nM or less, representing a submaximal P2X1 stimulus;40 thus, saturation of a paracrine-mediated P2X1 response cannot account for the lack of effect of altering platelet density in these experiments. A plausible explanation is that P2X1 receptors are activated by ATP close to the sites of secretion where the concentration of agonist is independent of cell density. Overall, these data are consistent with the concept that ATP released from platelets locally and efficiently activates P2X1 receptors, thereby allowing this ion channel to generate Ca2+ influx even at low levels of dense granule secretion.
Amplification of collagen-evoked Ca2+ responses by P2X1 receptors is independent of platelet density. Representative (A,C) and average (B,D,E) ATP secretion (A-B) and [Ca2+]i responses (C-E) evoked by collagen (0.5 μg mL−1) at platelet densities of 10% to 100% (where 100% is equivalent to that in plasma). The contribution of P2X1 receptors was assessed by desensitization before addition of external Ca2+ using 0.6μM α,βmeATP (desensitized P2X1). (D) Absolute peak Ca2+ response under control conditions (dark bars) and after desensitization of P2X1 receptors with 0.6μM α,βmeATP (light bars). (E) Peak Ca2+ response as a percentage of control responses after P2X1 receptor desensitization with 0.6μM α,βmeATP; there was no significant difference between responses in panel E across the range of platelet densities.
Amplification of collagen-evoked Ca2+ responses by P2X1 receptors is independent of platelet density. Representative (A,C) and average (B,D,E) ATP secretion (A-B) and [Ca2+]i responses (C-E) evoked by collagen (0.5 μg mL−1) at platelet densities of 10% to 100% (where 100% is equivalent to that in plasma). The contribution of P2X1 receptors was assessed by desensitization before addition of external Ca2+ using 0.6μM α,βmeATP (desensitized P2X1). (D) Absolute peak Ca2+ response under control conditions (dark bars) and after desensitization of P2X1 receptors with 0.6μM α,βmeATP (light bars). (E) Peak Ca2+ response as a percentage of control responses after P2X1 receptor desensitization with 0.6μM α,βmeATP; there was no significant difference between responses in panel E across the range of platelet densities.
Discussion
Among the numerous surface receptors expressed in platelets, P2X1 receptor ion channels exhibit several properties that allow them to contribute uniquely to activation by extracellular agonists.16 They are the only platelet receptors stimulated by the ATP that is released from damaged cells and secreted by activated platelets. Furthermore, the binding of ATP directly gates channel opening, thereby stimulating Ca2+ entry more rapidly than other receptors.16,37,41 Finally, P2X1 receptors are less sensitive to inhibition by cyclic nucleotides than the IP3-gated cation channels responsible for release of intracellular Ca2+ stores and thus also the initial event triggering store-operated Ca2+ entry during agonist stimulation.1,2,29,36 In the circulation, shear stress ensures the marginalization of platelets to the periphery of the vessel where platelets encounter endothelium-derived PGI2 and NO and CD39 expressed on the endothelial surface. Whereas we have an understanding of how these inhibitors regulate platelet function, it is unclear how platelets overcome their effects at sites of injury to enable hemostasis. Here, we show that P2X1 receptors provide a mechanism to overcome inhibition by PGI2, NO, and CD39 and to promote acute atherothrombotic events. Notably, because P2X1 receptors are able to contribute to secondary Ca2+ responses even at a high concentration of all 3 inhibitors, activation of this ionotropic receptor might be particularly important in the early stages of thrombosis and hemostasis during stimulation by collagen exposed in the subendothelium after normal vessel injury or fissure of atherosclerotic plaques.16,42,43 P2X1-dependent amplification of threshold signaling through GPVI would enhance the likelihood of individual platelet tethering and formation of the initial layer of platelets on the damaged vessel wall. This would be especially relevant under high-shear, high-flow conditions where the time available for activation is restricted,42,44 and provides an explanation for the greater contribution of P2X1 receptors to arterial compared with venous thrombosis.16,42,45 This amplifying role of P2X1 receptors could be more important at sites of atherosclerotic plaques where stenosis increases the shear level several fold higher than in the normal circulation.46 Given this unique contribution to platelet activation, P2X1 antagonists should be considered as potential antithrombotic therapies, possibly in combination with soluble CD39 to cotarget P2Y receptor activation.4,5 It is also worthwhile noting that we observe significant variation between donors in the magnitude and robustness of P2X1 responses ex vivo.16 Although the extent to which this variation occurs in vivo is unknown, it does raise the possibility that the effectiveness of anti-P2X1 therapies could be greater in a proportion of patients.
