Abstract
Lineage-specific cell-surface molecules, such as CD19 and CD20 on B-lineage malignancies are the targets for immunotherapies. However, the therapeutic success of CD19-specific T-cell therapy is predicted to be dependent on the continued persistence of adoptively transferred T cells. It is well-recognized that exogenous IL-2 can help sustain the in vivo persistence of ex vivo-propagated CD8+ T cells. Therefore, in order to target biologically active IL-2 to the tumor microenvironment, we have used an immunocytokine (ICK) to deliver this cytokine to binding-sites of a CD20-specific monoclonal antibody (mAb) on malignant B cells. This anti-CD20-IL2 ICK was based on the Leu16 anti-CD20 mAb that was dehumanized to remove T-helper epitopes. Flow cytometry demonstrated that anti-CD20-IL2 ICK specifically bound to CD20+ tumor and IL-2R+ T cells. Thus, we investigated the ability of this ICK to improve the persistence of adoptively transferred B-lineage lymphoma-specific T cells. To obtain CD19-specific T cells that could be non-invasively imaged in vivo, we used non-viral gene transfer to introduce a DNA plasmid to co-express both a CD19-specific immunoreceptor (designated CD19R) and firefly luciferase (ffLuc). The CD19R combines antibody recognition with T-cell effector functions mediated through CD3-ζ . The genetically modified T cells were characterized as differentiated CD8+ effector cells expressing the IL-2 receptor complex, which specifically recognize and lyse CD19+ lymphoma targets. To model the survival of adoptively transferred T cells and treatment of lymphoma in vivo, we generated a CD20+CD19+ ARH-77 tumor line expressing the Renilla luciferase (rLuc) reporter gene. Our data demonstrate that this tumor line is resistant to a CD20-specific mAb, Rituximab, in vivo. Sub-optimal doses of CD19R+ffLuc+ CD8+ T cells, which do not cause complete eradication of tumor by themselves, were infused along with anti-CD20-IL2 ICK and control ICK (with irrelevant specificity) in NOD/scid mice bearing xenografts of the rLuc+ tumor. In vivo non-invasive bioluminescent imaging (BLI) was used to longitudinally measure the persistence of ffluc+ T cells and growth of rluc+ tumor. In our mouse model, the T cells persisted significantly (p<0.05) longer in the mice treated with anti-CD20-IL2 ICK, compared to mice receiving the ICK with an irrelevant specificity. This improvement in T-cell persistence translated into augmented anti-tumor activity (Figure). These results suggest that combining tumor-specific ICK with tumor-specific T cells may improve the outcome of immunotherapy. Since Phase I trials are underway using anti-CD20-IL2 ICK and CD19-specific T cells as monotherapy, our results warrant clinical trials using combination of these immunotherapies.
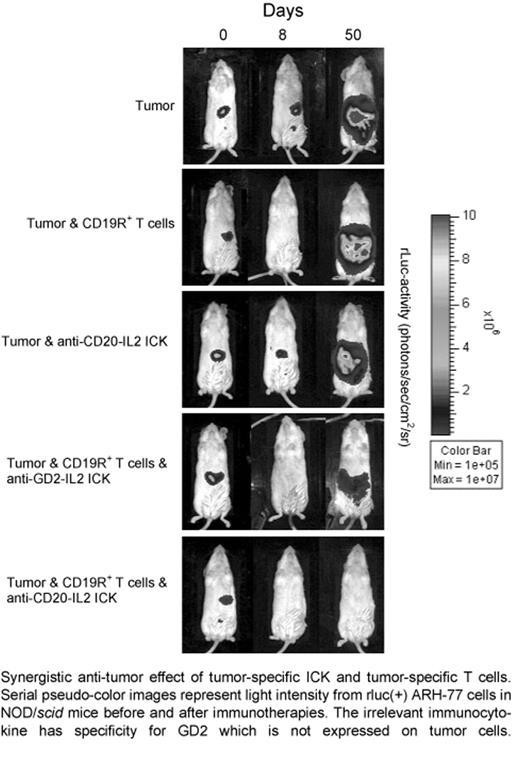
Synergistic anti-tumor effect of tumor-specific ICK and tumor-specific T cells. Serial pseudo-color images represent light intensity from rluc(+) ARH-77 cells in NOD/scid mice before and after immunotherapies. The irrelevant immunocytokine has specificity for GD2 which is not expressed on tumor cells.
Synergistic anti-tumor effect of tumor-specific ICK and tumor-specific T cells. Serial pseudo-color images represent light intensity from rluc(+) ARH-77 cells in NOD/scid mice before and after immunotherapies. The irrelevant immunocytokine has specificity for GD2 which is not expressed on tumor cells.
Author notes
Corresponding author