Atherosclerosis is widely recognized to be an inflammatory disease, because of the pivotal role of activated immune cells in plaque development.47 TLRs, key components of the innate immune system, have been implicated in the initiation and development of atherosclerosis.48 Platelets have emerging roles in immune responses20 and are known to possess several TLRs, with TLR2 representing the major functional subtype.21–24 Currently, the signaling pathways to which platelet TLRs are coupled are poorly defined, although it is known that Pam3CSK4 generates functional responses including secretion,TxA2 production, and aggregation via pathways conserved with GPVI, including PI3-kinase and phosphorylation of Akt, ERK1/2, and p38.21–24 Our findings suggest that TLR2/1 receptors, like GPVI, also stimulate secretion via PLCγ2 and are similarly resistant to cyclic nucleotides.49 However, GPVI and TLR2/1 must differ in their ability to activate PI3-kinase, because only TLR2/1-dependent Ca2+ release was incrementally blocked by wortmannin. Although further studies are required to investigate this differential coupling to PI3-kinase, our hypothesis also is supported by previous observations that the profile of phosphorylation events downstream of TLR2/1 differs markedly from that observed with classic thrombotic stimuli.24 Nevertheless, the ability of TLRs to evoke platelet secretion and Ca2+ mobilization in the presence of maximal PGI2 and NO offers the potential for enhanced platelet responses during infection and inflammation even in the intact circulation and thus to contribute to the progression of atherosclerosis.
At low concentrations of both collagen and the TLR2/1 complex agonist, cyclic nucleotide–resistant responses resulted primarily from efficient autocrine activation of P2X1. However at higher agonist concentrations, an additional Ca2+ mobilization pathway was uncovered. This resulted from release, rather than influx, of Ca2+. However, because larger amplitude Ca2+ responses evoked through Gq-coupled pathways were completely inhibited by PGI2 and NO, the response is unlikely to be explained purely by differential inhibition of IP3 receptors.15 A much lower cyclic nucleotide sensitivity of PLCγ2 compared with PLCβ may account for the Ca2+ release remaining in the presence of PGI2 and NO. A precedent for this proposal exists, because different PLCβ isoforms vary markedly in their sensitivity to PKA phosphorylation and subsequent inhibition.15 This is also likely to account for GPVI- and TLR2/1-dependent ATP secretion being more resistant to PGI2 and NO than that resulting from G protein-coupled receptors, as first demonstrated by Rink and Sanchez50 using collagen and thrombin.
In conclusion, this study provides evidence that platelets possess at least 2 Ca2+ mobilization mechanisms that are resistant to major endothelium-derived inhibitors of platelet function. Influx through the ATP-gated P2X1 receptor is largely responsible for the inhibitor-resistant pathway at low levels of GPVI and TLR2/1 stimulation. At higher collagen and Pam3CSK4 concentrations, a PLC-coupled Ca2+ release mechanism also contributes. The ability of P2X1 to amplify subthreshold or threshold stimuli could provide sufficient activation to initiate thrombosis when inhibitory endothelial influences remain active. Our findings provide further support that P2X1 represents a novel complementary drug target in the treatment of thrombosis.
There is an Inside Blood commentary on this article in this issue.
The publication costs of this article were defrayed in part by page charge payment. Therefore, and solely to indicate this fact, this article is hereby marked “advertisement” in accordance with 18 USC section 1734.
Acknowledgments
The authors thank Prof Richard Evans for comments on the manuscript, Dr Kam Pui Fung for assistance with statistical analysis, and Dr Joy Wright for measuring platelet counts.
This work was funded by the British Heart Foundation (PG/05/014).
Authorship
Contribution: C.Y.E.F. and S.J. performed the research and analyzed the data; A.N. performed the research; K.M.N. and R.W.F. contributed essential materials and discussion; and M.P.M.-S., S.J., and C.Y.E.F. designed the study and wrote the paper.
Conflict-of-interest disclosure: C.Y.E.F. and M.P.M.-S. hold a patent on “Potent small molecule P2X1 antagonist for antiplatelet drug development.” The remaining authors declare no competing financial interests.
Correspondence: Martyn P. Mahaut-Smith, Department of Cell Physiology and Pharmacology, Maurice Shock Medical Sciences Building, University Road, University of Leicester, PO Box 138, Leicester LE1 9HN, United Kingdom; e-mail: mpms1@le.ac.uk.
References
Author notes
C.Y.E.F. and S.J. contributed equally to this study.

![Figure 1. The potent endogenous inhibitor PGI2 abolishes platelet Ca2+ responses to G protein-coupled receptors but not those after activation of GPVI, Toll-like receptors, or P2X1 cation channels. Effect of a supramaximal concentration of PGI2 (60μM; 90 seconds) on [Ca2+]i increases mediated via a range of receptors. Representative responses from more than 4 donors are shown in panels A through E, and the average as a percentage of a paired control is shown in panel F. The G protein–coupled receptor agonists U46619 (A,F; U4) and thrombin (B,F; Thr) were used at near-EC50 concentrations (0.5μM U46619 and 0.03 U mL−1 thrombin). GPVI and TLR2/1 receptor Ca2+ responses were stimulated with a low or intermediate concentration of collagen (0.5 and 2 μg mL−1; C,F; Coll) or Pam3CSK4 (1 and 10 μg mL−1, D,F; Pam), respectively. P2X1 receptors were maximally activated with 10μM α,βmeATP (E-F). The asterisks indicate significance levels compared with samples in the absence of PGI2; the hash symbols indicate significance level compared with thrombin in the presence of PGI2. U4 indicates U46619; Pam, Pam3CSK4; Thr, thrombin; and Coll, collagen.](https://ash.silverchair-cdn.com/ash/content_public/journal/blood/119/15/10.1182_blood-2011-10-386052/5/m_zh89991286710001.jpeg?Expires=1766222429&Signature=oiKsf4d87RCnI0qzKz2YxDpnTFHSiQ5rRt9tXwyfJLDDujKW2vaJ6VdQy2apCD5dwwIfPjz8vTtgF-sCuioHmY6z03bTOwc4Egw--5z3FbaYrSHAg2wos55r5uICgvrQ7jRQSgXsj~JdAxqB66WO1TOQ0EOaJ6zAszR1QEqc6Hn~~r2wsnSWKxYyMju3wckRb2kHalbNMHrx5PchCERLF8UiPvIAHSbt3ePLoWwvtf-6X4-DBqXvMw6C1YannTPSgrAf9diGl2SrSbCSH4rDNYqmBj3q-2~npKBCO4iitZX7GMd8y5gWBtjPYc9lcUtEok55xJ6OHOVRO-z76PoDnA__&Key-Pair-Id=APKAIE5G5CRDK6RD3PGA)
![Figure 2. PGI2-resistant Ca2+ responses to GPVI and Toll-like receptors are mediated through both P2X1 receptor-dependent entry and release of intracellular stores. (A-D) Sample [Ca2+]i responses to collagen and Pam3CSK4 in the presence of 60μM PGI2 with and without functional P2X1 receptors. P2X1 receptors were desensitized by addition of 0.6μM α,βmeATP 60 seconds before addition of external Ca2+ and 90 seconds before agonist addition. PGI2-resistant Ca2+ responses at a low concentration of agonist (A, 0.5 μg mL−1 collagen and B, 1 μg mL−1 Pam3CSK4), were mainly because of P2X1 receptors. At a higher agonist concentration (C, 2 μg mL−1 collagen and D, 10 μg mL−1 Pam3CSK4), a slower, P2X1-independent component was revealed. (E-F) Average peak [Ca2+]i responses to 2 μg mL−1 collagen (coll; E) and 10 μg mL−1 Pam3CSK4 (Pam; F) under various conditions (60μM PGI2, desensitization of P2X1 receptors with 0.6μM α,βmeATP, 1mM EGTA (0 Ca2+) medium, 10μM U73122, and 100nM wortmannin. Asterisks indicate the significance level compared with control samples in the absence of PGI2, and hash symbols indicate the significance level compared with samples in the presence of PGI2 after desensitization of P2X1.](https://ash.silverchair-cdn.com/ash/content_public/journal/blood/119/15/10.1182_blood-2011-10-386052/5/m_zh89991286710002.jpeg?Expires=1766222429&Signature=0G7O5KsD-51G5MfCEhy0mgGOA2fySPzwBy3ykTLOdi2Dnq0m2LHMX8KGH~wJlgWu7u5lfK-L8LeVQV4bIZDtbG~sSkUMqhRrO1TKNr3bQaiLtkPb341redysUWChmrwKJtkA04BWmV2Dac4MoKU-qIl5ekWm-My1tLdPRDTYdtzUJtdxf6vzzUl9~erOZg8YWyiCNN7JEQB6hgOnR5kd7DAwCUqDWMKsP3ngc-U5ammJ4VMKxdqmL50YhRxLLD1S5C~w0FOSfEPN-Psi6mFMPA81QpSO0jsF5PhiaeJEoOWlG2pBFKp9rBnvvv90mRM-g723QX0GK4yRQxk8UCnLUw__&Key-Pair-Id=APKAIE5G5CRDK6RD3PGA)


![Figure 6. Secondary P2X1 receptor activation is resistant to nitric oxide but is substantially attenuated by increased ectonucleotidase activity. [Ca2+]i responses (A-E) and ATP secretion (F) induced by a range of agonists (U46619 [U4], thrombin [Thr], collagen [Coll], Pam3CSK4 [Pam], and α,βmeATP) were studied under control conditions and after exposure to either spermine NONOate (sNO; 100μM) or increased apyrase (3.2 U mL−1). In addition, the contribution of P2X1 receptors was assessed by desensitization before addition of external Ca2+ using 0.6μM α,βmeATP. Asterisks indicate the significance level compared with control samples in the absence of sNO, and hash symbols indicate the significance level compared with samples in the presence of sNO (E) or compared with thrombin in the presence of sNO (F).](https://ash.silverchair-cdn.com/ash/content_public/journal/blood/119/15/10.1182_blood-2011-10-386052/5/m_zh89991286710006.jpeg?Expires=1766222429&Signature=LB8TDwJKdZohUM0rYpzT38j-41ymjVOAFibsEmzVaeIG~p9haSbQWdBBernBsFbt9PLUc1Y6jqbJeB5Q-GNhzvsnJGOX98Av2~wwNNHJMWcmpMq0xF7KiOfO2vDryWq3pb7iAQQ9GQWNbKUZYWrbWYDUFNmIWqYmg-4MpPrUHsOrQy054t5pSlbc-TVYjG2Lm-5B5qB1m9dVSKrjlMOeBXSv9Vy6foKLAJA8SEn6Iq513LG~5OLSK9hOWB8RbevOaMXkwln2AXNUkLAO40Eu2iqDZtRip3obqSYoEYyTKwrfQiaHfYxu3h7NmHyEOWzC3o1rjoB07A65ZWtHJxJG9w__&Key-Pair-Id=APKAIE5G5CRDK6RD3PGA)
![Figure 7. Amplification of collagen-evoked Ca2+ responses by P2X1 receptors is independent of platelet density. Representative (A,C) and average (B,D,E) ATP secretion (A-B) and [Ca2+]i responses (C-E) evoked by collagen (0.5 μg mL−1) at platelet densities of 10% to 100% (where 100% is equivalent to that in plasma). The contribution of P2X1 receptors was assessed by desensitization before addition of external Ca2+ using 0.6μM α,βmeATP (desensitized P2X1). (D) Absolute peak Ca2+ response under control conditions (dark bars) and after desensitization of P2X1 receptors with 0.6μM α,βmeATP (light bars). (E) Peak Ca2+ response as a percentage of control responses after P2X1 receptor desensitization with 0.6μM α,βmeATP; there was no significant difference between responses in panel E across the range of platelet densities.](https://ash.silverchair-cdn.com/ash/content_public/journal/blood/119/15/10.1182_blood-2011-10-386052/5/m_zh89991286710007.jpeg?Expires=1766222429&Signature=4ovVjqe6KExg5GAWqCphiXqwZf92ukm2dXt55ARc6jwa3X945QmQbqb47OhwBjn2JDyExlv~Nn6P9ESQd1dUqt0geE7t8lG3WHoGq-mJPDvvmXFQeXMKkahoWajyV5Og4fFJvjn5UeZNRjXoq1qCogJSBrgA~2zzPXb7ryKdPfyI6HSQuWTenkF1dlljZpqMFZ00Q7XG5jMx6iMWnvzfTawA7gGZ9MbDLLcOADHhsFMLp~kxCb9zsZ2Q5i~LHUUNqGk50WRQ9CsYwvHTCDoIadJMLeT8mAjMTfcnQXSjVMIQohXINI6bsYPm6ZXRbyYPY23o8G~AtnzSLJ6y941Y7Q__&Key-Pair-Id=APKAIE5G5CRDK6RD3PGA)
